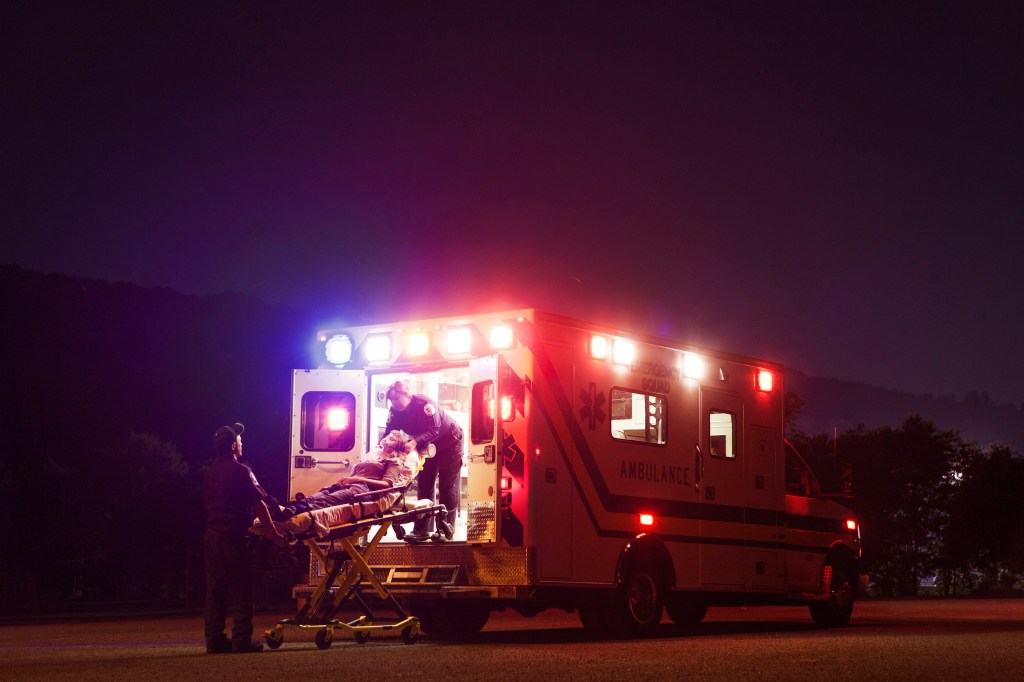
Niños que sobrevivieron al tiroteo del Super Bowl tienen miedo, ataques de pánico y trastornos del sueño
A seis meses de que las chispas de una bala quemaran las piernas de Gabriella Magers-Darger en el tiroteo del desfile del Super Bowl de los Kansas City Chiefs, la joven de 14 años está lista para dejar atrás el pasado.
Enfrenta los desafíos de ser una estudiante de primer año de secundaria, aunque también está emocionada de reencontrarse con sus amigos y volver a bailar y a jugar voleibol. Incluso podría unirse al equipo de lucha libre para ganarse el respeto en la escuela.
Pero el pasado sigue presente.
En una reunión del 4 de julio, un amigo de la familia llevó auriculares que amortiguan el ruido, por si los fuegos artificiales eran demasiado para ella. A principios del verano, Gabriella tuvo dificultades para ver la colección de armas de un pariente, especialmente las pistolas. Y comenzó a hiperventilar cuando vio la herida en el dedo de un amigo de la familia que se había cortado accidentalmente: la vista de la sangre le recordó a Lisa Lopez-Galván, quien murió por una herida de bala afuera de Union Station, la única fatalidad ese día.
Su madre, Bridget Barton, dijo que Gabriella ha tenido una actitud más dura desde el desfile. “Ha perdido algo de suavidad, algo de dulzura”, observó.
Los niños son particularmente vulnerables al estrés de la violencia con armas de fuego, y 10 de las 24 que sufrieron heridas de bala en el desfile del 14 de febrero tenían menos de 18 años. Muchos más niños como Gabriella experimentaron el trauma de primera mano. Enfrentan miedo, ira, problemas de sueño e hipersensibilidad a las multitudes y los ruidos.
Una adolescente de 15 años que recibió disparos en la mandíbula y el hombro prácticamente dejó la escuela por un tiempo, y los ataques de pánico diarios también le impidieron asistir a la escuela de verano.
Un niño de 11 años que recibió un disparo describió sentirse enojado en la escuela por razones que no podía explicar. Una niña de 5 años que estaba sobre los hombros de su padre cuando le dispararon entra en pánico cada vez que su papá se siente enfermo, temiendo que le hayan disparado de nuevo.
“No es la misma niña. Quiero decir, definitivamente no lo es”, dijo Erika Nelson, madre de Mireya, de 15 años, quien tiene cicatrices en la mandíbula y la cara. “Nunca sabes cuándo va a estallar. Nunca sabes. Podrías decir algo o alguien podría mencionar algo que le recuerde ese día”.
En 2020, las armas superaron a los accidentes automovilísticos como la principal causa de muerte de niños, pero un número mucho mayor sufren heridas de balas y sobreviven. La investigación sugiere que los niños sufren lesiones por armas de fuego no fatales entre dos y cuatro veces más a menudo de lo que son asesinados con armas.
Científicos dicen que los efectos a largo plazo de la violencia armada en los niños se investigan poco y son mal comprendidos. Pero el daño es generalizado. Investigadores de Harvard y del Hospital General de Massachusetts encontraron que durante el primer año después de una lesión por arma de fuego, los sobrevivientes infantiles experimentaron un aumento del 117% en trastornos del dolor, del 68% en afecciones psiquiátricas y del 144% en adicciones. Los efectos en la salud mental se extienden a madres, padres y hermanos.
Para muchos afectados por el tiroteo en Kansas City, Missouri, los desencadenantes comenzaron de inmediato.
“Me enojo fácilmente”
A solo 10 días que Samuel Arellano fuera baleado en el desfile, fue a otro gran evento deportivo.
Samuel fue invitado a un partido de baloncesto masculino de la Universidad de Kansas en el Allen Fieldhouse en Lawrence. Durante un descanso del partido, con una cámara de video apuntando a Samuel y a sus padres, Jalen Wilson, ex estrella de KU, apareció en la pantalla y se dirigió a él directamente.
“Escuché tu historia”, dijo Wilson, que ahora juega en la NBA, desde la pantalla gigante. “Estoy muy agradecido de que estés aquí hoy, y es una bendición que podamos tenerte para brindarte el amor y apoyo que realmente mereces”.
Wilson pidió a los 16,000 fans presentes que se pusieran de pie y aplaudieran a Samuel. Mientras la multitud aplaudía y un locutor exclamaba que era un “joven valiente”, Samuel miró a sus padres, luego al suelo, sonriendo tímidamente.
Pero minutos después, cuando el partido se reanudó, Samuel comenzó a llorar y tuvo que salir del auditorio con su madre, Abigail.
“Cuando se puso bastante ruidoso, fue cuando comenzó a desmoronarse de nuevo”, dijo su padre, Antonio. “Así que ella tuvo que salir con él por un momento. Así que cualquier lugar ruidoso, si es demasiado fuerte, lo afecta”.
Samuel, que cumplió 11 años en marzo, fue baleado a la altura de las costillas en su lado derecho. Ahora, la cicatriz en su espalda es apenas perceptible, pero los efectos persistentes del tiroteo son evidentes. Está viendo a un terapeuta, al igual que su padre, aunque a Abigail le ha resultado difícil encontrar uno que hable español y aún no ha tenido una cita.
En las primeras semanas luego del tiroteo, Samuel tuvo problemas para dormir y a menudo se metía en la cama con su madre y su padre. Solía tener buenas notas, pero eso se volvió más difícil, dijo Abigail. Su personalidad ha cambiado, algo que a veces se ha manifestado en la escuela.
“Me enojo fácilmente”, dijo Samuel. “Nunca he sido así antes, pero si me dicen que me siente, me enojo. No sé por qué”.
Los niños traumatizados a menudo tienen dificultades para expresar emociones y pueden tener arrebatos de ira, según Michelle Johnson-Motoyama, profesora de trabajo social en la Universidad Estatal de Ohio.
“Estoy segura que para ese niño hay una sensación de tremenda injusticia por lo que sucedió”, dijo Johnson-Motoyama.
Especialmente justo después del tiroteo, Samuel tenía ataques de pánico y comenzaba a sudar, contó Antonio. Los terapeutas les dijeron que eso era normal. Pero los padres también lo mantuvieron alejado de su teléfono por un tiempo: había demasiado sobre el tiroteo en las noticias y en internet.
Abigail, que trabaja en un concesionaria de automóviles con Antonio, está ansiosa por ver a su hijo cambiar, por su sufrimiento y tristeza. También está preocupada por sus tres hijas, una de 16 años y gemelas de 13. Su padre, Victor Salas, que estaba con Samuel en el desfile, también estaba devastado después de los hechos.
“Estoy llorando y llorando y llorando por lo que pasó”, dijo Salas en español cuatro días después del desfile. “Porque fue un caos. Eso no significa que las familias no amen a su familia, pero todos huyeron para salvar sus propias vidas. Salvé la vida de mis nietos, pero ¿qué pasa con el resto de la gente? No estamos preparados”.
En el lado positivo, Samuel se sintió muy apoyado por la comunidad en Kansas City, Kansas. Muchas personas de su escuela se acercaron en los primeros días para visitarlo, amigos e incluso un ex conductor de autobús, que estaba llorando. Tiene una “habitación llena de dulces”, dijo Abigail, en su mayoría Skittles, su favorito.
En su cumpleaños, recibió una pelota de fútbol americano autografiada por Patrick Mahomes, mariscal de campo de los Kansas City Chiefs. Lo hizo llorar, algo que ocurre con bastante frecuencia, dijo su padre.
“Hay días buenos y malos, días más normales y fáciles, y luego hay días en los que la familia tiene que estar un poco más atenta y apoyarlo”, dijo Abigail en español. “Siempre ha sido extrovertido y hablador como su madre, pero eso ha cambiado desde el desfile”.
El 4 de julio, disparador de una semana
El 4 de julio fue particularmente angustiante para muchos de los jóvenes sobrevivientes y para sus familias. ¿Deberían comprar fuegos artificiales? ¿Querrían celebrar? ¿Por qué todos los petardos que explotan en el vecindario suenan como disparos?
Este año, Gabriella, de 14 años, necesitó la ayuda de su padrastro, Jason Barton, para encender sus fuegos artificiales, algo que normalmente hace con entusiasmo. En el desfile, como muchas personas, la familia Barton primero confundió el sonido de los disparos con fuegos artificiales.
Y Erika Nelson, madre soltera de Belton, Missouri, temía incluso mencionar la celebración a Mireya, quien siempre ha amado el Día de la Independencia. Eventualmente, Mireya dijo que no quería fuegos artificiales grandes este año y que solo quería que su madre los encendiera.
“Cualquier pequeño desencadenante, quiero decir, podría ser un ligero chasquido, y ella se tensaba”, dijo Erika Nelson.
Patty Davis, gerente de programas para el cuidado informado sobre el trauma en el hospital Children’s Mercy en Kansas City, dijo que incluso clientes suyos que estuvieron en el desfile pero no resultaron heridos todavía se estremecen ante los sonidos de sirenas u otros ruidos fuertes. Es una respuesta poderosa a la violencia armada en general, no solo al desfile.
“No es una respuesta exagerada”, dijo Davis. “De hecho, es muy natural para los jóvenes, y no tan jóvenes, que han experimentado algo similar o han presenciado violencia con armas de fuego”.
“No se trata de un trauma accidental, sino de un trauma perpetrado con fines violentos, que puede provocar un mayor nivel de ansiedad en las personas que lo viven, que se preguntan si volverá a suceder. ¿Y qué tan seguras están?”, agregó.
Reviviendo el instante
Los ruidos extraños, las luces brillantes y las multitudes pueden tomar desprevenidos a los niños y a sus padres.
En junio, Mireya Nelson estaba esperando a su hermana mayor después de un recital, con la esperanza de ver a un muchacho. Su madre quería ir, pero Mireya la hizo callar. “De repente, se escuchó un estruendo muy fuerte”, dijo Erika. “Se agachó y luego se levantó de un salto. Dijo: ‘¡Dios mío, me estaban disparando otra vez!’”. Mireya lo dijo tan fuerte que la gente se quedó mirando, así que fue el turno de Erika de hacerla callar y tratar de calmarla. “Le dije: ‘Mireya, está bien. Estás bien. Se les cayó una mesa. Solo están sacando cosas. Fue un accidente’”, explicó Erika.
Pasaron unos minutos hasta que el shock se disipó y más tarde Mireya se rió de la situación, pero Erika siempre está atenta.
La tristeza inicial de su hija (que veía películas durante horas y lloraba todo el tiempo) se ha transformado en descaro. Medio año después, Mireya bromea sobre el tiroteo, lo que destroza a su madre. Pero tal vez eso sea parte del proceso de sanación, dijo Erika.
Antes del 4 de julio, Mireya fue a Worlds of Fun, un gran parque de diversiones, y la pasó bien. Se sintió bien porque había guardias de seguridad por todas partes. También disfrutó de una visita a la oficina local del FBI con una amiga que estaba con ella el día del tiroteo.
Pero cuando alguien le sugirió ir al ballet, Mireya lo descartó rápidamente: está cerca de Union Station, el lugar del tiroteo. Ya no quiere ir al centro. Erika dijo que ha habido muchas citas médicas y dificultades económicas, y que su mayor frustración como madre es no poder arreglar las cosas para su hija.
“Tienen que seguir su propio camino, su propio proceso de curación. No puedo sacudirla, como diciéndole: ‘Vuelve a ser tú misma’”, dijo Erika. “Podría llevar meses, años. ¿Quién sabe? Podría ser el resto de su vida. Pero espero que pueda superarlo un poco”.
Piel de gallina en medio del calor sofocante
James Lemons notó un cambio en su hija de 5 años, Kensley, que estaba sobre sus hombros cuando le dispararon en el desfile.
Antes del tiroteo, Kensley era extrovertida y comprometida, dijo James, pero ahora está retraída, como si estuviera dentro de una burbuja y se hubiera desconectado de la gente.
A Kensley, las grandes multitudes y los policías le recuerdan al desfile. Ambos estuvieron presentes en una graduación de secundaria a la que asistió la familia este verano, y Kensley solo quería irse. James la llevó a un campo de fútbol vacío, donde, dijo, se le puso la piel de gallina y se quejó de tener frío a pesar del calor sofocante.
La hora de dormir es un problema particular para la familia Lemons. Kensley ha estado durmiendo con sus padres. Otro hijo, Jaxson, de 10 años, ha tenido pesadillas. Una noche, soñó que el tirador se acercaba a su padre y lo hacía tropezar, dijo Brandie Lemons, la madrastra de Jaxson.
Los niños más pequeños como Kensley expuestos a la violencia con armas de fuego tienen más probabilidades de desarrollar un trastorno de estrés postraumático que los niños mayores, según Johnson-Motoyama, de la Universidad Estatal de Ohio.
Davis, del Children’s Mercy en Kansas City, dijo que los niños cuyos cerebros no están completamente desarrollados pueden tener dificultades para dormir y comprender que están seguros en sus hogares por la noche.
James le compró a la familia un nuevo cachorro, un bulldog americano que ya pesa 32 libras, para ayudarlos a sentirse protegidos. “Busqué el pedigrí”, dijo, “Son muy protectores. Muy cariñosos”.
En busca de una salida
Para desahogarse después del tiroteo, Gabriella comenzó a boxear. Su madre, Bridget, dijo que le devolvió algo de la confianza y el control que había bajado después del desfile. “Me gusta golpear a la gente, no de una manera mala, lo juro”, dijo Gabriella en abril mientras moldeaba un protector bucal a sus dientes antes de irse a entrenar.
Sin embargo, desde entonces ha dejado de boxear, por lo que el dinero puede destinarse a un viaje a Puerto Rico con su clase de español. Están pagando $153 al mes durante 21 meses para cubrir el viaje. Las clases de boxeo costaban $60 al mes.
Bridget pensaba que el boxeo era una buena salida para la ira que le quedaba, pero a finales de julio Gabriella no estaba segura de si todavía tenía el impulso para contraatacar de esa manera. “El pasado es el pasado, pero todos vamos a pasar por cosas. ¿Tiene sentido?”, preguntó Gabriella.
“Estás bien en general, pero todavía tienes desencadenantes. ¿Es eso lo que quieres decir?”, preguntó su madre. “Sí”, respondió.
Después del tiroteo, Mireya Nelson probó las clases en línea, que no funcionaron bien. Los primeros días de la escuela de verano, Mireya tenía un ataque de pánico todos los días en el auto y su madre la llevaba de vuelta a casa.
Mireya quiere regresar a la escuela secundaria este otoño, y Erika es cautelosa. “Sabes, si vuelvo a la escuela, existe la posibilidad de que me disparen, porque en la mayoría de las escuelas hoy en día hay tiroteos”, recordó Erika que dijo su hija. “Y yo digo: ‘Bueno, no podemos pensar así. Nunca se sabe lo que va a pasar’”.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
10 months 22 hours ago
Mental Health, Noticias En Español, Public Health, States, Children's Health, Guns, Investigation, Kansas, Latinos, Missouri, The Injured
Kids Who Survived Super Bowl Shooting Are Scared, Suffering Panic Attacks and Sleep Problems
KFF Health News and KCUR are following the stories of people injured during the Feb. 14 mass shooting at the Kansas City Chiefs Super Bowl celebration. Listen to how children wounded that day are dealing with their injuries or emotional scars.
Six months after Gabriella Magers-Darger’s legs were burned by sparks from a ricocheted bullet at the Kansas City Chiefs Super Bowl parade in February, the 14-year-old is ready to leave the past behind.
She is dreading the pitfalls of being a high school freshman, even as she looks forward to being back with friends and at color guard, dance, and volleyball. She might even join the wrestling team to get some respect at school.
But the past remains ever present.
At a July Fourth gathering, a family friend brought noise-canceling headphones in case the fireworks became too much. Earlier in the summer Gabriella had a hard time viewing a relative’s gun collection, the handguns in particular. And she hyperventilated when she saw a family friend’s finger after it was sliced by accident — the sight of blood reminds her of seeing a fatally wounded Lisa Lopez-Galvan minutes after she was shot outside Union Station, the only person killed that day.
Her mom, Bridget Barton, said Gabriella has had a chip on her shoulder since the parade.
“She’s lost some softness to her, some gentleness to her,” Barton said.
Children are particularly vulnerable to the stresses of gun violence, and 10 of 24 people injured by bullets at the Feb. 14 parade were under 18 years old. Countless more children like Gabriella experienced the trauma firsthand. They’ve endured fear, anger, sleep problems, and hypersensitivity to crowds and noises.
A 15-year-old girl who was shot through the jaw and shoulder effectively dropped out of school for a time and daily panic attacks kept her from summer school, too. An 11-year-old boy shot in the side described feeling angry at school for reasons he couldn’t explain. A 5-year-old girl who was on her father’s shoulders when he was hit by gunfire panics each time her dad feels sick, fearing he has been shot again.
“She’s not the same kid. I mean, she’s definitely not,” said Erika Nelson, mother of the 15-year-old, Mireya, who has scars on her jaw and face. “You never know when she’s going to snap. You never know. You might say something or someone might bring up something that reminds her of that day.”
Guns overtook motor vehicle accidents as the leading cause of death for children in 2020, but a far higher number of kids are hit by gunfire and survive. Research suggests that kids sustain nonfatal firearm injuries anywhere from two to four times more often than they are killed by guns.
Scientists say the long-term effects of gun violence on kids are little researched and poorly understood. But the harm is pervasive. Harvard and Massachusetts General Hospital researchers found that during the first year after a firearm injury, child survivors experienced a 117% increase in pain disorders, a 68% increase in psychiatric disorders, and a 144% increase in substance use disorders. The mental health effects spill over — to mothers, fathers, siblings.
For many affected by the shooting in Kansas City, Missouri, the triggers began right away.
‘I Get Mad Easily’
Just 10 days after Samuel Arellano was shot at the parade, he attended another big sporting event.
Samuel was invited to attend a University of Kansas men’s basketball game at Allen Fieldhouse in Lawrence. During a break in the game, with a video camera pointed at Samuel and his parents, former KU star Jalen Wilson appeared on the scoreboard and addressed him directly.
“I heard about your story,” Wilson, who now plays in the NBA, said on the big screen. “I’m so very thankful that you are here today and it is a blessing that we can have you to give you the love and support you truly deserve.”
Wilson asked the 16,000 fans in attendance to stand and give Samuel a round of applause. As the crowd clapped and an announcer bellowed about him being a “brave young man,” Samuel looked at his parents, then down at his feet, smiling shyly.
But minutes later when the game resumed, Samuel started to cry and had to leave the auditorium with his mom, Abigail.
“When it got pretty loud, that’s when he started breaking up again,” his dad, Antonio, said. “So she had to step out with him for a minute. So any loud places, if it’s too loud, it’s affecting him.”
Samuel, who turned 11 in March, was shot in the ribs on his right side. The scar on his back is barely noticeable now, but lingering effects from the parade shooting are obvious. He is seeing a therapist — as is his father, though Abigail has had a tough time finding a Spanish-speaking one and still hasn’t had an appointment.
Samuel had trouble sleeping in the first weeks after the shooting and often crawled in bed with his mom and dad. He used to get good grades, but that became more difficult, Abigail said. His personality has changed, which sometimes has shown up at school.
“I get mad easily,” Samuel said. “I [have] never been like this before but like, if they tell me to sit down, I get mad. I don’t know why.”
Traumatized children often have difficulty expressing emotions and may be given to outbursts of anger, according to Michelle Johnson-Motoyama, a professor of social work at Ohio State University.
“I’m sure for that child there is a sense of tremendous injustice about what happened,” Johnson-Motoyama said.
Especially right after the shooting, Samuel had panic attacks, Antonio said, and he’d break out in a sweat. Therapists told them that was normal. But the parents also kept him off his phone for a while, as there was so much about the shooting on the news and online.
Abigail, who works at a car dealership with Antonio, is anxious about seeing her son change, his suffering and sadness. She is also concerned for her three daughters, a 16-year-old and 13-year-old twins. Her father, Victor Salas, who was with Samuel at the parade, was also reeling in its aftermath.
“I’m crying and crying and crying about what happened,” Salas said in Spanish four days after the parade. “Because it was chaos. It doesn’t mean that families don’t love their family, but everyone took off to save their own lives. I saved my grandchildren’s lives, but what happens to the rest of the people? We’re not prepared.”
On the good side, Samuel felt very supported by the community in Kansas City, Kansas. Many people from his school stopped by in the first few days to visit, including friends and even a former bus driver, who was in tears. He has a “room full of candy,” Abigail said, mostly Skittles, his favorite.
An autographed football from Kansas City Chiefs quarterback Patrick Mahomes arrived on his birthday. It made him cry, his father said, which happens pretty often.
“There are good and bad days, days that are more normal and easier, and then there are days where the family has to be a little bit more aware and supportive,” Abigail said in Spanish. “He’s always been outgoing and talkative like his mom, but that has changed since the parade.”
Fourth of July a Weeklong Trigger
The Fourth of July was particularly harrowing for many of the young survivors and their families. Should they buy fireworks? Will they want to celebrate? And why do all the firecrackers going off in the neighborhood sound like gunshots?
Fourteen-year-old Gabriella needed help from her stepfather, Jason Barton, to light her fireworks this year, something she is ordinarily enthusiastic about doing herself. At the parade, like many people, the Barton family initially mistook the sound of gunfire for fireworks.
And Erika Nelson, a single mom in Belton, Missouri, feared even bringing up the holiday with Mireya, who has always loved Independence Day. Eventually Mireya said she didn’t want any big fireworks this year and wanted only her mom to set theirs off.
“Just any little trigger — I mean, it could be a light crackle — and she just clenched,” Erika Nelson said.
Patty Davis, a program manager for trauma-informed care at Children’s Mercy hospital in Kansas City, said even her clients who were at the parade but were not injured still flinch at the sounds of sirens or other loud noises. It’s a powerful response to gun violence, she said.
“So not just an accidental trauma,” she said, “but a trauma that was perpetrated for violent purposes, which can cause an increased level of anxiety for persons around that to wonder if it’s going to happen again. And how safe are they?”
Reliving Getting Shot
Random sounds, bright lights, and crowds can catch the kids and their parents off guard. In June, Mireya Nelson was waiting for her older sister after a dance recital, hoping to see a boy she knew give a flower to a girl everyone said he had a crush on. Her mom wanted to go, but Mireya shushed her.
“Then all of a sudden, there was a loud boom,” Erika said. “She dropped low to the ground. And then she jumped back up. She goes, ‘Oh my God, I was getting shot again!’”
Mireya said it so loudly people were staring, so it was Erika’s turn to shush her and try to soothe her.
“I was like, ‘Mireya, it’s OK. You’re all right. They dropped a table. They’re just moving stuff out. It was an accident,’” Erika said.
It took a few minutes for the shock to wear off and Mireya later giggled about it, but Erika is always on watch.
Her daughter’s early sadness — she watched movies for hours, crying throughout — has since changed to a cheekiness. Half a year later, Mireya will joke about the shooting, which tears her mother up. But maybe that is part of the healing process, Erika says.
Before the Fourth of July, Mireya went to Worlds of Fun, a large amusement park, and had a good time. She felt OK because there were security guards everywhere. She also enjoyed a visit to the local FBI office with a friend who was with her the day of the shooting. But when someone suggested a trip to the ballet, Mireya squashed it quickly — it’s near Union Station, the site of the shooting. She doesn’t want to go downtown anymore.
Erika said the doctor appointments and financial strains have been a lot to juggle and that her biggest frustration as a parent is that she’s not able to fix things for her daughter.
“They have to go their own way, their own process of healing. I can’t shake her, like, ‘Get back to yourself,’” Erika said. “It could take months, years. Who knows? It could be the rest of her life. But I hope that she can overcome a little bit of it.”
Goose Bumps in the Sweltering Heat
James Lemons noticed a change in his 5-year-old daughter, Kensley, who was on his shoulders when he was shot at the parade. Before the shooting Kensley was outgoing and engaged, James said, but now she is withdrawn, like she has closed off her bubble and disconnected from people.
Large crowds and police officers remind Kensley of the parade. Both were present at a high school graduation the family attended this summer, prompting Kensley to ask repeatedly to leave. James took her to an empty football field, where, he said, she broke out in goose bumps and complained of being cold despite the sweltering heat.
Bedtime is a particular problem for the Lemons family. Kensley has been sleeping with her parents. Another child, 10-year-old Jaxson, has had bad dreams. One night, he dreamt that the shooter was coming near his dad and he tripped him, said Brandie Lemons, Jaxson’s stepmom.
Younger children like Kensley exposed to gun violence are more likely to develop post-traumatic stress disorder than older children, according to Ohio State’s Johnson-Motoyama.
Davis, of Children’s Mercy in Kansas City, said children whose brains are not fully developed can have a hard time sleeping and understanding that they are safe in their homes at night.
James got the family a new puppy — an American bulldog that already weighs 32 pounds — to help them feel protected.
“I looked up the pedigree,” he said, “They’re real protective. They’re real loving.”
Searching for an Outlet to Let Off Steam
Gabriella took up boxing after the shooting. Her mother, Bridget, said it restored some of her confidence and control that dimmed after the parade.
“I like beating people up — not in a mean way, I swear,” Gabriella said in April as she molded a mouthguard to her teeth before leaving for training.
She has since stopped boxing, however, so the money can instead go toward a trip to Puerto Rico with her Spanish class. They’re paying $153 a month for 21 months to cover the trip. Boxing classes were $60 a month.
Bridget thought boxing was a good outlet for leftover anger, but by the end of July Gabriella wasn’t sure if she still had the drive to fight back that way.
“The past is the past but we’re still gonna all, like, go through stuff. Does that make sense?” Gabriella asked.
“You’re mostly OK but you still have triggers. Is that what you mean?” her mother asked.
“Yeah,” she replied.
After the shooting, Mireya Nelson tried online classes, which didn’t work well. The first few days of summer school, Mireya had a panic attack every day in the car and her mother took her home.
Mireya wants to return to high school this fall, and Erika is wary.
“You know, if I do go back to school, there’s a chance at school of being shot, because most schools nowadays get shot up,” Erika recalled her daughter saying. “And I’m like, ‘Well, we can’t think like that. You never know what’s gonna happen.’”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
10 months 2 days ago
Mental Health, Multimedia, Public Health, States, Audio, Children's Health, Guns, Investigation, Kansas, Missouri, The Injured
KFF Health News' 'What the Health?': SCOTUS Ruling Strips Power From Federal Health Agencies
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
In what will certainly be remembered as a landmark decision, the Supreme Court’s conservative majority this week overruled a 40-year-old legal precedent that required judges in most cases to yield to the expertise of federal agencies. It is unclear how the elimination of what’s known as the “Chevron deference” will affect the day-to-day business of the federal government, but the decision is already sending shockwaves through the policymaking community. Administrative experts say it will dramatically change the way key health agencies, such as the FDA and the Centers for Medicare & Medicaid Services, do business.
The Supreme Court also this week decided not to decide a case out of Idaho that centered on whether a federal health law that requires hospitals to provide emergency care overrides the state’s near-total ban on abortion.
This week’s panelists are Julie Rovner of KFF Health News, Joanne Kenen of the Johns Hopkins schools of public health and nursing and Politico Magazine, Victoria Knight of Axios, and Alice Miranda Ollstein of Politico.
Panelists
Joanne Kenen
Johns Hopkins University and Politico
Victoria Knight
Axios
Alice Miranda Ollstein
Politico
Among the takeaways from this week’s episode:
- In 1984, the Supreme Court ruled broadly that courts should defer to the decision-making of federal agencies when an ambiguous law is challenged. On Friday, the Supreme Court ruled that the courts, not federal agencies, should have the final say. The ruling will make it more difficult to implement federal laws — and draws attention to the fact that Congress, frequently and pointedly, leaves federal agencies much of the job of turning written laws into reality.
- That was hardly the only Supreme Court decision with major health implications this week: On Thursday, the court temporarily restored access to emergency abortions in Idaho. But as with its abortion-pill decision, it ruled on a technicality, with other, similar cases in the wings — like one challenging Texas’ abortion ban.
- In separate rulings, the court struck down a major opioid settlement agreement, and it effectively allowed the federal government to petition social media companies to remove falsehoods. Plus, the court agreed to hear a case next term on transgender health care for minors.
- The first general-election debate of the 2024 presidential cycle left abortion activists frustrated with their standard-bearers — on both sides of the aisle. Opponents didn’t like that former President Donald Trump doubled down on his stance that abortion should be left to the states. And abortion rights supporters felt President Joe Biden failed to forcefully rebut Trump’s outlandish falsehoods about abortion — and also failed to take a strong enough position on abortion rights himself.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: The Washington Post’s “Masks Are Going From Mandated to Criminalized in Some States,” by Fenit Nirappil.
Victoria Knight: The New York Times’ “The Opaque Industry Secretly Inflating Prices for Prescription Drugs,” by Rebecca Robbins and Reed Abelson.
Joanne Kenen: The Washington Post’s “Social Security To Drop Obsolete Jobs Used To Deny Disability Benefits,” by Lisa Rein.
Alice Miranda Ollstein: Politico’s “Opioid Deaths Rose 50 Percent During the Pandemic. in These Places, They Fell,” by Ruth Reader.
Also mentioned in this week’s podcast:
- Politico’s “Inside the $100 Million Plan To Restore Abortion Rights in America,” by Alice Miranda Ollstein.
- JAMA Network Open’s “Use of Oral and Emergency Contraceptives After the US Supreme Court’s Dobbs Decision,” by Dima M. Qato, Rebecca Myerson, Andrew Shooshtari, et al.
- JAMA Health Forum’s “Changes in Permanent Contraception Procedures Among Young Adults Following the Dobbs Decision,” by Jacqueline E. Ellison, Brittany L. Brown-Podgorski, and Jake R. Morgan.
- JAMA Pediatrics’ “Infant Deaths After Texas’ 2021 Ban on Abortion in Early Pregnancy,” by Alison Gemmill, Claire E. Margerison, Elizabeth A. Stuart, et al.
click to open the transcript
SCOTUS Ruling Strips Power From Federal Health Agencies
KFF Health News’ ‘What the Health?’Episode Title: ‘SCOTUS Ruling Strips Power From Federal Health Agencies’Episode Number: 353Published: June 28, 2024
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Mila Atmos: The future of America is in your hands. This is not a movie trailer, and it’s not a political ad, but it is a call to action. I’m Mila Atmos and I’m passionate about unlocking the power of everyday citizens. On our podcast, “Future Hindsight,” we take big ideas about civic life and democracy and turn them into action items for you and me. Every Thursday, we talk to bold activists and civic innovators to help you understand your power and your power to change the status quo. Find us at futurehindsight.com or wherever you listen to podcasts.
Julie Rovner: Hello, and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News, and I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Friday, June 28, at 10:30 a.m. As always, news happens fast and things might’ve changed by the time you hear this, so here we go.
We are joined today via video conference by Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Hello.
Rovner: Victoria Knight of Axios News.
Victoria Knight: Hello, everyone.
Rovner: And Joanne Kenen of the Johns Hopkins Schools of Nursing and Public Health and Politico Magazine.
Joanne Kenen: Hi, everybody.
Rovner: I hope you enjoyed last week’s episode from Aspen Ideas: Health. This week we’re back in Washington with tons of breaking news, so let’s get right to it. We’re going to start at the Supreme Court, which is nearing, but not actually at, the end of its term, which we now know will stretch into next week. We have breaking news, literally breaking as in just the last few minutes: The court has indeed overruled the Chevron Doctrine. That’s a 1984 ruling that basically allowed experts at federal agencies to, you know, expert. Now it says that the court will get to decide what Congress meant when it wrote a law. We’re obviously going to hear a lot more about this ruling in the hours and days to come, but does somebody have a really quick impression of what this could mean?
Ollstein: So this could prevent or make it harder for health agencies, and all the federal agencies that touch on health care, to both create new policies based on laws that Congress pass and update old ones. Things need to be updated; new drugs are invented. There’s been all these updates to what Obamacare does and doesn’t have to cover. That could be a lot harder going forward based on this decision. It really takes away a lot of the leeway federal agencies had to interpret the laws that Congress passed and implement them.
I think kicking things back to courts and Congress could really slow things down a lot, and a lot of conservatives see that as a good thing. They think that federal agencies have been too untouchable and not have the same accountability mechanisms because they’re career civil servants who are not elected. But this has health policy experts … Honestly, we interviewed members of previous Republican administrations and Democratic administrations and they’re both worried about this.
Rovner: Yeah, going forward, if Donald Trump gets back into the presidency, this could also hinder the ability of his Department of Health and Human Services to make changes administratively.
Knight: These agencies are stacked with experts. This is what they work on. This is what they really are primed to do. And Congress does not have that same type of staffing. Congress is very different. It’s very young. There’s a lot of turnover. There are experienced staffers, but usually when they’re writing these laws, they leave so much up to interpretation of the agency because they are experts.
So I think pushing things back on Congress would really have to change how Congress works right now. When I talked to experts, we would need staffers who are way more experienced. We would need them to write laws that are way more specific. And Congress is already so slow doing anything. This would slow things down even more. So that’s a really important congressional aspect I think to note.
Rovner: I think when we look back at this term, this is probably going to be the biggest decision. Joanne, you want to add something before we move on?
Kenen: We’re recording. We don’t know if immunity just dropped, which is all still going to be, not a health care decision but an important decision of the country. I’ve got SCOTUSblog on my other screen. Here’s a quote from [Justice Elena] Kagan’s dissent. She says, because it’s very unfocused for what we do on this podcast, “Chevron has become part of the warp and woof of modern government, supporting regulatory efforts of all kinds, to name a few, keeping air and water clean, food and drugs safe and financial markets honest.” So two of the three of us. Financial markets affect the health industry as well.
Rovner: Oh, yeah.
Kenen: But I think that what the public doesn’t always understand is how much regulatory stuff there is in Washington. Congress can write a 1,000-page law like the ACA [Affordable Care Act]. I’ve never counted how many pages of regulation because I don’t think I can count that high. It’s probably tens of thousands.
Rovner: At least hundreds of thousands.
Kenen: Right. And that every one of those, there’s a lobbying fight and often a legal fight. It’s like the coloring book when we were kids. Congress drew the outline and then we all tried to scribble within the lines. And when you go out of the lines, you have a legal case. So the amount of stuff, regulatory activity is something that the public doesn’t really see. None of us have read every reg pertaining to health care. You can’t possibly do it in a lifetime. Methuselah couldn’t have done it. And Congress cannot hire all the expert staff and all the federal agencies and put them in; they won’t fit in the Capitol. That’s not going to happen. So how do they come to grips with how specific are they going to have to be? What kind of legal language can they delegate some of this to agency experts. We’re in really uncharted territory.
Rovner: I think you can tell from the tones of all of our voices that this is a very big deal, with a whole lot of blanks to be filled in. But for the moment …
Kenen: Maybe they’ll just let AI do it.
Rovner: Yeah, for the moment, let’s move on because, until just now, the biggest story of the week for us was on Thursday. We finally got a decision in that case about whether Idaho’s near-total ban on abortion can override a federal law called EMTALA, the Emergency Medical Treatment and Active Labor Act, which requires doctors in emergency rooms to protect a pregnant woman’s health, not just her life. And much like the decision earlier this month to send the abortion pill case back to the lower courts because the plaintiffs lacked legal standing, the court once again didn’t reach the merits here. So Alice, what did they do?
Ollstein: So like you said, both on abortion pills and on EMTALA, the court punted on procedural issues. So it was standing on the one and it was ripeness on the other one. This one was a lot more surprising. I think based on the oral arguments in the mifepristone case, we could see the standing-based decision coming. That was a big focus of the arguments. This was more of a surprise. This was a majority of justices saying, “Whoops, we shouldn’t have taken this case in the first place. We shouldn’t have swooped in before the 9th Circuit even had a chance to hear it. And not only take the case, but allow Idaho to fully enforce its law even in ways that people feel violate EMTALA in the meantime.” And so what this does temporarily is restore emergency abortion access in Idaho. It restores a lower-court order that made that the case, but it’s not over.
Rovner: Right. It had stayed Idaho’s ban to the extent that it conflicted with EMTALA.
Ollstein: So this goes back to lower courts and it’s almost certain to come back to the Supreme Court as early as next year, if not at another time. Because this isn’t even the only major federal EMTALA case that’s in the works right now. There’s also a case on Texas’ abortion ban and its enforcement in emergency situations like this. And so I think the main reaction from the abortion rights movement was temporary relief, but a lot of fear for the future.
Rovner: And I saw a lot of people reminding everybody that this Texas ruling in Idaho, now the federal law is taking precedence, but there’s a stay of the federal law in the 5th Circuit. So in Texas, the Texas ban does overrule the federal law that requires abortions in emergency circumstances to protect a woman’s health. That’s what the dispute is basically about. And of course, you see a lot of legal experts saying, “This is a constitutional law 101 case that federal law overrides state law,” and yet we could tell by some of the add-on discussion in this case, as they’re sending it back to the lower court, that some of the conservatives are ready to say, “We don’t think so. Maybe the federal law will have to yield to some of these state bans.” So you can kind of see the writing on the wall here?
Ollstein: It’s really hard to say. I think that you have some justices who are clearly ready to say that states can fully enforce their abortion bans regardless of what the federal government’s federal protections are for patients. I think they put that out there. I think the case is almost certain to come back to them, and there was clearly not a majority ready to fully side with the Biden administration on this one.
Rovner: And clearly not a majority ready to fully side with Idaho on this one. I think everything that I saw suggested that they were split 3-3-3. And with no majority, the path of least resistance was to say, “Our bad. You take this back lower court. We’ll see when it comes back.”
Ollstein: It was a very unusual move, but some of the justification made sense to me in that they cited that Idaho state officials’ position on what their abortion ban did and didn’t do has wavered over time and changed. And what they initially said when they petitioned to the court is not necessarily exactly what they said in oral arguments, and it’s not exactly what they have said since. And so at the heart here is you have some people saying there’s a clear conflict between the patient protections under EMTALA — which says you have to stabilize anyone that comes to you at a hospital that takes Medicare — and these abortion bans, which only allow an abortion when there’s imminent life-threatening situation. And so you have people, including the attorney general of Idaho, saying, “There is no conflict. Our law does allow these emergency abortions and the doctors are just wrong and it’s just propaganda trying to smear us. And they just want to turn hospitals into free-for-all abortion facilities.” This is what they’re arguing. And then you have people say …
Rovner: [inaudible 00:11:12] … in the meanwhile, we know that women are being airlifted out of Idaho when they need emergency abortions because doctors are worried about actually performing abortions …
Ollstein: Correct.
Rovner: And possibly being charged with criminal charges for violating Idaho’s abortion ban.
Ollstein: Sure, but I’m saying even amongst conservatives, there are those who are saying, “There’s no conflict between these two policies. The doctors are just wrong either intentionally or unintentionally.” And then there’s those who say there is a conflict between EMTALA and state bans, and it should be fine for the state to violate EMTALA.
Rovner: No. Obviously this one will continue as the abortion pill case is likely to continue. Well, also in this end-of-term Supreme Court decision dump, an oddly split court with liberals and conservatives on both sides, struck down the bankruptcy deal reached with Purdue Pharma that would’ve paid states and families of opioid overdose victims around $6 billion, but would also have shielded the company’s owners, the Sackler family, from further legal liability. What are we to make of this? This was clearly a difficult issue. There were a lot of people even who were involved in this settlement who said the idea of letting the Sackler family, which has hidden billions of dollars from the bankruptcy settlement anyway, and clearly acted very badly, basically giving them immunity in exchange for actually getting money. This could not have been an easy… obviously was not an easy decision even for the Supreme Court.
Kenen: No, it wasn’t theoretical. The ones who opposed blowing up the agreement were very much, “This is going to add delay any kind of justice for the families and the plaintiffs.” It was not at all abstract. It was like there are a lot of people who aren’t going to get help. At least the help will be delayed if this money doesn’t start flowing. So I was struck by how practical, relating to the families who have lost people because of the actions of Purdue. But the other side was, also that was much more a clear-cut legal issue, that people didn’t give up their right to sue. It was cutting off the right to sue was imposed on potential plaintiffs by the settlement. So that was a much more legalistic argument versus, it was a little bit more real world, but they need the help now. And including some of the conservatives. This is an interesting thing to read. This was painstaking. This is a huge settlement. It took so long. It had many, many moving parts. And I don’t know how you go back and put it together again.
Rovner: But that’s where we are.
Kenen: Yes.
Rovner: They have to basically start from scratch?
Kenen: I don’t know if they have to start entirely from scratch. You’d have to be nuts to get the Sacklers to say, “OK, we’ll be sued,” which they’re obviously you’re not going to. Is somebody going to come up with a “Split the difference, let’s get this moving and we won’t sue anymore?” I don’t know. But I don’t know that you have to start 100% from scratch, but you’re surely not anywhere near a finish line anymore.
Rovner: That’s big Supreme Court case No. 3 for this week. Now let’s get to big Supreme Court case No. 4. Earlier this week, the court turned back a challenge that the government had wrongly interfered with free speech by urging social media organizations to take down covid misinformation. But again, as with the abortion pill case, the court did not get to the merits. But instead, they ruled that the states and individuals who sued did not have standing. So we still don’t know what the court thinks of the role of government in trying to ensure that health information is correct. Right?
Knight: Right. And I thought it was interesting. Basically the White House was like, “Well, we talked to the tech companies, but it was their decision to do this. So we weren’t really mandating them do this.” I think they’re just being like, “OK, we’ve left it up to the tech companies. We haven’t really interfered. We’re just trying to say these things are harmful.” So I guess we’ll have to see. Like you said, they didn’t take it up on standing, but overall, conservatives that were saying, “This was infringing on free speech.” It was particularly some scientists, I think, that promoted the herd immunity theory, things like that.
So I think they’re obviously going to be upset in some way because their posts were depromoted on social media. But I think it just leaves things the way they are, the same way. But it would be interesting, I guess, if Trump does go to the White House, how that might play out differently?
Rovner: This court has been a lot of the court deciding not to decide cases, or not to decide issues. Sorry, Alice, go ahead.
Ollstein: Yeah, so I think it is pretty similar to the abortion pill case in one key way, which is that it’s the court saying, “Look, the connection between the harm you think you suffered and the entity you are accusing of causing that suffering, that connection is way too tenuous. You can’t prove that the Biden administration voicing concerns to these social media companies directly led to you getting shadow-banned or actual banned,” or whatever it is. And the same in the abortion pill case, the connection between the FDA [Food and Drug Administration] approving the drug and regulating the drug and these individual doctors’ experiences is way too tenuous. And so that’s something to keep in mind for future cases that, we’re seeing a pattern here.
Rovner: Yes, and I’m not suggesting that the court is directly trying to duck these issues. These are legitimate standing cases and important legal precedents for who can sue in what circumstance. That is the requirement of constitutional review that first you have to make sure that there’s both standing in a live controversy and there’s all kinds of things that the court has to go through before they get to the merits. So more often than not, they don’t get there.
Well, meanwhile, we have our first hot-button, Supreme Court case slotted in for next term. On Monday, the court granted “certiorari” [writ by which a higher court reviews a decision of a lower court] to a case out of Tennessee where the Biden administration is challenging the state’s ban on transgender care for minors. It was inevitable that one of these cases was going to get to the high court sooner or later, right?
Kenen: Yeah, I think it’s not a surprise, the politics of it and the techniques or tools used by the forces that are against the treatment for minors. It’s very similar to the politics and patterns of the abortion case, of turning something into an argument that it’s to protect somebody. A lot of the abortion requirements and fights were about to protect the woman. Ostensibly, that was the political argument. And now we’re seeing we have to protect the children so that it’s the courts, as opposed to families and doctors, who are, “protecting the children.”
There’s a lot of misunderstanding about what these treatments do and who gets them and at what age; that they’re often described as mutilation and irreversible. For the younger kids, for preteen, middle school age-ish, early teens, nothing is irreversible. It’s drugs that if you stop them, the impact goes away. But it has become this enormous lightning rod for the intersection of health and politics. And I think we all have a pretty good guess as to where the Supreme Court’s going to end up on this. But you’re sometimes surprised. And also, there could be some …
Rovner: Maybe they don’t have standing.
Kenen: There could be some kind of moderation, too. It could be a certain … they don’t have to say all … it depends on how clinical they want to get. Maybe they’ll rule on certain treatments that are more less-reversible than a puberty blocker, which is very reversible, and some kind of safeguards. We don’t know the details. We’re not surprised that it ended up … and we know going in, you could have a gut feeling of where it’s likely to turn out without knowing the full parameters and caveats and details. They haven’t even argued it yet.
Rovner: This is a decision that we’ll be waiting for next June.
Kenen: Right. Well, could not. Maybe it’s so clear-cut, it’ll be May. Who knows, right?
Rovner: Yeah, exactly. All right, well, moving on. There was a presidential debate last night. I think it was fair to say that it didn’t go very well for either candidate, nor for anybody interested in what President Biden or former President Trump thinks about health issues. What did we learn, if anything?
Ollstein: Well, I was mainly listening for a discussion of abortion and, boy was it all over the place. What I thought was interesting was that both candidates pissed off their activist supporters with what they said. I was texting with a lot of folks on both sides and conservatives were upset that Trump doubled down on his position that this should be entirely left to states, and they disagree. They want him to push for federal restrictions if elected.
And on the left, there was a lot of consternation about Biden’s weird, meandering answer about Roe v. Wade. He was asked about abortions later in pregnancy. One, neither he nor the moderators pushed back on what Trump’s very inflammatory claims about babies being murdered and stuff. There was no fact-checking of that whatsoever. But then Biden gave a confusing answer, basically saying he supports going to the Roe standard but not further, which is what I took out of it. And that upset a lot of progressives who say Roe was never good enough. For a lot of people, when Roe v. Wade was still in place, abortion was a right in name only. It was not actually accessible. States could impose lots of restrictions that kept it out of reach for a lot of people. And in this moment, why should we go back to a standard that was never good enough? We should go further. So just a lot of anxiety on both sides of this.
Rovner: Yeah. Meanwhile, Trump seemed to say that he would leave the abortion pill alone, which jumped out at me.
Kenen: But that was a completely … CNN made a decision not to push back. They were going to have online fact-checking. Everybody else had online fact. … And they didn’t challenge. And I guess they assumed that the candidates would challenge each other, and Biden had a different kind of challenging night. Trump actually said that the previous Supreme Court had upheld the use of the abortion drug and that it’s over, it’s done. That was not a true statement. The Supreme Court rejected that case, as Alice just explained, on standing. It’s going to be back. It may be back in multiple forms, multiple times. It is not decided. It is not over, which is what Trump said, “Oh, don’t worry about the abortion drug. The Supreme Court OK’d it.” That’s not what the Supreme Court did, and Biden didn’t counter that in any way.
And then Biden, in addition to the political aspect that Alice just talked about, he also didn’t describe Roe, the framework of Roe, particularly accurately. And, as Alice just pointed out, the things that Trump said were over-the-top even for Trump, and that they went unchallenged by either the moderators or President Biden.
Rovner: I was a little bit surprised that there wasn’t anything else on health care or there wasn’t much else.
Knight: Biden tried to hit his health care talking points and did a very terrible job. Alice had a really good tweet getting the right. … He initially said wrong numbers for the insulin cap, for the cap on out-of-pocket for Medicare beneficiaries, how much they can spend on prescription drugs. He got both of those wrong. I think he got insulin right later in the night. And then the very notably, “We will beat Medicare.” That was just unclear what he even meant by that. Maybe it was about drug price negotiations, I’m sure. So he was trying, but just could not get the facts right and I don’t think it came across effective in any way. And health care does do really well for Democrats. Abortion does really well for Democrats. So he was not effective in putting those messages.
I also noticed the moderators asked a question about opioids, addressing the opioid epidemic. Trump did not answer at all, pivoted to I think border or something like that. I don’t think Biden really answered either, honestly. So that was an opportunity for them to also talk about addressing that, which I think is something they could both probably talk about in a winning way for both. But I thought it was mentioned more than I expected a little bit. I thought they may want to talk about it at all. So it was still not much substantive policy discussion on health care.
Kenen: Biden tried to get across some of the Democratic policies on drug prices and polls have shown that the public doesn’t really understand that is actually the law in going forward. So if any attempt to message that in front of a very large audience was completely muddled. Nobody listening to that debate would’ve come out — unless they knew going in — they would’ve not have come out knowing what was in the law about Medicare price negotiations. They would’ve gotten four different answers of what happened with insulin, although they probably figured something good, helpful happened. And a big opportunity to push a Democratic achievement that has some bipartisan popularity was completely evaporated.
Rovner: I think Biden did the classic over-prepare and stuff too many talking points into his head and then couldn’t sort them all out in the moment. That seemed pretty clear. He was trying to retrieve the talking point and they got a little bit jumbled in his attempt to bring them out. Well, back to abortion: Alice, you got a cool scoop this week about abortion rights groups banding together with a $100 million campaign to overturn the overturn of Roe. Tell us about that?
Ollstein: Yeah, so it’s notable because there’s been so much focus on the state level battles and fighting this out state by state, and the ballot initiatives that have passed at the state level and restored or protected access have been this glimmer of hope for the abortion rights movement. But I think there was a real crystallization of the understanding that that strategy alone would leave tens of millions of people out in the cold because a lot of states don’t have the ability to do a ballot initiative. And also, if there were to be some sort of federal restrictions imposed under a Trump presidency or whatever, those state level protections wouldn’t necessarily hold. So I think this effort of groups coming together to really spend big and say that they want to restore federal protections is really notable.
I also think it’s notable that they are not committing to a specific bill or plan or law they want to see. They are keeping on the, “This is our vision, this is our broad goal.” But they’re not saying, “We want to restore Roe specifically, we want to go further,” et cetera. And that’s creating some consternation within the movement. I’ve also, since publishing the story, heard a lot of anxiety about the level of spending going to this when people feel that that should be going to direct support for people who are suffering on the ground and struggling to access abortion. Right now you have abortion funds screaming that they’re being stretched to the breaking point and cannot help everyone who needs to travel out of state right now. So, of course, infighting on the left is a perennial, but I think it’s particularly interesting in this case.
Rovner: Well, meanwhile, we have a trio this week of examples of what I think it’s safe to call unintended consequences of the Supreme Court’s overturn of Roe. First, a study in the medical journal JAMA Pediatrics this week, found that in the first year abortion was dramatically restricted in Texas — remember, that was before the overturn of Roe — infant deaths rose fairly dramatically. In particular, deaths from congenital problems rose, suggesting that women carrying doomed fetuses gave birth instead of having abortions. What’s the takeaway from seeing this big spike in infant mortality?
Ollstein: So I’ve seen a lot of anti-abortion groups trying to spin this and push back really hard on it. Specifically picking up on what you just said, which is that a lot of these are fatal fetal anomalies. And so they were saying, “Were abortion still legal, those pregnancies could have been terminated before birth.” And so they’re saying, “There’s no difference really, because we consider that an infant death already. So now it’s an infant death after birth. Nothing to see here.”
Rovner: When everybody has suffered more, basically.
Ollstein: Yeah, that is the response I’m seeing on the right. On the left, I am seeing arguments that anyone who labels themselves pro-life should think twice about the impact of these policies that are playing out. And like you said, we’re only just beginning to get glimmers of this data. In part because Texas was out in front of everybody else, and so I think there’s a lot more to come.
The other pushback I’ve seen from anti-abortion groups is that infant mortality also rose in states where abortion remains legal. So I think that’s worth exploring, too. Obviously, correlation is not always causation, but I think it’s hard when you’re getting the data in little dribs and drabs instead of a full complete picture that we can really analyze.
Rovner: Well, in another JAMA study, this one in JAMA Network Open, they found that the use of Plan B, the morning-after birth control pill, fell by 60% in states that implemented abortion bans after the Dobbs [v. Jackson Women’s Health Organization] decision. Now, for the millionth time, Plan B is not the same as the abortion pill. It’s a high-dose contraceptive. But apparently, a combination of the closure of family planning clinics in states that impose bans, which are an important source of pills for people with low incomes who can’t afford over-the-counter versions, and misinformation about the continuing legality of the morning-after pill, which continues to be legal, contributed to the decline. At least that’s what the authors theorize. This is one of many ironies in the wake of Dobbs; that states with abortion bans may well be ending up with more unintended pregnancies rather than fewer.
Ollstein: Well, one trends that could be feeding this is that some of the clinics where people used to go to to access contraception, also provided abortion and have not been able to keep their doors open in a post-Roe environment. We’ve seen clinics shutting down across the South. I went to Alabama last year to cover this, and there are clinics there that used to get most of their revenue from abortion, and they’re trying to hang on and provide nonabortion gynecological services, including contraception, and the math just ain’t mathing, and they’re really struggling to survive.
And so this goes back to the finger-pointing within the movement about where money should be going right now. And I know that red state clinics that are trying to survive feel very left behind and feel that this erosion of access is a result of that.
Kenen: Julie, and also to put in, even before Dobbs, it was not easy in many parts of the country for low-income women to get free contraception. There are states in which clinics were few and far between. Federal spending on Title X has not risen in many years.
Rovner: Title X is a federal [indecipherable].
Kenen: Right. Alice knows this, and maybe I’ve said on the podcast, I once just pretty randomly with me and my cursor plunked my cursor down on a map of Texas and said, “OK, if I live here, how far is the nearest clinic?” And I looked at the map of the clinics and it was far, it was something like 95 miles, the nearest one. So we had abortion deserts. We’ve also had family planning deserts, and that has only gotten worse, but it wasn’t good in the first place.
Rovner: Well, finally, and for those who really want to make sure they don’t have unintended pregnancies, according to a study in a third AMA journal, JAMA Health Forum, the number of young women aged 18 to 30 who were getting sterilized doubled in the 15 months after Roe was overturned. Men are part of this trend, too. Vasectomies tripled over that same period. Are we looking at a generation that’s so scared, they’re going to end up just not having kids at all?
Kenen: Well, there are a lot of kids in this generation who are saying they don’t want to have kids for a variety of reasons: economic, climate, all sorts of things. I think that I was a little surprised to see that study because there are safe long-acting contraceptives. You can get an IUD that lasts seven to nine years, I think it is. I was a little surprised that people were choosing something irreversible because.. I do know young people who… You’re young, you go through lots of changes in life, and there is an alternative that’s multiyear. So I was a little surprised by that. But that’s apparently what’s happening. And it’s for… This generation is not as… What are they, Gen[eration] Z? They’re not as baby-oriented as their older brothers and sisters even.
Knight: Well, that age range is millennial and Gen Z. But I don’t know. I’m a millennial. I think a lot of my friends were not baby-oriented. So I think that’s probably a fair statement to say. But it is interesting that they wouldn’t choose an IUD or something like that instead. But I do think people are scared. We’ve seen the stories of people moving out of states that have really strict abortion bans because they are so concerned on what kind of medical care they could have, even if they think they want to get pregnant. And sometimes you don’t have a healthy pregnancy and then need to get an abortion. So I’m sure it has something to do with that but…
Rovner: Yeah, it’s one of those trends to keep an eye out for. Well, moving on, U.S. Surgeon General Vivek Murthy has been busy these past couple of weeks. First, he published an op-ed in The New York Times calling for a warning label for social media that’s similar to the one that’s already on tobacco products, warning that social media has not been proven safe for children and teenagers. Of course, he doesn’t have his own authority to do that. Congress would have to pass a law. Any chance of that? I know Congress is definitely into the “What are we going to do about social media” realm.
Kenen: But talking about it and doing something or thinking, it’s a long way. Is this as, compared to his other topic of the week, which was gun safety? He’s got a lot more bipartisan …
Rovner: We’re getting to that.
Kenen: … He’s got a lot more bipartisan support for the concern about health of young people and what social media is. What is social media? Social media is mixed. There are good things and bad things, and what is that balance? There is a bipartisan concern. I don’t know that that means you get to the labeling point. But the labeling point is one thing. That the larger concept of concern about it, and recognition about it, and what do we do about it, is bipartisan up to a point. How do you even label? What do you label? Your phone? Your computer? I’m not sure where the label goes. Your eyelids? [inaudible 00:33:07]
Knight: Right. Well, tech bills in Congress in general are like… Even though TikTok was surprisingly able to get done in the House. But TikTok lobby was big. But there would be a big social media lobby, I’m sure, against that. I guess there is bipartisan support. I don’t know. It’s not something I’ve asked members about, but I think that would be pretty far off from a reality actually happening.
Rovner: Well, also this week, as Joanne mentioned, the surgeon general issued a Surgeon General’s Advisory, declaring gun violence a public health crisis, calling for more research funding on gun injuries and deaths, universal background checks for gun buyers, and bans on assault weapons and high-capacity ammunition magazines. I feel like the NRA [National Rifle Association] has lost some of its legendary clout on Capitol Hill over the past few years, thanks to a series of scandals, but maybe not enough for some of these things. I feel like I’ve heard these suggestions before, like over the last 25 or 30 years.
Kenen: I think one of the interesting things about Vivek Murthy is he came to public prominence on gun safety and guns in public health before people were really talking about guns in public health. I forgot what year it was — 2016, 2017, whenever Obama first nominated him. Because remember, this is his second run as surgeon general. It was an issue that he had spoken about and had made a signature issue, and as he became a more public figure before the nomination. And then he went silent on it. He had trouble getting confirmed. He didn’t do anything about it. We never really heard … as far as I can recollect, we never even heard him talk about it once. Maybe there was a phrase or two here or there. He certainly didn’t push it or make it a signature issue.
Right now, he’s at the end of the last year with the Biden administration. Some kind of arc is being completed. He’s a young man, there’ll be other arcs. But this arc is winding down and the president cares about gun violence. Congress actually did, not the full agenda, but they did something on it, which was unusual. And I think that this is his chance to use his bully pulpit while he still has it in this particular perch to remind people that we do have tools. We don’t have all the solutions to gun violence. We do not understand everything about it. We do not understand why some people go and shoot a movie theater or a school or a supermarket or whatever, and there are multiple reasons. There are different kinds of mass killers. But we do know that there are some public health tools that do work. That red flag laws do seem to help. That safe gun storage … There are things that are less controversial than a spectrum of things one can do.
Some of them have broader support, and I think he is using this time — not that he expects any of these things to become law in the final year of the Biden administration — but I think he’s using it. This is bully pulpit. This is saying, “Moving forward, let’s think about what we can come to agreement on and do what we can on certain evidence-based things.” Because there’s been a lot of work in the last decade or so on the public health, not just the criminal… Obviously, it’s a legal and criminal justice issue. It’s also a public health issue, and what are the public health tools? What can we do? How do we treat this as basically an epidemic? And how can we stop it?
Rovner: Finally this week, since we didn’t really do news last week, there have been a couple of notable stories we really ought to mention. One is a court case, Braidwood v. Becerra. This is the case where a group of Christian businesses are claiming that the Affordable Care Act’s preventive services provisions that require them to provide no cost-sharing access to products, including HIV preventive medication, violates their freedom of religion because it makes them complicit in homosexual behavior. Judge Reed O’Connor, district court judge — if that name is familiar, it’s because he’s the Texas judge who tried to strike down the entire ACA back in 2018. Judge O’Connor not only found for the plaintiffs, he tried to slap a nationwide injunction on all of the ACA’s preventive services, which even the very conservative 5th Circuit appeals court struck down. But meanwhile, the appeals court has come up with its ruling. Where does that leave us on the ACA preventive services?
Ollstein: It leaves us right where we were when the 5th Circuit took the case because they said that, “We’re going to allow the lower court ruling to be enforced just for the plaintiffs in the meantime, but we’re not going to allow the entire country’s preventive care coverage to be disrupted while this case moves forward.” And so that basically continues to be the case. Some of the arguments are getting sent back down to the lower court for further consideration. And we still don’t know whether either side will appeal the 5th Circuit’s ruling to the Supreme Court.
Rovner: But notably, the appeals court said that U.S. Preventive Services Task Force, which is appointed by the Department of Health and Human Services, is basically illegally constituted because it should be nominated by the president, approved by the Senate, which it is not. That could in the long run be kind of a big deal. This is a group of experts that supposedly shielded from politics.
Kenen: Yeah, I don’t think this story is over either. It is for now. Right now we’re at the status quo, except for this handful of people who brought recommendations on all sorts of health measures, including vaccination and cancer screenings and everything else. They stand. They’re not being contested at this moment. How that will evolve under the next administration and this court remains to be seen.
Rovner: Finally, finally, finally, to end on a bit of a frustrating note, the National Academies of Sciences, Engineering, and Medicine, has found that two decades after it first called out some of the most egregious inequities in U.S. health care, not that much has changed. Joanne, this has been a very high-profile issue. What went wrong?
Kenen: Well, I think this report got very little attention probably because it’s like, oh, reports aren’t necessarily news stories. And it was like nothing changed, so why do we report it? But I think when I read the report — and I did not get through all 375 pages yet, but I did read a significant amount of it and I listened to a webinar on it — I think what really struck me is how we’re not any better than we really were 20 years ago. And what really was jarring is the report said, “And we actually know how to fix this and we’re not doing it. And we have the scientific and public health and sociological knowledge. We know if we wanted to fix it, we could, and we haven’t. Some of that is needing money and some of it is needing will.” So I thought the bottom line of it was really quite grim. If we didn’t know how bad it was, if the general public didn’t know how bad it was, the pandemic really should have taught them that because of the enormous disparities, and we’re back on this glide path toward nothing.
Rovner: I do think at very least, it is more talked about. It’s a little higher profile than it was, but obviously you’re right.
Kenen: They didn’t say no gains in any… I mean, the ACA helped. There are people who have coverage, including minorities, who didn’t have it before. That was one of the bright spots. But there’s still 10 states where it hasn’t been fully implemented. It was a pretty discouraging report.
Rovner: All right, well, that is this week’s news. Now it is time for our extra-credit segment. That’s when we each recommend a story we read this week we think you should read, too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Victoria, why don’t you go first this week?
Knight: Sure. So I was reading a story in The New York Times about PBMs [pharmacy benefit managers]. It was called “The Opaque Industry Secretly Inflating Prices for Prescription Drugs.” It’s by Rebecca Robbins and Reed Abelson. And so it kind of is basically an investigation into PBM practices. It was interesting for me because I cover health care in Congress, and so it’s always the different industries are fighting each other. And right now, one of the biggest fights is about PBMs. And for those that don’t know, PBMs negotiate with drug companies, they’re supposed to pay pharmacies, they help patients get their medications. And so they’re this middleman in between everyone. And so people don’t really know they exist, but they’re a big monopoly. There’s only three of them, really big ones in the U.S. that make up 80% of the market. And so they have a lot of control over things.
Pharma blames them for high drug prices and the PBMs blame pharma. So that’s always a fun thing to watch. There actually is quite a bit of traction in Congress right now for cracking down on PBM practices. Basically, The Times reporters interviewed a bunch of people and they came away with saying that PBMs …
Rovner: They interviewed like 300 people, right?
Knight: Yes, it said 300.
Rovner: A large bunch.
Knight: Yeah, and they came away with a conclusion that PBMs are causing higher drug prices and they’re pushing patients towards higher drugs. They’re charging employers of government more money than they should be. But it was interesting for me to watch this play out on Twitter because the PBM lobby was, of course, very upset by the story. They were slamming it and they put out a whole press release saying that it’s anecdotal and they don’t have actual data. So it was interesting, but I think it’s another piece in the policy puzzle of how do we reduce drug prices? And Congress thinks at least cracking on PBMs is one way to do it, and it has bipartisan support.
Rovner: And apparently this story is the first in a series, so there’s more to come.
Knight: Yes, I saw that. Yeah, more to come, so it’ll be fun. I also just noticed as I was just pulling it up on my phone and they had closed the comment section. It was causing some robust debate.
Rovner: Yes, indeed. Joanne?
Kenen: I should just say that after I read that story in The Times that same day, I think I got a phone call from a relative, a copay that had been something like $60 for 30 days is now $1,000. And this relative walked away without getting the drug because that’s not OK. So anyway, my extra credit [“Social Security To Drop Obsolete Jobs Used To Deny Disability Benefits,”] is from The Washington Post. Lisa Rein posted an investigation a couple of years ago, and this was the coda of the Social Security Administration finally followed through on what that investigation revealed. And Lisa wrote about the move, how it’s being addressed. That to get disability benefits, you have to be unemployable basically. And the Social Security Administration had a list of … it’s called the Dictionary of Occupational Titles. It had not been updated in 47 years. So disabled people were being denied Social Security disability benefits because they were being told, well, they could do jobs like being a nut sorter or a pneumatic tube operator or a microfilm something or other. And these jobs stopped existing decades ago.
So the Social Security Administration got rid of these obsolete jobs. You’re no longer being told, literally, to go store nuts. If you are, in fact, legitimately disabled, you’ll now be able to get the Social Security disability benefits that you are, in fact, qualified for. So thousands of people will be affected.
Rovner: No one can see this, but I’m wearing my America Needs Journalists T-shirt today. Alice?
Ollstein: I chose a piece [“Opioid Deaths Rose 50 Percent During the Pandemic. in These Places, They Fell”] by my colleague Ruth Reader, about a county in Ohio that, with some federal funds, implemented all of these policies to reduce opioid overdoses and deaths, and they had a lot of success. Overdoses went down 20% there, even as they went up by a lot in most of the country. But bureaucracy and expiring funding means that those programs may not continue, even though they’re really successful. The federal funding has run out. It is not getting renewed, and the state may not pick up the slack.
So it’s just a really good example. We see this so often in public health where we invest in something, it works, it makes a difference, it helps people, and then we say, “Well, all right, we did it. We’re done.” And then the problems come roaring back. So hopefully that does not happen here.
Rovner: Alas. Well, my extra credit this week is from The Washington Post. It’s called “Masks Are Going From Mandated to Criminalized in Some States.” It’s by Fenit Nirappil. I hope I’m pronouncing that right. In some ways, it’s a response to criminals who have obviously long used masks, and also to protesters, particularly those protesting the war in Gaza. But it’s also a mark of just how intolerant we’ve become as a society that people who are immunocompromised or just worried about their own health can’t go out masked in public without getting harassed. The irony, of course, is that this is all coming just as covid is having what appears to be now its annual summer surge, and the big fight of the moment is in North Carolina where the Democratic governor has vetoed a mask ban bill, that’s likely to be overridden by the Republican legislature. Even after covid is no longer front and center in our everyday lives, apparently a lot of the nastiness remains.
All right, that is our show. As always, if you enjoy the podcast, you can subscribe wherever you get your podcast. We’d appreciate it if you left us a review. That helps other people find us, too. Special thanks as always to our technical guru, Francis Ying, and our editor, Emmarie Huetteman. As always, you can email us your comment or questions. We’re at whatthehealth@kff.org, or you can still find me at Twitter, which the Supreme Court has now decided it’s going to call Twitter. I’m @jrovner. Alice?
Ollstein: I’m @AliceOllstein on X.
Rovner: Victoria?
Knight: I’m @victoriaregisk.
Rovner: Joanne?
Kenen: I’m at Twitter, @JoanneKenen. And I’m on Threads @joannekenen1, and I occasionally decided I just have better things to do.
Rovner: It’s all good. We will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ “What the Health?” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
11 months 2 weeks ago
Courts, Elections, Health Care Costs, Medicaid, Medicare, Mental Health, Multimedia, Public Health, States, Abortion, Biden Administration, Emergency Medicine, FDA, Guns, Idaho, KFF Health News' 'What The Health?', Misinformation, Opioid Settlements, Opioids, Podcasts, reproductive health, Trump Administration, Women's Health
Impacted by anxiety: Suzanne’s experience
Dr Alvis noted that avoiding places, people and situations are very common behaviours of a person with anxiety
View the full post Impacted by anxiety: Suzanne’s experience on NOW Grenada.
Dr Alvis noted that avoiding places, people and situations are very common behaviours of a person with anxiety
View the full post Impacted by anxiety: Suzanne’s experience on NOW Grenada.
1 year 3 weeks ago
Health, alisa alvis, anxiety, Mental Health, sorana mitchell, world health organisation
Is the Caribbean ready for radical change in mental health?
“Mental health practitioners in the Caribbean are being encouraged to ensure that the rights of patients they treat are respected, reducing stigma and discrimination and promoting human rights and recovery”
View the full post Is the Caribbean ready for radical change in mental health? on NOW Grenada.
1 year 3 weeks ago
Health, barbados, bvi, curacao, Grenada, Mental Health, montserrat, paho, pan american health organisation, sorana mitchell, st vincent, tortola, who, world health organisation
Steps to prevent further spread of chickenpox at Mt Gay Hospital
“The ministries of Health, Mental Health, Wellness, and Religious Affairs said if no new cases of chickenpox emerge, visits to the Mt Gay Hospital will resume on Saturday, 6 April 2024”
View the full post Steps to prevent further spread of chickenpox at Mt Gay Hospital on NOW Grenada.
1 year 2 months ago
Community, Health, PRESS RELEASE, chickenpox, coronavirus, COVID-19, gis, government information service, Mental Health, mt gay hospital, religious affairs, wellness
Readers Call on Congress to Bolster Medicare and Fix Loopholes in Health Policy
Letters to the Editor is a periodic feature. We welcome all comments and will publish a selection. We edit for length and clarity and require full names.
Occupational Therapists Change Lives. CMS Must Better Support Them.
Letters to the Editor is a periodic feature. We welcome all comments and will publish a selection. We edit for length and clarity and require full names.
Occupational Therapists Change Lives. CMS Must Better Support Them.
Occupational therapists are critical in helping patients adjust to new circumstances, empowering them with the tools they need to overcome barriers and regain control over their lives. Whether you’re transitioning from homelessness into a home (“In Los Angeles, Occupational Therapists Tapped to Help Homeless Stay Housed,” Jan. 24) or relearning how to do everyday tasks following a stroke, OTs are key to patients’ care plan.
But the critical care provided by OTs is being threatened by another year of payment cuts imposed by Medicare, our nation’s health care program for people age 65 and up. Many older patients treated by OTs access insurance coverage through Medicare, which typically reimburses providers at a lower rate than private insurers. And now, with payment cuts that went into effect on Jan. 1 — despite warnings and backlash from lawmakers, patients, and providers — OTs are struggling to deliver care with lower Medicare payment.
Investing in occupational therapy improves health outcomes for patients, has the potential to reduce the burden on hospitals and other health care clinicians, and keeps individuals healthy and independent. Medicare’s payment cuts only compromise the ability of providers to deliver comprehensive, compassionate care. Medicare must recognize the long-term patient benefits occupational therapy has to offer.
Luckily, Congress is considering a bill that would reverse these harmful payment cuts. The Preserving Seniors’ Access to Physicians Act of 2023 (HR 6683), would reverse the cuts that went into effect on Jan. 1, alleviating financial stress for occupational therapists and preserving patient access. I strongly urge lawmakers to prioritize and protect occupational therapy services and immediately pass HR 6683 for America’s Medicare patients.
— Doug Fosco, an occupational therapist practicing at Two Trees Physical Therapy in Ventura, California
An assistant professor at Ontario’s Western University weighed in on X.
Great to see the role of #occupationaltherapy with persons who experience #homelessness profiled in @latimes. Thanks #deborahpitts for your work in LA with @USC and #skidrowhousingtrust . Check it out @CAOT_ACE @OSOTvoice ! @CAEHomelessness https://t.co/S5s9jhgoxI
— Carrie Anne Marshall, PhD (@cannemarshall) January 24, 2024
— Carrie Anne Marshall, Sydenham, Ontario
Congress Must Finish the Job on Site-Neutral Payments
There’s an obvious solution to rein in government spending and patient out-of-pocket costs: Pay identical prices for identical care (“In Fight Over Medicare Payments, the Hospital Lobby Shows Its Strength,” Feb. 13).
As a community oncologist, it is clear to me how Medicare favors hospitals by paying more for services provided in hospital outpatient departments (HOPDs) than the same care delivered in community-based facilities. For example, last year, Medicare paid over 2.5 times as much in an HOPD as in a free-standing office for drug administration services. It’s not just Medicare paying too much; patients also face higher out-of-pocket costs for care provided in HOPDs. If the Lower Costs, More Transparency Act is signed into law, cancer patients would immediately pay less for treatments like chemotherapy.
One unintended consequence of current payment disparities is consolidation. To leverage higher reimbursements, health systems scoop up independent practices — a growing problem that is particularly pronounced in oncology. From 2008 to 2020, 435 community cancer clinics closed, while 722 contracted with or were acquired by hospitals. This consolidation is reducing patient access, particularly in rural areas, where many independent clinics operate small satellite sites that tend to be the first to close when hospitals acquire a community-based practice.
It’s time for Congress to finish the job through bills like the Lower Costs, More Transparency Act and the SITE Act, which would help level the playing field once and for all.
— Scott Rushing, Vancouver, Washington
The chief marketing officer of SKYGEN cut to the chase on X.
In the battle to control healthcare costs, hospitals are deploying their political power to protect their bottom lines. https://t.co/97r502KrpM
— Donald H. Polite (@DonaldPolite) February 15, 2024
— Donald H. Polite, Milwaukee
The ‘Gold Card’ Shuffle
Prior authorization, by definition, creates delays in care and bureaucratic barriers for physicians — which is why it is so troubling that many insurers now require prior authorization for large categories of procedures with no evidence of overuse or inappropriate use. With health insurers increasingly implementing questionable prior authorization policies, state and federal lawmakers are racing to erect safeguards that ensure patients’ access to timely care (“States Target Health Insurers’ ‘Prior Authorization’ Red Tape,” Feb. 12).
Much of the legislation to address this growing problem centers around the use of “Gold Cards” that exempt providers whose previous requests for prior authorization have been approved for a certain period. In general, these laws are important for patients who can’t afford to wait for care — especially in the field of gastroenterology where severe abdominal pain or blood in the stool could indicate a serious condition like cancer.
However, some insurance companies are co-opting the “Gold Card” term to justify new prior authorization requirements instead of streamlining existing ones. Consider the case of UnitedHealthcare, which announced it would roll out a “Gold Card” prior authorization program this year for most colonoscopies and endoscopies. No other insurer has levied such a policy, nor does the research suggest there is an overutilization of these vital services. Despite nearly a year of good faith efforts to seek transparency and guidance from UHC, the company has failed to release any data or justification that these services are improperly utilized.
If anything, diagnostic and surveillance colonoscopies and endoscopies may be underutilized. New research from the American Cancer Society shows an alarming spike in the number of younger Americans being diagnosed with and dying from colorectal cancer. Since symptoms of colorectal cancer don’t often appear until the disease is at a more advanced stage, early detection is key. Any disruption to surveillance colonoscopies (which follow removal of a precancerous polyp and are part of the screening continuum) caused by UHC’s forthcoming prior authorization policy would be dangerous for the company’s 27 million commercial beneficiaries.
The American Gastroenterological Association strongly urges UHC to rescind its “Gold Card” prior authorization policy. Policymakers must monitor how insurers are co-opting concepts meant to protect patients, in particular UHC’s faux “Gold Card,” which threatens patient access to a procedure proven to save lives.
— Barbara Jung, president of the American Gastroenterological Association, Seattle
In an X post, a senior fellow at the Manhattan Institute pointed out the value in requiring prior authorization.
Case-by-case prior authorization is never fun, but surely preferable to most other methods of eliminating needless spending (ex post denials of reimbursement, higher cost-sharing, capped global budgets, etc…) https://t.co/nYijeiAUtP
— Chris Pope (@CPopeHC) February 12, 2024
— Chris Pope, a senior fellow at the Manhattan Institute, New York City
Hospice in Prison: A Transformative View
I was so impressed with Markian Hawryluk’s exceptionally well-written article “Death and Redemption in an American Prison” (Feb. 21). I was privileged to serve as an inaugural member of the American Hospital Association’s Circle of Life Award committee, from 1999 to 2004. The awards were established to recognize the most outstanding hospice and palliative care programs in the U.S. The very first year, we received an application from the country’s largest maximum-security prison in Angola, Louisiana, the subject of Mr. Hawryluk’s wonderful article. The prison was one of the five finalists chosen for a site visit in 2000. I volunteered to be on team to visit and evaluate the prison’s hospice services.
Twenty-four years later, I still remember my conversation with one of the inmate volunteers who had just returned from bathing and feeding a dying prisoner. He told me the inmate said, “I love you.” Then the inmate volunteer stated, “I never heard those words before — not from my father, who I never met, nor from my mother.” In 2000, if one were sentenced to life at the Louisiana State Penitentiary, there was no chance for parole. When we met with the warden, he mentioned there was a waiting list of prisoners who wanted to be hospice volunteers.
Please convey my deep appreciation to Mr. Hawryluk for his outstanding article.
— Paul Hofmann, president of the Hofmann Healthcare Group, Moraga, California
A digital storyteller shared the article on X.
Your one, long read for today – it's beautifully and thoughtfully written and reported"Sometimes when you're in a dark place, you find out who you really are and what you wish you could be," Steven Garner said. "Even in darkness, I could be a light."https://t.co/57asjh11ZV
— Ameera B. ا ميرة بت 🪬 (@meerabee) February 19, 2024
— Ameera Butt, Los Angeles
Feeling Insecure Because of Social Security Tactics
When will you continue your series on the overpayments to the Social Security Administration (“Overpayment Outrage”)? People are still suffering without benefits because the agency says people were overpaid and wants the money back. Why is nobody else asking more questions?
People in this country worked hard and paid taxes. And when it is time to retire, the Social Security Administration refuses to pay if, all of a sudden, it discovers you have been overpaid. They have told me I owe them $30,000 from over 20 years ago, and I do not know what they are talking about, but they want to take my retirement money until it’s paid off. Or they want you to say it is OK to take a percentage out. Doing that would say you’re guilty and you owe the money — to me, that’s blackmail.
New immigrants get free phones, medical care, debit cards, food assistance, schooling … that comes to more than my little amount of retirement money. It seems the government can afford to take care of them, but not their own. Everyone who has had their Social Security taken away should be entitled to the free services they get, as we are in the same position — now we have nothing either.
— Thomas Troy, New York City
Lifelong Minnesotan and epidemiologist Eric Weinhandl chimed in on X.
Relatively severe incompetency. Social Security Chief Apologizes to Congress for Misleading Testimony on Overpaymentshttps://t.co/HYPcTU5tVW
— Eric Weinhandl (@eric_weinhandl) December 27, 2023
— Eric Weinhandl, Victoria, Minnesota
A Balanced View of the Law Curbing Surprise Bills
KFF Health News’ Elisabeth Rosenthal has long advocated for quality, patient-centric medical care. However, her recent article, “The No Surprises Act Comes with Some Surprises” (Feb. 14), falls short in its analysis of surprise medical billing and the federal No Surprises Act (NSA). While she places blame on physicians, the reality is more complicated.
Patients with health insurance should not be burdened with paying more than their normal in-network cost-sharing amount for unexpected out-of-network care. This is not controversial. The legislative debate was never about whether to act on surprise billing, but rather how to act. While insurers favored policies that would allow them to calculate the payment rate medical providers receive, with the NSA, Congress instead chose an approach intended to protect sustainable payment rates that would preserve patients’ access to care. The NSA removes patients from payment disputes between insurers and providers and is intended to encourage negotiations between insurers and providers, with an option for neutral arbitration.
Rosenthal’s article implies a “greedy doctor” narrative, omitting discussion of insurers as contributing to the problems with the NSA’s implementation. While the article notes that many requests for arbitration came from private equity-associated provider organizations, it neglected to note that a single insurance company (UnitedHealthcare) was involved in almost 40% of arbitration disputes. That is more than the rest of the top five insurance organizations combined. The article also quotes and references papers by Zack Cooper, whose undisclosed connections with UnitedHealthcare came to light through litigation. As reported, UnitedHealthcare not only provided data to Cooper, but helped frame the narrative of the work.
NSA rulemaking has financially incentivized insurers to leverage the NSA to unilaterally reduce existing contracted rates and push physicians out-of-network. As for the projected number of requests for arbitration in 2022 (which underestimated “providers’ ire by an order of magnitude”), that projection ignored existing data. In just the first six months of 2021, Texas alone had more than twice as many arbitration submissions for its state law as the federal government projected for the nation for a full year. More importantly, the article ignores the issue of why doctors request arbitration. Since arbitration is baseball-style and “loser pays,” there is a strong disincentive to request it without a solid reason. In the second quarter of 2023, providers won nearly 80% of disputes, reflecting the fact that doctors are going to arbitration when insurers’ actions are unreasonable.
Further, while it is true that before the NSA too many patients were receiving bills for unexpected out-of-network care, a report from the Department of Health and Human Services noted that out-of-network billing was actually declining prior to the NSA. Physician survey data suggests that post-NSA out-of-network care is now increasing due to some insurers’ actions.
The bipartisan NSA is a balanced solution to a complicated problem. Difficulties with the law’s implementation, including the volume of dispute submissions and backlog of cases, are due to unintended consequences from rulemaking. Addressing these challenges requires an honest conversation about their cause. Going forward, rulemaking is needed to promote fair network contracting, limit the need for arbitration, and, most importantly, protect patients’ access to care.
— Rich Heller, a pediatric radiologist and the associate chief medical officer for health policy, Radiology Partners, Chicago
Anesthetist-emergency physician-family doctor David Moniz, in an X post, warned of the “unseen consequences” of the No Surprises Act.
Check out the surprising outcomes of the No Surprises Act, designed to protect patients from unexpected medical bills. While it's successfully shielded many patients, there are unseen consequences. Read the full article here: https://t.co/YFa0xweRe7#health, #healthpolicy, #he…
— David Moniz (@DavidMoniz15) February 14, 2024
— David Moniz, Chilliwack, British Columbia
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 3 months ago
Health Care Costs, Health Industry, Insurance, Mental Health, Homeless, Letter To The Editor, Prison Health Care, U.S. Congress
KFF Health News' 'What the Health?': All About the (Government) Funding
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
As this election year begins in earnest, making it harder for Congress to pass bills, lawmakers on Capitol Hill are still struggling to fund the government for the fiscal year that began last October. And many health priorities hang in the balance.
Meanwhile, the Supreme Court is again wading into the abortion debate, accepting a case out of Idaho that pits a federal law requiring emergency care, including for pregnant women, against the state’s strict abortion ban.
This week’s panelists are Julie Rovner of KFF Health News, Sarah Karlin-Smith of the Pink Sheet, Tami Luhby of CNN, and Alice Miranda Ollstein of Politico.
Panelists
Sarah Karlin-Smith
Pink Sheet
Tami Luhby
CNN
Alice Miranda Ollstein
Politico
Among the takeaways from this week’s episode:
- In Washington, lawmakers have reportedly reached a deal that could pave the way for passing necessary government spending bills. But it is unlikely they will pass a full package before the current extensions end, leaving many federal health programs hanging. And ahead of next week’s Iowa caucuses, it bears asking what Republicans would do in health if the party reclaims the White House.
- The Supreme Court is again stepping into the fray over abortion rights, choosing to review the conflict between Idaho’s abortion ban and a federal law requiring emergency medical care. It is notable that justices did not have to take this case and, by swooping in now, are setting up another major abortion ruling before the 2024 election.
- The Biden administration announced it will scale back so-called conscience protections for health providers that the Trump administration sought to beef up. The back-and-forth over the policy — which was created during the George W. Bush administration — reinforces the importance of pressing presidential candidates about what they would do administratively on abortion policy, rather than asking what bills they might sign into law.
- News out of Florida this week: Newly introduced legislation there would, among other things, classify abortion as a felony and penalize those outside the state involved in the sale or distribution of abortion pills if they are “likely to be used in Florida” — a concerning example of a state effort to regulate access to abortion nationwide.
- And the FDA approved Florida’s request to import drugs from Canada, a change for which Republican Gov. Ron DeSantis is taking credit — though both President Joe Biden and former president Donald Trump could also claim some of that credit. But there are a lot of hurdles left before the state receives its first shipments, and due to the way the policy will be implemented, it may not save the state much money anyway.
“This Week in Health Misinformation” highlights Olympic gold medalist and medical crowdfunding beneficiary Mary Lou Retton, who said this week she could not afford health insurance before her headline-grabbing bout of pneumonia because her preexisting conditions made having insurance too expensive. But a decade into the existence of the Affordable Care Act, the fact is that patients can no longer be penalized on the insurance market for preexisting conditions — and, as the record 20 million Americans who enrolled in ACA coverage this year may attest, there are plenty of federal subsidies available to help afford insurance, too.
Also this week, Rovner interviews American Medical Association President Jesse Ehrenfeld, whose focus is helping the nation’s physicians navigate a rapidly changing health care system.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: CNN’s “Bottled Water Contains Thousands of Nanoplastics So Small They Can Invade the Body’s Cells, Study Says,” by Sandee LaMotte. Also, ScienceAlert’s “It Turns Out Paper Straws Might Pose a Serious Problem Too,” by Carly Cassella. Also, The Washington Post’s “How Plastic Hides in Supposedly Eco-Friendly Laundry Products,” by Michael J. Coren.
Tami Luhby: KFF Health News’ “Most People Dropped in Medicaid ‘Unwinding’ Never Tried to Renew Coverage, Utah Finds,” by Phil Galewitz.
Alice Miranda Ollstein: Stat’s “Texas Taxpayers Wanted to Help the Poor Get Health Care. Instead They’re Funding a Medical School at a Wealthy University,” by Rachel Cohrs.
Sarah Karlin-Smith: The New York Times’ “The F.D.A. Warned an Asthma Drug Could Induce Despair. Many Were Never Told,” by Christina Jewett and Benjamin Mueller.
click to open the transcript
Transcript: All About the (Government) Funding
KFF Health News’ ‘What the Health?’Episode Title: 329Episode Number: All About the (Government) FundingPublished: Jan. 11, 2024
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News, and I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, Jan. 11, at 10 a.m. As always, news happens fast, and things might have changed by the time you hear this, so here we go. We are joined today via video conference by Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Hello.
Rovner: Sarah Karlin-Smith of the Pink Sheet.
Sarah Karlin-Smith: Hi, everybody.
Rovner: And Tami Luhby of CNN.
Tami Luhby: Good morning.
Rovner: Later in this episode, we’ll have my interview with Jesse Ehrenfeld, this year’s president of the American Medical Association. It’s a bumpy time to be a doctor, and the AMA is more relevant than it’s been for quite a few years. But first, this week’s news. So we heard over the weekend that House and Senate negotiators reached a deal on top-line spending ceilings for defense and non-defense discretionary spending.
Actually, they were kind of the top lines, I believe, that they agreed to last summer, and then the House Republicans tried to change. That is all well and good, and it is definitely a prerequisite for passing full-year appropriations bills, but that’s not going to happen between now and Jan. 19, when the first of two temporary spending bills expires. So what do we expect to happen?
Ollstein: I was up on the Hill yesterday, and it’s a very “what they’re saying vs. what they’re doing” situation. They’re talking a lot about, “We got this top line. We’re moving forward. People are somewhat warming to the idea of another short-term CR [continuing resolution] to give them a little breathing room to get this done.” But then Republicans who were pissed about the entire process voted down an unrelated rule on an unrelated bill just to say, “We’re mad.” So that’s obviously not a good sign for getting big things done quickly in the next few weeks.
An issue I’m tracking is also conservatives who are disgruntled about the level of spending being higher than they wanted, saying, “Well, if we’re going to agree to this, we might as well get some policy wins out of it.” And they’re digging in harder on some of these anti-abortion provisions, other culture war things. I think the health care ones are being somewhat overshadowed right now by the immigration border stuff, but the health care things are still in the mix, for sure.
Rovner: Yeah. The CR that expires first also includes continuing authorizations for a bunch of health programs like community health centers and a delay of a bunch of scheduled Medicare payment cuts. Tami, you’re following WIC [Women, Infants, and Children nutrition program], I know, and food stamps. Do we have any idea what the fate is going to be of these things that will also expire when that first CR expires? Do we expect they’ll continue until Congress decides what to do?
Luhby: Well, actually things are looking a little better for WIC participants in terms of a shutdown, not necessarily in terms of full-year funding. But if the government had shut down in October, the USDA warned that it actually only had a few days left of money to provide for WIC. But if the government does shut down next week, then the USDA has told me that SNAP participants, food stamp participants, and WIC participants can expect to continue to get their benefits for food stamps January and February and for WIC January, February, March.
But separate from that, one of the issues that WIC participants have — and WIC, by the way, is the program that provides funding for pregnant women, new moms, infants, and young children to buy groceries. The WIC program is underfunded because there’s actually a big growth in enrollment. And so, even though the Senate provided some more money in their initial bill, they actually need more than a billion dollars more to continue the program at the current participation levels.
And a lot of folks are warning that if Congress doesn’t provide more money, there could actually be waiting lists for the first time in decades. So it’s a big issue that’s continuing because, as we know, the Republicans are not looking to add more money to nutrition assistance.
Rovner: Jumping ahead, it’s a little bit to the abortion debate. This is the argument that if you’re basically going to force women to have babies, you’re going to need to help support them if the women otherwise would’ve had an abortion because they couldn’t afford it. I think where we are with WIC, I think, is sort of the leading edge of this.
Luhby: And WIC is actually very important to that because it also provides breastfeeding assistance and guidance as well as other supports for new moms.
Rovner: So there were things, though, that didn’t even make it into the CR. One of them is the 3.4% cut in Medicare doctor pay. That took effect Jan. 1. Doctors I know would like to get that rolled back. There’s other things that are hoping to catch a ride on whatever the next vehicle is, right?
Karlin-Smith: I mean, one thing I had been watching is PBM [pharmacy benefit manager] reform. There seemed like there was some bipartisan and bicameral momentum to try and tack that on to the next big moving package. And one positive thing for that is that it does offer some amount of savings that then could be applied to other areas like spending, including potentially helping maybe with some of the Medicare cuts. So that’s something in the mix to look for.
Rovner: Yeah. Something that actually is proceeding on a separate track, right? We don’t expect that to be folded into the appropriations — unless we do. My impression was that was proceeding on its own, at least for the moment.
Karlin-Smith: I think it was proceeding on its own, but there’s been talk of could they fold it into any deal that struck to fund the government, because I think the likelihood that it really does fully clear both the House and Senate on their own is small.
Rovner: Yes, it is an election year. It is harder for Congress to get anything done. Speaking of which, on the campaign trail, the Iowa caucus is next week. Boy, that sort of snuck up on us. Former President [Donald] Trump still seems very likely to win, and he’s once again vowing to undo the Affordable Care Act, which, by the way, hit an all-time enrollment record of 20 million this week. And open enrollment isn’t even quite over. Tami, do we know what Trump would do instead? That seems to be the part. He doesn’t ever say.
Luhby: No. It’s pretty much the same plan that he probably has from 2016 and 2017, which we never really fully learned about. So, no, it’s just going to be replaced with a “better plan” because, in his view, Obamacare is failing, and as we know, [Florida Gov.] Ron DeSantis also jumped on the same bandwagon, saying that he would actually also come up with a better plan, but he needs a few months to think about it.
Rovner: Because it’s always been right about to happen, of course.
Luhby: Well, as you may have heard, health care is complicated.
Rovner: And we’ll see something in two weeks.
Luhby: Right. Along with his block grant proposal for Medicaid that he mentioned at last night’s CNN debate.
Rovner: Yes. I was sort of taken by the comments of how they would fix health care in that debate, because Nikki Haley says, “We can fix it with tort reform and transparency.”
Luhby: Transparency. Yes.
Rovner: Right. Which are nice things, and as we say, almost every week, Congress is working on those things, but they are not going to solve what ails the health care system. All right, let us turn to abortion. Remember last week when I said we were still waiting to hear from the Supreme Court on the emergency petition from Idaho regarding the conflict between its state abortion ban and the federal Emergency Medical Treatment & Active Labor Act, EMTALA?
Well, on Friday, the court not only took the case, it overturned the stay of Idaho’s ban. So, at least for now, doctors cannot even provide abortions in medical emergencies unless the woman is at immediate risk of death. Alice, I assume that gives us a hint of where the court might be going with this case, and I imagine also that similar case out of Texas.
Ollstein: Yeah. So again, with the Supreme Court, you kind of have to read the tea leaves and make educated guesses. They’re obviously very secretive. But people who are following this case closely that I’ve spoken to, they think that both the stay of the lower-court ruling and the fact that they took this case at all is the sign that they’re really gunning for ruling on the side of the state abortion restrictions. Because this is really about the state-federal clash. When state abortion bans run into federal protections for patients in emergency circumstances, and which will prevail in that circumstance. So they didn’t have to take this case. The thinking was there is eventually going to be a circuit split on this issue between the 9th Circuit and the 5th Circuit. But the 9th Circuit hasn’t had a chance to rule yet. And so they could have waited, let this play out, allowed the 9th Circuit to hear the case and issue a decision, that would’ve probably punted this case until after the election. So it’s really interesting that they instead wanted to swoop in, allow Idaho to leapfrog the 9th Circuit, and also insert themselves into this really politically volatile case, and now they’re poised to issue a ruling right before the 2024 election that could have major implications for the whole country.
Rovner: They’re going to hear the mifepristone case before this summer too, right?
Ollstein: Absolutely. And so even people who had sort of assumed on the mifepristone case like, “Oh, the Supreme Court’s going to kind of punt. They’re going to dismiss on standing.” Now, because of how aggressive they’re being in this other case, I have experts telling me, “Well, now I’m not so sure about the mifepristone case. Maybe they don’t care about optics as much as they used to.”
Rovner: Well, also, I think this is this Supreme Court’s theme, of “let states do whatever they want.” Even though federal law is supposed to trump state law, they seem to be reversing that in a rather aggressive fashion.
Ollstein: Yes. A big theme is definitely skepticism of federal rulemaking power. This falls under that same category as well.
Rovner: Well, speaking of federal rulemaking power, those who follow abortion policy in D.C. know that every time an administration changes parties, the so-called Mexico City policy that bans funding to international groups that support abortion rights gets either canceled or restored, depending on which party is in power. Well, now we have another policy that seems to be flip-flopping every time an administration changes. It was a rule first issued at the end of the George W. Bush administration. The so-called conscience rule made it easier for medical professionals and others in health care to decline to provide care that violates their religious or moral beliefs. So not just abortion but transgender care, in some cases, just treating people with AIDS. The Obama administration scaled back the Bush rule, and then the Trump administration broadened it. Then it got blocked by the courts, and now the Biden administration has formally rolled back the Trump changes that never really took effect. Alice, where are we with this?
Ollstein: Like you said, this is a back-and-forth, and I think this is why a lot of the questions being asked of candidates on the campaign trail right now, related to abortion, are the wrong questions. They keep getting asked about what kind of bills they would sign. That’s not the question. The question is what would they do administratively, which they could do so much. They could undo this. They could reverse all kinds of things. I follow the Title X stuff. I follow the Mexico City policy on restrictions on international spending on reproductive health. There’s just so much, obviously — FDA regulation of abortion pills — but these are the things we should be focused [on], not a bill that Congress has shown itself unable to pass even with one-party control of Congress.
Rovner: Nikki Haley keeps correctly saying there aren’t 60 votes for anything in the Senate related to abortion.
Ollstein: Right. But then, she also is saying that to mean a future Republican president couldn’t really do much, and that part is not true. They could do a lot.
Rovner: Exactly. Well, moving on, it’s January, and state legislatures are coming back into session. And we’re seeing some pretty eye-popping bills introduced in Florida, where abortion rights supporters just secured enough signatures to get a referendum protecting abortion rights on the 2024 ballot. Republican state Rep. David Borrero introduced a bill that would not only ban abortion, it would classify it as a third-degree felony with penalties of up to 10 years in prison. It also seeks to reach anyone outside the state who makes, sells, or mails abortion pills if they are, quote, “likely to be used in Florida.” The bill also defines personhood as beginning at the moment of fertilization, which would, among other things, make most birth control illegal and give fetuses constitutional rights. Alice, this bill is obviously not likely to pass, but legislators are playing the long game here by trying to make these things look sort of not out of the ordinary, right?
Ollstein: Yeah, the pill one, I think, is more the one to watch there. I’m curious if other states try to do that as well. Obviously, that runs into legal concerns about regulating interstate commerce, et cetera. But I think that we’ve seen these sort of nation attempts to restrict the movement of both people and medications across state lines, since that is a huge way that people are managing to terminate pregnancies despite bans right now. And so I think there’s only going to be more and more activity in that area to try to close off those remaining outlets for people. But yes, on the personhood front, that’s something that states have been attempting to do for a long time now, obviously more recently. And I think there’s sort of a strategy of, “Let’s just put it in everything we can. Let’s throw it in everything we can. Let’s throw it in bills. Let’s throw it in amicus briefs.” And the hope is to eventually force this issue in court and to get a court to rule on whether the 14th Amendment covers fetuses, basically. Will that happen and when remains to be seen, but there’s definitely an effort to sort of seed it in the landscape.
Rovner: Sarah, this obviously — not so much the personhood part, although maybe that too — but trying to ban the movement of medication is something that clearly impacts the FDA. They seem to have been pretty quiet about this, but there’s an awful lot that seems to be sort of threatening the basic core procedures of what the FDA does. Are you hearing anybody whispering about this? Is there concern?
Karlin-Smith: I think the mifepristone case at the Supreme Court is a concern for people who watch FDA’s power and regulation, not just because of abortion but because it is seen as depending on how the court decides that case is something that really could touch on all of its regulatory authority as well. Certainly, this provision that Florida is trying to put in is really something where they seem like they’re effectively trying to regulate the abortion pill throughout the entire country and regulate manufacturers. So that would be concerning, again, if that somehow came to pass and was not struck down by courts, as Alice mentioned, for interstate commerce regulation, which is not some power that is usually given to the states, but so, in general, the abortion pill controversy makes anybody who’s impacted by the FDA regulation nervous.
Rovner: Well, meanwhile, the Federal Trade Commission has entered the chat. This week, it barred a tech company from selling data on people’s visits to medical centers and other health facilities. This was not affecting abortion. They were actually just trying to help people figure out where people are and help them sort of get through their medical undertakings. But this seems like kind of a big deal enforcing privacy post-Dobbs. It’s the first one of these I’ve seen. Have you seen any of these, Alice?
Ollstein: I’m in the same camp as you. Yeah. This is sort of the first I’ve seen of this. But as has been the trend over the last couple of years, it’s a very “throw things against the wall and see what sticks” kind of environment, and so you can’t dismiss the outliers because the outliers can very quickly become the norm.
Rovner: This obviously was not a company that was trying to get women’s menstrual data and figure out whether they’re pregnant and whether they’re going to have an abortion. But there is a lot of concern that because there’s so much medical data floating out now in the metaverse, shall we say, that it would not be that hard to do that. And I guess the FTC is trying to plant a flag and say, “Mm-mm, don’t even try.” Although I’m sure people will …
Ollstein: Again, circling back to our previous theme, like, who a presidential administration installs at places like the FTC that you might not think that has anything to do with health care and abortion, but it certainly does. It certainly can. Same with DOJ, Labor Department. A lot of these things touch on reproductive health in ways that aren’t always obvious.
Rovner: That’s right. Well, turning to prescription drug news, the FDA has approved Florida’s request to import cheaper drugs from Canada. But, Tami, you wrote about this. This comes with a long list of caveats, right? It’s not like they just opened the borders and said, “OK, buy what you want.”
Luhby: No, and Florida has also put forth a fairly restricted proposal. It’s only going to be for people in their public payer program, people like inmates and people who are cared for by the county health systems and, later, Medicaid. And it’s also a pretty small list of drugs, drugs for HIV/AIDS and mental illness, and certain ones. But no, there’s a lot of hurdles before the state can actually start importing drugs. There’s going to likely be a lawsuit by PhRMA. They came out pretty strongly against it. They don’t want this, and Canada doesn’t necessarily want this. They said this in 2020 when the Trump administration first indicated that they were going to move in this direction, and then Health Canada on Friday put out a pretty strong statement saying they are clear in its position. “Bulk importation will not provide an effective solution to the problem of high drug prices in the U.S.” So there’s a long path before Florida will be able to actually see this and an even longer path before its general residents will see it. People may think, “Oh, I can go up to CVS now and order my Canadian version of the drug, which will be much cheaper.” And that’s not at all the case.
Rovner: Sarah, this has been going on for more than 20 years — I think I covered it first time in 1998 — because it’s really popular among Republicans and Democrats because it sounds so good. “We’ll just buy cheaper drugs from other countries where they have the same drugs, and they sell them for less money because they have price controls.” But Canada can’t even supply Florida, much less the rest of the country, right?
Karlin-Smith: Right. I think people, sometimes you look at Canada on a map geographically. It’s a very large area, but the population compared to the U.S. is much smaller. So the supply chain that’s feeding Canada is very different. And then you get into why HHS and FDA has usually pushed back against this idea is because they’re concerned about securing the supply-chain safety and making sure people are actually getting what they … think they’re getting and know how to use the drug. And what’s basically happened under starting the Trump administration and then Biden’s kind of continued it is they came up with a pathway to sort of make importation potentially possible. But they put in so many hoops that these states will have to go through and so many processes in place to ensure the safety of it that by the time Florida does all of this, and again, as Tami mentioned, FDA hasn’t cleared any specific drugs for Florida to import yet; each drug product still is going to have to go through a bunch of steps to get that OK. So by the time they do all of that, it doesn’t look like it’s going to save very much money. Florida’s estimating maybe not quite $200 million for the first year and about the same the second year. If you look at just their Medicaid spending in a year on outpatient drugs, it’s like $1.-something billion. So you can see how tiny a savings that is.
Rovner: Yes. This is one of those things that’s not been partisan. It’s always been sort of the FDA wanting to protect the integrity of the supply chain, whether it’s controlled by Democrats or Republicans versus Democrats and Republicans who would like to find a way to help their constituents get cheaper drugs.
Luhby: One thing also to note that’s going to be interesting, because there’ve been so many people involved in this, we saw Ron DeSantis say yesterday at the debate that he took credit for pushing the federal government and beating the federal government, I think he said, to be allowed to import drugs. But this is also going to be a talking point that Trump and Biden will also be able to say on the campaign. So basically, everyone is probably going to try to take credit for this.
Rovner: Right. Everybody’s going to take credit for something that’s probably only going to happen in a very small way, if it happens at all.
Luhby: If it all happens at all.
Rovner: That’s right. Well, also this week, drug maker Eli Lilly said it is setting up its own telehealth service to help patients access not only its soon-to-be blockbuster weight loss drug Zepbound but also other diabetes and migraine drugs, basically cutting out the doctor or at least cutting out the patient’s regular doctor, if they have one. Sarah, this feels to me like a really big sea change. Is the FDA going to let this happen? Is the AMA going to let this happen?
Karlin-Smith: It’s really interesting. I think the first headline of it makes it seem a little bit more extreme or maybe novel than once you actually look into the details because Lilly’s …
Rovner: Kind of like drug importation.
Karlin-Smith: Right. Although I think more patients maybe will actually be served by this program. But, basically, Eli Lilly is setting up a website that will then connect patients to outside telehealth companies that have the ability to prescribe the drug. Again, these telehealth companies are supposedly prescribing all different drugs, not just Eli Lilly products. The doctor’s supposed to make sure you actually qualify for the product, and so forth. And then Lilly also seems to have developed partnerships with a couple online pharmacy companies that could then directly mail you the product. So Eli Lilly is sort of helping facilitate these connections for patients. But I think probably to avoid various scrutinies by the federal government, they’ve tried to disconnect themselves a few steps, but certainly make the process of getting a drug and their drug easier for patients. Also helping ease the process of getting any copay support or coupons the company offers. So they seem to be kind of taking advantage of a trend that we’ve seen in other areas, with ADHD, like male sexual health products, and so forth, of people wanting to do this through telehealth. And so they’re trying to, I think, get at least a cut of it or at least help steer their product there. But there’s definitely going to be questions, I think, around how you handle advertising and other things for the government to look at.
Rovner: Yeah, it’s definitely a space that, now, we’re going to have to start watching as well as everything else. All right. Well, now it is time for “This Week in Health Misinformation,” which is going to Olympic gold medalist gymnast Mary Lou Retton. Retton, who is now in her mid-50s, contracted a rare form of pneumonia, ended up in the hospital for a month, and became the subject of a crowdfunding effort launched by her daughter because she didn’t have health insurance. Retton, who has been very closed-mouthed about her illness and what happened to the half a million dollars the crowdfunding campaign raised, as is her right, did do an interview this week with the “Today” show on NBC in which she said she couldn’t afford health insurance because her preexisting conditions made it too expensive. For the record, if you’re uninsured, you can still sign up for an Affordable Care Act Plan in most states, and you can’t be charged more due to preexisting conditions. And there are still extra subsidies that we talked about earlier that were implemented during covid that makes insurance even more affordable. Why is it that people don’t know this yet?
Ollstein: Well, as we saw with record-breaking enrollment, a lot of people do know it, but the people who don’t are still loud.
Rovner: We’re 10 years into the ACA!
Ollstein: Yes. It’s funny. I mean, living in D.C. and doing this work, I always try to think about what of all of our reporting actually breaks through around the country. And it’s always interesting to see what does and what doesn’t.
Rovner: I used to stomp around the NPR newsroom when the ACA was just getting up and running, saying, “It is not my job to do the administration’s publicity. It’s really not my job.” But …
Luhby: Yeah.
Rovner: … they are still working on it.
Luhby: It also may be selective ignorance, because I’m sure if she actually asked anyone about health insurance or called any agent or insurer and said, “Well, I have this preexisting condition,” they may have said, “Well, on the ACA, it doesn’t matter anymore.”
Rovner: Yes. And that if she said she didn’t have the money after her divorce, it’s like those are the people who are eligible for big subsidies. All right. Well, that is this week’s news. Now, we will play my interview with AMA President Jesse Ehrenfeld, and then we will come back and do our extra credits.
I am pleased to welcome to the podcast, in person here in our D.C. studio, Dr. Jesse Ehrenfeld, president of the American Medical Association. Dr. Ehrenfeld is an anesthesiologist, medical school professor, researcher on medical information technology, and director of a statewide health philanthropy in Wisconsin, among other activities. He’s an Afghanistan combat veteran twice over, as well as the first openly gay president of the AMA and a national advocate for LGBTQ+ rights. Dr. Ehrenfeld, thank you so much for coming in. You are a very busy person.
Jesse Ehrenfeld: Well, thanks for having me. It’s great to talk to you today.
Rovner: So I want to start on Capitol Hill, since we’re here in D.C.
Ehrenfeld: Sure.
Rovner: And Congress is coming back and working on a budget, or so we hear.
Ehrenfeld: We hope they’re working.
Rovner: I know physicians are facing, again, a cut in Medicare pay, but that’s not the only AMA priority here in Washington at the moment, right?
Ehrenfeld: Well, it’s a big one for us. And, you know, it’s really painful that you turn the clock back, Jan. 1, and 3.37% Medicare cut to physician payments. It’s unconscionable. And so we’re optimistic that we can get a fix, hopefully retroactive, as the omnibus consolidation work goes forward, short of this Jan. 19 deadline coming up. But we can’t have it. Physicians continue to struggle. My parents lost their own primary care physician because of a challenge with their primary care doctor not being able to take Medicare anymore. And what we’re seeing is more and more doctors just stopping seeing new Medicare patients, or opting out of the program entirely. So, every other provider under Medicare is actually fighting for how many increase they’re getting while doctors are getting cut. So we’re hopeful that we can solve this, but it really is something that’s just urgent for us as an association.
Rovner: I thought we took care of this in 2015. I feel like it’s Groundhog Day. I covered it every year from about 2003 to about 2015, and then we solved it briefly.
Ehrenfeld: We solved one problem and replaced it with another, unfortunately. And the doomed SGR did die in 2015 — the unsustainable “sustainable growth rate” problem — that did lead to those year-end patches. And, unfortunately now, though, because of budget neutrality rules and other — we’ll call them “features” — of the program, we’re in the situation again. We do have optimism, though, that we might get some standing inflationary updates. There was the introduction of a bill last session. And we hope that that can be something that does move forward once we get through this time-sensitive issue to deal with the 3.37% cut.
Rovner: So I feel like the physician shortage is kind of like climate change. People have been warning about it for decades, and suddenly it’s here.
Ehrenfeld: It’s here.
Rovner: With people having to wait weeks or sometimes months to see a doctor. Obviously, like with climate change, it’s going to take a while to get out of the hole that we have dug. I know we’ve seen the establishment of several new medical schools, both allopathic and osteopathic, in the past decade. How soon might we be able to see some relief, and what more will it take beyond training more doctors?
Ehrenfeld: Well, we’re opening more medical schools, but we’re not actually training more doctors. And that’s the problem. We haven’t expanded GME [Graduate Medical Education] residency programs. And unfortunately, because, as you know, GME funding through the federal government is tied to a fixed cap, set in the 1990s by Medicare, we’ve opened all these new schools and the students don’t have a place to go to train. So that’s a problem that we need to solve. We’ve had a little tiny, tiny increase these past few years, a couple of hundred spots here and there. We need thousands more training spots open. We need the GME dollars to come from Medicare. We also need to solve some of the issues around how we get international medical graduates here and ready to practice in the U.S. Twenty-five percent of practicing physicians in the U.S. were trained abroad. Most people don’t know that. We already have a huge international workforce, but we do silly things, like we’ll let an international doctor train their residency here, and then we make them go away for two years to their home country before they can come back. There are H-1B visa waiver bills that are circulating around the Conrad 30 extension. We need to do those things as well. Unfortunately, as you’re aware, immigration reform is a challenging issue here in Washington. But there are commonsense solutions that have bipartisan support. And we’re hopeful that we can get some workforce pressure reductions, not just by expanding GME for U.S.-trained individuals, but also those international graduates.
Rovner: Yeah, I feel like people forget that immigration is about more than just people coming across the southern border. There are a lot of skilled-worker issues in the immigration debate.
Ehrenfeld: In lots of industries, health care, technology, other places as well.
Rovner: I know the rise — or should I say the “re-rise” — of prior authorization requirements from insurance companies is something that contributes to physician burnout and the physician shortage by driving doctors out of practice, just from frustration. The Biden administration has a new regulation to limit prior authorization in the pipeline. Assuming that that regulation is finalized soon, how close will that come to fully addressing the problem for your members?
Ehrenfeld: You know, we hope it’ll move the needle a little bit, but we need wholesale reform, and we need to do more than Medicare Advantage plans. Unfortunately, I hear every week from colleagues who are just at their wits’ end, and it’s frustrating. I see it with my own parents. I’m an anesthesiologist. I have a habit now, I ask my patients: “So how long did it take your surgery to get scheduled?” Eh, it’s a couple weeks or a month. I said, “And how long did it take for your insurance company to approve the procedure?” And it’s months. And often what they tell me is they approved it, and then they denied it after they approved it. And they have to go through all of this rigmarole that just doesn’t make sense.
Rovner: You think that Congress is going to need to step in at some point, or is this something that can be worked out?
Ehrenfeld: I think we’re going to have to have regulatory relief from Congress, and we’re pushing for that through our grassroots network. Certainly, we try to bring all the third-party payers together. We have a set of principles that, theoretically, third-party payers have agreed to, and yet they ignore them, and they continue to just harass patients, really to improve their bottom line, but not doing what’s in their best interests.
Rovner: So I want to talk a little bit about physician autonomy. Since the overturn of Roe v. Wade, we’ve seen an increasing level of what I call legislators practicing medicine. Now we have the Supreme Court …
Ehrenfeld: It’s OK if they have an MD.
Rovner: [laughs] That’s true. Now we have the Supreme Court — none of whom have an MD as far as I know — about to decide whether doctors facing women with pregnancy emergencies should obey state abortion bans, the federal EMTALA law, or their medical ethics, all of which may conflict. What’s the AMA doing to help doctors navigate these very choppy and changing legal waters?
Ehrenfeld: “Choppy” is a good word for it. It’s confusing. And since the decision, the Dobbs decision, came out, we have been working with all of our state and federation partners to try to help physicians navigate this. And I can tell you, it’s unbelievable that now physicians are having to call their attorneys, the hospital legal counsel to figure out what they can and can’t do. And obviously, this is not a picture that is a picture that supports women’s health. So we are optimistic that we might get a positive ruling with this EMTALA decision on the Supreme Court. But, obviously, there’s a long way that we need to go to make sure that we can maintain access for reproductive care.
Rovner: You’re younger than I am, but when I was growing up and covering this, the AMA didn’t want to talk about abortion because it was controversial. And now, certainly in the last five or 10 years, the AMA has come out. Do you think that’s something that has dawned on the rest of the members of the AMA that this is not necessarily about abortion, this is about the ability to practice medicine?
Ehrenfeld: Well, you know, look, if you look at some of these socially charged restrictive laws, whether it’s in transgender health or abortion access, or other items, we take the same foundational approach, which is that physicians and patients ought to be making their health care decisions without legislative interference.
Rovner: So it’s not just abortion and reproductive health where lawmakers are trying to dictate medical practice but also care for transgender kids and adults and even treatment for covid and other infectious diseases. How big a priority is this for the AMA, and what are you doing to fight the sort of “pushing against” scientific discourse?
Ehrenfeld: Well, we will always stand up for science. And it’s so important that as an association we do that. Our foundation in 1847 was to get rid of quackery and snake oil salesmen in medicine. And yet here we are trying to do some of those same things with misinformation, disinformation. And obviously, even if you look at the attack on PrEP, preexposure prophylaxis for HIV prevention — you know, an important part of the Affordable Care Act, right? Making it basically zero out-of-pocket cost for many Americans — those things are just unconscionable. We have treatments. We know that they work. We ought to make sure that patients and their physicians can have access to them.
Rovner: What about doctors who are pushing things that you know to be not helpful?
Ehrenfeld: We call them out, and we would encourage others to call them out. If somebody is trying to sell something that’s inappropriate or do something that doesn’t follow the evidence, we need to call it for what it is, which is inappropriate.
Rovner: It’s not just legislators who want to practice medicine these days. We also have the rise of artificial intelligence, which I know promises both huge advances …
Ehrenfeld: I’m real, by the way.
Rovner: [both laugh] Yes, I can attest that you’re real. At least you seem real. But, obviously, our artificial intelligence can portend huge advances and also other issues, not all of which are good. How is the AMA trying to push the AMA more towards the former, the good things, and less towards the latter, the unintended consequences?
Ehrenfeld: Well, we’re really excited about it. I’m excited about it. I have an informatics background. So, you know, I believe that there is so much power that these technologies and tools can bring, but we need to make sure that the technology is an asset, not a burden. And we have all lived through the painful rollout of electronic health records where that just was not the case. So we did survey — we do routine surveys, data that’s a nationally representative sample — in August of this year, it’s on our website. An equal number of physicians are excited about AI as they are terrified about AI, anxious, concerned, right? And we need to make sure that we have the right regulatory framework. We’re very appreciative of the ONC [Office of the National Coordinator for Health Information Technology] rule that came out, out of HHS [the Department of Health and Human Services], at the end of last year. Certainly, the Biden administration’s, whole of government’s approach we think is important, but that is no substitution for regulation. And we need to make sure that we have appropriate regulation. The FDA doesn’t have the framework that they need. The system set up in the ’60s and ’70s for drugs and biologics and devices hasn’t held up. So we know that there have to be changes. We just need to make sure that those changes only let safe and effective algorithms, AI tools, AI-powered products come to the marketplace.
Rovner: Dr. Ehrenfeld, that’s all the time we have. Thank you so much for joining us.
Ehrenfeld: Oh, thanks for having me. It’s been a treat.
Rovner: OK, we are back. It’s time for our extra-credit segment. That’s when we each recommend a story we read this week we think you should read, too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Tami, why don’t you go first this week?
Luhby: OK. Well, my extra credit is titled “Most People Dropped in Medicaid ‘Unwinding’ Never Tried to Renew Coverage, Utah Finds,” by KFF Health News’ Phil Galewitz. And as many of our podcast listeners know, states are reviewing the eligibility of their residents in Medicaid and terminating the coverage of those they deem ineligible. Roughly 14.4 million people have been disenrolled. And the big question is, what has happened to them? Did they return to Medicaid? Did they find coverage elsewhere, or did they become uninsured? And that’s the question that many actually Medicaid directors have been unable to answer.
So Phil’s story looks at a first-of-its-kind study conducted in October by Utah’s Medicaid agency. And in Utah, 94% of those disenrolled were dropped for procedural reasons, such as not returning their paperwork, rather than being deemed ineligible. And the study found that 57% of respondents did not attempt to renew their Medicaid coverage. Thirty-nine percent shifted to employer plans, and 15% signed up for Affordable Care Act coverage. So they remained insured, but 30% became uninsured. The story also shows that many Medicaid enrollees said that they had trouble reapplying for Medicaid coverage. They didn’t get the documents. They didn’t have the necessary paperwork. They couldn’t get their questions answered. And these are all things that we’ve heard about anecdotally, but the Utah study and Phil’s story actually put some numbers to it. And interestingly, Utah officials also confirmed that the U.S. Department of Health and Human Services is conducting two audits of the state’s Medicaid unwinding. So we’ll see what happens and what we find out from Utah may inform us about what’s happening in the rest of the country.
Rovner: Yes, we have noted before that HHS has been very close-mouthed about how it is trying to get states to maintain coverage for these people who are, if not eligible for Medicaid anymore, eligible for something else. Alice, you have kind of a related story, so why don’t you go next?
Ollstein: Yeah, I have something from our own Rachel Cohrs at Stat. It’s called “Texas Taxpayers Wanted to Help the Poor Get Health Care. Instead They’re Funding a Medical School at a Wealthy University.” It’s a great accountability story about how taxpayers were convinced to put up tens of millions of dollars that they thought was going to provide care for very poor people in the area around Austin, Texas. And instead, basically, none of that money is going to … directly to provide that care to people. And instead, it’s gone to build fancy buildings at this medical school, and overhead, and recruiting faculty. And the school and hospital insist that all of this trickles down eventually to patients. But it’s not what taxpayers feel they were promised. And so they’re getting upset about that.
Rovner: It is a very nice medical school. Sarah.
Karlin-Smith: I looked at a New York Times story from Christina Jewett and Benjamin Mueller, “The F.D.A. Warned an Asthma Drug Could Induce Despair. Many Were Never Told,” and it’s about Singulair, a now generic asthma medicine. Over 20 years after it was first approved, FDA added what’s known as its strictest warning, a black box warning, warning of very serious mental health side effects, including suicidal thoughts. And The New York Times investigation seems to have found out that really these messages are not reaching doctors. They’re not reaching patients, or parents, and many young kids who are taking this medicine. And that has led to many ill effects, including some very young people who have died by suicide. And it’s a really good dive into the challenges that FDA faces and kind of translating their regulatory action into something that then gets communicated to a doctor, and then a doctor translates to a patient. In many ways, it’s not that surprising a story to me because I think it’s kind of well known that not a lot of people read drug labels and then certainly not on an individual level, but even on a doctor level. And I think a lot of the risk-benefit conversations that FDA envisions happen between doctors and patients before people take drugs don’t actually happen in the real world. I once actually had a doctor who told me, “This medicine has a box warning, but don’t worry about it.” Which I always find as a pretty funny story as a drug reporter. And it just also raises a lot of issues, this story, about how drugs are studied on children and what’s done to make sure that as a drug goes generic, the safety is still being monitored, and somebody is responsible again for ensuring people are aware of new safety updates. So it’s a really good dive. I think the thing I was most struck by, though, is I think the solutions perhaps here are not ones that would be very popular in the U.S., which is that by design, the FDA does not regulate the practice of medicine. And, in most cases, I don’t think Americans would want FDA pushing the boundaries much further to get at the safety hurdles this story maybe flags.
Rovner: Yeah. More along our theme of the federal government and its role in society. Well, my extra credit this week is actually a collection of stories. It’s sparked by the headline on this month’s issue of Consumer Reports, which is “How to Eat Less Plastic.” The first story is from CNN reporting on a study in the proceedings of the National Academy of Sciences called “Bottled Water Contains Thousands of Nanoplastics So Small They Can Invade the Body’s Cells, Study Says.” And it basically says that plastic sheds just like skin cells do. So anything you eat or drink that’s stored or wrapped in plastic is going to get into whatever it is you’re putting into your body. If that’s not enough to give you pause, my second story is from ScienceAlert, which is a website, called “It Turns Out Paper Straws Might Pose a Serious Problem Too.” And it’s about a study that found that many paper straws contain those forever chemicals we keep hearing about, called PFAS, which, of course, are also in many plastics. Finally, if that’s not enough plastic for you, here’s a story from The Washington Post called “How Plastic Hides in Supposedly Eco-Friendly Laundry Products.” Basically, those laundry sheets that can replace the use of all those plastic bottles that we keep seeing ads for? Apparently, even many of those sheets that claim to be, quote, “plastic-free” contains something called polyvinyl alcohol, which is, you guessed it, a plastic that’s been found in drinking water and breast milk. I think the message here is everything you do is probably bad for you in some way, so be humble and do the best you can.
OK, that is our show. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us, too. Special thanks, as always, to our technical guru, Francis Ying, and our editor, my fellow happy Michigan Wolverine this week, Emmarie Huetteman. As always, you can email us your comments or questions. We’re at whatthehealth@kff.org, or you can still find me at X, @jrovner, or @julierovner at Bluesky and @julie.rovner at Threads. Sarah, where are you these days?
Karlin-Smith: I’m trying to be places, but then it’s hard to be at all of them. So mostly Twitter and Bluesky, @SarahKarlin or @sarahkarlin-smith.
Rovner: Tami?
Luhby: The best place to find me is cnn.com.
Rovner: There you go. Alice.
Ollstein: Still on X @AliceOllstein, and @alicemiranda on Bluesky.
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ “What the Health?” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 5 months ago
Courts, Elections, Health Care Costs, Health Industry, Medicaid, Medicare, Mental Health, Multimedia, Public Health, States, Abortion, Biden Administration, KFF Health News' 'What The Health?', Misinformation, Podcasts, Pregnancy, U.S. Congress, Women's Health
As Foundation for ‘Excited Delirium’ Diagnosis Cracks, Fallout Spreads
When Angelo Quinto’s family learned that officials blamed his 2020 death on “excited delirium,” a term they had never heard before, they couldn’t believe it. To them, it was obvious the science behind the diagnosis wasn’t real.
Related Links
-
Police Blame Some Deaths on ‘Excited Delirium.’ ER Docs Consider Pulling the Plug on the Term.
Oct 2, 2023
-
California Bans Controversial ‘Excited Delirium’ Diagnosis
Oct 12, 2023
-
Doctors Abandon a Diagnosis Used to Justify Police Custody Deaths. It Might Live On, Anyway.
Oct 16, 2023
Quinto, 30, had been pinned on the ground for at least 90 seconds by police in California and stopped breathing. He died three days later.
Now his relatives are asking a federal judge to exclude any testimony about “excited delirium” in their wrongful death case against the city of Antioch. Their case may be stronger than ever.
Their push comes at the end of a pivotal year for the long-standing, nationwide effort to discard the use of excited delirium in official proceedings. Over the past 40 years, the discredited, racially biased theory has been used to explain away police culpability for many in-custody deaths. But in October, the American College of Emergency Physicians disavowed a key paper that seemingly gave it scientific legitimacy, and the College of American Pathologists said it should no longer be cited as a cause of death.
That same month, California’s Democratic Gov. Gavin Newsom signed the nation’s first law to ban the term “excited delirium” as a diagnosis and cause of death on death certificates, autopsy reports, and police reports. Legislators in other states are expected to consider similar bills next year, and some law enforcement agencies and training organizations have dropped references to excited delirium from their policy manuals and pulled back from training police on the debunked theory.
Despite all that momentum, families, attorneys, policing experts, and doctors say much remains to be done to correct the mistakes of the past, to ensure justice in ongoing trials, and to prevent avoidable deaths in the future. But after years of fighting, they’re heartened to see any movement at all.
“This entire thing, it’s a nightmare,” said Bella Collins, Angelo’s sister. “But there are silver linings everywhere, and I feel so fortunate to be able to see change happening.”
Ultimately, the campaign against excited delirium seeks to transform the way police deal with people undergoing mental health crises.
“This is really about saving lives,” said Joanna Naples-Mitchell, an attorney who worked on an influential Physicians for Human Rights review of excited delirium.
Changing Law Enforcement Training
The use of the term “excited delirium syndrome” became pervasive after the American College of Emergency Physicians published a white paper on it in 2009. It proposed that individuals in a mental health crisis, often under the influence of drugs or alcohol, can exhibit superhuman strength as police try to control them, and then die suddenly from the condition, not the police response.
The ACEP white paper was significant in catalyzing police training and policy, said Marc Krupanski, director of criminal justice and policing at Arnold Ventures, one of the largest nonprofit funders of criminal justice policy. The theory contributed to deaths, he said, because it encouraged officers to apply greater force rather than call medical professionals when they saw people in aggressive states.
After George Floyd’s 2020 death, which officers blamed on excited delirium, the American Medical Association and the American Psychiatric Association formally rejected it as a medical condition. Then came disavowals from the National Association of Medical Examiners and the emergency physicians’ and pathologists’ groups this year.
The moves by medical societies to renounce the term have already had tangible, albeit limited, effects. In November, Lexipol, a training organization used by thousands of public safety agencies in the U.S., reiterated its earlier move away from excited delirium, citing the California law and ACEP’s retraction of the 2009 white paper.
Lexipol now guides officers to rely on what they can observe, and not to guess at a person’s mental status or medical condition, said Mike Ranalli, a lawyer and police trainer with the Texas-based group. “If somebody appears to be in distress, just get the EMS,” he said, referring to emergency medical services.
Patrick Caceres, a senior investigator at the Bay Area Rapid Transit’s Office of the Independent Police Auditor, successfully pushed to remove excited delirium from the BART Police Department’s policy manual after learning about Quinto’s death in 2020 and seeing the American Medical Association’s rejection of it the following year.
Caceres fears that rooting out the concept — not just the term — more broadly will take time in a country where law enforcement is spread across roughly 18,000 agencies governed by independent police chiefs or sheriffs.
“The kinds of training and the kinds of conversations that need to happen, we’re still a long way away from that,” said Caceres.
In Tacoma, Washington, where three police officers have been charged with the 2020 death of Manuel Ellis, The Seattle Times reported that local first responders testified as recently as October that they still “embrace” the concept.
But in Colorado, the state’s Peace Officer Standards and Training board ruled on Dec. 1 to drop excited delirium training for new law enforcement officers, KUSA-TV reported.
And two Colorado lawmakers, Democratic state Reps. Judy Amabile and Leslie Herod, have drafted a bill for the 2024 legislative session banning excited delirium from other police and EMS training and prohibiting coroners from citing it as a cause of death.
“This idea that it gives you superhuman strength causes the police to think they should respond in a way that is often completely inappropriate for what’s actually happening,” Amabile said. “It just seems obvious that we should stop doing that.”
She would like police to focus more on de-escalation tactics, and make sure 911 calls for people in mental health crisis are routed to behavioral health professionals who are part of crisis intervention teams.
Taking ‘Excited Delirium’ Out of the Equation
As the Quinto family seeks justice in the death of the 30-year-old Navy veteran, they are hopeful the new refutations of excited delirium will bolster their wrongful death lawsuit against the city of Antioch. On the other side, defense lawyers have argued that jurors should hear testimony about the theory.
On Oct. 26, the family cited both the new California law and the ACEP rebuke of the diagnosis when it asked a U.S. District Court judge in California to exclude witness testimony and evidence related to excited delirium, saying it “cannot be accepted as a scientifically valid diagnosis having anything to do with Quinto’s death.”
“A defense based on BS can succeed,” family attorney Ben Nisenbaum said. “It can succeed by giving jurors an excuse to give the cops a way out of this.”
Meanwhile, advocates are calling for a reexamination of autopsies of those who died in law enforcement custody, and families are fighting to change death certificates that blame excited delirium.
The Maryland attorney general’s office is conducting an audit of autopsies under the tenure of former chief medical examiner David Fowler, who has attributed various deaths to excited delirium. But that’s just one state reviewing a subset of its in-custody deaths.
The family of Alexander Rios, 28, reached a $4 million settlement with Richland County, Ohio, in 2021 after jail officers piled on Rios and shocked him until he turned blue and limp in September 2019. During a criminal trial against one of the officers that ended in a mistrial this November, the pathologist who helped conduct Rios’ autopsy testified that her supervisor pressured her to list “excited delirium” as the cause of death even though she didn’t agree. Still, excited delirium remains his official cause of death.
The county refused to update the record, so his relatives are suing to force a change to his official cause of death. A trial is set for May.
Changing the death certificate will be a form of justice, but it won’t undo the damage his death has caused, said Don Mould, Rios’ stepfather, who is now helping to raise one of Rios’ three children.
“Here is a kid that’s life is upside down,” he said. “No one should go to jail and walk in and not be able to walk out.”
In some cases, death certificates may be hard to refile. Quinto’s family has asked a state judge to throw out the coroner’s findings about his 2020 death. But the California law, which takes effect in January and bans excited delirium on death certificates, cannot be applied retroactively, said Contra Costa County Counsel Thomas Geiger in a court filing.
And, despite the 2023 disavowals by the main medical examiners’ and pathologists’ groups, excited delirium — or a similar explanation — could still show up on future autopsy reports outside California. No single group has authority over the thousands of individual medical examiners and coroners, some of whom work closely with law enforcement officials. The system for determining a cause of death is deeply disjointed and chronically underfunded.
“One of the unfortunate things, at least within forensic pathology, is that many things are very piecemeal,” said Anna Tart, a member of the Forensic Pathology Committee of the College of American Pathologists. She said that CAP plans to educate members through conferences and webinars but won’t discipline members who continue to use the term.
Justin Feldman, principal research scientist with the Center for Policing Equity, said that medical examiners need even more pressure and oversight to ensure that they don’t find other ways to attribute deaths caused by police restraint to something else.
Only a minority of deaths in police custody now cite excited delirium, he said. Instead, many deaths are being blamed on stimulants, even though fatal cocaine or methamphetamine overdoses are rare in the absence of opioids.
Yet advocates are hopeful that this year marks enough of a turning point that alternative terms will have less traction.
The California law and ACEP decision take “a huge piece of junk science out of the equation,” said Julia Sherwin, a California civil rights attorney who co-authored the Physicians for Human Rights report.
Sherwin is representing the family of Mario Gonzalez, who died in police custody in 2021, in a lawsuit against the city of Alameda, California. Excited delirium doesn’t appear on Gonzalez’s death certificate, but medical experts testifying for the officers who restrained him cited the theory in depositions.
She said she plans to file a motion excluding the testimony about excited delirium in that upcoming case and similar motions in all the restraint-asphyxia cases she handles.
“And, in every case, lawyers around the country should be doing that,” Sherwin said.
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 6 months ago
california, Mental Health, States, Colorado, Emergency Medicine, Legislation, Maryland, Ohio, Washington
El condado de Los Angeles ofrece terapia virtual gratuita de salud mental para estudiantes
LOS ANGELES – Las escuelas públicas del condado de Los Angeles han puesto en marcha una ambiciosa iniciativa para ofrecer servicios gratuitos de salud mental a sus 1,3 millones de estudiantes de primaria y secundaria (K-12), una prueba clave del amplio programa de $4,700 millones del gobernador de California, Gavin Newsom, para hacer frente a la crisis de salud mental entre los jóvenes.
Impulsado por los planes Medi-Cal del condado —que proporcionan seguro médico a los residentes con bajos ingresos— en colaboración con su Oficina de Educación y el Departamento de Salud Mental, el programa se basa en servicios de teleterapia proporcionados por Hazel Health, una de las empresas que han surgido para hacer frente a la escasez nacional de servicios de salud mental, algo que se agravó durante la pandemia de covid-19.
La teleterapia es uno de los cuatro proyectos del condado de Los Angeles que recibirán en conjunto hasta $83 millones del Programa de Incentivos de Salud Mental para Estudiantes del estado, uno de los componentes del “plan maestro” del gobernador demócrata para subsanar las deficiencias en el acceso de los jóvenes a los servicios de salud mental.
El contrato de Hazel Health en Los Angeles tiene como meta ayudar a las escuelas sobrecargadas a hacer frente al aumento de la demanda de estos servicios. Promete ser una iniciativa piloto para demostrar tanto la eficacia de la terapia virtual para los alumnos, como la capacidad de educadores y administradores para gestionar eficazmente un programa extenso y delicado en colaboración con una empresa con fines de lucro.
Para algunos educadores y familias los resultados iniciales son prometedores.
Anjelah Salazar, de 10 años, dijo que el especialista de Hazel la ha ayudado a sentirse mucho mejor. La estudiante de quinto grado empezó a sufrir ataques de pánico diarios al cambiar de escuela este año a la primaria Stanton de Glendora.
Su madre, Rosanna Chavira, contó que no sabía qué hacer —aunque es coordinadora clínica de una empresa que trata enfermedades mentales— y le preocupaba no poder pagar un terapeuta que aceptara su seguro. Cuando Chavira supo de Hazel, no lo dudó.
“El hecho de que sea gratis y de que un profesional le enseñe estrategias para sobrellevar distintas situaciones significa mucho”, dijo Chavira. “Ya se notan los resultados”.
Salazar dijo que hasta ahora tuvo cinco citas virtuales con su terapeuta. Una técnica de afrontamiento que aprecia especialmente es un ejercicio de tapping: todas las noches, antes de acostarse, se presiona con el dedo un poquito los ojos, las mejillas, el pecho y las rodillas. Con cada toque, dice: “Soy valiente”.
Christine Crone, madre de Brady, alumno de séptimo grado, afirmó que aún no ha comprobado si las sesiones son eficaces para su hijo, que estudia en Arroyo Seco Junior High en Santa Clarita, pero sí sabe que las disfruta.
“Normalmente le cuesta llegar a tiempo y estar preparado, pero con estas sesiones siempre deja lo que está haciendo y es puntual”, dijo Crone. “Dice que su terapeuta es agradable, divertido y que es fácil hablar con él”.
Jennifer Moya, consejera de salud mental en la escuela primaria Martha Baldwin de Alhambra, una ciudad al este de Los Angeles, dijo que a sus alumnos les gusta la flexibilidad de la teleterapia, que les permite reunirse con los terapeutas en cualquier momento entre las 7 de la mañana y las 7 de la tarde.
“Esta generación de niños ha crecido en la era digital”, señaló Moya, que se encarga de remitir a los alumnos a Hazel en su centro. “Les encanta que esto sea fácil”.
Pablo Isais, consejero de salud mental en la escuela primaria Granada’s Alhambra, dijo que los servicios también pueden ser una solución provisional mientras un estudiante espera una cita en persona, que puede tomar de seis a ocho semanas.
“Ser capaz de comunicarles que hay servicios disponibles a los que pueden acceder en la próxima semana es increíble”, dijo Moya.
Hasta ahora, sólo 607 estudiantes del condado de Los Angeles han participado en las sesiones desde que se ofrecieron por primera vez, en Compton, en diciembre de 2022, explicó Alicia Garoupa, jefa de servicios de bienestar y apoyo de la Oficina de Educación. Ella reconoció algunos problemas iniciales, pero aseguró que Hazel es “otra herramienta en nuestra caja de herramientas”.
El estado confía en las empresas con fines de lucro
La teleterapia desempeña un papel cada vez más importante en las escuelas del país, a medida que educadores y trabajadores sociales se enfrentan a la presión de abordar los crecientes problemas de salud mental. Según un informe de abril de Chalkbeat, 13 de los 20 distritos escolares más grandes del país, incluido Los Angeles Unified, la han incorporado desde que comenzó la pandemia.
El acuerdo del condado de Los Angeles con Hazel prevé el pago a la empresa de hasta $20 millones hasta finales de 2024. Además, Hazel puede facturar a los seguros de los estudiantes.
La empresa con sede en San Francisco, fundada en 2015, ha recaudado $112,5 millones de inversores y tiene contratos en 15 estados. Entre las empresas que buscan los dólares destinados para la salud mental de los jóvenes están otra startup de San Francisco, Daybreak Health, graduada de la prestigiosa incubadora tecnológica Y Combinator, junto con BeMe, Brightline y Kooth.
California eligió a Brightline y Kooth para una iniciativa estatal de $532 millones, en 2024, sobre servicios virtuales de comportamiento juvenil, otro componente importante del plan maestro de Newsom. Algunos programas estatales y locales se superponen, reconoció Naomi Allen, cofundadora y CEO de Brightline, pero dijo que la oferta de Brightline es más amplia que lo que Hazel hace en las escuelas, con servicios que incluyen desde sesiones de coaching para cuidadores hasta recursos de meditación.
“El estado financia el acceso gratuito a los servicios para todos los niños del estado, lo cual es un programa extraordinariamente ambicioso”, afirmó Allen.
Aún así, quedan muchos interrogantes sobre la eficacia de la teleterapia para estudiantes. Tampoco ha resultado ser una fuente de ingresos segura para las empresas: Brightline despidió al 20% de su plantilla la primavera pasada, la segunda ronda de despidos en seis meses.
Complemento, no solución
Chelsy Duffer-Dunbar, que en aquel momento trabajaba para Los Angeles Unified como trabajadora social psiquiátrica, declaró a KFF Health News en octubre que aún no había trabajado con Hazel, pero señaló que el condado exige que un miembro del personal permanezca a la vista del estudiante durante sus citas y le ayude si surgen problemas técnicos.
“Le sigue quitando tiempo al personal”, aseguró Duffer-Dunbar. “Mi día ya es muy estresante. No puedo imaginar tener una evaluación por amenaza y otra por suicidio en el trabajo y luego tener que buscar a alguien para que se siente en esta sesión de terapia con el niño o la niña y su iPad”.
Duffer-Dunbar añadió que quiere que el distrito dé prioridad a los terapeutas en persona que trabajan con la comunidad local, especialmente para los niños más pequeños que tienen problemas con la teleterapia.
Duffer-Dunbar ha dejado el distrito por recortes presupuestarios que la obligaban a desempeñar un trabajo más agobiante.
Hazel insistió en que la teleterapia no es una solución para todas las situaciones.
“Es una oportunidad para ampliar el acceso”, apuntó Andrew Post, jefe de innovación de la empresa.
Colaboración entre educación y salud
Fue necesaria una complicada colaboración entre los distritos escolares, las agencias del condado y los dos planes de Medi-Cal, L.A. Care Health Plan y Health Net, para poner en marcha el programa de terapia escolar. Las normas de financiación estatales se diseñaron para ayudar a las entidades a trabajar juntas.
“Este programa nos ha ayudado a acercarnos a los distritos escolares”, comentó Michael Brodsky, director de salud comunitaria de L.A. Care Health Plan. “Si podemos tratar a los niños cuando van a la escuela y derivarlos para que reciban tratamiento mientras están en la escuela, eso es bueno”.
Hazel ofrece principalmente sesiones de terapia individual de corta duración con trabajadores sociales clínicos u otros consejeros, el 40% de los cuales son bilingües. Son los más indicados para prestar apoyo temporal a quienes tienen necesidades leves o moderadas, como los estudiantes que luchan contra el estrés académico o empiezan en una escuela nueva, pero también pueden derivar a pacientes para que reciban atención a largo plazo.
El mayor distrito inscrito en el programa, Los Angeles Unified, cuenta con el 41% de los alumnos del condado, pero no todos los distritos están preparados para dar el salto. Cuatro de cada 10 distritos han optado por no ofrecer los servicios de Hazel, lo que Garoupa atribuye en parte a la preocupación por el intercambio de información sobre los estudiantes.
El contrato con Hazel termina en diciembre de 2024, pero Garoupa dijo que la Oficina de Educación y sus socios tienen la intención de mantener los servicios hasta junio de 2025. Cualquier prórroga posterior dependerá de los resultados.
Sonya Smith, colega de Garoupa, indicó que la Oficina de Educación evaluará la eficacia de Hazel a través de una encuesta anual, informes mensuales de impacto y reuniones semanales.
“El número de estudiantes que utilizan Hazel va a ser, obviamente, una medida clave”, añadió Smith. “La tasa de utilización de Hazel es del 3% al 8%. Evaluaremos si esas cifras se mantienen, si los estudiantes acceden a la atención en el momento oportuno y si alivia la carga del personal escolar y los proveedores comunitarios”.
Esta historia fue producida por KFF Health News, que publica California Healthline, un servicio editorialmente independiente de la California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 6 months ago
california, Mental Health, Noticias En Español, States, Children's Health, Latinos, Telemedicine