A Peek at Big Pharma’s Playbook That Leaves Many Americans Unable to Afford Their Drugs
America’s pharmaceutical giants are suing this summer to block the federal government’s first effort at drug price regulation.
America’s pharmaceutical giants are suing this summer to block the federal government’s first effort at drug price regulation.
Last year’s Inflation Reduction Act included what on its face seems a modest proposal: The federal government would for the first time be empowered to negotiate prices Medicare pays for drugs — but only for 10 very expensive medicines beginning in 2026 (an additional 15 in 2027 and 2028, with more added in later years). Another provision would require manufacturers to pay rebates to Medicare for drug prices that increased faster than inflation.
Those provisions alone could reduce the federal deficit by $237 billion over 10 years, the Congressional Budget Office has calculated. That enormous savings would come from tamping down drug prices, which are costing an average of 3.44 times — sometimes 10 times — what the same brand-name drugs cost in other developed countries, where governments already negotiate prices.
These small steps were an attempt to rein in the only significant type of Medicare health spending — the cost of prescription drugs — that has not been controlled or limited by the government. But they were a call to arms for the pharmaceutical industry in a battle it assumed it had won: When Congress passed the Medicare prescription drug coverage benefit (Part D) in 2003, intense industry lobbying resulted in a last-minute insertion prohibiting Medicare from negotiating those prices.
Without any guardrails, prices for some existing drugs have soared, even as they have fallen sharply in other countries. New drugs — some with minimal benefit — have enormous price tags, buttressed by lobbying and marketing.
AZT, the first drug to successfully treat HIV/AIDS, was labeled “the most expensive drug in history” in the late 1980s. Its $8,000-a-year cost was derided as “inhuman” in a New York Times op-ed. Now, scores of drugs, many with much less benefit, cost more than $50,000 a year. Ten drugs, mostly used to treat rare diseases, cost over $700,000 annually.
Pharmaceutical manufacturers say high U.S. prices support research and development and point out that Americans tend to get new treatments first. But recent research has shown that the price of a drug is related neither to the amount of research and development required to bring it to market nor its therapeutic value.
And selling drugs first in the U.S. is a good business strategy. By introducing a drug in a developed country with limited scrutiny on price, manufacturers can set the bar high for negotiating with other nations.
Here are just a few of the many examples of drug pricing practices that have driven consumers to demand change.
Exhibit A is Humira, the best-selling drug in history, earning AbbVie $200 billion over two decades. Effective in the treatment of various autoimmune diseases, its core patent — the one on the biologic itself — expired in 2016. But for business purposes, the “controlling patent,” the last to expire, is far more important since it allows an ongoing monopoly.
AbbVie blanketed Humira with 165 peripheral patents, covering things like a manufacturing step or slightly new formulation, creating a so-called patent thicket, making it challenging for generics makers to make lower-cost copycats. (When they threatened to do so, AbbVie often offered them valuable deals not to enter the market.) Meanwhile, it continued to raise the price of the drug, most recently to $88,000 a year. This year, Humira-like generics (called biosimilars for its type of molecule) are entering the U.S. market; they have been available for a fraction of the price in Europe for five years.
Or take Revlimid, a drug by Celgene (now part of Bristol Myers Squibb), which treats multiple myeloma. It won FDA approval to treat that previously deadly disease in 2006 at about $4,500 a month; today it retails at triple that. Why? The company’s CEO explained price hikes were simply a “legitimate opportunity” to improve financial “performance.”
Since it must be taken for life to keep that cancer in check, patients who want to live (or their insurers) have had no choice but to pay. Though Revlimid’s patent protection ran out in 2022, Celgene avoided meaningful price-cutting competition by offering generic competitors “volume-limited licenses” to its patents so long as they agreed to initially produce a small share of the drug’s $12 billion monopoly market.
Par Pharmaceutical, another drugmaker, maneuvered to create a blockbuster market out of a centuries-old drug, isoproterenol, through a well-meaning FDA program that gave companies a three-year monopoly in exchange for performing formal testing on drugs in use before the agency was formed.
During those three years, Par wrapped its branded product, Vasostrict, used to maintain blood pressure in critically ill patients, with patents — including one on the compound’s pH level — extending its monopoly eight additional years. Par raised the price by 5,400% between 2010 and 2020. When the covid-19 pandemic filled intensive care units with severely ill patients, that hike cost Americans $600 million to $900 million in the first year.
And then there is AZT and its successors, which offer a full life to HIV-positive people. Pills today contain a combination of two or three medicines, the vast majority including one similar to AZT, tenofovir, made by Gilead Sciences. The individual medicines are old, off-patent. Why then do these combination pills, taken for life, sometimes cost $4,000 monthly?
It’s partly because many manufacturers of the combination pills have agreements with Gilead that they will use its expensive branded version of tenofovir in exchange for various business favors. Peter Staley, an activist with HIV, has been spearheading a class-action suit against Gilead, alleging “collusion.” The negotiated price for these pills is hundreds of dollars a month in the United Kingdom, not the thousands charged in the U.S.
Faced with such tactics, 8 in 10 Americans now support drug price negotiation, giving Congress and the Biden administration the impetus to act and to resist Big Pharma’s legal challenges, which many legal experts view as a desperate attempt to stave off the inevitable.
“I don’t think they have a good legal case,” said Aaron Kesselheim, who studies drug pricing at Harvard Medical School. “But it can delay things if they can find a judge to issue an injunction.” And even a year’s delay could translate into big money.
Yes, American patients are lucky to have first access to innovative drugs. And, sadly, patients in countries that refuse to pay up once in a while go without the latest treatment. But more sadly, polling shows, large numbers of Americans are forgoing prescribed medicines because they can’t afford them.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 2 months ago
Health Care Costs, Health Care Reform, Health Industry, Pharmaceuticals, Drug Costs, Legislation, Prescription Drugs
KFF Health News' 'What the Health?': On Abortion Rights, Ohio Is the New Kansas
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
Ohio voters — in a rare August election — turned out in unexpectedly high numbers to defeat a ballot measure that would have made it harder to pass an abortion-rights constitutional amendment on the ballot in November. The election was almost a year to the day after Kansas voters also stunned observers by supporting abortion rights in a ballot measure.
Meanwhile, the percentage of Americans without health insurance dropped to an all-time low of 7.7% in early 2023, reported the Department of Health and Human Services. But that’s not likely to continue, as states boot from the Medicaid program millions of people who received coverage under special eligibility rules during the pandemic.
This week’s panelists are Julie Rovner of KFF Health News, Emmarie Huetteman of KFF Health News, Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico, and Rachel Roubein of The Washington Post.
Panelists
Emmarie Huetteman
KFF Health News
Joanne Kenen
Johns Hopkins Bloomberg School of Public Health and Politico
Rachel Roubein
The Washington Post
Among the takeaways from this week’s episode:
- It should not have come as much of a surprise that Ohio voters sided with abortion-rights advocates. Abortion rights so far have prevailed in every state that has considered a related ballot measure since the Supreme Court overturned Roe v. Wade, including in politically conservative states like Kentucky and Montana.
- Moderate Republicans and independents joined Democrats in defeating the Ohio ballot question. Opponents of the measure — which would have increased the threshold of votes needed to approve state constitutional amendments to 60% from a simple majority — had not only cited its ramifications for the upcoming vote on statewide abortion access, but also for other issues, like raising the minimum wage.
- A Texas case about exceptions under the state’s abortion ban awaits the input of the state’s Supreme Court. But the painful personal experiences shared by the plaintiffs — notable in part because such private stories were once scarce in public discourse — pressed abortion opponents to address the consequences for women, not fetuses.
- The uninsured rate hit a record low earlier this year, a milestone that has since been washed away by states’ efforts to strip newly ineligible Medicaid beneficiaries from their rolls as the covid-19 public health emergency ended.
- The promise of diabetes drugs to assist in weight loss has attracted plenty of attention, yet with their high price tags and coverage issues, one thorny obstacle to access remains: How could we, individually and as a society, afford this?
- Lawmakers are asking more questions about the nature of nonprofit, or tax-exempt, hospitals and the care they provide to their communities. But they still face an uphill battle in challenging the powerful hospital industry.
Also this week, Rovner interviews Kate McEvoy, executive director of the National Association of Medicaid Directors, about how the “Medicaid unwinding” is going as millions have their eligibility for coverage rechecked.
Plus, for “extra credit” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: KFF Health News’ “How the Texas Trial Changed the Story of Abortion Rights in America,” by Sarah Varney.
Joanne Kenen: Fox News’ “Male Health Care Leaders Complete ‘Simulated Breastfeeding Challenge’ at Texas Hospital: ‘Huge Eye-Opener’,” by Melissa Rudy.
Rachel Roubein: Stat’s “From Windows to Wall Art, Hospitals Use Virtual Reality to Design More Inclusive Rooms for Kids,” by Mohana Ravindranath.
Emmarie Huetteman: KFF Health News’ “The NIH Ices a Research Project. Is It Self-Censorship?” by Darius Tahir.
Also mentioned in this week’s episode:
- Politico’s “Abortion Rights Won Big in Ohio. Here’s Why It Wasn’t Particularly Close,” by Madison Fernandez, Alice Miranda Ollstein, and Zach Montellaro.
- KFF Health News’ “Seeking Medicare Coverage for Weight Loss Drugs, Pharma Giant Courts Black Influencers,” by Rachana Pradhan.
- Stat’s “Alarmed by Popularity of Ozempic and Wegovy, Insurers Wage Multi-Front Battle,” by Elaine Chen.
click to open the transcript
Transcript: On Abortion Rights, Ohio Is the New Kansas
KFF Health News’ ‘What the Health?’Episode Title: On Abortion Rights, Ohio Is the New KansasEpisode Number: 309Published: Aug. 10, 2023
[Editor’s note: This transcript, generated using transcription software, has been edited for style and clarity.]
Julie Rovner: Hello and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News, and I’m joined by some of the best and smartest health reporters in Washington. We’re taping a day early this week, on Wednesday, Aug. 9, at 3:30 p.m. As always, news happens fast, and things might have changed by the time you hear this. So here we go. We are joined today via video conference by Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico.
Joanne Kenen: Hey, everybody.
Rovner: Rachel Roubein of The Washington Post.
Rachel Roubein: Hi, everybody.
Rovner: And my colleague and editor here at KFF Health News Emmarie Huetteman.
Emmarie Huetteman: Hey, everyone. Glad to be here.
Rovner: So later in this episode, we’ll have my interview with Kate McEvoy, executive director of the National Association of Medicaid Directors. She’s got her pulse on how that big post-public health emergency “Medicaid unwinding” is going. And she’ll share some of that with us. But first, this week’s news. I guess the biggest news of the week is out of Ohio, which, in almost a rerun of what happened in Kansas almost exactly a year ago, voters soundly defeated a ballot issue that would have made it harder for other voters this fall to reverse the legislature’s strict abortion ban. If you’re having trouble following that, so did they in Ohio. [laughs] This time, the fact that the abortion rights side won wasn’t as much of a surprise because every statewide abortion ballot question has gone for the abortion rights side since Roe v. Wade was overturned last year. What do we take away from Ohio? Other than it looked a lot like … the split looked a lot like Kansas. It was almost 60-40.
Kenen: It shows that there’s a coalition around this issue that is bigger than Democrat or Republican. Ohio was the classic swing state that has turned into a conservative Republican-voting state — not on this issue. This was clearly independents, moderate Republicans joined Democrats to … 60-40, roughly, is a pretty big win. Yes, we’ve seen it in other states. It’s still a pretty big win.
Roubein: I agree. And I think one of my colleagues, Patrick Marley, and I spent some time just driving around and traveling Ohio in July. And one of the things that we did find is that — this ballot measure to increase the threshold for constitutional amendments is 60% — it had in some, in many, ways turned into a proxy war over abortion. But, in some ways, both sides also didn’t talk about abortion when they were, you know, canvassing different voters. You know, they use different tools in the toolbox. I was following around someone from Ohio Right to Life and, you know, he very much said, “Abortion is the major issue to me.” But, you know, they tried to kind of bring together the side that supported this. Other issues like legalizing marijuana and raising the minimum wage, and, you know, the abortion rights side was very much a part of, you know, the opposition here. But when some canvassers went out — my colleague Patrick had traveled and followed some, and some, you know, kind of focused on other issues like, you know, voters having a voice in policy and keeping a simple majority rule.
Rovner: Yeah, I think it’s important — for those who have not been following this as closely as we have — what the ballot measure was was to make future ballot measures — and they said they were not going to have them in August anymore, which, this was the last one — in order to amend the constitution by referendum, you would need a 60% majority rather than a 50% majority. And just coincidentally, there is an abortion ballot measure on Ohio’s ballot for November, and it’s polling at about 58%. But, yes, this would have applied to everything, and it was defeated.
Kenen: And it’s part of a larger trend. It began before the overturning of Roe v. Wade. Over the last couple of years, you’ve seen conservative states move to tighten these rules for ballot initiatives. And that’s because more liberal positions have been winning. I mean, Medicaid, the Medicaid expansion on the ballot, has won, and won big. Only one was even close …
Rovner: In very red states!
Kenen: They often won very big in a number of very, very conservative states, places like Idaho and Nebraska. So, you know, there’s always been … the conventional wisdom is that, you know, the political parties are more extreme than many voters, that the Democratic Party is for the left and the Republican Party is for the right. And there are a lot of people who identify with one party or the other but aren’t … who are more moderate or, in this case, more liberal on Medicaid. And Medicaid … what was it, seven states? I think it’s seven. Seven really conservative states. And then the abortion has won in every single state. And there’s a little bit of conversation and it’s … very early. And I don’t know if it’s going to go anywhere, but if I’ve heard it and written a bit about it, conservative lawmakers have heard about it, too, which is there are groups interested in trying to get some gun safety initiatives on ballots. So that’s complicated. And it may not happen. But they’re seeing, I mean, that’s the classic example of both a criminal justice and a public health issue — so we can talk about it — a classic example where the country is much more in the center.
Rovner: Well, let us move to Texas, because that’s where we always end up when we talk about abortion. You may remember that lawsuit where several women who nearly died from pregnancy complications sued the state to clarify when medical personnel are able to intercede without being subjected to fines and/or jail sentences. Well, the women won, at least for a couple of days. A Texas district judge who heard the case ruled in their favor, temporarily blocking the Texas ban for women with pregnancy complications. But then the state appealed, and a Texas appeals court blocked the lower-court judge’s blocking of part of the ban. If you didn’t follow that, it just means that legally nothing has changed in Texas. And now the case goes to the Texas Supreme Court, which has a conservative majority. So we pretty much know what’s going to happen. But whether these women ultimately win or lose their case may not be the most important thing. And, to explain why I’m going to do my extra credit early this week. It’s by my KFF Health News colleague Sarah Varney. It’s called “How the Texas Trial Changed the Story of Abortion Rights in America.” She writes that this trial was particularly significant because it put abortion foes on the defensive by graphically depicting harm to women of abortion bans — rather than to fetuses. And it’s also about the power of people publicly telling their stories. I’ve done a lot of stories over the years about women whose very wanted pregnancies went very wrong, very late. And, I have to tell you, it’s been hard to find these women. And when you find them, it’s been really hard to get them to talk to a journalist. So, the fact that we’re seeing more and more people actually come out publicly, you know, may do for this issue what, you know, perhaps what gay rights, you know, what people coming out as gay did for gay marriage? I don’t know. What do you guys think?
Kenen: Well, I think these stories have been really compelling, but they’re also, they’re the most dramatic and maybe easiest to push back. But it’s, you know, there’s a whole lot of other reasons women want abortions. And the focus — and it’s life and death, so the focus, quite rightfully, has to be on these really extreme cases. But that’s not … it’s still in some ways shifting attention from the larger political discussion about choice and rights. But, clearly, some of these states, we’ve seen so many stories of women who, their lives are at stake, their doctors know it, and they just don’t think they have the legal power; they’re afraid of the consequences if they’re second-guessed. There are tremendous financial and imprisonment [risks] for a doctor who is deemed to have done an unnecessary abortion. And this idea that’s taken hold … among some conservatives is that there’s never a need for a medical abortion. And that’s just not true.
Rovner: And yet, I mean, what this trial and a lot of things in Sarah’s piece too point out is that that line between miscarriage and abortion is really kind of fuzzy in a lot of cases. You know, if you go to the hospital with a miscarriage and they’re going to say, “Well, did you initiate this miscarriage?” And we’ve seen women thrown in jail before for losing pregnancies, with them saying, “You know, you threw yourself down the stairs to end this pregnancy.” That actually happened, I think it was in Indiana. So this is —
Kenen: And miscarriage is very common.
Rovner: That was what I was saying.
Kenen: Early miscarriage is very common. Very, very common.
Huetteman: One of the things that’s so striking about the past year, since Dobbs overturned Roe v. Wade ,is that we’ve seen this kind of national education about what pregnancy is and how dangerous it can be and how care needs to really be flexible to meet those sorts of challenges. And this actually got me thinking about something that another familiar voice on this podcast, Alice Miranda Ollstein, and some colleagues wrote this morning about the Ohio outcome, which is they pointed out that the anti-abortion movement really hasn’t evolved in terms of the arguments that they’re making in the past year about why abortion should continue to be less and less available. Meanwhile, we’ve got these, like, really incredible, really emotional, moving stories from women who have experienced this firsthand. And that’s a hard message to overcome when you’re trying to reach voters in particular.
Rovner: And it’s interesting; both sides like to take — you know, they all go to the hardest cases. So, for years and years, the anti-abortion side has, you know, has gone to the hardest cases. And that’s why they talk about abortion in the ninth month up till birth, which isn’t a thing, but they talk about it. And you know, now the abortion rights side has some hard cases now that abortions are harder to get. Well, while we are on the subject of Texas lawsuits, States Newsroom — and thank you for sending this my way, Joanne — has a story reporting that the publisher of the scientific paper that both the lower court judge and the appeals court judges used to conclude that the abortion drug mifepristone causes frequent complications — it does not — is being reviewed for potential scientific misconduct. The paper comes from the Charlotte Lozier Institute, which is the research arm of the anti-abortion group the Susan B. Anthony List. Sage, which is the publisher of the journal that the paper appeared in, has posted something called an expression of concern, saying that the publisher and editor, quote, “were alerted to potential issues regarding the representation of data in the article and author conflicts of interest. SAGE has contacted the authors of this article and an investigation is underway.” This was sort of a whistleblower by a pharmacist who looked at the way the data in this paper was put together and says, “No, that’s really very misleading.” I don’t think I’ve ever seen this, though; I’ve never seen a scientific paper that’s now being questioned for its political bent, a peer-reviewed scientific paper. I mean, this could change a lot of things, couldn’t it?
Kenen: Well, not if people decide that they still think it’s true. I mean, look at — you know, the vaccine autism paper was retracted. That wasn’t initially political. It’s become more political over the years; it wasn’t political at the time. That was retracted. And people have been jumping up and down screaming, “It was retracted! It was retracted!” And, you know, millions of people still believe it. So, I mean, legally, I’m not sure how much it changes. I mean, I thought we had all heard that there were flaws in this study. This article was good because I hadn’t been aware of how deeply flawed and in all the many ways it was flawed. And also the whistleblower yarn was interesting. I’m not sure how much it changes anything.
Rovner: Well, I’m thinking not in terms of this case. And by the way, I think we didn’t say this, that the study was of emergency room visits by women who’d had either surgical or medical abortions. And the contention was that medical abortions were more dangerous than surgical abortions because more women ended up in the emergency room. But as several people have pointed out, more people ended up in the emergency room after medical abortions because there have been so many more medical abortions over the years. I mean, you don’t actually have to be a data scientist to see some of the problems.
Kenen: Right. And some of them also weren’t that — really, were nervous, and they didn’t know what was normal and they went to the ER because they were scared and they really were safe. They were not — they didn’t need — you know, they just weren’t sure how much pain and discomfort or bleeding you’re supposed to have. And they went and they were reassured and were sent home. So it’s not even that they really had a medical emergency or that they were harmed.
Rovner: Or that they had a complication.
Kenen: Right. There were many flaws pointed out with this research.
Rovner: But my broader question is, I mean, if people are going to start questioning the politics of scientific papers, I mean, I could see the other side going after this.
Kenen: Well, there’s climate science, too, that’s bad. I mean, I don’t think this is actually unique. I think it’s egregious. But there were studies minimizing the risk of smoking, which was also a political business, commercial. Climate is certainly political. I mean, I think this is sort of the most politicized and most acute example, but I don’t think it’s the only one.
Roubein: And I think, Julie, as you’d mentioned, I think when [U.S. District Judge] Matthew Kacsmaryk in Texas came down with his decision — you know, for instance, there are media outlets — that my colleagues at the Post did a story just kind of unpacking some of the kind of flaws and some of the studies that were used to make, you know, a court decision.
Rovner: Yeah, to give the judge what he assumes to be evidence that this is a dangerous drug. So it’s — yeah.
Kenen: Which he came in believing, we know, from the profiles of him and his background.
Rovner: Right. All right, well, let us move on. The official Census Bureau estimate of how many people lack health insurance won’t be out until next month. But the Department of Health and Human Services is out with a report based on that other big federal population survey that shows the uninsured rate early this year was at its lowest level since records started being kept, which I think was in the 1980s: 7.7%. Now, that’s clearly going to be the high point for the fewest number of people uninsured, at least for a while, because clearly not all of the millions of people who are losing or about to lose their Medicaid coverage are going to end up with other insurance. But I remember — Joanne, you will, too — when the rate was closer to 18% … was a huge news story, and the thing that triggered the whole health reform debate in the first place. I’m surprised that there’s been so little attention paid to this.
Kenen: Because, you know … [unintelligible] … it’s so yesterday. And also, as you alluded to, you know, we’re in the middle of the Medicaid unwinding. So the numbers are going up again now. And we don’t know. We know that it’s a couple of million people. I think 3 million might be the last —
Rovner: I think it’s 4 [million], it’s up to 4.
Kenen: Four, OK. And some of them will get covered again and some of them will find other sources of coverage. But right now, there’s an uptick, not a downtick.
Roubein: And I think when you look at just, like, estimates of what the insured and the uninsured rates would be in 2030, like, the CMS’ [Centers for Medicare & Medicaid Services] analysis, one of the other questions is, you know, whether the enhanced Obamacare subsidies continue past 2025. So there’s Medicaid and then there’s also some other kind of question marks and cliffs coming up on how and whether it will fluctuate.
Rovner: No, it’s worth watching. And remember, when the census numbers come out, those will be for 2022. Well, moving on, we have two stories this week looking at the potential cost of those breakthrough obesity drugs, but through two very different lenses. One is from my KFF Health News colleague Rachana Pradhan, details how the makers of the current “it” drug, Ozempic, which is Novo Nordisk, in an effort to get the votes to lift the Medicare payment ban on weight loss drugs, is quietly contributing large amounts of money to groups like the Congressional Black Caucus Foundation and the Congressional Hispanic Caucus Institute. It’s sort of a backdoor lobbying that’s pretty age-old, but that doesn’t mean it doesn’t work. The other story, by Elaine Chen at Stat, looks at how health insurers are pushing back hard against the off-label use of diabetes medications that also work to help people lose weight. They’re doing things like allowing the more expensive weight loss drugs only if people have tried and failed other methods or disallowing them if the other methods had been slightly successful. So, if you take a lesser drug and you lose enough weight, they won’t let you take the better drug because, look, you lost weight on the other drug. We’ve talked about this, obviously, before: These drugs, on the one hand, have the potential to make a lot of people both healthier and happier. There’s a study out this week that shows that Mounjaro, the Eli Lilly drug, actually reduces heart disease by 20%.
Kenen: In people who have heart disease.
Rovner: Right, in people who have heart disease.
Kenen: It’s not lowering everybody’s risk.
Rovner: But still, I mean, everybody’s — well, I mean, there are medical indications for using these drugs for weight loss. But if everybody who wants them could get them, it would literally break the bank. Nobody can afford to give everybody who’s eligible for these drugs these drugs. Is the winner here going to be the side with the most effective lobbying, or is that too cynical?
Huetteman: Isn’t that always the winner? Speaking of cynical.
Rovner: Yeah, in health care.
Kenen: Well, I mean, I also think there’s questions about, like, these drugs clearly are really wonderful for people who they were designed for; you don’t have to be on insulin. They’re having not just weight loss and diabetes. There are apparently cardiac and other — you know, these are probably really good drugs. But there are a lot of people who do not have diabetes or heart disease who want them because they want to lose 20 pounds. And some of them are being told you have to take it for the rest of your life. I mean, I just know this anecdotally, and I’m sure we all know it anecdotally.
Rovner: Right. It’s like statins.
Kenen: Yes.
Rovner: Or blood pressure medication. If you stop taking your blood pressure medication, your blood pressure goes back up.
Kenen: Right. So, I mean, should the goal for the weight loss be, “OK, this is going to help you take off that weight and then you’re going to have to maintain it through diet and exercise and healthy lifestyle,” blah, blah, blah, which is hard for people. We know that. Or are we putting healthy people on a really expensive drug that changes an awful lot of things about their body indefinitely? We don’t have safety data for lifelong use in otherwise healthy people. So, you know, I’m always a little worried because even the best clinical trial is small compared to the entire — it’s small and it’s time-limited. And maybe these drugs are going to turn out to be absolutely phenomenal and we’re going to all live another 20 healthy years. But maybe not, you know. Or maybe they’re going to be really great for a certain subpopulation, but, you know, we’re not going to want to put it in the water supply. So, I still think that there’s this sort of pell-mell rush. And I think it’s partly because there’s a lot of money at stake. And it’s also, like, most people who are overweight have tried to lose it, and it’s very difficult to lose and maintain weight. So, you know, people want an easier way to do it. And I think the other thing is right now it’s an injection. There are side effects for some people on discomfort. There probably will be an oral version, a pill, sometime fairly soon, which will open — you know, there are people who don’t want to take a shot who would take a pill. It also means you might be able to tell — I mean, I don’t know the science of the pills, but it would make sense to me that you could take a lower dose, you know, maybe ease into it without the side effects, or could you stay on it longer with fewer problems? I mean, we’re just the very beginning of this, but it’s a huge amount of money.
Rovner: Yeah. You could see — I mean, my big question, though, is why can’t we force the drugmakers to lower the price? That would, if not solve the problem, make it a lot better. I mean, really, we’re going to have to wait until there is generic competition?
Kenen: It’s not just this.
Rovner: Yeah.
Kenen: I mean, it’s all sorts of cancer treatments and it’s hepatitis treatments. And it’s, I mean, there’s a lot of expensive drugs out there. So, this one just has a lot of demand because it makes you skinny.
Rovner: Well, that was the thing. We went through this with the hepatitis C drugs, which were really super expensive. It’s much more like that.
Kenen: Well, they seemed super expensive at the time —
Rovner: Not so much anymore.
Kenen: — but maybe for a thousand dollars, in retrospect.
Rovner: All right. Well, let’s move on. So, speaking of powerful lobbies, let’s talk about hospitals. Iowa Republican Sen. Chuck Grassley and Massachusetts Democrat Elizabeth Warren — now, there is an unlikely couple — are among those asking the IRS to more carefully examine tax-exempt hospitals to make sure they’re actually benefiting the community in exchange for not paying taxes, which is supposed to be the deal. Now, Sen. Grassley has been on this particular hobbyhorse for many, many years, I think probably more than 20, but not much ever seems to come of this. I can’t tell you how many workshops I’ve been to on, you know, how to measure community benefits that tax-exempt hospitals are providing. Any inkling that this time is going to be any different?
Roubein: Well, hospitals don’t tend to be sort of the losers. They try and kind of frame themselves as, like, “We’re your sort of friendly neighborhood hospital,” and every — I mean, every congressman, most congressmen have, you know, hospitals in their district. So they they get lobbied a lot, though, you know — I mean, this is a different issue, but particularly on the House side, hospitals are facing site-neutral payments, which if that actually went through Congress would be a loss. So yeah, but lawmakers have found it in general hard to take on the hospital industry.
Rovner: Yeah, very much so.
Kenen: Yeah. I mean, I think that we think of nonprofits and for-profits as, they’re different, but they’re not as different as we think they are, in that, you know, nonprofits are getting a tax break and they have to reinvest their profits. But it doesn’t mean they’re not making a lot of money. Some of them are. I mean, some of them have, you know, we’ve all walked into fancy nonprofits with, you know, fancy art and marble floors and so on and so forth. And we’ve all been in nonprofits that are barely keeping their doors open. So it’s your tax status. It’s not really, you know, your ethical status or the quality of care. I mean, there’s good nonprofits, there’s good for-profits. You know, this whole thing is like, if I were a hospital, I would be getting this huge tax break, and what am I doing to deserve it? And that’s the question.
Rovner: And I think the argument is, you know, that the 7.7% uninsured we were talking about, that hospitals are supposed to be providing care as part of their community benefit that the federal government now is ending up paying for. I think that’s sort of the frustration. If nonprofit hospitals were doing what they were supposed to do, it would cost federal and state governments less money, which always surprises me because this is not gone after more. I mean, Grassley has spent his whole career working on various types of government fraud. So this is totally in line for him. But it’s never just seemed to be a big priority for any administration.
Huetteman: There’s a little bit of an X factor here. Look at the fact that Grassley and Warren are talking about this publicly now. Maybe I’m just really optimistic from all the journalism we’ve been doing about projects like “Bill of the Month.” But the reality is that a lot of people are now seeing reporting that’s showing to them what nonprofit hospitals are actually doing when it comes to pursuing patients who don’t pay bills. And what it means to have community benefit comes into question a lot when you talk about wage garnishment, suing patients who are low-income for their medical debt. These are things that journalists have uncovered over and over again, happening at — ding, ding, ding — nonprofit hospitals. It’s harder to argue that hospitals are just doing their best for people when you have these stories of poor people who are losing their homes over unpaid medical bills, for instance. And I think that right now, when we’re in this political moment where health care costs are so, so potent to people and so important, I mean, could we see that this will actually be more effective, that we’re heading towards something that’s more effective? Maybe.
Rovner: Well, repeats the journalist, as we all are, the power of storytelling. Definitely the public is primed. I imagine that’s why they’re doing it now. We’ll see what comes of it.
Kenen: think the public is primed for bad practices. I’m not sure how many patients understand if the hospital they go to is a nonprofit or a for-profit. I think the public understands that everything in health care costs too much and that there are bad actors and greed. There’s a difference between profit and greed, and I think many people would say that we’re now in an era of greed. And not everybody in the health care sector — before anybody calls us up and shouts, “Not everybody who provides care is greedy” — but we’ve seen, you know, it is clearly out there. You know, you had Zeke Emanuel on a couple of weeks ago. Remember what he said, that, you know, 10 years ago, some people still liked their health care and now nobody likes their health care, rich or poor.
Rovner: Yeah, he’s right. All right. Well, that is this week’s news. Now, we’ll play my interview with Kate McEvoy of the National Association of Medicaid Directors about how the Medicaid unwinding is going. And one note before you listen: Kate frequently refers to the federal CMCS, which is not a misspeak; it stands for the Center for Medicaid and CHIP Services, which is the branch of CMS, the Centers for Medicare & Medicaid Services, that deals with Medicaid. So, here’s the interview:
I am pleased to welcome to the podcast Kate McEvoy, executive director of the National Association of Medicaid Directors, which is pretty much exactly what the name says, a group where state Medicaid officials can share information and ideas. Kate, welcome to “What the Health?”
Kate McEvoy: Good afternoon. Thanks for having me.
Rovner: Obviously, the Medicaid unwinding, which we have talked about a lot on the podcast, is Topic A for your members right now. Remind us again which Medicaid recipients are having their coverage eligibility rechecked? It’s not just those in the expansion group from the Affordable Care Act, right?
McEvoy: It’s not, no. Each and every person served by the country nationwide has to be reevaluated from an eligibility standpoint this year.
Rovner: What do we know about how it’s going? We’re seeing lots of reports that suggest the vast majority of people losing coverage are for paperwork reasons, not because they’ve been found to be no longer eligible. I know you recently surveyed your members. What are they telling you about this?
McEvoy: So, I first want to say this is an unprecedented task and it’s obviously historically significant for everyone served by the program. The volume of the work, and also the complexity, makes it a challenging task for all states and territories. But what we are seeing to date is a few things. First, we have seen an incredible effort on the part of states and territories to saturate really every means of communicating with their membership, really getting out that message around connecting with the programs, especially if an individual has moved during the period of the pandemic, which is very typical for people served by Medicaid. So that saturation of messaging and use of new means of connecting with people, like texting, really does represent a tremendous advance for the Medicaid program that has traditionally relied on a lot of complex, formal, legal notices to people. So that seems like a very positive thing. What we are seeing, and this is not unexpected, is that, you know, for reasons related to complex life circumstances and competing considerations, many people are not responding to those notices, no matter how we are transmitting those messages. And so that is a piece that is of great interest and concern to all of us, notably Medicaid directors wanting to make sure that eligible folks do not lose coverage simply because they are not responsive to the requests for more information. So we’re at a point where we’re beyond that initial push around messaging and now are really focused on means of protecting people who remain eligible, either through automatic review of their eligibility — the ex parte process — or by restoring them through such means as reconsideration. That’s really the main focus right now.
Rovner: And there’s that 90-day reconsideration window. Is that … how does that work?
McEvoy: So the federal law gives this period of 90 days to families and children within which they can be renewed with very little effort, essentially removing the responsibility to complete a new application. We also have long-standing help to people called “presumptive eligibility.” So if someone goes to a federally qualified health center or, more unfortunately, goes to the hospital, many of those types of providers can restore someone’s eligibility. So those are important protective pieces. We also know from the survey that you mentioned of our membership that many states and territories are extending those reconsideration protections to all coverage groups — also including older adults and people with disabilities.
Rovner: So are there any states that are doing anything that’s different and innovative? I remember when CHIP [the federal Children’s Health Insurance Program] was being stood up — and boy, that was a long time ago, like 1999 — South Carolina put flyers in pizza boxes, and some other state put flyers in sneaker boxes for back-to-school stuff. Are there better ways to maybe get ahold of these people?
McEvoy: So I think the answer is: a lot of different channels. Our colleagues in Louisiana have a partnership with Family Dollar stores to essentially feature this information on receipts. There’s a lot of work at pharmacy counters. Some of the big chain pharmacies have QR codes and other means of prompting people around their Medicaid eligibility. There’s going to be a big push for the back-to-school effort. And I think CMS and states are really interested, particularly in ensuring that children do not lose coverage even if their parents have regained employment and they’re no longer eligible. Another thing that’s going on is a lot of innovation in the means of enabling access to information. So many states have put in place personal apps through which people can track their own eligibility. There’s interest and some uptake of the so-called pizza-tracker function — so you can kind of see where you’re situated in that pipeline — and also a lot of use of automation to help call people back if they’re trying to get to state call centers. So really, all of those types of strategies … we’re seeing a huge amount of effort across the country.
Rovner: How’s the cooperation going with the Department of Health and Human Services? I know that … they seem to be not happy with some states. Are they being helpful, in general?
McEvoy: They’re being extraordinarily helpful. I would say that we often talk about Medicaid representing a federal-state equity partnership, and we’ve seen that manifest from the beginning of the first notice of the certainty around the start of the unwinding. CMCS has consistently offered guidance to states. They work with states using a mitigation approach as opposed to moving rapidly to compliance. We feel mitigation is the best way of essentially working out the strategies that are going to best protect continuing eligibility for people at the state level. And we really appreciate CMS’ efforts on that. We understand they do have to ensure accountability across the country, and we’re mutually committed to that.
Rovner: You better explain mitigation strategies.
McEvoy: Yeah, so this is a year where we are calling the question on eligibility standards that help ensure that the pathway to Medicaid coverage is a smooth one, and also that there is continuity of coverage. So, for any state that wasn’t yet meeting all those standards, CMCS essentially entered into an agreement with the state or territory to say, here is how you will get there. And that could have involved some means of improving the automatic renewals for Medicaid. It could have meant relying on an integrated eligibility processes. There are a lot of different tools and strategies that were put in place, but essentially that is a path to every state and territory coming into full compliance.
Rovner: Is there anything unexpected that’s happening? I know so much of this was predicted, and it was predicted that the states that went first that, you know, were really in a hurry to get extra people off of their rolls seem to be doing just that: getting extra people off of their rolls. Are you surprised at the differences among states?
McEvoy: I think that there have definitely been differences among states in terms of the tools they have used from a system standpoint, but I don’t see any differences in terms of retention of eligible people. That remains a shared goal across the entire country. And again, this is a watershed point where we have the opportunity to bring everyone to the same standards, ongoing, so that we help to prevent some of the heartache of the eligibility process for folks ongoing.
Rovner: Anything else I didn’t ask?
McEvoy: Well, I think that piece around the reconsideration period is particularly important. We are struck by there being probably less literacy around that option, and that’s something we want to continue to promote. The other piece I’d wind up by saying is that the Medicaid program is always available for people who are eligible. So in the worst-case scenario in which an otherwise eligible person loses coverage, they can always come back and be covered. This is in contrast to private insurance that may have an annual open enrollment period. Medicaid, as you know, is available on a rolling basis, and we want to keep reinforcing that theme so that no one goes with a gap in coverage.
Rovner: Kate McEvoy, thank you very much. And I hope we can call you back in a couple of months.
McEvoy: I would be very happy to hear from you.
Rovner: OK. We are back and it’s time for our extra credit segment. That’s when we each recommend a story we read this week we think you should read too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. I did mine already. Emmarie, why don’t you go next?
Huetteman: My story this week comes from KFF Health News, my colleague Darius Tahir. He has a story called “The NIH Ices a Research Project. Is It Self-Censorship?” Now, the story talks about the fact that the former head of NIH Francis Collins, was, as he was leaving, announcing an effort to study health communications. And we’re talking about not just doctor-to-patient communications, but actually also how mass communications impact American health. But as Darius found out, the acting director quietly ended the program as NIH was preparing to open its grant applications. And officials who spoke with us said that they think political pressure over misinformation is to blame. Now, we don’t have to look too far for examples of conservative pressure over misinformation and information these days. In particular, there’s a notable one from just last month out of a Louisiana court, the federal court decision that blocked government officials from communicating with social media companies. You really don’t have to look too far to see that there’s a chilling effect on information. And we’re talking about the NIH was going to study or rather fund studies into communication and information. Not misinformation, information: how people get information about their health. So it’s a pretty interesting example and a really great story worth your read.
Rovner: And I’ve done nothing but preach about public health communication for three years now.
Kenen: It’s a very good story.
Rovner: Yeah, it was a really good story. Rachel, you’re next.
Roubein: All right. This story is called “From Windows to Wall Art, Hospitals Use Virtual Reality to Design More Inclusive Rooms for Kids,” by Stat News, by Mohana Ravindranath. And I thought this story was really interesting because she kind of dived into what Mohana called “a budding movement to make architecture more inclusive” for the people and patients who are spending a lot, a lot of time in hospital walls. And what some researchers are doing is using virtual reality to essentially gauge how comfortable children who are patients are in hospital rooms. And she talked to researchers at Berkeley who were using these, like, virtual reality headsets to kind of study and explore mocked-up hospital rooms. And, I didn’t know a ton about this field. I mean, apparently it’s not new, but it’s this kind of growing sort of movement to make patients more comfortable in the space that they’re inhabiting for perhaps long periods of time.
Rovner: I went to a conference on architecture, hospital architecture, making it more patient-centered, 10 years ago. But my favorite thing that I still remember from that is they talked about putting art on the ceiling because people are either in bed or they’re in gurneys. They’re looking up at the ceiling a lot. And ceilings are scary in hospitals. So that was one of the things that I took away from that. OK, Joanne, now it’s your turn.
Kenen: OK. This is from Fox News. And yes, you did hear that right. It’s by Melissa Rudy, and the headline is “Male Health Care Leaders Complete ‘Simulated Breastfeeding Challenge’ at Texas Hospital: ‘Huge Eye-Opener’.” So at Covenant Health, they had a bunch of high-level guys in suits pretend they were nursing and/or pumping mothers, and they had to nurse every three hours for 20 minutes at a time. And they found it was quite difficult and quite cumbersome and they didn’t have enough privacy. And as one of them said, “There was no way to multitask.” But trust me, if you have two kids, you have to figure that out, too. So it was a really good story.
Rovner: Some of these things that we feel like should be required everywhere, but it was a great read; it was a really good story. OK, that is our show for this week. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us too. Special thanks this week to Zach Dyer, sitting in for the indefatigable Francis Ying. And as always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can tweet me or X me or whatever; I’m @jrovner. And also on Bluesky and Threads. Rachel?
Roubein: @rachel_roubein — that’s on Twitter.
Rovner: Joanne.
Kenen: In most places I’m @JoanneKenen. On Threads, I’m @joannekenen1.
Rovner: Emmarie.
Huetteman: And I am @emmarieDC.
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
Zach Dyer
Senior Audio Producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ “What the Health?” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 2 months ago
Courts, Health Industry, Insurance, Multimedia, Pharmaceuticals, Public Health, States, Abortion, Drug Costs, KFF Health News' 'What The Health?', Obesity, Ohio, Podcasts, texas, Women's Health
The Real Costs of the New Alzheimer’s Drug, Most of Which Will Fall to Taxpayers
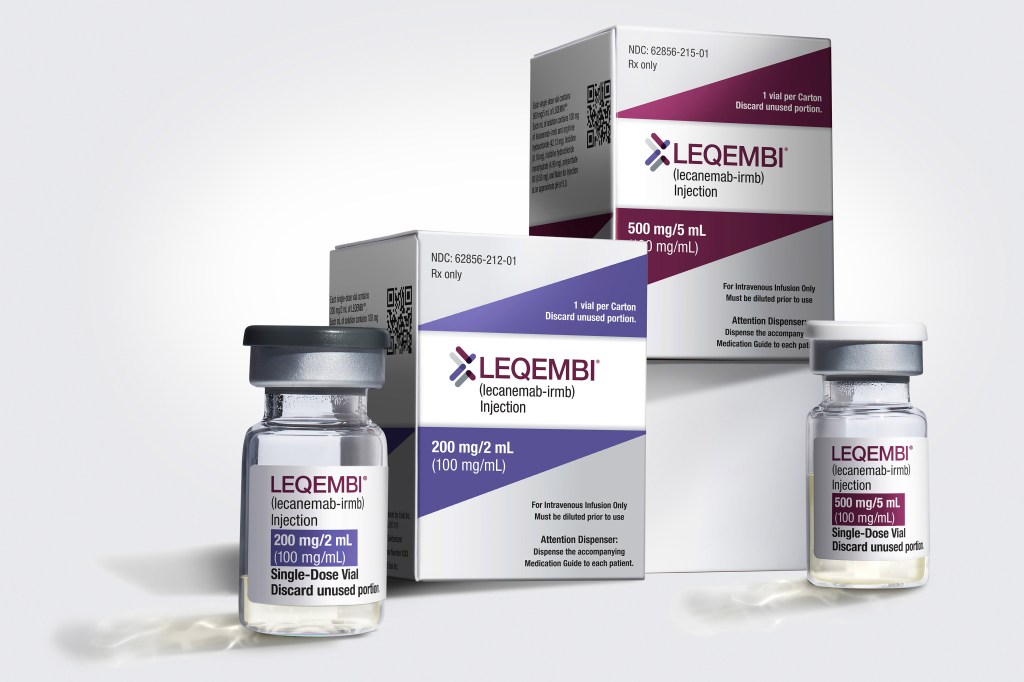
The first drug purporting to slow the advance of Alzheimer’s disease is likely to cost the U.S. health care system billions annually even as it remains out of reach for many of the lower-income seniors most likely to suffer from dementia.
Medicare and Medicaid patients will make up 92% of the market for lecanemab, according to Eisai Co., which sells the drug under the brand name Leqembi. In addition to the company’s $26,500 annual price tag for the drug, treatment could cost U.S. taxpayers $82,500 per patient per year, on average, for genetic tests and frequent brain scans, safety monitoring, and other care, according to estimates from the Institute for Clinical and Economic Review, or ICER. The FDA gave the drug full approval July 6. About 1 million Alzheimer’s patients in the U.S. could qualify to use it.
Patients with early Alzheimer’s disease who took lecanemab in a major clinical trial declined an average of five months slower than other subjects over an 18-month period, but many suffered brain swelling and bleeding. Although those side effects usually resolved without obvious harm, they apparently caused three deaths. The great expense of the drug and its treatment raises questions about how it will be paid for, and who will benefit.
“In the history of science, it’s a significant achievement to slightly slow down progression of dementia,” said John Mafi, a researcher and associate professor of medicine at the David Geffen School of Medicine at UCLA. “But the actual practical benefits to patients are very marginal, and there is a real risk and a real cost.”
To qualify for Leqembi, patients must undergo a PET scan that looks for amyloid plaques, the protein clumps that clog the brains of many Alzheimer’s patients. About 1 in 5 patients who took Leqembi in the major clinical test of the drug developed brain hemorrhaging or swelling, a risk that requires those taking the drug to undergo frequent medical checkups and brain scans called MRIs.
In anticipation of additional costs from the Leqembi drug class, the Centers for Medicare & Medicaid Services in 2021 increased monthly premiums for Medicare patients by 15%, and premiums may rise again in 2024 after a slight decline this year.
Such increases can be a significant burden for many of the 62 million Medicare subscribers who live on fixed incomes. “Real people will be affected,” Mafi said. He contributed to a study that estimated lecanemab and related care would cost Medicare $2 billion to $5 billion a year, making it one of the most expensive taxpayer-funded treatments.
In its analysis, ICER suggested that Leqembi could be cost-effective at an annual price of $8,900 to $21,500. In an interview, David Rind, ICER’s chief medical officer, said $10,000 to $15,000 a year would be reasonable. “Above that range doesn’t seem like a good place,” he said.
Whatever its price, patients may be delayed getting access to Leqembi because of the relative shortage of specialists capable of managing the drug, which will require genetic and neuropsychological testing as well as the PET scan to confirm a patient’s eligibility. A similar drug, Eli Lilly’s donanemab, is likely to win FDA approval this year.
Already there are long waits for the testing needed to assess dementia, Mafi said, noting that one of his patients with mild cognitive impairment had to wait eight months for an evaluation.
Such testing is not readily at hand because of the paucity of effective treatment for Alzheimer’s, which has helped to make geriatrics a relatively unappealing specialty. The United States has about a third as many dementia specialists per capita as Germany, and about half as many as Italy.
“Time is of the essence” for the neuropsychological testing, Mafi said, because once a patient’s cognitive ability declines below a certain threshold, they become ineligible for treatment with the drug, which was tested only in patients in the earliest stages of the disease.
Mafi’s study estimates that patients without supplemental Medicare coverage will have to pay about $6,600 out-of-pocket for each year of treatment. That could put it out of reach for many of the 1 in 7 “dual eligible” Medicare beneficiaries whose income is low enough to simultaneously qualify them for state Medicaid programs. Those programs are responsible for about 20% of physician bills for drug infusions, but they don’t always cover the full amount.
Some practitioners, such as cancer centers, cover their Medicaid losses by receiving higher rates for privately insured patients. But since almost all lecanemab patients are likely to be on government insurance, that “cross-subsidization” is less of an option, said Soeren Mattke, director of the Center for Improving Chronic Illness Care at the University of Southern California.
This poses a serious health equity issue because “dual eligibles are low-income patients with limited opportunities and education, and at higher risk of chronic illnesses including dementia,” Mattke said in an interview. Yet many doctors may not be willing to treat them, he said. “The idea of denying access to this group is just appalling.”
Eisai spokesperson Libby Holman said the company was reaching out to specialists and primary care physicians to make them aware of the drug, and that reimbursement options were improving. Eisai will provide the drug at no cost to patients in financial need, she said, and its “patient navigators” can help lock down insurance coverage.
“A lot of clinicians are excited about the drug, and patients are hearing about it,” said David Moss, chief financial officer of INmune Bio, a company that has another Alzheimer’s drug in development. “It’s a money center for infusion centers and MRI operators. It provides reasons for patients to come into the office, which is a billing thing.”
Outstanding doubts about Leqembi and related drugs have given urgency to efforts to monitor patient experiences. CMS is requiring Leqembi patients to be entered into a registry that tracks their outcomes. The agency has established a registry, but the Alzheimer’s Association, the leading advocacy group for dementia patients, is funding its own database to track those being treated, offering physician practices $2,500 to join it and up to $300 per patient visit.
In a letter to CMS on July 27, a group of policy experts said CMS should ensure that any and all Leqembi registries create and share data detailed enough for researchers and FDA safety teams to obtain a clear picture of the drug’s real-world profile.
The anti-amyloid drugs like lecanemab have created a polarized environment in medicine between those who think the drugs are a dangerous waste of money and those who believe they are a brilliant first step to a cure, said ICER’s Rind, who thinks lecanemab has modest benefits.
“People are as dug in on this as almost anything I’ve ever seen in medicine,” he said. “I don’t think it’s healthy.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 2 months ago
Aging, Health Care Costs, Health Industry, Medicaid, Medicare, Pharmaceuticals, Alzheimer's, CMS, Drug Costs
KFF Health News' 'What the Health?': The Long Road to Reining In Short-Term Plans
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
It took more than two years, but the Biden administration has finally kept a promise made by then-candidate Joe Biden to roll back the Trump administration’s expansion of short-term, limited-duration health plans. The plans have been controversial because, while they offer lower premiums than more comprehensive health plans, they offer far fewer benefits and are not subject to the consumer protections of the Affordable Care Act.
Also this week, the FDA for the first time approved the over-the-counter sale of a hormonal birth control pill. With more states imposing restrictions on abortion, backers of the move say making it easier to prevent pregnancy is necessary now more than ever.
This week’s panelists are Julie Rovner of KFF Health News, Alice Miranda Ollstein of Politico, Amy Goldstein of The Washington Post, and Rachel Cohrs of Stat.
Panelists
Alice Miranda Ollstein
Politico
Amy Goldstein
The Washington Post
Rachel Cohrs
Stat News
Among the takeaways from this week’s episode:
- The FDA’s much-anticipated approval of the first over-the-counter hormonal birth control pill followed the advice of its outside advisory committee. The pill, Opill, will be available on shelves without age restrictions.
- The Biden administration announced moves to limit so-called junk plans on insurance marketplaces. The Trump administration had dropped many restrictions on the plans, which were originally intended to be used for short-term coverage gaps.
- As the nation continues to settle into a post-Dobbs patchwork of abortion laws, the Iowa Legislature approved a six-week ban on the procedure. And an Idaho law offers a key test of cross-border policing of abortion seekers, as other states watch how it unfolds.
- In other news, Georgia’s Medicaid work requirements took effect July 1, implementing new restrictions on who is eligible for the state-federal program for people with low incomes or disabilities. And the Supreme Court’s decision on affirmative action has the potential to shape the health care workforce, which research shows could have implications for the quality of patient care and health outcomes.
Also this week, Rovner interviews KFF Health News’ Bram Sable-Smith, who reported and wrote the latest KFF Health News-NPR “Bill of the Month” feature, about a patient who lacked a permanent mailing address and never got the hospital bills from an emergency surgery — but did receive a summons after she was sued for the debt. If you have an outrageous or exorbitant medical bill you want to share with us, you can do that here.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: KFF Health News’ “Doctor Lands in the Doghouse After Giving Covid Vaccine Waivers Too Freely,” by Brett Kelman.
Rachel Cohrs: ProPublica’s “How Often Do Health Insurers Say No to Patients? No One Knows,” by Robin Fields, and Stat’s “How UnitedHealth’s Acquisition of a Popular Medicare Advantage Algorithm Sparked Internal Dissent Over Denied Care,” by Casey Ross and Bob Herman.
Amy Goldstein: The New York Times’ “Medicare Advantage Plans Offer Few Psychiatrists,” by Reed Abelson.
Alice Miranda Ollstein: The Wall Street Journal’s “America Is Wrapped in Miles of Toxic Lead Cables,” by Susan Pulliam, Shalini Ramachandran, John West, Coulter Jones, and Thomas Gryta.
Also mentioned in this week’s episode:
- Stat’s “How One Medical School Became Remarkably Diverse — Without Considering Race in Admissions,” by Usha Lee McFarling.
- The New York Times’ “With End of Affirmative Action, a Push for a New Tool: Adversity Scores, by Stephanie Saul.
click to open the transcript
Transcript: The Long Road to Reining In Short-Term Plans
KFF Health News’ ‘What the Health?’Episode Title: The Long Road to Reining In Short-Term PlansEpisode Number: 305Published: July 13, 2023
[Editor’s note: This transcript, generated using transcription software, has been edited for style and clarity.]
Julie Rovner: Hello and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News. And I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, July 13, at 10 a.m. As always, news happens fast and things might have changed by the time you hear this. So here we go. Today we are joined via video conference by Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Good morning.
Rovner: Rachel Cohrs of Stat News.
Rachel Cohrs: Hi, everybody.
Rovner: And Amy Goldstein of The Washington Post.
Goldstein: Good to be with you.
Rovner: Later in this episode, we’ll have my interview with KFF Health News’ Bram Sable-Smith, who wrote the latest KFF Health News-NPR “Bill of the Month.” The hospital that provided care to this month’s patient couldn’t find her to send her a bill, but the debt collectors sure could. But first, this week’s news. Actually, it’s more like the last month’s news because we actually haven’t talked about news in a while. So we’re going to try to hit a bunch of items in sort of a lightning round. Let’s start with something we knew was coming. We just didn’t know exactly when. Last week, the Biden administration finally cracked down on short-term health plans. Those are the ones that are not subject to the strict rules of the Affordable Care Act. Amy, you wrote about this. What are short-term plans, and why have they been so controversial?
Goldstein: Well, short-term plans — they’re called short-term limited-duration plans, and really terrible argot, but that’s their name. They’ve been around as an alternative to plans that are meeting the rules of the Affordable Care Act. They were originally designed for people to use as small bridges between, say, when they lost a job and they were about to get a new job and they needed something in the interim to provide health coverage. Republicans, during the time that they were trying very hard several years ago to get rid of as much as the Affordable Care Act as they could — they didn’t succeed at a lot of that, but they did succeed during the Trump administration at lengthening the time that people could have these plans. So they extended them from what had been a three-month maximum during the latter part of the [Barack] Obama administration to 12 months, and then they were renewable for up to three years. And Democrats began calling these “junk plans,” saying that people didn’t exactly know what they were buying, that the premiums were low but the benefits were small and if people got sick and really needed a lot of care they could be stuck paying for a lot of it on their own.
Rovner: And these were the very plans that the ACA was kind of designed to get rid of, right, where people would say, I have this great health plan, it only costs me $50 a month — but by the way, it only provides $500 worth of care.
Goldstein: Well, there’s that. And the other thing that the ACA was designed to do is treat people with preexisting conditions equally. And these plans do not have to do that. Some do, but they’re not required to. So President [Joe] Biden, since he was candidate Biden running for the 2020 election, has been saying for quite a while that he was going to knock down the duration of these plans, and some of his fellow Democrats have been leaning on him: “Why haven’t you done it yet?” And last week, he finally did. He didn’t bring it exactly to where the Obama administration had it, but he brought them down to three months with a one-month extension, so a total of four months.
Rovner: And I guess the resistance here is that they’re still kind of popular, right, for people who think they would rather pay very low premiums for very few benefits?
Goldstein: Well, the catch is that we don’t really know how popular they are because there aren’t very reliable data on how many people have these. But the presumption is that some people like them.
Rovner: All right, well we will see what happens with this time they’re trying to crack down. Let us move on to abortion and reproductive rights. We will start with the breaking news. The Food and Drug Administration just this morning approved Opill, which is the first over-the-counter birth control pill. Alice, we’ve known this was coming, right?
Ollstein: Yes, we did. We thought it would be a little later in the summer. But the decision itself reflects what the FDA’s outside advisory panel strongly recommended, which is to make these pills available over the counter without a prescription and without an age restriction, which was one looming question over this process.
Rovner: Yeah, I guess, Rachel, I mean, the issue here has been can women be trusted enough to know when they shouldn’t take birth control pills because they are contraindicated for some people?
Rachel Cohrs: Right. And I think that certainly it’s important to read through the information. There’s a question as to whether women will do that. And one part of the release that stood out to me is that the specific type of pill that this is requires women to take it around the same time every day, which is not necessarily the case for all birth control pills. And I think there’s a little bit more flexibility than there used to be with this kind of pill. But it is just important that all of this communication happens. And if there’s not a doctor or pharmacist in the middle, I think it will be kind of interesting to see how this plays out in the real world.
Rovner: Well, while this could definitely help people prevent pregnancy who don’t want to get pregnant, there’s certainly a lot of action still in the states around abortion. We’re going to start in Iowa, which since the last time we spoke has done basically a 360 on abortion. Last month, the state Supreme Court deadlocked on whether to reinstate a 2018 ban on almost all abortions. That left a lower court order blocking the ban intact, so abortion remained legal in Iowa. But anti-abortion Gov. Kim Reynolds refused to take no for an answer. She called a special session of the state legislature, which on Tuesday essentially repassed the 2018 ban. It’s supposed to take effect as soon as the governor signs it, which could be as soon as Friday. But first it goes back to court, right, Alice?
Ollstein: Right. As with all of these things, there’s just a lot of back-and-forth before it’s final. Groups have already filed a lawsuit. And, you know, because the courts’ sort of mixed treatment of the previous version of this, we sort of don’t know what’s going to happen. But the law could go into effect and then be blocked by courts later or it could be blocked before it goes into effect. There’s a lot of different ways this could go, but this is one of several states where new restrictions are coming online. We’re more than a year out from the Dobbs decision now, and things are not settled at all. Things are still flipping back and forth in different states.
Rovner: Yeah, there’s a lot of states where old restrictions came into effect and then were blocked and now they’re putting new restrictions and they might be blocked. Well, turning to another “I” state, this time Idaho, where the legislature this spring passed a first-in-the-nation bill attempting to criminalize the act of helping a minor cross state lines for an abortion, even if the abortion is legal in the state the minor travels to. Now, abortion rights supporters have filed a first-in-the-nation lawsuit to block the first-in-the-nation law. This could have really big ramifications. This is different from a lot of what’s going on in a lot of the other states, right?
Ollstein: Yeah. Over the last year, there’s been a lot of fear on the left of states reaching across their borders to try to police abortion. And it hasn’t really happened yet that we have seen. And so this, I think, is a key test of whether more states will attempt to go in this direction. You know, a lot of blue states passed sort of shield laws for patients, for providers, for data, out of fear that more red states would attempt more cross-border policing. But that really hasn’t materialized broadly yet.
Rovner: I remember Missouri was the one that was talking about it, right, to make it a crime if —
Ollstein: Right.
Rovner: I know they didn’t do it, but they were talking about if women went particularly to Illinois, which is now one of these abortion havens, and came back, they would try to prosecute them, although that never really came to be.
Ollstein: Exactly. And so it’s interesting that even really conservative states with big Republican majorities, most have not gone down this road yet. And so I imagine a lot of them are watching how this case goes.
Rovner: Well, as long as we’re talking about states that start with “I,” let’s turn to Indiana, where Planned Parenthood reports that all of their appointments for abortions are taken between now and when that state’s near-total ban takes effect in a few weeks. This points out something I think often gets missed in these sort of score card maps of states that have bans and restrictions, which is there’s a lot of states where abortion is technically still legal but realistically not available, right?
Ollstein: The difference between being technically legal and available is nothing new. This was true prior to Dobbs as well. There were lots of states that only had one abortion clinic for the entire state. There were, like, six of those. And so, you know, you may have the right to have the procedure on paper, but if there’s only one place you could go and you’re not able to physically get there or they don’t have an appointment within the time window you need, you’re out of luck; that right isn’t, you know, meaningful for you. And so that’s becoming, you know, more true as abortion access is eliminated in a lot of the country and more and more people are depending on fewer and fewer states.
Rovner: And fewer and fewer clinics in fewer and fewer states. Well, finally, an update on the one-man nomination blockade by Alabama Republican Sen. Tommy Tuberville, who we talked about in March. He has stopped approval of basically all Defense Department personnel moves, including routine promotions, in protest of the Biden administration’s policy of providing leave and travel expenses for servicewomen to get abortions if they’re stationed in states where it’s illegal. Now, for the first time in more than 150 years, the Marine Corps has no approved commandant. Any idea which side’s going to back down here? Rachel, this is backing up the entire legislative calendar in the Senate, right?
Cohrs: It is. And I think some of the coverage this week has highlighted just how there hasn’t really been a willingness among Republican leadership to really put the pressure on Tuberville. But honestly, I don’t know when this stops for him. Having temporary leadership in all these positions isn’t kind of the impetus for him to say that he’s made his point. And I think there are also questions about — there may be more education required about exactly what the difference is between a temporary leader and a permanently installed leader. Obviously, the decisions that they’re making every day are life-and-death and are different than the leadership positions we see over at something like the NIH [National Institutes of Health], where, you know, I think it is —
Rovner: Which is also held up. But that’s another story.
Cohrs: Right, another story. But I just don’t see where this ends quite yet, unless there’s some will from Republican leadership to really bring him in line. And they just haven’t summoned that yet.
Rovner: I imagine there’ll be a vote on this when they get to the defense bill, right, which —the defense authorization, which is going to come up, I think, in both houses in the coming weeks. I mean, one would think that if there’s a vote and he loses, he might back down. I’m just guessing here. I guess we’ll have to wait and see what happens with that. All right. Well, it’s also been a busy couple of weeks in other social policy. On the one hand, a new federal law took effect that makes it easier for people to get accommodations to be able to do their jobs while pregnant. And Maine is going to start offering paid family and parental leave, although not until 2026. That makes it the 13th state to enact such a policy. On the other hand, Georgia is the first state to implement work requirements for Medicaid. Amy, the last time we discussed this, federal judges had tossed out Medicaid work requirements and Republicans in Congress were unsuccessful in getting those requirements back into the debt ceiling compromise. So how come Georgia gets to do this?
Goldstein: Well, I’ve begun to think of Medicaid work requirements as whack-a-mole, if you remember the arcade game in which you knock down an animal with a mallet only to have it pop up unexpectedly somewhere else. So, as you say, work requirements was something that Republicans were very eager to institute in 2017, 2018, when the Trump administration’s Center for Medicare & Medicaid Services encouraged states to adopt them. And there were basically plans to give people Medicaid at the time, mainly people in Medicaid expansion groups, if they worked or went to school or did community service for at least 80 hours a month. As you say, that was knocked down both by a district court and then a federal circuit court. And it looked like that was that, particularly when the Biden administration came along and undid the Trump administration’s regulation that had allowed states to submit proposals, the waivers for these kinds of plans. Well, lo and behold, Georgia said they wanted to do this. They said they wanted to do it in a little bit different way, because, for the first time ever, Georgia was going to be a partial expansion state for Medicaid, allowing people to get onto Medicaid if they had incomes up to the poverty level but not up to the full expansion poverty level that the ACA allows. And the Biden administration didn’t like that so much. And that partial expansion was to be twinned with work requirements. The Biden administration didn’t —
Rovner: For that expansion group, though, right? Not for everybody.
Goldstein: Just for that partial expansion group. The Biden administration didn’t like that so much. But last summer, a judge in Georgia said, no, she thinks this is OK. And the reason was that, unlike the other states, if this was pegged to a partial expansion, any expansion with work requirements would increase the number of people with Medicaid. So that was sort of in her judge judgment — I shouldn’t say the judge’s judgment — consistent with the purposes of the program. So Georgia has gone ahead, and the beginning of this month they allowed people to start enrolling in something called Georgia Pathways to Coverage. And we’ll have to see how it goes.
Rovner: Yeah. And just to be clear, I mean, Alice, you did some stellar work back a couple of years ago about Arkansas, about people losing coverage because of the work requirements, even if they were working, just because of how hard it was to report the work hours, right?
Ollstein: Absolutely. I mean, it’s kind of what we’re seeing now with the Medicaid unwinding, is that, you know, people just aren’t able to know what’s going on, aren’t able to be reached, fall through the cracks, can’t navigate the bureaucracy, and lose coverage that they should be entitled to. So we saw that happen, and I think to Amy’s point, the administration seems to be taking a very different stance on states like Arkansas, you know, which already had expanded Medicaid and then went to impose a work requirement, whereas Georgia didn’t have it before and this is kind of a compromise because it’s like, well, more people will be insured if we allow this to go forward total, you know, so maybe it’s better than nothing, although a lot of folks on the left are very opposed to the concept of work requirements, citing data that the people who are on Medicaid who can work are already working — the vast, vast, vast majority. And those who are not working, either they are caring for a child or someone with disability, or they themselves have a disability, or they’re a student. You know, there’s all these categories of why folks are unable to work.
Rovner: But in this expansion group, one would assume that if they’re earning up to the federal poverty line, they have some source of income. So one would assume that many of them are working. But I think it’ll be really interesting for researchers to watch to see, you know, a sort of a proof of concept in either direction with this.
Goldstein: And let me quickly mention a couple of things. Georgia’s rules are actually in some ways the same as what other states had tried to do previously. But in other ways, this is the strictest set of work requirements that anyone has tried in a couple of ways: People have to meet these work requirements up to age 64, which is older than other states had done for the most part. There’s also no exemption if you’re taking care of a child or taking care of an older family member. So how well people, in addition to the bureaucratic hoops that Alice was talking about, which are of grave concern to some of the people who oppose this in Georgia — there’s also a question of who’s going to actually be able to qualify for this.
Rovner: While we are on the subject of court decisions, one of the odd court decisions that I think has happened over the past few weeks is a federal district court decision out of Louisiana barring many officials in the Biden administration, including the surgeon general and the head of the CDC [Centers for Disease Control and Prevention], from talking to social media sites, particularly about things like medical misinformation. This feels like something I had not seen before in terms of actually trying to ban the administration from talking to private companies based on First Amendment concerns, which is what this is.
Cohrs: Right. Well, I mean, the First Amendment protects speech from interference from the government —
Rovner: Right
Cohrs: — which has always been, you know, this gray area with these independent platforms. And I think this issue, you know, has obviously become highly politicized. It came up several times when Rochelle Walensky, the former CDC director, was testifying on the Hill. So I think certainly we’ve seen this trend overall in these highly political court decisions and this strategy that certain litigants are taking where they’re trying to find defendants in a certain jurisdiction that’s going to be advantageous to them. So it will certainly be interesting to see how this plays out in the future and makes its way through the court system, but certainly is an eye-popping precedent. Like you mentioned, we don’t usually see something like this.
Rovner: And I wanted to mention, I think also because this is yet another of these judges that the right has found that are likely to agree with them. Like we’ve seen now: The judges in Texas, we now have one in Louisiana. Sort of kind of watch that docket. While we are still on the subject of courts, 2023 was the first year in the last decade or so that there was not a major health-related decision in the last big cases decided by the Supreme Court. But it seems like one of those non-health cases, the one essentially striking down affirmative action, might have some major implications for health care after all, particularly for medical education, right?
Cohrs: Yes. Some of my colleagues did some I think great follow-up reporting on this. And I think the idea is that there has been research that has shown that when patients are able to see a doctor of their same racial background, that it does have positive implications for their care. And there has also been studies of schools where there have been bans on race-conscious admissions showing that there is a decrease in medical school students from underrepresented backgrounds traditionally. And so I think that cause and effect is concerning for people, that if there are fewer medical students — there already aren’t a representative amount — from underrepresented groups, that could trickle down to, again, just exacerbating so many of these inequities that we see in health care provision. I know there was just a big study on the maternal mortality outcomes that came out recently as well. And I think all of these things are tied together. And I think Axios reported on one interesting potential loophole, was using proxy measures, like where someone went to school or their parents’ background, something like that, to try to ensure diversity from that lens. But I think it certainly is going to make these medical schools recalculate how they’re doing admissions and make some hard choices about how to maintain diversity that can be beneficial for patients.
Rovner: One thing that I think has come up in all of these discussions is the fact that the University of California-Davis has done an interesting job of creating a very diverse medical school class, even though race-conscious admissions have been banned in California for years. So I think a lot of schools are going to be looking sort of to see what UC Davis has done and perhaps emulate that. And I will put one of the UC Davis stories in the show notes for everybody. All right. Finally in this week’s news, the drug industry has filed a lawsuit challenging the Medicare drug price negotiation program that’s just now starting to get off the ground. Rachel, you wrote about this. How does pharma think it can block price-setting for Medicare that Medicare does for pretty much everything else that Medicare pays for? They set prices for hospitals and doctors and medical equipment. Why are drugmakers thinking that they’re special?
Cohrs: Right. So, again, this is four lawsuits as well, not just one: two from two trade groups and two drugmakers. And they’re each kind of using different arguments. But I think the big picture here is if the government called it price-setting, I don’t think pharma would have as much of an argument, but they’re calling it a negotiation. And I think one of the drugmakers’ key claims is that by signing these contracts to enter into this process, they’re tacitly admitting that this price that they come up with in this process is, quote-unquote, “fair.” And, you know, they don’t want to agree to that because then it makes the price that they’re charging everyone else look unfair on the other side of the coin. And I think there’s also these really high penalties for these companies who decide not to participate; I mean, tens of millions of dollars on the first day is the kind of number that we’re seeing for some of these companies that have filed lawsuits. And I think there’s also the option for them to take all of their drugs off of the market. But I think there’s a question with the timeline of whether they could have even done that before the law was passed. So the big picture from the drugmaker side of things is that the penalties are so high for them not to participate and that the government is framing this as a negotiation when it really is just price-setting, like Medicare does in so many other areas. So I think one interesting development that happened this week was that the [U.S.] Chamber of Commerce filed a motion for a preliminary injunction, which could make all of these lawsuits move much faster and really put a stop to the program. We hadn’t seen either of these lawsuits request a motion like that. And I think they requested a ruling by Oct. 1, which is when the first kind of round of 10 drugmakers would have had to sign their contracts with Medicare. So I think this certainly is picking up speed and urgency as we’re moving toward that Sept. 1 selection date.
Rovner: I didn’t even notice. Are these lawsuits all filed here in Washington, D.C., or —
Cohrs: No, they are not. As we’ve seen, the drugmakers are very strategic in where they filed. I think Merck did file in D.C., but the chamber filed in Ohio; it had some of their local chapters join in as well. I think we saw another company file in New Jersey. So I think they are kind of hedging their bets and trying to get rulings from as many different jurisdictions as they can.
Rovner: Find a judge who’s willing to slap an injunction on this whole thing.
Cohrs: Yes.
Rovner: Which we will talk about when and if it happens. All right. That is this week’s news, or at least as much as we have time to get to. Now, we will play my “Bill of the Month” interview with Bram Sable-Smith, and then we will be back with our extra credits. We are pleased to welcome back to the podcast Bram Sable-Smith, who reported and wrote the latest KFF Health News-NPR “Bill of the Month.” Bram, so nice to see you again.
Bram Sable-Smith: Always a pleasure to be here.
Rovner: So, this month’s patient was, like a lot of young people, an uninsured 23-year-old when she ended up in the emergency room. Tell us who she is and what kind of medical care she needed and got.
Sable-Smith: Yeah, that’s right. Her name was Bethany Birch. And, in addition to being uninsured, she was also unemployed at the time, and she had had pain in her diaphragm for eight months. It prevented her from eating. She lost about 25 pounds in that time. And when she went to the emergency room, she found out she needed her gallbladder removed.
Rovner: And got it, right?
Sable-Smith: And got it. Yeah, she got that surgery almost immediately. Because she hadn’t been eating food — her food resistance — it meant she could get in for surgery right away.
Rovner: And that cured her? Yes?
Sable-Smith: It did cure her. Yes, she felt a lot better.
Rovner: So now we’re talking about the bill. The hospital tried to send her the bill, but apparently it couldn’t find her. Is this a common thing, and why couldn’t they find her? One presumes she gave them an address when she presented at the emergency room.
Sable-Smith: She did give them an address, but by the time she was discharged, she had lost her housing. Her home situation was unstable. So just that brief visit to the hospital, by the time she left, she had no more house to live in. And she did end up crashing with her family for several months. And, eventually, she did update her address with the post office. But by the time she had done that, it was after the hospital had sent the three bills to her for her visit.
Rovner: So the hospital doesn’t get any response, and they do what we know hospitals do. They sued for nonpayment. And the debt collection firm did manage to find her. So then what happened?
Sable-Smith: Well, she went to court, and like so many people who end up in court with medical debt, she did not have a lawyer representing her. She met with a representative from the debt collection firm, and she worked out a payment plan to pay her bill, plus court costs, in $100 monthly installments. But at the time, Tennessee had a default interest rate on judgments like the one that Bethany had of 7%. So the judge tacked on a 7% interest rate to her bill.
Rovner: So, yeah, and that was presumably a lot for her to carry. What finally happened with the bill?
Sable-Smith: Well, she paid her $100 monthly payments for over four years. It totaled about $5,200 she paid in that time. But at the same time, the interest rate was accruing. And so she owed an additional $2,700 on top of the initial bill that she had gotten. From her perspective, it was just impossible. She wasn’t digging out of this debt. So she started getting help from a family friend, who’s a billing expert, who took on her case. They asked the hospital and the debt collection firm to settle her debt because she had already paid so much. But they were unsuccessful in doing so. They sent their bill to us. We started reporting the story. Then they asked again to settle her debt by paying an additional $100 on top of what she had already paid. And this time they agreed. And so she settled her debt and she got a balance-zero statement.
Rovner: Amazing how just one phone call from us can do some work. Now, as somebody who is unemployed and, as you pointed out, uninsured at the time she got the care, Bethany should have been eligible for the hospital’s financial assistance policy. Why didn’t she get help before the debt ballooned with court costs and all that interest?
Sable-Smith: Well, the simple answer is that she never applied. But, as we know, it’s much more complicated than that. So given her status as single, uninsured, unemployed, it’s very possible that she would have qualified for financial help, maybe even for free care altogether. But the onus was on her as a patient to apply. And we know her situation was unstable. You know, she went through a period of homelessness. She didn’t have a lot of expendable money at the time. It’s a long process to apply for these programs. There’s a lot of forms. It can be cumbersome. And that prevents a lot of people from applying to these programs. So advocates push for something called presumptive eligibility, where the hospital takes the onus of applying away from patients and they automatically put them through the process. And this hospital that Bethany went to, they actually have switched to that presumptive eligibility model, just not in time to help her case.
Rovner: So what’s the takeaway here? I guess everybody has to be a proactive patient, not just with your medical care, but especially with your bills. What happens to a patient who finds themselves in a similar situation?
Sable-Smith: Well, you know, from a consumer standpoint like that, one takeaway is to ask for financial help. A lot more people qualify than you might think. You might not think you qualify, but it’s very possible you could. And then from a policy perspective, hospitals switching to presumptive eligibility — that’s something that they’re able to do. And also, some states have pushed to ban or even limit interest payments on this kind of medical debt. So that’s something that other people are considering as well.
Rovner: Or you can write to us, and we will show you how in our show notes.
Sable-Smith: That’s always a possibility, too.
Rovner: Bram Sable-Smith, thank you so much.
Sable-Smith: Yeah, thanks for having me.
Rovner: OK, we’re back, and it’s time for our extra credit segment. That’s when we each recommend a story we read this week we think you should read too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Rachel, why don’t you go first?
Cohrs: OK, I’m cheating a little bit and I’m doing a double feature. So the first story for my extra credit is headlined “How Often Do Health Insurers Say No to Patients? No One Knows.” It’s in ProPublica by Robin Fields, and I think it’s just a great feature on the idea that Obamacare entitled the government and patients to more information about how often insurers deny care to patients. And the government hasn’t really pursued that information. And even, like, state health insurance commissions aren’t providing the information they’re collecting. And Robin just had such a difficult time getting any sort of information from anyone, even though we’re legally entitled to it. So I thought that was just kind of a great highlight of this next area of criticism of the health insurance industry, which, and I think that —
Rovner: I would say, all this focus on premiums and not as much focus on what you actually get for those premiums.
Cohrs: Exactly. So true. I think there’ve been some high-profile examples, great reporting. And I thought that meshed well with some reporting from my colleagues Casey Ross and Bob Herman, who wrote a follow-up to some of their prior reporting titled “How UnitedHealth’s Acquisition of a Popular Medicare Advantage Algorithm Sparked Internal Dissent Over Denied Care.” Again, looking at how algorithms in this one privatized Medicare program, which is growing in size and enrollment across the country, was actually overruling clinicians’ decisions about how long patients should be receiving care in facilities. And if the algorithm says they should be done, then they’re done. And I think it definitely sparked some concerns from people in the company who were willing to speak to them just because they were so concerned about this trend.
Rovner: Alice.
Ollstein: I have a very impressive investigation from The Wall Street Journal. There are five bylines, and we will post the link. This is about lead-covered telecom cables owned by AT&T, Verizon, other companies that have been left to decay and leach into the environment all around the country. This documents how the companies knew about them but have not moved to clean them up and get rid of them. They are impacting water sources. They are near playgrounds where children are, and it goes into the very disturbing health impacts of lead exposure. This is something the country has made a lot of progress on when it comes to paint and other sources, but obviously we still have a long way to go.
Rovner: Yeah, because there’s not enough things to be worried about environmentally, here is something else. It is very good reporting.
Rovner: Amy.
Goldstein: My extra credit this week is from The New York Times, by Reed Abelson, with the headline “Medicare Advantage Plans Offer Few Psychiatrists.” And this isn’t a giant story, but I think it is at the nexus of two very important questions: one, the long-standing question of whether privatized Medicare is better or worse for people who are older Americans on Medicare than the traditional version of Medicare; and the question of are people getting enough access to mental health care? And I guess what struck me is that there’s been so much attention lately to the question of access to mental health services for younger Americans, and this looked at the question of access to mental health services for older Americans. And what this story, based on a study, talks about is that the study found that more than half of the counties, the researchers who did this study found, is that those counties did not have a single psychiatrist participating in Medicare Advantage and that a lot of these plans have what’s called “narrow” or “skinny” networks, where a very small fraction of the available psychiatrists in a community were in that plan’s network. Now, [there are] people who are criticizing that study saying, well, you can’t look at just psychiatrists; there are other people who provide competent mental health care. But I think it just raises the question of who is getting what they need.
Rovner: Indeed. Well, my story this week is also about just plain good reporting. It’s called “Doctor Lands in the Doghouse After Giving Covid Vaccine Waivers Too Freely.” It’s by Brett Kelman of KFF Health News. But it’s about some old-fashioned reporting by another outlet, Nashville’s NewsChannel 5. It seemed that during the height of the covid vaccine rollout, when lots of places were requiring proof of vaccines and lots of people didn’t want to get them, the doctor in question, named Robert Coble, was providing waivers through a website without much —OK, any — oversight. How did they prove it? By obtaining a waiver for a reporter’s black Labrador retriever, Charlie. Earlier this spring, Coble quietly surrendered his medical license to the state Department of Health. Journalism works. OK, that is our show for this week. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us too. Special thanks, as always, to our producer, Francis Ying. Also as always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can still tweet me. I’m @jrovner. I’m on Threads too, @julie.rovner.
Rovner: Amy.
Goldstein: I’m @goldsteinamy.
Rovner: Rachel.
Cohrs: I’m @rachelcohrs on Twitter and @rachelcohrsreporter on Threads.
Rovner: Alice.
Ollstein: @AliceOllstein.
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ ‘What the Health?’ on Spotify, Apple Podcasts, Stitcher, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 3 months ago
Courts, Health Care Costs, Health Industry, Insurance, Medicaid, Medicare, Multimedia, Biden Administration, Contraception, Drug Costs, FDA, KFF Health News' 'What The Health?', Podcasts, Pregnancy, Women's Health
Slow Your Disenroll
The Host
Mary Agnes Carey
KFF Health News
Partnerships Editor and Senior Correspondent, oversees placement of KFF Health News content in publications nationwide and covers health reform and federal health policy. Before joining KFF Health News, Mary Agnes was associate editor of CQ HealthBeat, Capitol Hill Bureau Chief for Congressional Quarterly, and a reporter with Dow Jones Newswires. A frequent radio and television commentator, she has appeared on CNN, C-SPAN, the PBS NewsHour, and on NPR affiliates nationwide. Her stories have appeared in The Washington Post, USA Today, TheAtlantic.com, Time.com, Money.com, and The Daily Beast, among other publications. She worked for newspapers in Connecticut and Pennsylvania, and has a master’s degree in journalism from Columbia University.
The Biden administration this week pleaded with states to slow the post-pandemic removal of beneficiaries from their Medicaid rolls, as government data shows more than a million Americans have lost coverage since pandemic protections ended in April. Meanwhile, the Supreme Court ruled Medicaid beneficiaries may sue over their care.
In an appearance at the U.S. Capitol, the outgoing chief of the Centers for Disease Control and Prevention, Rochelle Walensky, offered no revelations as House Republicans pressed her about the agency’s response to the covid-19 pandemic. And senators are pushing for action on drug pricing, with Sen. Bernie Sanders (I-Vt.) vowing to hold up nominations to press the Biden administration for drug pricing reform.
This week’s panelists are Mary Agnes Carey of KFF Health News, Rachel Cohrs of Stat, Alice Miranda Ollstein of Politico, and Sandhya Raman of CQ Roll Call.
Panelists
Rachel Cohrs
Stat News
Alice Miranda Ollstein
Politico
Sandhya Raman
CQ Roll Call
Among the takeaways from this week’s episode:
- Asking states to slow the pace of Medicaid disenrollment, Health and Human Services Secretary Xavier Becerra offered options intended to reduce the number of Americans who lose coverage due to bureaucratic hurdles, such as by allowing community organizations to help people get coverage reinstated. But those options are only guidance for Medicaid programs across the country, and nothing says that states — especially conservative ones that have rushed to trim the number of low-income and disabled people relying on the program — will adopt the administration’s suggestions.
- A deal in the Braidwood Management v. Becerra court case will preserve, for now, the mandate requiring insurance coverage of preventive services for all but the litigants. The threat of a court order halting that coverage mandate nationwide has contributed to growing concerns about the overuse of injunctions allowing a single judge to bring down an entire program or law.
- The Supreme Court ruled that a woman is entitled to sue over the nursing home care her husband received that was covered by Medicaid, setting a precedent that allows beneficiaries to pursue legal action over their care.
- This week, House Republicans pressed CDC Director Walensky about the agency’s response to the pandemic, but, producing few new details, the hearing mostly proved an attempt by Republicans to relitigate concerns over issues like gain-of-function research funding. And Ashish Jha, the White House’s covid coordinator, is preparing to step down without a successor, offering more fodder for the argument that the Biden administration is de-emphasizing covid policy.
- Reports of threats against an Alabama clinic that does not provide abortions illuminate the realities of the post-Dobbs era: Even the state attorney general has taken issue with the clinic’s efforts to provide non-abortion maternal health care — and 40% of Alabama counties already have no access to maternal care.
- And on Capitol Hill, Sanders — head of a key Senate health committee — has said he will hold up reviewing nominations in an effort to pressure the Biden administration to produce a comprehensive drug pricing plan. Meanwhile, another key Senate committee releases its proposal to rein in fees charged by pharmacy benefit managers.
Also this week, KFF Health News’ Julie Rovner interviews Dan Mendelson, chief executive of Morgan Health — the successor project to Haven Healthcare, a joint venture by Amazon, Berkshire Hathaway, and JPMorgan Chase that aimed in 2018 to disrupt how Americans get health coverage but quickly disbanded. Rovner and Mendelson discuss the role of employers in insuring American workers.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Mary Agnes Carey: The Washington Post’s “I Lost 40 Pounds on Ozempic. But I’m Left With Even More Questions,” by Ruth Marcus.
Alice Miranda Ollstein: Stat’s “AMA Asks Doctors to De-Emphasize Use of BMI in Gauging Health and Obesity,” by Brittany Trang and Elaine Chen.
Rachel Cohrs: Politico’s “Thousands Lose Medicaid in Arkansas: Is This America’s Future?” by Megan Messerly.
Sandhya Raman: The Markup’s “Suicide Hotlines Promise Anonymity. Dozens of Their Websites Send Sensitive Data to Facebook,” by Colin Lecher and Jon Keegan.
Also mentioned in this week’s episode:
- KFF Health News’ “Biden Admin Implores States to Slow Medicaid Cuts After More Than 1M Enrollees Dropped,” by Hannah Recht.
- Politico Magazine’s “This Alabama Health Clinic Is Under Threat. It Doesn’t Provide Abortions,” by Alice Miranda Ollstein.
click to open the transcript
Transcript: Slow Your Disenroll
KFF Health News’ ‘What the Health?’
Episode Title: Slow Your Disenroll
Episode Number: 302
Published: June 15, 2023
[Editor’s note: This transcript, generated using transcription software, has been edited for style and clarity.]
Mary Agnes Carey: Hello and welcome back to “What the Health?”. I’m Mary Agnes Carey, partnerships editor at KFF Health News, filling in for Julie Rovner this week. I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, June 15, at 10:30 a.m. As always, news happens fast and things might have changed by the time you hear this. So here we go. We’re joined today by video conference by Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Good morning.
Carey: Rachel Cohrs of Stat.
Rachel Cohrs: Hi, everybody.
Carey: And Sandhya Raman of CQ Roll Call.
Sandhya Raman: Good morning.
Carey: Later in the episode, we’ll have Julie’s interview with Dan Mendelson, CEO of Morgan Health. That’s the successor organization to the ambitious but ultimately unsuccessful effort by JPMorgan Chase, Amazon, and Berkshire Hathaway to remake employee health benefits. But first, let’s go to this week’s news. The Biden administration announced that more than a million Americans have lost their Medicaid coverage since early April as part of the ending of the covid public health emergency. Administration officials said that too many people were losing Medicaid due to red tape. About 4 in 5 people dropped so far either didn’t return paperwork to verify their eligibility or they omitted documents, according to federal and state data from 20 states. Department of Health and Human Services Secretary [Xavier] Becerra has sent a letter to state governors with some ideas on how to help stop this trend. What is he asking states to do?
Raman: So he gave states a few options. He said states could let Medicaid managed care organizations do a renewal on the beneficiaries’ behalf or let states kind of delay some of these cuts to allow for more outreach or let the community organizations in the state help individuals reinstate their coverage if they’ve fallen through some of the gaps here. But I think the thing to keep in mind is that all this is a guidance. All the Medicaid programs are different from each other. So while Becerra says that these are options, it doesn’t mean that any number of states will actually take on any of these opportunities to get more folks back into the program if they’re eligible.
Carey: To your point, some of the biggest drops in the enrollment in Medicaid have been in those more conservative states that are at political odds with the Biden administration. For example, in last week’s podcast, there was a lot of discussion about Arkansas and Indiana. For the panel, what are your thoughts on how state governments will respond to this guidance from HHS?
Ollstein: This is why there was so much anxiety last year when this was all being hashed out in the bill in Congress. Advocacy groups were sounding the alarm that there just weren’t enough guardrails to prevent this from happening. There were carrots; there were incentives for states to go slower and be more deliberate and careful in how they kick ineligible or, you know, can’t-determine-eligibility people off the rolls. But there weren’t a lot of sticks. There were carrots and not a lot of sticks. There weren’t a lot of penalties or repercussions for states that wanted to go as fast as possible and kick as many people off as possible, even if that meant folks falling through the cracks, which is what’s now happening.
Carey: So Sandhya sort of referenced this a moment ago. But I know, I mean, Medicaid is a shared federal-state program, but states, are they legally required to follow any of this guidance? I mean, what happens if a state just doesn’t do anything that’s in the letter? Does it matter?
Raman: I think the issue is that it doesn’t. I mean, there are some requirements that are applied to all programs if it’s in the Medicaid statute and sometimes when states do things that violate that and it ends up going to court. But I think anything here is they still have to follow what has been in the law that had said that after the public health emergency ended, that they could start slowly ripping people off the program. And that’s kind of the issue here.
Carey: Well, we’ll keep our eye on that one. And it sounds like another solution to find its way through the courts. Speaking of the courts, let’s move on to another major news development, and this one is regarding the preventive services coverage under the Affordable Care Act. It’s also known as the ACA. Texas conservatives that challenge the law’s preventive care mandate have reached a tentative compromise with the Justice Department that preserves free coverage for a range of medical services. Alice, I know you wrote about this agreement this week. Could you start us off and take us through the highlights?
Ollstein: Sure. So this was teased during oral arguments. The judges at the 5th Circuit [Court of Appeals] said explicitly, “Can’t you guys work something out?” And it turns out they could. So basically what the deal does is the Justice Department is agreeing not to enforce the preventive services mandate against the folks who are suing. So this is a group of conservative employers and some individual workers who say that the requirement to buy insurance that covers things like the HIV prevention drug PrEP violate their rights. And so the Biden administration is agreeing, OK, we won’t force you to buy the insurance that the law says you are required to buy. And in exchange, they agree not to push for the law to be frozen nationwide. So basically, everybody else’s insurance coverage gets to stay the same for now. There was a lot of anxiety about the nationwide injunction on the mandate that the lower judge ordered. So that is going to be on hold for now. The arguments on this case are going to drag on a lot longer, but this means that, for now, nationwide, the roles stay the same.
Carey: So how, if you know, how usual is this, in the middle of litigation, to come up with a deal that protects the people that are suing to stop a law, but it doesn’t affect the rest of the population, at least for now? I mean, is that unusual to kind of cut this kind of deal?
Ollstein: I think there has been a lot of debate recently about nationwide injunctions and the fact that some judges seem to like handing them out like candy. And just because of one person or a few people suing somewhere can bring down an entire law or program for the entire country. And there has been anxiety in the legal world about this getting kind of too common and out of hand. And so I think this is a sign that even very conservative judges like the ones on the 5th Circuit are looking for ways to rein it in and limit impacts.
Carey: Rachel, do you want to jump in? I see you nodding your head.
Cohrs: Yeah, it is just important to think about that trend, you know, as we see so many lawsuits play out. I know we’re seeing lawsuits over the Inflation Reduction Act as well. It’s a tactic that is being used. And I think if there is some more intention by DOJ to try to kind of limit the reach of these injunctions, then I think that is a really interesting trend, looking to other areas as well.
Carey: So that sounds like there’s no threat to the fall ACA enrollment season, that a ruling wouldn’t come before that enrollment season that could threaten preventive services for the entire ACA enrollment population and for those employer-sponsored plans as well.
Ollstein: So the 5th Circuit, after they blessed this deal officially, put out a briefing schedule that runs into November, so even after that, there could be more arguments, there could be an appeal up to the Supreme Court. So, yes, this is definitely running on into next year, if not longer.
Carey: OK. Well, the Supreme Court had a ruling this week that preserves Medicaid recipients’ right to sue , and policy watchers are saying that this is a major, major civil rights victory for Medicaid recipients. Before we were taping, we were chatting about it a little bit. Alice, fill us in here.
Ollstein: I mean, the specifics are that this is about a woman’s right to sue the state over the treatment of her husband in a nursing home. He was given chemical restraints, which is a horrible thing, if you look it up, that worsened his dementia. He was drugged, you know, in order to be easier to control, essentially, which is a very damaging practice. But that was sort of just the narrow issue at play. But this was seen as a major victory for any Medicaid beneficiary’s right to sue over not getting the care that they’re entitled to., and so this could have implications in the future for things like coverage of reproductive health services, including abortion, and other areas as well. So there was a lot of anxiety that this conservative Supreme Court majority would move to limit Medicaid beneficiaries’ rights to bring challenges. And that didn’t happen here.
Carey: It was a7-2 ruling, right?
Ollstein: Yeah. Yeah. It wasn’t as close as people thought.
Carey: There you go. So let’s move our discussion from the courts to Capitol Hill. Outgoing Centers for Disease Control and Prevention director Rochelle Walensky appeared before a House panel this week to talk about her agency’s response to the covid pandemic. Rachel, you covered the hearing. What were your key takeaways?
Cohrs: I mean, I think my key takeaway is that Republicans are re-litigating some of these comments that were made in early 2021 and that there wasn’t a whole lot of new revelation that came out. Walensky was pretty well prepared to stay on topic. She kind of deflected questions about gain-of-function research at NIH [the National Institutes of Health, a separate division within HHS] and lawsuits around kind of how CDC officials interacted with social media networks and regarding vaccine misinformation. So, I mean, lawmakers brought those things up, and she didn’t really engage on that at all. But she really didn’t give a lot of ground. I mean, there were criticisms of comments she had made about vaccines preventing the spread of covid-19. And I think her position was that her comments were backed by science at the time, and that as the virus has mutated, the truth about covid has changed. So I think she was not apologizing. It was not really engaging with them. And I think it was just kind of this anticlimactic kind of end. I mean, there had been so much buildup. Lawmakers had been requesting her testimony for, like, two months, and it was over and I don’t think she suffered any really significant hits there.
Carey: Were there any sort of agreement on lessons learned from how the CDC and, more broadly, the Biden administration handled its response to the pandemic? I mean, are there lessons learned here? Is there any road map to doing things differently or better next time?
Cohrs: Well, one thing she did bring up was, she said that the CDC didn’t really have visibility into how many people who were hospitalized with covid were also vaccinated. And I think that led to kind of an interesting back-and-forth. I think Republicans were obviously implying that vaccines didn’t work as well as they were initially pitched to. But I think she pivoted that to saying that “CDC would love more data on this. We don’t have the authority to collect it. And doctors are putting all this information into electronic health records and it’s not making its way to public health departments.” And so I think that kind of fits into the administration’s asks for the pandemic preparedness legislation that Congress is kind of working through right now. So I think she pivoted that to ask for more authority for her agency, which I don’t know that Republicans will be particularly enthusiastic about. But I think that was an interesting back-and-forth where she did concede that they just didn’t have a whole lot of information in the moment.
Carey: Would state health departments have to direct hospitals to collect that and then share it with the federal government, if she’s saying she doesn’t have the regulatory authority to do it?
Cohrs: I’m not an expert in this area, I’ll say. But my understanding is that the CDC was collecting information and had to, like, have individual agreements with health departments on how that was going to be collected. They couldn’t mandate that. So I think it would just make it a lot faster and I think give CDC a lot more authority to compel states to report some of this information in real time.
Carey: Sure. No, I know, that’s been one of the most interesting things in watching and reporting and reading all the coverage of how so many things changed with the covid pandemic as [we] received new information. I mean, it was a place we hadn’t been before, but we might be back there again, so. There’s another high-profile covid official who’s stepping down. Dr. Ashish Jha is leaving his post. I think today is actually his last day as the White House covid-19 response coordinator. This departure was announced a while ago, and it’s not a surprise, especially with the end of the public health emergency. But what do these departures mean for the administration’s future plans to handle covid? I mean, what message does it send to the public with these two folks leaving at this time?
Ollstein: I think if folks are already primed to think this administration is not making it a priority, this is more fodder for that viewpoint. You know, you could also note that these folks have been serving a long time in a very difficult role and this is, you know, sort of natural turnover. But I think that, with all of the protections lifting right now, and hearing very little about covid at all from the administration — I mean, the president hasn’t talked about it publicly in months; he didn’t say anything on the day the public health emergency ended, which folks were a little upset about. So you could see this as more evidence that it might not be a priority for them going forward. You know, on the other hand, they are setting up this, like, permanent pandemic office in the White House, although it doesn’t have a leader yet. So it’s a little TBD.
Raman: With Jha, you know, we don’t have someone replacing him in the way we do with a lot of other positions. So it’s going to be the first time in 14 months now that he’s not there, but it’s also, there’s not someone else there. And if you’re quietly removing that role, it just is another layer of saying, you know, this is less of a priority compared to some of the other things as it gets phased out.
Cohrs: I was just going to pop in and say that I think there’s a really interesting opening for Mandy Cohen here at CDC. There is this vacuum of leadership here. You know, the White House hasn’t appointed anyone to fill that spot. Secretary Becerra really hasn’t shown any appetite in leading on covid, and Dr. Fauci is gone, Walensky’s gone — just so many of these, like, old-guard kind of the covid response in the Biden administration have turned over. And my colleague Helen Branswell had a great story, I think that was sharp about how, you know, Mandy Cohen really is prepared, unlike a lot of other CDC directors in the past, to navigate these political dynamics. And I think it is a recognition that the CDC is political and public health is now political, and they can’t ignore that any longer. So I will be curious to see if they elevate her to communicate some more of that information in the absence of Dr. Jha.
Carey: Sure. And can you just remind our listeners who Mandy Cohen is and why she’s expected to get this job, or be nominated for this job?
Cohrs: Yes, she’s a longtime federal and state health official. I think she was in North Carolina, and most recently she was at a ACO [accountable care organization] company working with another former Obama administration official. And the White House, I think — there’s been a lot of reporting; I don’t know that they have officially tapped her yet.
Carey: I don’t think that’s happened yet. No, that has not.
Cohrs: Right. But it doesn’t have to go through a confirmation process. So if they do choose to move forward, I think the process would move pretty quickly to have her in place. So that is what our reporting has shown. Many other outlets have reported the same thing. So I think that’s just kind of the expectation for who’s next in line.
Carey: Well, let’s move on to another topic that appears frequently on this podcast, abortion. It continues to be a major news story around the country. And I’d like to start our discussion with a story that Alice did for Politico Magazine. Here’s the headline: “This Alabama Clinic Is Under Threat. It Doesn’t Provide Abortions.” So, Alice, tell us why a clinic that doesn’t provide abortion is being threatened.
Ollstein: Yeah. So when abortion became illegal in Alabama from conception, with no exemptions for rape and incest, abortion clinics either closed their doors, some picked up and moved to other states, but some, like the one I profiled, West Alabama Women’s Center, decided to stay and pivot to nonabortion services. And they have found it’s still a very hostile landscape and they very well might go out of business themselves in the coming months. They’re running into legal threats. The state attorney general has suggested that he views the kind of abortion-adjacent care they provide, you know, such as letting people know what their options are in terms of ordering pills or traveling to another state — that he might consider that aiding and abetting an abortion under the state’s criminal law. And so they are bracing for that at all times. At the same time, they have also really struggled financially. Most of their revenue in the past was from abortions, and they mainly serve a population now that struggles to pay for services and is often uninsured. The state has not expanded Medicaid, and so lots and lots of low-income people are uninsured. And so it’s just showing that what it means to be under threat in the post-Dobbs era is really different than what it meant to be under threat in the pre-Dobbs era and just how sparse the health care landscape is at all. There are just so few providers, hospitals in these areas, lots of places going out of business. And if clinics like this and other red-state clinics can’t survive, there’s going to be a lot of health care consequences.
Carey: I think in your story you said that 40% of the state was considered a maternal health desert.
Ollstein: Yeah. Right. Which means no access in those counties. And even more of the state is considered low-access, and so people are really struggling to find anywhere to go. A lot of rural hospitals have closed entirely. A lot are on the brink of closure. Some have closed their maternal care units. And so there’s just fewer and fewer options, especially fewer and fewer options for people to feel safe going to if they have an abortion either out of state or at home with pills and need follow-up care. Folks are afraid to go to a regular provider or hospital over fear of being reported to law enforcement, which is actually happening in a lot of places.
Carey: We just talked about the South. Let’s move to the Midwest. In Ohio, voters are going to head to the polls in August to weigh in on a proposal that, if passed, would require at least 60% of voters to pass any amendment to the state’s constitution. And that’s up from the current requirement of a simple majority. There would also be new, higher requirements on the number of signatures needed to get a constitutional amendment on the ballot. A Republican lawmaker in favor of the changes said they were aimed at blocking an abortion rights question that abortion rights supporters had hoped to get on the November ballot. So that’s Ohio. So in Indiana, there’s a separate issue. A class-action lawsuit asserts that the state’s abortion ban violates Hoosiers’ religious freedom. That lawsuit, which was filed by the ACLU [American Civil Liberties Union], says that Indiana’s abortion ban violates a religious freedom law that was once championed by former Indiana Gov. Mike Pence, who we know served as vice president to Donald Trump and is now challenging former President Trump and other Republicans for the 2024 GOP presidential nomination. Thoughts from the panel on these developments?
Raman: I think what’s happening in Ohio is pretty interesting because, you know, we’ve had other states before kind of try to change the threshold for passing something by ballot. And a lot of times it’s not said explicitly, but advocates have said that it’s targeting some measure, whether it’s Medicaid expansion or something else. And here we have a representative and the secretary of state kind of being pretty clear that it is about abortion in this case. And I think it being the secretary of state is especially interesting, because the secretary of state is who is certifying ballot measures and who you would look to for being the person in charge of that and making sure, you know, the t’s are crossed, the i’s dotted. So what happens there will be pretty interesting because that’s kind of an unusual play. And already we’re looking at an August ballot versus traditionally the November ballot. And a lot of times when things are pushed for a different date versus, like, traditional election day, it’s kind of, see if we can get a different turnout or kind of discourage people that might vote one way or the other. So it’ll be interesting to see how this kind of plays out in August or if there are changes before then.
Ollstein: And as for Indiana, I mean, this is one of a bunch of cases around the country where religious people are challenging abortion bans as infringing on their beliefs and right to practice. It’s sort of flipping the assumption on its head. You know, you have a lot of religious support of abortion bans. And this is showing that there are folks on the other side as well within the faith community. And it’s especially interesting in Indiana because they’re challenging one law signed by Mike Pence — the state’s pre-Dobbs abortion ban — by using another law signed by Mike Pence, which is the state’s RFRA law [Religious Freedom Restoration Act], the religious freedom law, and saying that, you know, the state law imposes one particular religion’s view of when life begins and when abortion is or is not acceptable. And that’s not shared by all people of faith. And in Judaism, a child is not a child until it takes its first breath, and that conflicts with abortion bans that are much earlier in pregnancy that sort of posit that it is a child and a life before that. So this will be really interesting to watch.
Carey: Sure. We’ll be watching all these cases very closely. But we’re going to turn now to another topic that’s important to millions of Americans, and that’s the cost of prescription drugs. Sen. Bernie Sanders — he’s a Vermont independent who chairs the Senate Health, Education, Labor and Pensions Committee, also known as the HELP Committee — he’s vowed not to move forward with any Biden administration health nominees, including the president’s pick to head the National Institutes of Health. That’s Dr. Monica Bertagnolli. Sen. Sanders is saying he’s going to keep this hold on until he sees a comprehensive plan from the White House on how to lower drug prices. What is he upset about specifically? And is he going to have other senators — have they joined him? Do you think that will be in the cards, or is this kind of a one-man band here?
Cohrs: My take on this is that he knows he can’t get the votes in Congress, so this is kind of his only option, is to try to pressure the administration to do it. And the only lever he has is nominees, so he’s using that. I don’t know how long he’ll hold out on this. I mean, it is — basically he’s arguing that the public has invested research dollars to help develop kind of the basic science that’s the foundation for a lot of important medications. And right now, the government isn’t really getting enough return on that investment. And there’s no requirement that companies that end up actually manufacturing these drugs and bringing them to market would price them in a fair, reasonable way. And so, I think his staff put out a report as well, with a release to the Post, making that argument, that the NIH could have leverage here if they chose to, and that in the past there have been clauses in contracts that could have given the government some leverage to go after these companies more aggressively but they’re just choosing not to. And so far, the Biden administration has shown no appetite to go after companies’ patents because of pricing issues. It’s never been done before. But I think, you know, Sen. Sanders realizes that he has an opening here, and he’s using the bully pulpit as much as he can. But I think ultimately I don’t see how this is resolved. And I think given that the Biden administration has overseen the passage of the most significant drug pricing reform in 20 years — which doesn’t fix all the problems, will say that. I think Sen. Sanders sent a letter about —
Carey: It’s in the Inflation Reduction Act, right?
Cohrs: Yes. Yes. The Inflation Reduction Act.
Carey: Which he voted for, OK.
Cohrs: Yes, he did vote for that. But I think there are outstanding issues about new medications especially that he’s trying to highlight here and saying, The problem isn’t fixed. We need to do more.
Carey: And so separately, a bipartisan group of Senate Finance Committee members have unveiled a proposal that they said would reform pharmacy benefit managers, or PBMs. That’s another entity we talk a lot about on the podcast. And the belief is that this measure would lower the cost of drugs. Rachel, I know that you have been covering this plan. Can you tell us about it?
Cohrs: I don’t know that this would lower the cost of drugs necessarily, and I think it’s more limited than the lawmakers who are sponsoring it have claimed it is. I think the problem that it’s trying to solve is that the payments between drugmakers and PBMs, and PBMs and the insurance companies or the employees that they’re working for, have traditionally been tied to a drug’s price. And so, just kind of like the — if anyone’s familiar with the medical loss ratio from the Affordable Care Act — it’s a similar idea, that if the price is higher, then there’s a bigger piece of the pie for everyone, percentagewise. So this bill aims to delink some of the fees in contracts with PBMs from the price of drugs. Now, this doesn’t change the rebates that drugmakers and PBMs negotiate on themselves, doesn’t touch that at all. It’s just fees. So I think it’s kind of hard to know how these work. You know, we don’t have them. They’re not public, but I think they’re trying to get at regulating this space a little bit more and trying to align those incentives a little bit better to make sure PBMs aren’t preferring more expensive medications for their own gain.
Carey: And what’s been the response from the PBM industry?
Cohrs: It is pretty fresh, but I think in general they have argued that the reason for high prices is drugmakers, because they set the prices. And I think this has been a food fight that’s been going on for a very long time. But I think lawmakers are kind of coming around to the idea of doing some sort of reform to the PBM industry. We’ll just have to wait and see what that ends up looking like.
Carey: All right. Well, we’ll keep our eyes on that one as well. And that’s this week’s news. Now we’re going to play Julie Rovner’s interview with Dan Mendelson of Morgan Health, and then we’ll be back with our extra credits.
Julie Rovner: I am pleased to welcome to the podcast Dan Mendelson, CEO of Morgan Health, a new business unit of the financial services giant JPMorgan Chase. Morgan Health’s goal is to improve health care for the company’s more than a quarter of a million employees and dependents, as well as everyone else with employer-provided insurance. If that sounds familiar, that’s because Morgan Health is the successor organization to Haven Healthcare. That was the high-profile 2018 project of JPMorgan, Amazon, and Berkshire Hathaway to remake the U.S. health care system from the ground up, led by one of the nation’s leading health care thinkers, surgeon, author, and policy wonk Atul Gawande. Today, Gawande is running global health programs at the U.S. Agency for International Development. Haven is no more. And if you listened to our special 300th episode earlier this month, our experts came down pretty hard on employers’ contributions to fixing what ails the health care system. So I’ve asked Dan here to talk about what is going on. Welcome, Dan.
Dan Mendelson: My pleasure.
Rovner: So, Dan may not have as high a public profile as Atul Gawande, but he has broad and long experience in health policy, from overseeing federal health programs at the Office of Management and Budget during the Bill Clinton administration to founding and growing Avalere Health, a successful health care consulting and advisory group. Dan, why did this job appeal to you and what made you think you could succeed where so many have tried before and failed, including very recently?
Mendelson: Look, this is a collaborative effort, and we’re working closely with a whole range of stakeholders from insurers to providers. I mean, the work that we’re doing in Columbus, for example, is with a really innovative primary care practice called Central Ohio Primary Care that has broad experience in delivering value through accountable care models in Medicare. So, I’d say that our belief that we will succeed really comes from the fact that we’re taking a very collaborative approach with other stakeholders in the health care system.
Rovner: Let’s start at the very beginning. Why are employers interested in the nation’s health care system and how it works? For most of them, it’s not their main line of business.
Mendelson: Well, I’d say that employers feel an obligation to provide insurance for their employees, and it’s an important benefit, and it’s one that employees expect. And it’s also an opportunity for employers to provide for the health and well-being of their employees.
Rovner: So employers really did used to drive a lot of health care innovation, probably coming only after Medicare in terms of shifting actual health care delivery. But they seem to have taken a back seat lately. What changed?
Mendelson: Well, look, you know, you had employers really active in the quality movement, and NCQA came out of employer interest, for example. So there really was kind of a head of steam. But it did wane. And I think that anyone who’s looking at the scene sees that Medicare and Medicaid have made a lot of progress with respect to driving accountable care and quality, whereas, at this point, there’s really … most of what’s happening through employers is fee for service. And it’s really problematic in terms of driving the quality agenda.
Rovner: And NCQA, that’s …?
Mendelson: National Commission for Quality Assurance.
Rovner: Thank you. The National Commission for Quality Assurance. Yeah, which used to be a big deal. And you’re right, I think most of what we’re seeing is now going on in the Medicare and Medicaid space. I feel like, you know, the millions of people who have employer-provided insurance right now have three main problems: the increasing unaffordability of care, with large and growing deductibles and copays; the increasing time and effort it takes to figure out what is and isn’t covered, and fighting for things that aren’t covered to be covered sometimes; and the fragmentation of the delivery system, making what was already hard to navigate very nearly impenetrable for some people, including people who are sick. I assume you’re trying to address all of those.
Mendelson: Yeah, we’re focused on quality and improving the quality of services, for sure. We’re focused on affordability. And then the one that you didn’t mention is health equity, which is one of the most difficult aspects of health care in America today, and certainly our focus as well. I mean, we see inequity in the health care system in the employer space, as well as in Medicare and Medicaid. So that’s also a target for us.
Rovner: What kind of steps are you taking to fix some of these problems? I mean, I know it’s what people get frustrated most with. It’s, like, they have insurance, but they feel like they can’t use it very well.
Mendelson: Yes. So, the way that we’re structured, there are three things that we’re doing to address these issues. And I’d say that we see our efforts as very collaborative. So we don’t believe that we alone can fix these problems, but rather what we’re doing is really driving innovation and trying to get employers, more broadly, focused on innovation in health care. So there are three ways that we’re doing this. First is that we’re investing, from the JPMorgan Chase balance sheet, in innovative health care companies that are proven to drive quality, improve quality, reduce costs, and better health equity. So that’s the first piece. And we can talk a little bit about some of the investments that we’ve made in the first two years of our operation.
Rovner: Give me one example of a company that’s doing that that you’re investing in.
Mendelson: Yes. An example is apree health. apree is a company that offers a[n] accountable care product to employers. And we’re using apree in Columbus, where we have 40,000 employees and dependents, and we’re now offering their services to our employees as an option to drive better health care.
Rovner: What do you see as the biggest challenge in health care going forward, particularly from the employer point of view?
Mendelson: Well, look, we’ve talked about a number of the issues. I’d say that, you know, we’re focused broadly on accountable care — and “accountable care” meaning making sure that there is a focus on quality and cost that is being held by an organization that can really take responsibility for care. So, to me, it’s really about alignment of incentives and making sure that those incentives are aligned not only in the employer sector but also across in the public programs.
Rovner: So you’re involved in private equity and, you know, the track record of private equity in health care, which was supposed to be an effort to get incentives aligned, hasn’t always worked out so well. I mean, in a lot of cases we’ve seen private equity just sucking money out of the health care system rather than putting it back in.
Mendelson: Look, as an investor, what we’re focused on is finding companies that are driving innovation and helping them succeed. And we’re putting our capital behind these companies, but we’re also really spending the time with them to make sure that they can be effective. And so, you know, we’ve done five investments over the course of two years, and they’re not only in accountable care, but also making sure that there’s good primary care in the system, driving better digital care, shifting expensive care from inpatient and outpatient settings into the home. So these are all facets of how employer-sponsored health care needs to be improved, and that’s the focus of our investing.
Rovner: So what does it look like when you get it all fixed?
Mendelson: When we get it all fixed …? I mean, look, I think we’re going to be at this for quite some time. But it’s really important for employers to articulate their needs and to make sure that those who are offering insurance for their employees are actually being attentive to not only cost but also quality and health equity. And I think that the facet that we’re really looking for is to make sure that health care improves and that these improvements are coming along not only in the public programs but also in the employer sector.
Rovner: Dan Mendelson, thank you so much for joining us.
Mendelson: My pleasure.
Carey: All right. We’re back, and it’s time for our extra credit segment. That’s when we each recommend a story that we read this week and we think you should read it, too. As always, don’t worry if you miss it. We’ll post the links on the podcast page at kffhealthnews.org and in the show notes on your phone or other mobile device. So, Alice, why don’t you go first this week?
Ollstein: Sure. I chose a piece in Stat by Brittany Trang and Elaine Chen. It’s called “AMA Asks Doctors to De-Emphasize Use of BMI in Gauging Health and Obesity.” I’ve heard in the medical community there has been a lot of discussion about moving away from using the BMI [body mass index] to evaluate people’s health. It was created to track population-level statistics and was never intended to be used to gauge individual health. It was not invented by someone with a medical background at all. And so people have been saying that, you know, it’s inaccurate and it leads to a lot of stigma. And so it’s interesting to see that sort of bubble up to this very mainstream, leading health care organization saying, “Look, you can’t just rely on the BMI. You also have to look at all these other factors.” Because extremely fit NFL players have really high BMIs, you know. You can’t — someone’s size does not necessarily determine their health. You can have people of all sizes be healthy or unhealthy. So this was encouraging to see.
Carey: Great. And for folks interested in more on that, we have a lot of coverage on that at kffhealthnews.org, so check that out. Rachel, why don’t you go next?
Cohrs: Sure. My piece this week is by one of Alice’s colleagues in Politico, Megan Messerly, and the headline is “Thousands Lose Medicaid in Arkansas: Is This America’s Future?” And she kind of got out beyond the Beltway and just spent some time in Arkansas really talking to everyday people who were having trouble staying on Medicaid. And I think it’s easy to get caught up in just talking about numbers and talking about policies and all of that. But I think she really brought to life the issues and the barriers that some people are facing in Arkansas, which really is the center of these disenrollments that we’re seeing right now. So I think it was really timely, really well done, very much put the human face on both the people who are getting disenrolled, but also kind of some of the on-the-ground efforts to stop that from happening and just kind of the challenges that they are working on with these compressed timelines. I thought it was really well done.
Carey: Yeah, it’s a great story. Sandhya.
Raman: My extra credit this week is called “Suicide Hotlines Promise Anonymity. Dozens of Their Websites Send Sensitive Data to Facebook.” It’s by Colin Lecher and Jon Keegan for The Markup in partnership with Stat. And I thought this was just a really interesting piece that investigated whether crisis center websites that were using Meta Pixel, which is like a piece of code that tracks user behavior for advertising that a lot of sites use — and just, like, the worry here is sharing sensitive information to Facebook, especially when it is personally identifiable. And with the crisis center, it’s much, much more sensitive data than, you know, maybe, like, shopping habits. And so they looked at data from 186 local call center websites. And I will let you read to see how many of them were using this.
Carey: Mine is from Ruth Marcus at The Washington Post. And it’s called “I Lost 40 Pounds on Ozempic. But I’m Left With Even More Questions.” In this article, she talks about her lifelong struggle to lose weight, to keep it off, but how those pounds always find their way back. And Marcus explores the history and the science behind the weight loss drugs. And she also takes on societal debate over obesity itself: Do we think of it as a personal failing, or is it a disease, a chronic condition whose underpinnings are in genetics and brain chemistry? It is a great read. All right. That’s our show for the week. And as always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left a review; that helps other people find us too. Special thanks, as always, to the amazing Francis Ying, our producer. You can email us with your comments or questions. We’re at whatthehealth@kff.org. Or you can tweet me. I’m @maryagnescarey.
Carey: Alice.
Ollstein: @AliceOllstein.
Carey: Rachel.
Cohrs: @rachelcohrs.
Carey: And Sandhya.
Raman: @SandhyaWrites.
Carey: We’ll be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ ‘What the Health? on Spotify, Apple Podcasts, Stitcher, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 4 months ago
Health Care Costs, Health Industry, Medicaid, Medicare, Multimedia, Abortion, Drug Costs, KFF Health News' 'What The Health?', Legislation, Podcasts, U.S. Congress, Women's Health
Debt Deal Leaves Health Programs (Mostly) Intact
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
A final deal cut between President Joe Biden and House Republicans extends the U.S. debt ceiling deadline to 2025 and reins in some spending. The bill signed into law by the president will preserve many programs at their current funding levels, and Democrats were able to prevent any changes to the Medicare and Medicaid programs.
Still, millions of Americans are likely to lose their Medicaid coverage this year as states are once again allowed to redetermine who is eligible and who is not; Medicaid rolls were frozen for three years due to the pandemic. Data from states that have begun to disenroll people suggests that the vast majority of those losing insurance are not those who are no longer eligible, but instead people who failed to complete required paperwork — if they received it in the first place.
This week’s panelists are Julie Rovner of KFF Health News, Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico, Lauren Weber of The Washington Post, and Jessie Hellmann of CQ Roll Call.
Panelists
Jessie Hellmann
CQ Roll Call
Joanne Kenen
Johns Hopkins Bloomberg School of Public Health and Politico
Lauren Weber
The Washington Post
Among the takeaways from this week’s episode:
- Lawmakers and White House officials spared health programs from substantial spending cuts in a last-minute agreement to raise the nation’s debt ceiling. And Biden named Mandy Cohen, a former North Carolina health director who worked in the Obama administration, to be the next director of the Centers for Disease Control and Prevention. Though she lacks academic credentials in infectious diseases, Cohen enters the job with a reputation as someone who can listen and be listened to by both Democrats and Republicans.
- The removal of many Americans from the Medicaid program, post-public health emergency, is going as expected: With hundreds of thousands already stripped from the rolls, most have been deemed ineligible not because they don’t meet the criteria, but because they failed to file the proper paperwork in time. Nearly 95 million people were on Medicaid before the unwinding began.
- Eastern and now southern parts of the United States are experiencing hazardous air quality conditions as wildfire smoke drifts from Canada, raising the urgency surrounding conversations about the health effects of climate change.
- The drugmaker Merck & Co. sued the federal government this week, challenging its ability to press drugmakers into negotiations over what Medicare will pay for some of the most expensive drugs. Experts predict Merck’s coercion argument could fall flat because drugmakers voluntarily choose to participate in Medicare, though it is unlikely this will be the last lawsuit over the issue.
- In abortion news, some doctors are pushing back against the Indiana medical board’s decision to reprimand and fine an OB-GYN who spoke out about providing an abortion to a 10-year-old rape victim from Ohio. The doctors argue the decision could set a bad precedent and suppress doctors’ efforts to communicate with the public about health issues.
Also this week, Rovner interviews KFF Health News senior correspondent Sarah Jane Tribble, who reported the latest KFF Health News-NPR “Bill of the Month” feature, about a patient with Swiss health insurance who experienced the sticker shock of the U.S. health care system after an emergency appendectomy. If you have an outrageous or exorbitant medical bill you want to share with us, you can do that here.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: The New York Times’ “This Nonprofit Health System Cuts Off Patients With Medical Debt,” by Sarah Kliff and Jessica Silver-Greenberg.
Jessie Hellmann: MLive’s “During the Darkest Days of COVID, Some Michigan Hospitals Made 100s of Millions,” by Matthew Miller and Danielle Salisbury.
Joanne Kenen: Politico Magazine’s “Can Hospitals Turn Into Climate Change Fighting Machines?” by Joanne Kenen.
Lauren Weber: The Washington Post’s “Smoke Brings a Warning: There’s No Escaping Climate’s Threat to Health,” by Dan Diamond, Joshua Partlow, Brady Dennis, and Emmanuel Felton.
Also mentioned in this week’s episode:
KFF Health News’ “As Medicaid Purge Begins, ‘Staggering Numbers’ of Americans Lose Coverage,” by Hannah Recht.
Click to open the transcript
Transcript: Debt Deal Leaves Health Programs (Mostly) Intact
KFF Health News’ ‘What the Health?’Episode Title: Debt Deal Leaves Health Programs (Mostly) IntactEpisode Number: 301Published: June 8, 2023
[Editor’s note: This transcript, generated using transcription software, has been edited for style and clarity.]
Julie Rovner: Hello and welcome back to “What the Health?”. I’m Julie Rovner, chief Washington correspondent at KFF Health News. And I’m joined by some of the best and smartest health reporters in Washington. We are taping this week from the smoky, hazy, “code purple” Washington, D.C., area on Thursday, June 8, at 10 a.m. As always, news happens fast and things might have changed by the time you hear this. So here we go. We are joined today via video conference by Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico.
Joanne Kenen: Hi, everybody.
Rovner: Lauren Weber, of The Washington Post.
Lauren Weber: Hi.
Rovner: And Jessie Hellmann, of CQ Roll Call.
Hellmann: Hello.
Rovner: Later in this episode we’ll have my interview with KFF Health News’s Sarah Jane Tribble about the latest KFF Health News-NPR “Bill of the Month.” This month is about the sticker shock of the American health care system experienced by residents of other countries. Before we get to this week’s news, I hope you all enjoyed our special panel of big health policy thinkers for our 300th episode. If you didn’t listen, you might want to go back and do that at some point. Also, that means we have two weeks of news to catch up on, so let us get to it. We’re going to start this week, I hope, for the last time with the fight over the debt ceiling. Despite lots of doubts, President Biden managed to strike a budget deal with House Republicans, which fairly promptly passed the House and Senate and was signed into law a whole two days before the Treasury Department had warned that the U.S. might default. The final package extends the debt ceiling until January 1, 2025, so after the next election, which was a big win for the Democrats, who don’t want to do this exercise again anytime soon. In exchange, Republicans got some budget savings, but nothing like the dramatic bill that House Republicans passed earlier this spring. So, Jessie, what would it do to health programs?
Hellmann: The deal cuts spending by 1.5 trillion over 10 years. It has caps on nondefense discretionary funding. That would have a big impact on agencies and programs like the NIH [National Institutes of Health], which has been accustomed to getting pretty large increases over the years. So nondefense discretionary spending will be limited to about 704 billion next fiscal year, which is a cut of about 5%. And then there’s going to be a 1% increase in fiscal 2025, which, when you consider inflation, probably isn’t much of an increase at all. So the next steps are seeing what the appropriators do. They’re going to have to find a balance between what programs get increases, which ones get flat funding — it’s probably going to be a lot of flat funding, and we’re probably at the end of an era for now with these large increases for NIH and other programs, which have traditionally been very bipartisan, but it’s just a different climate right now.
Rovner: And just to be clear, I mean, this agreement doesn’t actually touch the big sources of federal health spending, which are Medicare and Medicaid, not even any work requirements that the Republicans really wanted for Medicaid. In some ways, the Democrats who wanted to protect health spending got off pretty easy, or easier than I imagine they expected they would, right?
Hellmann: Advocates would say it could have been much worse. All things considered, when you look at the current climate and what some of the more conservative members of the House were initially asking for, this is a win for Democrats and for people who wanted to protect health care spending, especially the entitlements, because they — Republicans did want Medicaid work requirements and those just did not end up in the bill; they were a nonstarter. So, kind of health-care-related, depending on how you look at it, there was an increase in work requirements for SNAP [Supplemental Nutrition Assistance Program], which is, like, a food assistance program. So that will be extended to age 55, though they did include more exemptions for people who are veterans —
Rovner: Yeah, overall, that may be a wash, right? There may be the same or fewer people who are subject to work requirements.
Hellmann: Yeah. And all those changes would end in 2030, so —
Weber: Yeah, I just wanted to say, I mean, if we think about this — we’re coming out of a pandemic and we’re not exactly investing in the health system — I think it’s necessary to have that kind of step-back context. And we’ve seen this before. You know, it’s the boom-bust cycle of pandemic preparedness funding, except accelerated to some extent. I mean, from what I understand, the debt deal also clawed back some of the public health spending that they were expecting in the billions of dollars. And I think the long-term ramifications of that remain to be seen. But we could all be writing about that in 10 years again when we’re looking at ways that funding fell short in preparedness.
Rovner: Yeah, Joanne and I will remember that. Yeah, going back to 2001. Yeah. Is that what you were about to say?
Kenen: I mean, this happens all the time.
Weber: All the time, right.
Kenen: And we learn lessons. I mean, the pandemic was the most vivid lesson, but we have learned lessons in the past. After anthrax, they spent more money, and then they cut it back again. I mean, I remember in 2008, 2009, there was a big fiscal battle — I don’t remember which battle it was — you know, Susan Collins being, you know, one of the key moderates to cut the deal. You know, what she wanted was to get rid of the pandemic flu funding. And then a year later, we had H1N1, which turned out not to be as bad as it could have been for a whole variety of reasons. But it’s a cliche: Public health, when it works, you don’t see it and therefore people think you don’t need it. Put that — put the politics of what’s happened to public health over the last three years on top of that, and, you know, public health is always going to have to struggle for funds. Public health and larger preparedness is always going to happen to have to struggle for funds. And it would have, whether it was the normal appropriations process this year, which is still to come, or the debt ceiling. It is a lesson we do not learn the hard way.
Weber: That’s exactly right. I’ll never forget that Tom Harkin said to me that after Obama cut, he sacrificed a bunch of prevention funding for the CDC [Centers for Disease Control and Prevention] in the ACA [Affordable Care Act] deal, and he never spoke to him again, he told me, because he was so upset because he felt like those billions of dollars could have made a difference. And who knows if 10 years from now we’ll all be talking about this pivotal moment once more.
Rovner: Yeah, Tom Harkin, the now-former senator from Iowa, who put a lot of prevention into the ACA; that was the one thing he really worked hard to do. And he got it in. And as you point out, and it was almost immediately taken back out.
Weber: Yeah.
Kenen: Not all of it.
Weber: Not all of it, but a lot of it.
Kenen: It wasn’t zero.
Rovner: It became a piggy bank for other things. I do want to talk about the NIH for a minute, though, because Jessie, as you mentioned, there isn’t going to be a lot of extra money, and NIH is used to — over the last 30 years — being a bipartisan darling for spending. Well, now it seems like Congress, particularly some of the Republicans, are not so happy with the NIH, particularly the way it handled covid. There’s a new NIH director who has been nominated, Dr. Monica Bertagnolli, who is currently the head of the National Cancer Institute. This could be a rocky summer for the NIH on Capitol Hill, couldn’t it?
Hellmann: Yeah, I think there’s been a strong desire for Republicans to do a lot of oversight. They’ve been looking at the CDC. I think they’re probably going to be looking at the NIH next. Francis Collins is no longer at NIH. Anthony Fauci is no longer there. But I think Republicans have indicated they want to bring them back in to talk about some of the things that happened during the pandemic, especially when it comes to some of the projects that were funded.
Kenen: There was a lull in raising NIH spending. It was flat for a number of years. I can’t remember the exact dates, but I remember it was — Arlen Specter was still alive, and it … [unintelligible] … because he is the one who traditionally has gotten a lot of bump ups in spending. And then there was a few years, quite a few years, where it was flat. And then Specter got the spigots opened again and they stayed open for a good 10 or 15 years. So we’re seeing, and partly a fiscal pause, and partly the — again, it’s the politicization of science and public health that we did not have to this extent before this pandemic.
Rovner: Yeah, I think it’s been a while since NIH has been under serious scrutiny on Capitol Hill. Well, speaking of the CDC, which has been under serious scrutiny since the beginning of the pandemic, apparently is getting a new director in Dr. Mandy Cohen, assuming that she is appointed as expected. She won’t have to be confirmed by the Senate because the CDC director won’t be subject to Senate approval until 2025. Now, Mandy Cohen has done a lot of things. She worked in the Obama administration on the implementation of the Affordable Care Act. She ran North Carolina’s Department of Health [and Human Services], but she’s not really a noted public health expert or even an infectious disease doctor. Why her for this very embattled agency at this very difficult time?
Kenen: I think there are a number of reasons. A lot of her career was on Obamacare kind of things and on CMS kind of quality-over-quantity kind of things, payment reform, all that. She is a physician, but she did a good job in North Carolina as the top state official during the pandemic. I reported a couple of magazine pieces. I spent a lot of time in North Carolina before the pandemic when she was the state health secretary, and she was an innovator. And not only was she an innovator on things like, you know, integrating social determinants into the Medicaid system; she got bipartisan support. She developed not perfect, but pretty good relations with the state Republicans, and they are not moderates. So I think I remember writing a line that said something, you know, in one of those articles, saying something like, “She would talk to the Republicans about the return on investment and then say, ‘And it’s also the right thing to do.’ And then she would go to the Democrats and say, ‘This is the right thing to do. And there’s also an ROI.’”. So, so I think in a sort of low-key way, she has developed a reputation for someone who can listen and be listened to. I still think it’s a really hard job and it’s going to batter anyone who takes it.
Rovner: I suspect right now at CDC that those are probably more important qualities than somebody who’s actually a public health expert but does not know how to, you know, basically rescue this agency from the current being beaten about the head and shoulders by just about everyone.
Kenen: Yeah, but she also was the face of pandemic response in her state. And she did vaccination and she did disparities and she did messaging and she did a lot of the things that — she does not have an infectious disease degree, but she basically did practice it for the last couple of years.
Rovner: She’s far from a total novice.
Kenen: Yeah.
Rovner: All right. Well, it’s been a while since we talked about the Medicaid “unwinding” that began in some states in early April. And the early results that we’re seeing are pretty much as expected. Many people are being purged from the Medicaid rolls, not because they’re earning too much or have found other insurance, but because of paperwork issues; either they have not returned their paperwork or, in some cases, have not gotten the needed paperwork. Lauren, what are we seeing about how this is starting to work out, particularly in the early states?
Weber: So as you said, I mean, much like we expected to see: So 600,000 Americans have been disenrolled so far, since April 1. And some great reporting that my former colleague Hannah Recht did this past week: She reached out to a bunch of states and got ahold of data from 19 of them, I believe. And in Florida, it was like 250,000 people were disenrolled and somewhere north of 80% of them, it was for paperwork reasons. And when we think about paperwork reasons, I just want us all to take a step back. I don’t know about anyone listening to this, but it’s not like I fill out my bills on the most prompt of terms all of the time. And in some of these cases, people had two weeks to return paperwork where they may not have lived at the same address. Some of these forms are really onerous to fill out. They require payroll tax forms, you know, that you may not have easily accessible — all things that have been predicted, but the hard numbers just show is the vast majority of people getting disenrolled right now are being [dis]enrolled for paperwork, not because of eligibility reasons. And too, it’s worth noting, the reason this great Medicaid unwinding is happening is because this was all frozen for three years, so people are not in the habit of having to fill out a renewal form. So it’s important to keep that in mind, that as we’re seeing the hard data show, that a lot of this is, is straight-up paperwork issues. The people that are missing that paperwork may not be receiving it or just may not know they’re supposed to be doing it.
Rovner: As a reminder, I think by the time the three-year freeze was over, there were 90 million people on Medicaid.
Kenen: Ninety-five.
Rovner: Yeah. So it’s a lot; it’s like a quarter of the population of the country. So, I mean, this is really impacting a lot of people. You know, I know particularly red states want to do this because they feel like they’re wasting money keeping ineligible people on the rolls. But if eligible people become uninsured, you can see how they’re going to eventually get sicker, seek care; those providers are going to check and see if they’re eligible for Medicaid, and if they are, they’re going to put them back on Medicaid. So they’re going to end up costing even more. Joanne, you wanted to say something?
Kenen: Yeah. Almost everybody is eligible for something. The exceptions are the people who fall into the Medicaid gap, which is now down to 10 states.
Rovner: You mean, almost everybody currently on Medicaid is eligible.
Kenen: Anyone getting this disenrollment notification or supposed to receive the disenrollment notification that never reaches them — almost everybody is eligible for, they’re still eligible for Medicaid, which is true for the bulk of them. If they’re not, they’re going to be eligible for the ACA. These are low-income people. They’re going to get a lot heavily subsidized. Whether they understand that or not, someone needs to explain it to them. They’re working now, and the job market is strong. You know, it’s not 2020 anymore. They may be able to get coverage at work. Some of them are getting coverage at work. One of the things that I wrote about recently was the role of providers. States are really uneven. Some states are doing a much better job. You know, we’ve seen the numbers out of Florida. They’re really huge disenrollment numbers. Some states are doing a better job. Georgetown Center on Health Insurance — what’s the right acronym? — Children’s and Family. They’re tracking, they have a state tracker, but providers can step up, and there’s a lot of variability. I interviewed a health system, a safety net in Indiana, which is a red state, and they have this really extensive outreach system set up through mail, phone, texts, through the electronic health records, and when you walk in. And they have everybody in the whole system, from the front desk to the insurance specialists, able to help people sort this through. So some of the providers are quite proactive in helping people connect, because there’s three things: There’s understanding you’re no longer eligible, there’s understanding what you are eligible for, and then actually signing up. They’re all hard. You know, if your government’s not going to do a good job, are your providers or your community health clinics or your safety net hospitals — what are they doing in your state? That’s an important question to ask.
Rovner: Providers have an incentive because they would like to be paid.
Kenen: Paid.
Weber: Well, the thing about Indiana too, Joanne, I mean — so that was one of the states that Hannah got the data from. They had I think it was 53,000 residents that have lost coverage in the first amount of unwinding. 89% of them were for paperwork. I mean, these are not small fractions. I mean, it is the vast majority that is being lost for this reason. So that’s really interesting to hear that the providers there are stepping up to face that.
Kenen: It’s not all of them, but you can capture these people. I mean, there’s a lot that can go wrong. There’s a lot that — in the best system, you’re dealing with [a] population that moves around, they don’t have stable lives, they’ve got lots of other things to deal with day to day, and dealing with a health insurance notice in a language you may not speak delivered to an address that you no longer live at — that’s a lot of strikes.
Rovner: It is not easy. All right. Well, because we’re in Washington, D.C., we have to talk about climate change this week. My mother, the journalist, used to say whenever she would go give a speech, that news is what happens to or in the presence of an editor. I have amended that to say now news is what happens in Washington, D.C., or New York City. And since Washington, D.C., and New York City are both having terrible air quality — legendary, historically high air quality — weeks, people are noticing climate change. And yes, I know you guys on the West Coast are saying, “Uh, hello. We’ve been dealing with this for a couple of years.” But Joanne and Lauren, both of your extra credits this week have to do with it. So I’m going to let you do them early. Lauren, why don’t you go first?
Weber: Yeah, I’ve highlighted a piece by my colleague Dan Diamond and a bunch of other of my colleagues, who wrote all about how this is just a sign of what’s to come. I mean, this is not something that is going away. The piece is titled “Smoke Brings a Warning: There’s No Escaping Climate’s Threat to Health.” I think, Julie, you hit the nail on the head. You know, we all live here in Washington, D.C. A lot of other journalist friends live in New York. There’s been a lot of grousing on Twitter that everyone is now covering this because they can see it. But the reality is, when people can see it, they pay attention. And so the point of the story is, you know, look, I mean, this is climate change in action. We’re watching it. You know, it’s interesting; this story includes a quote from Mitch McConnell saying [to] follow the public health authorities, which I found to be quite fascinating considering the current Republican stance on some public health authorities during the pandemic. And I’m just very curious to see, as we continue to see this climate change in reality, how that messaging changes from both parties.
[Editor’s note: The quote Weber referenced did not come from McConnell but from Senate Majority Leader Chuck Schumer, a Democrat, and would not have warranted as much fascination in this context.]
Kenen: But I think that you’ve seen, with the fires on the West Coast, nobody is denying that there’s smoke and pollutants in the air — of either party. You know, we can look out our windows and see it right now, right? But they’re not necessarily accepting that it’s because of climate change, and that — I’m not sure that this episode changes that. Because many of the conservatives say it’s not climate change; it’s poor management of forests. That’s the one you hear a lot. But there are other explain — or it’s just, you know, natural variation and it’ll settle down. So it remains to be seen whether this creates any kind of public acknowledgment. I mean, you have conservative lawmakers who live in parts of the country that are already very — on coasts, on hurricane areas, and, you know, forest fire areas there. You have people who are already experiencing it in their own communities, and it does not make them embrace the awareness of poor air quality because of a forest fire. Yes. Does it do what Julie was alluding to, which is change policy or acknowledging what, you know, the four of us know, and many millions of other people, you know, that this is related to climate change, not just — you know, I’m not an expert in forestry, but this is not just — how many fires in Canada, 230?
Rovner: Yeah. Nova Scotia and Quebec don’t tend to have serious forest fire issues.
Kenen: Right. This is across — this is across huge parts of the United States now. It’s going into the South now. I was on the sixth floor of a building in Baltimore yesterday, and you could see it rolling in.
Rovner: Yeah. You have a story about people trying to do something about it. So why don’t you tell us about that.
Kenen: Well it was a coincidence that that story posted this week, because I had been working on it for a couple of months, but I wrote a story. The headline was — it’s in Politico Magazine — it’s “Can Hospitals Turn Into Climate Change Fighting Machines?” Although one version of it had a headline that I personally liked more, which was “Turn Off the Laughing Gas.” And it’s about how hospitals are trying to reduce their own carbon footprint. And when I wrote this story, I was just stunned to learn how big that carbon footprint is. The health sector is 8.5% of greenhouse gas emissions in the United States, and that’s twice as high as the health sector in comparable industrial countries, and —
Rovner: We’re No. 1!
Kenen: Yes, once again, and most of it’s from hospitals. And there’s a lot that the early adopters, which is now, I would say about 15% of U.S. hospitals are really out there trying to do things, ranging from changing their laughing gas pipes to composting to all sorts of, you know, energy, food, waste, huge amount of waste. But one of the — you know, everything in hospitals is use once and throw it out or unwrap it and don’t even use it and still have to throw it out. But one of the themes of the people I spoke to is that hospitals and doctors and nurses and everybody else are making the connection between climate change and the health of their own communities. And that’s what we’re seeing today. That’s where the phenomenon Laura was talking about is connected. Because if you look out the window and you can see the harmful air, and some of these people are going to be showing up in the emergency rooms today and tomorrow, and in respiratory clinics, and people whose conditions are aggravated, people who are already vulnerable, that the medical establishment is making the connection between the health of their own community, the health of their own patients, and climate. And that’s where you see more buy-in into this, you know, greening of American hospitals.
Rovner: Speaking of issues that that seem insoluble but people are starting to work on, drug prices. In drug price news, drug giant Merck this week filed suit against the federal government, charging that the new requirements for Medicare price negotiation are unconstitutional for a variety of reasons. Now, a lot of health lawyers seem pretty dubious about most of those claims. What’s Merck trying to argue here, and why aren’t people buying what they’re selling?
Hellmann: So there’s two main arguments they’re trying to make. The primary one is they say this drug price negotiation program violates the Fifth Amendment, which prohibits the government from taking private property for public use without just compensation. So they argue that under this negotiation process they would basically be coerced or forced into selling these drugs for a price that they think is below its worth. And then the other argument they make is it violates their First Amendment rights because they would be forced to sign an agreement they didn’t agree with, because if they walk away from the negotiations, they have to pay a tax. And so it’s this coercive argument that they are making. But there’s been some skepticism. You know, Nick Bagley noted on Twitter that it’s voluntary to participate in Medicare. Merck doesn’t have a constitutional right to sell its drugs to the government at a price that they have set. And he also noted — I thought this was interesting — I didn’t know that there was kind of a similar case 50 years ago, when Medicare was created. Doctors had sued over a law Congress passed requiring that a panel review treatment decisions that doctors were making. The doctors sued also under the Fifth Amendment in the courts, and the Supreme Court sided with the government. So he seems to think there’s a precedent in favor of the government’s approach here. And there just seems to be a lot of skepticism around these arguments.
Rovner: And Nick Bagley, for those of you who don’t know, is a noted law professor at the University of Michigan who specializes in health law. So he knows whereof he speaks on this stuff. I mean, Joanne, you were, you were mentioning, I mean, this was pretty expected somebody was going to sue over this.
Kenen: It’s probably not the last suit either. It’s probably the first of, but, I mean, the government sets other prices in health care. And, you know, it sets Medicare Advantage rates. It sets rates for all sorts of Medicare procedures. The VA [U.S. Department of Veterans Affairs] sets prices for every drug that’s in its formulary or, you know, buys it at a negotiated —
Rovner: Private insurers set prices.
Kenen: Right. But that’s not government. That’s different.
Rovner: That’s true.
Kenen: They’re not suing private insurers. So, you know, I’m not Nick Bagley, but I usually respect what Nick Bagley has to say. On the other hand, we’ve also seen the courts do all sorts of things we have not expected them to do. There’s another Obamacare case right now. So, precedent, schmecedent, you know, like — although on this one we did expect the lawsuits. Somebody also pointed out, I can’t remember where I read it, so I’m sorry not to credit it, maybe it was even Nick — that even if they lose, if they buy a extra year or two, they get another year or two of profits, and that might be all they care about.
Rovner: It may well be. All right. Well, let us turn to abortion. It’s actually been relatively quiet on the abortion front these last couple of weeks as we approach the one-year anniversary of the Supreme Court striking down Roe v Wade. I did want to mention something that’s still going on in Indiana, however. You may remember the case last year of the 10-year-old who was raped in Ohio and had to go to Indiana to have the pregnancy terminated. That was the case that anti-abortion activists insisted was made up until the rapist was arraigned in court and basically admitted that he had done it. Well, the Indiana doctor who provided that care is still feeling the repercussions of that case. Caitlin Bernard, who’s a prominent OB-GYN at the Indiana University Health system, was first challenged by the state’s attorney general, who accused her of not reporting the child abuse to the proper state authorities. That was not the case; she actually had. But the attorney general, who’s actually a former congressman, Todd Rokita, then asked the state’s medical licensing board to discipline her for talking about the case, without naming the patient, to the media. Last month, the majority of the board voted to formally reprimand her and fine her $3,000. Now, however, lots of other doctors, including those who don’t have anything to do with reproductive health care, are arguing that the precedent of punishing doctors for speaking out about important and sometimes controversial issues is something that is dangerous. How serious a precedent could this turn out to be? She didn’t really violate anybody’s private — she didn’t name the patient. Lauren, you wanted to respond.
Weber: Yeah, I just think it’s really interesting. If you look at the context, the number of doctors that actually get dinged by the medical board, it’s only a couple thousand a year. So this is pretty rare. And usually what you get dinged for by the medical board are really severe things like sexual assault, drug abuse, alcohol abuse. So this would seem to indicate quite some politicization, and the fact that the AG was involved. And I do think that, especially in the backdrop of all these OB-GYN residents that are looking to apply to different states, I think this is one of the things that adds a chilling effect for some reproductive care in some of these red states, where you see a medical board take action like this. And I just think in general — it cannot be stated enough — this is a rare action, and a lot of medical board actions will be, even if there is an action, will be a letter in your file. I mean, to even have a fine is quite something and not it be like a continuing education credit. So it’s quite noteworthy.
Rovner: Well, meanwhile, back in Texas, the judge who declared the abortion pill to have been wrongly approved by the FDA, Trump appointee Matthew Kacsmaryk, is now considering a case that could effectively bankrupt Planned Parenthood for continuing to provide family planning and other health services to Medicaid patients while Texas and Louisiana were trying to kick them out of the program because the clinics also provided abortions in some cases. Now, during the time in question, a federal court had ordered the clinics to continue to operate as usual, banning funding for abortions, which always has been the case, but allowing other services to be provided and reimbursed by Medicaid. This is another of those cases that feels very far-fetched, except that it’s before a judge who has found in favor of just about every conservative plaintiff that has sought him out. This could also be a big deal nationally, right? I mean, Planned Parenthood has been a participant in the Medicaid program in most states for years — again, not paying for abortion, but for paying for lots of other services that they provide.
Kenen: The way this case was structured, there’s all these enormous number of penalties, like 11,000 per case or something, and it basically comes out to be $1.8 billion. It would bankrupt Planned Parenthood nationally, which is clearly the goal of this group, which has a long history that — we don’t have time to go into their long history. They’re an anti-abortion group that’s — you know, they were filming people, and there’s a lot of history there. It’s the same people. But, you know, this judge may in fact come out with a ruling that attempts to shut down Planned Parenthood completely. It doesn’t mean that this particular decision would be upheld by the 5th Circuit or anybody else.
Rovner: Or not. The same way the mifepristone ruling finally woke up other drugmakers who don’t have anything to do with the abortion fight because, oh my goodness, if a judge can overturn the approval of a drug, what does the FDA approval mean? This could be any government contractor — that you can end up being sued for having accepted money that was legal at the time you accepted it, which feels like not really a very good business partner issue. So another one that we will definitely keep an eye on.
Kenen: I mean, that’s the way it may get framed later, is that this isn’t really about Planned Parenthood; this is about a business or entity obeying the law, or court order. I mean, that’s how the pushback might come. I mean, I think people think Planned Parenthood, abortion, they equate those. And most Planned Parenthood clinics do not provide abortion, while those that do are not using federal funds, as a rule; there are exceptions. And Planned Parenthood is also a women’s health provider. They do prenatal care in some cases; they do STD [sexually transmitted disease] treatment and testing. They do contraception. They, you know, they do other things. Shutting down Planned Parenthood would mean cutting off many women’s access to a lot of basic health care.
Rovner: And men too, I am always reminded, because, particularly for sexually transmitted diseases, they’re an important provider.
Kenen: Yeah. HIV and other things.
Rovner: All right. Well, that is this week’s news. Now we will play my “Bill of the Month” interview with Sarah Jane Tribble, and then we will be back with our extra credits. We are pleased to welcome back to the podcast Sarah Jane Tribble, who reported and wrote the latest KFF Health News-NPR “Bill of the Month” story. Sarah, thanks for coming in.
Sarah Jane Tribble: Thanks for having me.
Rovner: So this month’s patient is a former American who now lives in Switzerland, a country with a very comprehensive health insurance system. But apparently it’s not comprehensive enough to cover the astronomical cost of U.S. health care. So tell us who the patient is and how he ended up with a big bill.
Tribble: Yeah. Jay Comfort is an American expatriate, and he has lived overseas for years. He’s a former educator. He’s 66 years old. And he decided to retire in Switzerland. He has that country’s basic health insurance plan. He pays his monthly fee and gets a deductible, like we do here in the U.S. He traveled last year for his daughter’s wedding and ended up with an emergency appendectomy in the ER [emergency room] at the University of Pittsburgh in Williamsport.
Rovner: And how big was the ultimate bill?
Tribble: Well, he was in the hospital just about 14 hours, and he ended up with a bill of just over $42,000.
Rovner: So not even overnight.
Tribble: No.
Rovner: That feels like a lot for what was presumably a simple appendectomy. Is it a lot?
Tribble: We talked to some experts, and it was above what they had predicted it would be. It did include the emergency appendectomy, some scans, some laboratory testing, three hours in the recovery room. There was also some additional diagnostic testing. They had sent off some cells for a diagnostics and did find cancer at the time. Still, it didn’t really explain all the extra cost. Healthcare Bluebook, which you can look up online, has this at about $14,000 for an appendectomy. One expert told me, if you look at Medicare prices and average out in that region, it would be between $6,500 and $18,000-ish. So, yeah, this was expensive compared to what the experts told us.
Rovner: So he goes home and he files a claim with his Swiss insurance. What did they say?
Tribble: Well, first let me just say, cost in the U.S. can be two to three times that in other countries. Switzerland isn’t known as a cheap country, actually. Its health care is —
Rovner: It’s the second most expensive after the U.S.
Tribble: Considered the most expensive in Europe, right. So this is pretty well known. So he was still surprised, though, when he got the response from his Swiss insurance. They said they were willing to pay double because it was an emergency abroad. Total, with the appendectomy and some extra additional scans and so forth: About $8,000 is what they were willing to pay.
Rovner: So, double what they would have paid if he’d had it done in Switzerland.
Tribble: Yeah.
Rovner: So 42 minus 8 leaves a large balance left. Yeah. I mean, he’s stuck with — what is that — $34,000. He’s on the hook for that. I mean, it’s better than having nothing, obviously, but it’s a lot of money and it’s really striking, the difference, because, you know, in Switzerland, they’re very much like, we would pay this amount, then we’ll double it to pay you back. And he still has this enormous bill he’s left paying. He’s on a fixed income. He’s retired. So it’s quite the shock to his system.
Rovner: So what happened? Has this been resolved?
Tribble: Let me first tell you what happened at the ER, because Jay was very diligent about providing documents and explaining everything. We had multiple Zoom calls. Jay’s wife was with him, and she provided the Swiss insurance card to UPMC. Now, UPMC had confirmed that there was some confusion, and it took months for Jay to get his bill. He had to call and reach out to UPMC to get his bill. He wants to pay his bill. He wants to pay his fair share, but he doesn’t consider $42,000 a fair share. So he wants to now negotiate the bill. We’ve left it at that, actually. UPMC says they are charging standard charges and that he has not requested financial assistance. And Jay says he would like to negotiate his bill.
Rovner: So that’s where we are. What is the takeaway here? Obviously, “don’t have an emergency in a country where you don’t have insurance” doesn’t feel very practical.
Tribble: Well, yeah, I mean, this was really interesting for me. I’ve been a health care reporter a long time. I’ve heard about travel insurance. The takeaway here for Jay is he would have been wise to get some travel insurance. Now, Jay did tell me previously he had tried to get Medicare. He is a U.S. citizen residing in Switzerland. He does qualify. He had worked in the U.S. long enough to qualify for it. He had gone through some phone calls and so forth and didn’t have it before coming here. He told me in the last couple of weeks that he now has gotten Medicare. However, that may not have helped him too much because it was an outpatient procedure. And it’s important to note that if you have Medicare and you’re 65 in the U.S., when you go overseas, it’s not likely to cover much. So the takeaway: Costs in the U.S. are more expensive than most places in the world, and you should be prepared if you’re traveling overseas and you find yourself in a situation, you might consider travel insurance anyway.
Rovner: So both ways.
Tribble: Yeah.
Rovner: Americans going somewhere else and people from somewhere else coming here.
Tribble: Well, if you’re a contract worker or a student on visa or somebody visiting the U.S., you’re definitely [going to] want to get some insurance because, wherever you’re coming from, most likely that insurance isn’t going to pay the full freight of what the costs are in the U.S.
Rovner: OK. Sarah Jane Tribble, thank you very much.
Tribble: Thanks so much.
Rovner: OK, we’re back, and it’s time for our extra credit segment. That’s where we each recommend a story we read this week that we think you should read, too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Lauren and Joanne, you’ve already given us yours, so Jessie, you’re next.
Hellmann: Yeah. My extra credit is from MLive.com, an outlet in Michigan. It’s titled “During the Darkest Days of COVID, Some Michigan Hospitals Made 100s of Millions.” They looked at tax records, audited financial statements in federal data, and found that some hospitals and health systems in Michigan actually did really well during the pandemic, with increases in operating profits and overall net assets. A big part of this was because of the covid relief funding that was coming in, but the article noted that, despite this, hospitals were still saying that they were stretched really thin, where they were having to lay off people. They didn’t have money for PPE [personal protective equipment], and they were having to institute, like, other cost-saving measures. So I thought this was a really interesting, like, a local look at how hospitals are kind of facing a backlash now. We’ve seen it in Congress a little bit, just more of an interest in looking at their finances and how they were impacted by the pandemic, because while some hospitals really did see losses, like small, rural, or independent hospitals, some of the bigger health systems came out on top. But you’re still hearing those arguments that they need more help, they need more funding.
Rovner: Well, my story is also about a hospital system. It’s yet another piece of reporting about nonprofit hospitals failing to live up to their requirement to provide, quote, “community benefits,” by our podcast panelist at The New York Times Sarah Kliff and Jessica Silver-Greenberg. It’s called “This Nonprofit Health System Cuts Off Patients With Medical Debt.” And it’s about a highly respected and highly profitable health system based in Minnesota called Allina and its policy of cutting off patients from all nonemergency services until they pay back their debts in full. Now, nonemergency services because federal law requires them to treat patients in emergencies. It’s not all patients. It’s just those who have run up debt of at least $1,500 on three separate occasions. But that is very easy to do in today’s health system. And the policy isn’t optional. Allina’s computerized appointment system will actually block the accounts of those who have debts that they need to pay off. It is quite a story, and yet another in this long list of stories about hospitals behaving badly. OK, that is our show for this week. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us too. Special thanks, as always, to our ever-patient producer, Francis Ying. As always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can tweet me, at least for now. I’m still there. I’m @jrovner. Joanne?
Kenen: @JoanneKenen
Rovner: Jessie.
Hellmann: @jessiehellmann
Rovner: Lauren.
Weber: @LaurenWeberHP
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ ‘What the Health? on Spotify, Apple Podcasts, Stitcher, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 4 months ago
Capitol Desk, Health Care Costs, Health Care Reform, Health Industry, Insurance, Medicaid, Medicare, Multimedia, Pharmaceuticals, Public Health, States, Abortion, Drug Costs, KFF Health News' 'What The Health?', Podcasts, U.S. Congress, Women's Health
When an Anti-Vaccine Activist Runs for President
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
How should journalists cover political candidates who make false claims about the safety and effectiveness of vaccines? That question will need to be answered now that noted anti-vaccine activist Robert F. Kennedy Jr. has officially entered the 2024 presidential race.
Meanwhile, South Carolina has become one of the last states in the South to pass an abortion ban, making the procedure all but impossible to obtain for women across a broad swath of the country.
This week’s panelists are Julie Rovner of KFF Health News, Alice Miranda Ollstein of Politico, Rachel Cohrs of Stat, and Sarah Karlin-Smith of the Pink Sheet.
Panelists
Rachel Cohrs
Stat News
Sarah Karlin-Smith
Pink Sheet
Alice Miranda Ollstein
Politico
Among the takeaways from this week’s episode:
- Republican lawmakers and President Joe Biden continue to bargain over a deal to avert a debt ceiling collapse. Unspent pandemic funding is on the negotiating table, as the White House pushes to protect money for vaccine development — though the administration has drawn criticism for a lack of transparency over what would be included in a clawback of unspent dollars.
- In abortion news, South Carolina is the latest state to vote to restrict access to abortion, passing legislation this week that would ban abortion after six weeks of pregnancy — shortly after pregnant people miss their first period. And Texas is seeing more legal challenges to the state law’s exceptions to protect a mother’s life, as cases increasingly show that many doctors are erring on the side of not providing care to avoid criminal and professional liability.
- Congress is scrutinizing the role of group purchasing organizations in drug pricing as more is revealed about how pharmacy benefit managers negotiate discounts. So-called GPOs offer health care organizations, like hospitals, the ability to work together to leverage market power and negotiate better deals from suppliers.
- Lawmakers are also exploring changes to the way Medicare pays for the same care performed in a doctor’s office versus a hospital setting. Currently, providers can charge more in a hospital setting, but some members of Congress want to end that discrepancy — and potentially save the government billions.
- And our panel of health journalists discusses an important question after a prominent anti-vaccine activist entered the presidential race last month: How do you responsibly cover a candidate who promotes conspiracy theories? The answer may be found in a “truth sandwich.”
Also this week, Rovner interviews KFF Health News senior correspondent Aneri Pattani about her project to track the money from the national opioid settlement.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: KFF Health News’ “Remote Work: An Underestimated Benefit for Family Caregivers,” by Joanne Kenen
Alice Miranda Ollstein: Reuters’ “How Doctors Buy Their Way out of Trouble,” by Michael Berens
Rachel Cohrs: ProPublica’s “In the ‘Wild West’ of Outpatient Vascular Care, Doctors Can Reap Huge Payments as Patients Risk Life and Limb,” by Annie Waldman
Sarah Karlin-Smith: The New York Times’ “Heat Wave and Blackout Would Send Half of Phoenix to E.R., Study Says,” by Michael Levenson
Also mentioned in this week’s episode:
- KFF Health News’ “Abortion Bans Are Driving Off Doctors and Closing Clinics, Putting Basic Health Care at Risk,” by Julie Rovner.
- Stat’s “House Panel Takes First Steps Toward Reining In Hospitals With ‘Site-Neutral’ Changes,” by Rachel Cohrs.
- Vice’s “ABC News and CNN Manage to Demonstrate Exactly What Not to Do With Robert F. Kennedy Jr.,” by Anna Merlan.
click to open the transcript
Transcript: When an Anti-Vaccine Activist Runs for President
KFF Health News’ ‘What the Health?’
Episode Title: When an Anti-Vaccine Activist Runs for President
Episode Number: 299
Published: May 25, 2023
[Editor’s note: This transcript, generated using transcription software, has been edited for style and clarity.]
Julie Rovner: Hello and welcome back to “What the Health?”. I’m Julie Rovner, chief Washington correspondent at KFF Health News. And I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, May 25, at 10 a.m. As always, news happens fast and things might have changed by the time you hear this. So here we go. Today we are joined via video conference by Rachel Cohrs of Stat News.
Rachel Cohrs: Hi, everybody.
Rovner: Sarah Karlin-Smith of the Pink Sheet.
Sarah Karlin-Smith: Hi, Julie.
Rovner: And Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Hello.
Rovner: Later in this episode we’ll have my interview with KFF Health News’ Aneri Pattani about her project tracking where all of that opioid settlement money is going. But first, this week’s news. I suppose we have to start with the debt ceiling again, because how this all eventually plays out will likely impact everything else that happens in Washington for the rest of the year. First of all, as of this taping, at 10 o’clock on Thursday morning, there’s still no settlement here, right?
Ollstein: There is not. And depending who you listen to, we are either close or not close at all, on the brink of disaster or on the brink of being all saved from disaster. There’s a lot of competing narratives going around. But yes, as of this taping, no solution.
Rovner: I want to do a spreadsheet of how often the principals come out and say, “It was productive,” “It’s falling apart,” “It was productive,” “It’s falling apart.” I mean, it seems like literally every other time, particularly when Speaker [Kevin] McCarthy comes out, it was either “very productive” or “we’re nowhere near.” That seems to have been the gist for the past two weeks or so. Meanwhile, it seems like one thing Republicans and Democrats have at least tentatively agreed to do is claw back something like $30 billion in unspent covid funds. But, not so fast. The New York Times reports that the Biden administration wants to preserve $5 billion of that to fund the next generation of covid vaccines and treatment and another $1 billion to continue giving free covid vaccines to people without insurance. I feel like this is the perfect microcosm of why these talks are almost impossible to finish. They’re trying to negotiate a budget resolution, an omnibus spending bill, and a reconciliation bill all at the same time, with the sword of Damocles hanging over their head and a long holiday weekend in between. Somebody please tell me that I’m wrong about this.
Ollstein: Well, Congress never does anything unless there’s a sword of Damocles hanging over them and a vacation coming up that they really want to go on. I mean, do they ever make it happen otherwise? Not — not in our experience. But I do want to note that it is interesting that the Biden administration is trying to fight for some of that covid funding. Meanwhile, what they’re not reportedly fighting for is some of the other public health funding that’s at risk in that clawback, and I reported last week that some of Biden’s own health officials are warning that losing those tens of billions of dollars could undermine other public health efforts, including the fight against HIV and STDs [sexually transmitted diseases]. We have syphilis at record rates right now, and public health departments all around the country are counting on that money to preserve their workforces and do contact tracing, etc. And so that is another piece of this that isn’t getting as much attention.
Cohrs: There has been this ongoing fight between the White House and Republicans over covid money and how it’s being spent, for years at this point. And the White House has never really been fully transparent about exactly what was going to get clawed back. The Appropriations Committee was the one who actually put out some real information about this. And I think that trust has just been broken that the money is used where it’s supposed to be. I mean, even for the next-generation research project [Project NextGen] — I mean, they launched that like a couple of months ago, after Republicans had already threatened to take the money back. So I think there are some questions about the timing of the funding. [White House COVID-19 Response Coordinator] Ashish Jha said they didn’t know they had leftovers until recently, but I think this has just really turned into a mess for the White House, and I think the fact that they’re willing to offer some of this money up is just kind of a symbol and just a “ending with a whimper” of this whole fight that’s been going on for two years where they’ve been unsuccessful in extracting any more money.
Rovner: And yeah, I was just going to say, the White House keeps asking for more money and then they keep, quote-unquote, “finding money” to do things that are really important. Sarah, I wanted to ask you, how freaked out is the research establishment and the drug industry at whether, you know, will they or won’t they actually pony up money here?
Karlin-Smith: I think this could be pretty problematic because some of the type of companies that get this funding — some of them might be in a position to do this on their own, but others would essentially — you know, there isn’t necessarily a market for this without the government support, and that’s why they do it. That’s why the U.S. created this BARDA [Biomedical Advanced Research and Development Authority], which kind of funds this type of pandemic and other threats research. And so I think there are companies that definitely wouldn’t be able to continue without this money, because some of it is for things that we think we might need but don’t know if we definitely will. And so you don’t necessarily want to make the investment in the same way you know you need cancer drugs or something like that.
Rovner: We will see how this plays out. Perhaps it will be played out by next week or perhaps they will find some sort of short-term patch, which is another tried-and-true favorite for Congress. All right. Let’s turn to abortion. Last week, the North Carolina Legislature overrode the Democratic governor’s veto to pass a 12-week ban. This week was the South Carolina Legislature’s chance to say, “Hold my beer.” Alice, what happened in South Carolina, and what does it mean for availability of abortion in the whole rest of the South?
Ollstein: The governor is expected to sign this new restriction into law. Like many other GOP-led states. South Carolina was expected to quickly pass restrictions last year as soon as Roe v. Wade was overturned, but they got into fights within the Republican Party over how far to go, whether to have exceptions, what kind of exceptions, etc. It was the classic story we’ve seen play out over and over and over where, while Roe v. Wade was still in place, it was very easy for people to say, “I’m pro-life, I’m against abortion,” and not have to make those difficult, detailed decisions. So, yes, this could have a big impact, you know, especially with Florida moving for a much stricter ban. You know, the whole region is becoming more and more unavailable, and people are going to have to travel further and further.
Rovner: And South Carolina ended up with one of these six-week, quote-unquote, “heartbeat bills,” right?
Ollstein: That’s right.
Rovner: So it’s sort of shutting off yet another state where abortion is or really could be available. There’s more abortion-related court action, too. This week, in Texas, eight more women who experienced dangerous pregnancy complications joined a lawsuit seeking to force just a clarification of that state’s abortion ban that they say threatened their lives. One of them, Kiersten Hogan, had her water break prematurely, putting her at risk of infection and death, but says she was told by the hospital that if she tried to leave to seek care elsewhere, she could be arrested for trying to kill her baby. Four days later, the baby was born stillborn. Yet sponsors of the state’s abortion bill say it was never intended to bar, quote, “medically necessary abortions.” Why is there such a disconnect? And Texas is hardly the only place this is happening, right?
Ollstein: Yeah. Situations like this are why people are arguing that the whole debate over exceptions is sort of a fig leaf. It’s papering over how these work in practice. You can have exceptions on the book that say “life-threatening situations, medical emergencies,” etc. But because doctors are so afraid of being charged with a crime or losing their license or other professional repercussions, that’s just creating a huge chilling effect and making them afraid to provide care in these situations. A lot of times the state law also contradicts with federal law when it comes to medical emergencies, and so doctors feel caught in the middle and unsure what they’re supposed to do. And as we’re seeing, a lot of them are erring on the side of not providing care rather than providing care. So this is playing out in a lot of places. So I’m interested to see if this informs the debate in other states about whether to have these exceptions or not.
Rovner: And I get to promote my own story here, which is that we’re seeing in a lot of states either doctors leaving or doctors deciding not to train in states with abortion bans because they’re afraid of exactly those restrictions that could land them, you know, either in court or, even worse, in jail. We’ve long had abortion care deserts. Now we could see entire women’s health care deserts in a lot of these states, which would, you know, hurt not just the people who want to have abortions, but the people who want to get pregnant and have babies. We will continue to watch that space. Well, meanwhile, in West Virginia, another court case, filed by the maker of the generic version of the abortion pill mifepristone, could turn on a recent Supreme Court decision about pork products in California. Can somebody explain what one has to do with the other?
Karlin-Smith: There is basically a ruling that the Supreme Court issued the other week in a California case where the state was regulating how pigs were treated on farms in California. And the court basically allowed the law to stand, saying, you know, it didn’t interfere with interstate commerce. And the people who are protesting GenBioPro’s suit in West Virginia are basically saying that this, again, is an example where West Virginia’s regulation of the abortion drug, again, doesn’t really impact the distribution of the drug outside of the state or the availability of the drug outside of the state, and so this should be allowable. Of course, GenBioPro and the folks who are protesting how West Virginia is curtailing access to the suit are trying to argue the same ruling helps their cause. To me, what I read — and it seems like the comparison works better against the drug company, but it always is interesting to see this overlapping — you know, the cases you don’t expect. But I also, I think, when this ruling came out, saw somebody else making another argument that this should help GenBioPro. So it’s very hard to know.
Rovner: If it’s not confusing enough, I’m going to add another layer here: While we’re talking about the abortion pill, a group of House Democrats are reaching out to drug distribution company AmerisourceBergen, following reports that it would decline to deliver the pill to pharmacies in as many as 31 states, apparently fearing that they would be drawn into litigation between states and the federal government, the litigation we’ve talked about now a lot. So far, the company has only said that it will distribute the drug in states, quote, “where it is consistent with the law.” In the end, this could end up being more important than who wins these lawsuits, right? If — I think they’re the sole distributor — is not going to distribute it, then it’s not going to be available.
Ollstein: It also depends on the — at the 5th Circuit, and that will go back to the Supreme Court, because if it’s not an FDA-approved drug, then nobody can distribute it. That’s the ultimate controlling factor. But yes, since they are the sole distributor, they will have a lot of power over where this goes. And when I was reporting on Walgreens’ decision, they were pointing to this and saying that their decisions, you know, depend on other factors as well.
Karlin-Smith: And there’s a lot of nuance to this because my understanding is AmerisourceBergen, they’re particularly talking about distributing it to pharmacies where you could — under this new FDA permission to let pharmacies distribute the drug, which in the past they hadn’t.
Rovner: And which hasn’t happened yet.
Karlin-Smith: Right. They haven’t actually gone through the process of certifying the pharmacies. So it’s like a little bit premature, which is why I think Walgreens realized they probably jumped the gun on making any decision because it couldn’t happen yet anyway. But AmerisourceBergen is still saying, “Oh, we’re giving it to providers and other places that can distribute the drug in some of these states.” So it’s not necessarily like the drug is completely unavailable. It’s just about ease of access, I think, at this point.
Rovner: Yeah, we’re not just in “watch that space”; now we’ve progressed to “watch all those spaces,” which we will continue to do. Well, while we were on the discussion of drug middlepeople, there’s a story in Stat about the Federal Trade Commission widening its investigation of pharmacy benefit managers to include group purchasing organizations. Sarah, what are group purchasing organizations and how do they impact the price of prescription drugs?
Karlin-Smith: So group purchasing organizations are basically where you sort of pool your purchasing power to try and get better deals or discounts. So like, in this case, one of the GPOs FTC is looking at negotiates drug rebates on behalf of a number of different PBMs, not just one PBM. And so, again, you know, the idea is the more people you have, the more marketing you have, the better discount you should be able to get, which is — I think some people have been a little shocked by this because they’re like, “Wait, we thought the PBMs were the ones that did the negotiation. Why are they outsourcing this? Isn’t that the whole purpose of why they exist?” Yeah, so FTC has sort of a broader investigation into PBMs, so this is kind of the next step in it to kind of figure out, OK, what is the role of these companies? How are they potentially creating bad incentives, contributing to increased drug pricing, making it harder for people to perhaps, like, get their drug at particular pharmacies or more expensive at particular pharmacies? Again, because there’s been a lot of integration of ownership of these companies. So like the PBMs, the health insurance, some of these pharmacy systems are sort of all connected, and there’s a lot of concern that that’s led to incentives that are harming consumers and the prices we’re paying for our health care.
Rovner: Yeah, there’s all that money sloshing around that doesn’t seem to be getting either to the drug companies or to the consumers. Rachel, you wanted to add something?
Cohrs: Sure. I think GPOs are more used with hospitals when they buy drugs, because I think PBMs — you think of, like, going to pick up your drug at the pharmacy counter. But obviously hospitals are buying so many drugs, too. And their, you know, market power is pretty dispersed across the country. And so they also are a big customer of GPOs. So I think they’re also trying to get at this, like, different part of the drug market where, you know, a lot of these really expensive medications are administered in hospitals. So it will be interesting. They’re certainly not very transparent either. So, yeah, interesting development as to how they relate to PBMs, but also the rest of — you know, encompassing a larger part of the health care system.
Karlin-Smith: Yeah, I have seen complaints from hospital systems that the GPOs require them to enter into contracts that make it very difficult for the hospital to pivot if, say, the GPO can’t supply them with a particular product or maybe it’s … [unintelligible] … and then they end up stuck in a situation where they should, in theory, be able to get a product from another supplier and they can’t. So there’s lots of different levels of, again, concern about potential bad behavior.
Rovner: Well, while we are on the topic of nerdy practice-of-medicine stuff, Rachel, you had a story on the latest on the, quote, “site-neutral” Medicare payment policy. Remind us what that is and who’s on which side, and wasn’t that one of the bills — or I guess that wasn’t one of the bills that was approved by the House Energy and Commerce Committee yesterday, right?
Cohrs: No, so “site neutral” is basically hospitals’ worst nightmare. It essentially makes sure that Medicare is paying the same amount for a service that a doctor provides, whether it’s on a hospital campus or provided in a doctor’s office. And I think hospitals argue that they need to charge more because they have to be open 24/7. You know, they don’t have predictable hours. They have to serve anyone, you know, regardless of willingness to pay. It costs more overhead. That kind of thing. But I think lawmakers are kind of losing patience with that argument to some degree, that the government should be paying more for the same service at one location versus another. And it’s true that House Republicans had really wanted an aggressive form of this policy, and it could save like tens of billions of dollars. I mean, this is a really big offset we’re talking about here, if they go really aggressively toward this path, but instead they weren’t able to get Democrats on board with that plan yet. I think the chair, Cathy McMorris Rodgers, and the ranking member, Frank Pallone, have said they want to keep working on this. But what they did do this week is took a tiny little part out of that and advanced it through the committee. And it would equalize payment for, like, drug administration in physician’s offices versus a physician doing it in the hospital, and the savings to the federal government on that policy was roughly $3 billion. So, again, not a huge hit to industry, but it’s, you know, significant savings, certainly, and a first step in this direction as they think about how they want to do this, if they want to go bigger.
Rovner: So while we’re talking about the Energy and Commerce Committee, those members, in a fairly bipartisan fashion, are moving a bunch of other bills aimed at price transparency, value-based care, and a lot of other popular health buzzwords. Sarah, I know you watched, if not all, then most of yesterday’s markup. Anything in particular that we should be watching as it perhaps moves through the House and maybe the Senate?
Karlin-Smith: Yeah. So there was — probably the most contentious health bill that cleared yesterday was a provision that basically would codify a Trump-era rule in Medicaid that the Biden administration has sort of tweaked a bit but generally supported that basically tweaks Medicaid’s “best price” rule. So Medicaid is kind of guaranteed the best price that the private sector gets for drugs. But drugmakers have argued this prevents them from doing these unique value-based arrangements where we say, “OK, if the patient doesn’t perform well or the drug doesn’t work well for the patient, we’ll kind of give you maybe even all your money back.” Well, they don’t want the Medicaid best price to be zero. So they came up with a kind of a very confusing way to tweak that and also as part of that to, you know, hopefully allow Medicaid to maybe even take advantage of these programs. And Rep. [Brett] Guthrie [(R-Ky.)], Rep. [Anna] Eshoo [(D-Calif.)] on the Democratic side, want to codify that. But a number of the Democrats pushed back and over worries this might actually raise prices Medicaid pays for drugs and be a bit more problematic. And the argument from the Democrats, the majority of Democrats on the committee who oppose it, were not completely against this idea but let it play out in rulemaking, because if it stays in rulemaking, it’s a lot easier to —er, sorry — as a rule, it’s already made.
Rovner: To fix it if they need to.
Karlin-Smith: Right. It’s a lot easier to fix it, which, as anybody who follows health policy knows, it’s not actually as easy as you would think to fix a rule, but it’s definitely a lot easier to fix a rule than it is to fix something codified in law. So that’s sort of a very wonky but meaningful thing, I think, to how much drugs cost in Medicaid.
Rovner: Last nerdy thing, I promise, for this week: The Biden administration says it plans to conduct an annual audit of the cost of the most expensive drugs covered by Medicaid and make those prices public in what one of your colleagues, Alice, described as a “name and shame” operation? I mean, could this actually work, or could it end up like other HHS [Department of Health and Human Services] transparency rules, either not very followed or tied up in court?
Karlin-Smith: Experts that my colleague Cathy Kelly talked to to write about this basically were not particularly optimistic it would lead to big changes in savings to Medicaid, basically. One of the reasons is because Medicaid actually gets pretty good deals on drugs to begin with. But that said, even, again, like I said, they’re guaranteed these really large rebates are the best price. But in exchange for that, they have to cover all drugs. So that’s where you start to lose some of your leverage. So the hope with some of this extra transparency is they’ll get more information to have, like, a little bit of additional leverage to say, “Oh, well your manufacturing costs are only this, so you should be able to give us an additional rebate,” which they can negotiate that. Again, I think people think there’ll be sort of maybe some moderate, if any, benefits to that. But some states have actually tried similar things in kind of similar “name, shame” affordability boards. And the drugmakers have basically just said, “No, we’re not going to give you any more discounts.” And they’re kind of stuck.
Rovner: “And we’re not ashamed of the price that we’re charging.”
Karlin-Smith: Right.
Rovner: “Or we wouldn’t be charging it.”
Karlin-Smith: So it’s a tough one, but there’s, like, an argument to be made that drugmakers just don’t want to be on this list. So maybe some of them will more proactively figure out like how to get their price point and everything discounts to a point where they at least won’t get on the list. So maybe, again, it might tweak things around the edges, but it’s not a big price savings move.
Rovner: And we shall see. All right. Well, this is — finally this week, it’s something I’ve wanted to talk about for a couple of weeks. I’m calling it the “How do you solve a problem like RFK Jr.?” For those of you who don’t already know, the son of the former senator and liberal icon Robert Kennedy has declared his candidacy for president. He’s an environmental lawyer, but at the same time, he’s one of the most noted anti-vaxxers, not just in the country but in the world. Vice has a provocative story — this actually goes back a couple of weeks — about how the media should cover this candidacy or, more specifically, how it shouldn’t. According to the story, ABC did an interview with RFK Jr. and then simply cut out what they deemed the false vaccine claims that he made. CNN, on the other hand, did an interview and simply didn’t mention his anti-vaccine activism. I am honestly torn here about how should you cover someone running for president who traffics in conspiracy theories that you know are not true? I realize here I am now speaking of a wider — wider universe than just RFK Jr. But as a journalist, I mean, how do you handle things that — when they get repeated and you know them to be untrue, at least in the health care realm?
Karlin-Smith: I mean, I really like the thing that Vice mentioned, and I think maybe Jay Rosen, who’s a journalism professor at NYU [New York University], he might be the person that sort of coined this, I’m not sure — this, like, “truth sandwich” idea, where you make sure you sort of start with what is true, in the middle you put the sort of — this is what the false claim of X person — and then you go back to the truth. Because I think that really helps people grasp onto what’s true, versus a lot of times you see the coverage starts with the lie or the falsehood. And I think sometimes people might even just see that headline or just see the little bit of what’s correct and never make it to the truth. And I understand some of the decisions by the news outlets that decided not to air these segments and just didn’t want to deal with the topic. But then I guess I thought they did make a good point that then you let somebody like Kennedy say, “Oh, they’re suppressing me, they’re deliberately hiding this information.” So the Vice argument was that this truth sandwich idea kind of gets you in a better … [unintelligible]. And again, as journalists, our job is not to suppress what politicians are saying. People should know what these people claim, because that is what the positions they stand for. But it’s figuring out how to add the context and be able to, you know, in real time if you need to, fact-check it.
Rovner: I confess, over the years I have been guilty of the CNN thing of just not bringing it up and hoping it doesn’t come up. But then, I mean, it’s true, the worst-case scenario — probably not going to happen with somebody running for president — but I think we’ve discovered all these people running for lower offices, that they get elected, you don’t talk about the controversial things and then you discover that you have a legislator in office who literally believes that the Earth is flat. There are — can Google that. So if these things aren’t aired, then there’s no way for voters to know. Anybody else have a personal or organizational rule for how to handle this sort of stuff?
Ollstein: I think there can be smart decisions about when to let someone say in their own voice what they believe versus saying as the news organization, “In the speech, he spent X minutes advancing the discredited assertion of blah, blah, blah, blah, blah,” and not just handing over the platform for them to share the misinformation.
Rovner: Yeah, I just want the audience to know that we do think seriously about this stuff. We are not just as sort of blithe as some may believe. All right. Well, that is this week’s news. Now, we will play my interview with Aneri Pattani, and then we will come back with our extra credits. I am pleased to welcome back to the podcast my colleague Aneri Pattani, who is here to talk about her investigation into where those billions of dollars states are getting in pharmaceutical industry settlements for the opioid crisis are actually going. Aneri, I am so glad to have you back.
Aneri Pattani: Thanks so much for having me.
Rovner: So let’s start at the beginning. How much money are we talking about? Where’s it coming from, and where is it supposed to be going?
Pattani: So the money comes from companies that made, distributed, or sold opioid painkillers. So these are places like Purdue Pharma, AmerisourceBergen, Walgreens, and a bunch of others. They were all accused of aggressively marketing the pills and falsely claiming that they weren’t addictive. So thousands of states and cities sued those companies. And rather than go through with all the lawsuits, most of the companies settled. And as a result, they’ve agreed to pay out more than $50 billion over the next 15 or so years. And the money is meant to be used on opioid remediation, which is a term that means basically anything that addresses or fixes the current addiction crisis and helps to prevent future ones.
Rovner: So the fact is that many or most states — we don’t actually know where this money is going or will go in the future because that information isn’t being made public. How is that even legal, or, I guess it’s not public funds, but it’s funds that are being obtained by public entities, i.e., the attorneys general.
Pattani: Yeah, a lot of people feel this way. But the thing is, the national settlement agreements have very few requirements for states to publicly report how they use the money. In fact, the only thing that’s in there that they’re required to report is when they use money for non-opioid purposes. And that can be at most 15% of the total funds they’re getting. And that reporting, too, is on an honor system. So if a state doesn’t report anything, then the settlement administrators are supposed to assume that the state used all of its money on things related to the opioid crisis. Now, states and localities can enact stricter requirements. For example, North Carolina and Colorado are two places that have created these public dashboards that are supposed to show where the money goes, how much each county gets, how the county spends it. But honestly, the vast majority of states are not taking steps like that.
Rovner: So for people of a certain age, this all feels kind of familiar. In the late 1990s, a group of state attorneys general banded together and sued the tobacco companies for the harm their products had done to the public. They eventually reached a settlement that sent more than $200 billion to states over 25 years, so that money is only just now running out. But it didn’t all get used for tobacco cessation or even public health, did it?
Pattani: No. In fact, most of it didn’t get used for that. The Campaign for Tobacco-Free Kids, which has been tracking that tobacco settlement money for years, found that about only 3% of the money goes to anti-smoking programs a year. The rest of it has gone towards plugging state budget gaps, infrastructure projects like paving roads, or, in the case of North Carolina and South Carolina, the money even went to subsidizing tobacco farmers.
Rovner: Great. Given the lessons of the tobacco settlement, how do the attorneys general in this case try to make sure that wasn’t going to happen? I mean, was it just by requiring that that non-opioid-related money be made public?
Pattani: So they have added some specific language to the settlements that they point to as trying to avoid, you know, the, quote, “tobacco nightmare.” Essentially, the opioid settlements say that at least 85% of the money must be spent on opioid remediation. Again, that term — that’s like things that stop and prevent addiction. And there’s also a list included at the end of the settlement, called Exhibit E, with potential expenses that fall under opioid remediation. That’s things like paying for addiction treatment for people who don’t have insurance or building recovery housing or funding prevention programs in schools. But the thing is, that list is pretty broad and it’s nonexhaustive, so governments can choose to do things that aren’t on that list, too. So there are guidelines, but there’s not a lot of hard enforcement to make sure that the money is spent on these uses.
Rovner: So, as you’ve pointed out in your reporting, it’s not always simple to determine what is an appropriate or an inappropriate use of these settlement funds, particularly in places that have been so hard-hit by the opioid crisis and that it affects the entire economy of that state or county or city. So tell us what you found in Greene County, Tennessee. That was a good example, right?
Pattani: Yeah, Greene County is an interesting place. And what I learned is happening there is actually, you know, repeating in a lot of places across the country. So Greene County, it’s an Appalachian county, it’s been hard-hit. It has a higher rate of overdose deaths than the state of Tennessee overall or even the country. But when the county got several million dollars in opioid settlement funds, it first put that money towards paying off the county’s debt. And that included putting some money into their capital projects fund, which was then used to buy a pickup truck for the sheriff’s office. So a lot of folks are looking at that, saying, “That’s not really opioid-related.” But county officials said to me, you know, this use of the money makes sense, because the opioid epidemic has hurt their economy for decades; it’s taken people out of the workforce, it’s led to increased costs for their sheriff’s office and their jail with people committing addiction-related crimes, it’s hurt the tax base when people move out of the county. So now they need that money to pay themselves back. Of course, on the other hand, you have advocates and people affected by the crisis saying, “If we’re using all the money now to pay back old debts, then who’s addressing the current crisis? People are still dying of overdoses, and we need to be putting the opioid settlement money towards the current problem.”
Rovner: So I suppose ideally they could be doing both.
Pattani: I think that’s the hard thing. Although $54 billion sounds like a lot of money, it’s coming over a long period of time. And so at the end of the day, it’s not enough to fund every single thing people want, and there is a need for prioritization.
Rovner: So I know part of your project is helping urge local reporters to look into where money is being used in their communities. How is that going?
Pattani: It’s going well. I think it’s important because the money is not only going to state governments, but to counties and cities too. So local reporters can play a really big role in tracking that money and holding local officials accountable for how they use it. So I’m trying to help by sharing some of the national data sets we’re pulling together that can be used by local reporters. And I’ve also hopped on the phone with local reporters to talk about where they can go to talk to folks about this or finding story ideas. Some of the reporters I’ve spoken with have already published stories. There was one just a week ago in the Worcester Telegram from a student journalist, actually, in that area —
Rovner: Cool.
Pattani: — so there’s a lot of good coverage coming.
Rovner: I’m curious: What got you interested in pursuing this topic? I know you cover addiction, but this is the kind of reporting that can get really frustrating.
Pattani: It definitely can. But I think it’s what you said: As someone who’s been covering addiction and mental health issues for a while, kind of focusing on some of the problems and the systemic gaps, when I learned that this money was coming in, it was exciting to me too, like, maybe this money will be used to address the issues that I’m often reporting on, and so I want to follow that and I want to see if it delivers on that promise.
Rovner: So what else is coming up in this project? I assume it’s going to continue for a while.
Pattani: Yes. So this will be a yearlong project, maybe even more, because, as I said, the funds are coming for a long time. But essentially the next few things I’m looking at, I have a big data project looking at who sits on opioid settlement councils. These are groups that advise or direct the money in different states and, you know, may represent different interests. And then we’re going to be looking at some common themes in the ways different states are using this money. So a lot of them are putting it towards law enforcement agencies, a lot of them are putting them toward in-school prevention programs, and taking a look at what the research tells us about how effective these strategies are or aren’t.
Rovner: Well, Aneri Pattani, thank you so much, and we will post links to some of Aneri’s work on the podcast homepage at kffhealthnews.org and in this week’s show notes. Thanks again.
Pattani: Thank you so much.
Rovner: OK, we’re back and it’s time for our extra credit segment. That’s when we each recommend a story we read this week we think you should read too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Sarah, why don’t you go first this week?
Karlin-Smith: Sure. I looked at a piece in The New York Times called “Heat Wave and Blackout Would Send Half of Phoenix to E.R., Study Says,” by Michael Levenson. And it’s just really sort of a horrifying piece where researchers were sort of able to model the impact of the growing frequency of heat waves due to climate change, and obviously, the U.S. had some electric grid stability issues, and just the disconnect between the amount of hospital beds and people that would be able to care for people in a very hot city due to, you know, heat waves without being able to access air conditioning and other cooling methods. And the amount of people that would be hospitalized or die or just wouldn’t have a hospital bed. The one thing I did think was sort of positive is the piece does have some suggestions, and some of them are fairly simple that could really change the degrees in cities in relevant ways, like planting more trees in particular areas, and often this affects sort of — the poorest areas of cities tend to be the ones with less trees — or, you know, changing colors or the material on roofing. So as much as sometimes I think climate change becomes sort of such an overwhelming topic where you feel like you can’t solve it, I think the one nice thing here is it does sort of show, like, we have power to make the situation better.
Rovner: We can perhaps adapt. Alice.
Ollstein: I picked a upsetting piece but really good investigation from Reuters by Michael Berens. It’s called “How Doctors Buy Their Way out of Trouble.” It’s about doctors who are charged federally with all kinds of wrongdoing, including operating on patients who don’t need to be operated on for profit and having a pattern of doing so. And it’s about how often these cases settle with federal prosecutors and the settlement allows them to keep practicing, and the settlement money goes to the government, not to the victims. And often the victims aren’t even aware that the settlement took place at all. And new patients are not aware that the doctor they may be going to has been charged. And so it’s a really messed up system and I hope this shines a light on it.
Rovner: Rachel.
Cohrs: All right. So mine is from ProPublica, and the headline is, “In the ‘Wild West’ of Outpatient Vascular Care, Doctors Can Reap Huge Payments as Patients Risk Life and Limb,” by Annie Waldman. And I think I found this story timed really well kind of as lawmakers do start to talk a little bit more about incentives for patients to be seen in a hospital versus in more physician offices. And certainly there are cost reasons that that makes sense for some procedures. But I think this story does a really good job of kind of following one doctor, who I think, similar to kind of the story Alice was talking about, you know, was taking advantage of these inflated payments that were supposed to incentivize outpatient treatment to perform way more of these procedures than patients needed. And so I think it’s just important, a cautionary tale about the safeguards that could be necessary, you know, if more of this care is provided elsewhere.
Rovner: Yeah, I think these two stories are very good to be read together. My story this week is from our fellow podcast panelist Joanne Kenen for KFF Health News. It’s called “Remote Work: An Underestimated Benefit for Family Caregivers,” and it’s about how the U.S., still one of the few countries without any formal program for long-term care, that most of us will need at some point, has accidentally fallen into a way to make family caregiving just a little bit easier by letting caregivers do their regular jobs from home, either all the time or sometimes. While many, if not most, employers have policies around childbirth and child care, relatively few have benefits that make it easier for workers to care for other sick family members, even though a fifth of all U.S. workers are family caregivers. More flexible schedules can at least make that a little easier and possibly prevent workers from quitting so that they can provide care that’s needed. It’s no substitute for an actual national policy on long-term care, but it’s a start, even if an accidental one. OK, that is our show for this week. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us, too. Special thanks, as always, to our ever-patient producer, Francis Ying. And next week is our 300th episode. If all goes as planned, we’ll have something special, so be sure to tune in. As always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can tweet me. I’m still there. I’m @jrovner. Sarah?
Karlin-Smith: I’m @SarahKarlin.
Rovner: Alice.
Ollstein: @AliceOllstein.
Rovner: Rachel.
Cohrs: @rachelcohrs.
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ ‘What the Health? on Spotify, Apple Podcasts, Stitcher, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 5 months ago
Elections, Health Care Costs, Medicare, Multimedia, Pharmaceuticals, Public Health, States, Abortion, Drug Costs, KFF Health News' 'What The Health?', Opioids, Podcasts, Prescription Drugs, South Carolina, U.S. Congress, vaccines, Women's Health
This Panel Will Decide Whose Medicine to Make Affordable. Its Choice Will Be Tricky.
Catherine Reitzel’s multiple sclerosis medication costs nearly $100,000 a year. Kris Garcia relies on a drug for a blood-clotting disorder that runs $10,000 for a three-day supply. And Mariana Marquez-Farmer would likely die within days without her monthly $300 vial of insulin.
At best, a Colorado panel of medical and pharmacy experts seeking to cut the costs of expensive drugs will be able to help only one of them.
Starting this summer, the state’s Prescription Drug Affordability Board will choose up to 18 high-cost drugs for review over the next three years to determine if the medications are unaffordable and whether to cap what health plans and consumers pay for them.
But with hundreds of expensive drugs to choose from, the board members face tough decisions about who will get help now and who will have to wait.
Do they tackle drugs with extremely high costs taken by only a handful of patients, or drugs with merely very high costs taken by a larger group? Should they consider only out-of-pocket costs paid by consumers, such as for insulin, whose copays Colorado caps at $50 a month, or the total cost of the drug to the health system? Will they weigh only drug prices, or will they try to right social wrongs with their choices?
And what does “affordable” even mean?
“That question alone is a lot harder to answer than it might seem at face value,” said Jennifer Reck, project director for the National Academy for State Health Policy’s Center for State Prescription Drug Pricing. “You immediately get into how utterly complex our drug supply chain is, how opaque it is, how many different prices there are,” she said.
Maryland was the first state to establish a drug affordability board in 2019, but funding challenges and the pandemic have slowed its progress. Colorado passed a bill creating its board in 2021 and has already moved ahead of Maryland in the process. Washington followed in 2022 but is still in its early phases of implementation.
Maine, New Hampshire, Ohio, and Oregon have also established boards, but they lack the power to limit drug payments. And at the federal level, the Inflation Reduction Act of 2022 included a provision requiring the Health and Human Services secretary to negotiate prices with drug companies for a small number of the most costly medications covered by Medicare.
It’s taken years for the Colorado and Maryland board members to create all the rules and regulations to govern their work before getting to the point of looking at specific drugs.
“It’s just a long, tortuous government process to get things up and running,” said Gerard Anderson, a professor of health policy and management at Johns Hopkins University, and a member of Maryland’s board. “You basically have to dot every ‘i’ and cross every ‘t’ in order not to get sued.”
Setting Priorities
On May 12, Colorado released its first list of hundreds of drugs eligible for review, mostly because they each cost more than $30,000 for a course of treatment. Next month, they’ll release a dashboard ranking those drugs according to the board’s priorities. The dashboard can also be used to examine which drugs have the highest price tags, which have had the largest increases in price, and which the state spends the most on. That would allow the board to begin affordability reviews this summer and set payment limits for the first four to eight drugs sometime in 2024. But board members will first have to set their priorities, and those could change from year to year.
“Maybe one year we focus on the impact to the system, and another year we focus on out-of-pocket costs, and one year we focus on a lifesaving drug that has smaller utilization,” said Lila Cummings, director of the Colorado board.
Such approaches could pit one group of patients against others looking for cost relief. But Cummings said not all groups are eager to see payment limits.
“Some of them said, ‘We want the board to focus on our drugs,’ and others said, ‘Please leave us alone,’” she said.
That reluctance likely reflects the close ties that some patient groups have with the manufacturers of their medications, including receiving funding from the drugmakers.
“We have seen cases in public hearings — it seems counterintuitive or surprising — where a patient group, instead of being thrilled that they might have access to the drugs at a lower price, instead are arguing against upper payment limits,” Reck said. “But in most cases, there’s a pretty clear financial connection to drug manufacturers.”
Maryland has also received input from patient groups as it finalizes its regulations.
“So far it has not been, ‘Pick me! Pick me! Pick me!’” Anderson said. But that could change once the Maryland board begins its affordability reviews this fall.
The drug that Garcia, 47, of Denver, takes did not make the board’s list. Diagnosed with four bleeding disorders, including von Willebrand disease, he needs the medication Humate-P, made by CSL Behring, to replace one of the clotting factors missing in his blood. This winter, driving home from his job at the airport, Garcia hit a patch of black ice, spun out, and careened into a concrete barrier at 75 mph. He needed the expensive medication every day for the first five days after the accident, and then every other day for a full month.
“It’s not like I can just sit there and say no to this medication, because my bleeds get so bad,” he said.
According to Perry Jowsey, executive director of the National Hemophilia Foundation’s Colorado chapter, about 300 to 400 individuals are being treated for von Willebrand disease in Colorado. That’s far fewer than the roughly 10,000 Coloradans with MS or the 74,000 who manage their diabetes with insulin.
“In my shoes, I would target what would help the most people,” Garcia said. “You have to find a balance, especially starting out. You’re not going to be able to help everyone.”
The Colorado and Maryland boards will rely on data from state databases that show how much various public and private health plans pay for drugs. That data, however, doesn’t capture what uninsured patients pay, and it doesn’t give any insight into how much manufacturers pay for research and development.
“The goal is not to stifle innovation,” Anderson said. “But we can’t get any public data, so we have to ask the pharmaceutical industry, and they’re not required to give us the data.”
The boards want to ensure that patients like Reitzel still have access to new and better therapies. Reitzel, 38, of Highlands Ranch, was diagnosed with multiple sclerosis in 2008 and has switched medications several times seeking one whose side effects she could tolerate. “They’re all terrible in their own special way,” she said.
In 2021, she began taking a relatively new drug from Biogen and Alkermes called Vumerity, which was included on Colorado’s list of eligible drugs. But the cost of a three-month supply was nearly $24,000, including a copay of more than $7,000. Biogen provides up to $20,000 in annual copay assistance through a debit card she can use at the pharmacy. But now her health plan no longer credits those payments toward her deductible. It makes it almost impossible for her to meet the $25,000 out-of-pocket maximum under her plan.
“Primarily for this reason, I am no longer taking any medication,” Reitzel said, “and have to only hope my disease does not progress.”
Colorado legislators passed a bill to require health plans to count copay assistance programs toward patients’ deductibles for drugs with no generic equivalents, but that provision does not take effect until 2025.
Insulin as an Outlier?
Just a couple of years ago, insulin may have been a higher priority for drug affordability boards, but now it’s not so clear. Both Colorado and Maryland have established insulin copay caps that provide pocketbook relief, at least for patients with coverage. And manufacturers are making their own moves to lower insulin prices. That could prompt the boards to bypass insulin and concentrate their limited resources on other high-cost drugs.
Copay caps do not lower the actual cost of insulin but instead spread it among members of the health plan through higher premiums. The Colorado copay caps don’t help new state residents and initially did not help those without insurance, either. Both of those hurdles would have applied to Marquez-Farmer when she moved from California to Colorado Springs a couple of years ago.
“I got married to my husband during covid because I didn’t have insurance,” she said. “I loved him, and it all worked out, but a big reason for me to marry him was because I would not be able to afford insulin.”
Marquez-Farmer, 34, said that while insulin may not be the most expensive drug on the market, many Coloradans, particularly those from marginalized communities who have higher rates of diabetes, struggle to afford it.
“I’m not saying the other medicines are not important, because obviously they are,” she said. “The reality is there’s more people who are being affected by not being able to afford their insulin and a lot of people who are dying because of them rationing insulin.”
Andrew York, executive director of the Maryland board, said the payment limits should be viewed as a last resort, a tool that can be used when other cost-control measures haven’t worked.
“The goal is for folks to never be able to say that they can’t afford their insulin. And I think we may get there soon enough just because of how much is happening in that space,” he said. “So if that’s the case, then maybe boards don’t need to use the upper payment limit tool.”
At least one form of insulin was included on Colorado’s list of drugs eligible for review, but not the most commonly taken brand-name insulins. That precludes the Colorado board from addressing insulin costs more broadly.
The pharmaceutical industry has pushed back against the concept of payment limits, warning that drugmakers could pull out of states that set payment limits.
“The boards are acutely aware of this discussion point. The interest and the purpose of these boards is to increase access to the drugs, not decrease it,” York said. “But there’s kind of this game theory element of: How will manufacturers react?”
Reck discounted the notion that a payment limit would prompt a manufacturer to abandon a profitable market.
“Unfortunately, it’s kind of a scary message and it can be impactful on patients,” she said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 5 months ago
Health Care Costs, Pharmaceuticals, States, Colorado, Drug Costs, Maine, Maryland, New Hampshire, Ohio, Oregon, Prescription Drugs, Washington
A More Aggressive FTC Is Starting to Target Drug Mergers and Industry Middlemen
Under the leadership of an aggressive opponent of anti-competitive business practices, the Federal Trade Commission is moving against drug companies and industry middlemen as part of the Biden administration’s push for lower drug prices at the pharmacy counter.
On May 16, the FTC sued to block the merger of drugmakers Amgen and Horizon Therapeutics, saying the tangled web of drug industry deal-making would enable Amgen to leverage the monopoly power of two top Horizon drugs that have no rivals.
In its lawsuit, the FTC said that if it allowed Amgen’s $27.8 billion purchase to go through, Amgen could pressure the companies that manage access to prescription drugs — pharmacy benefit managers, or PBMs — to boost the two extremely expensive Horizon products in a way that would inhibit any competition.
The suit, the first time since 2009 that the FTC has tried to block a drug company merger, reflects Chair Lina Khan’s strong interest in antitrust action. In announcing the suit, the agency said that by fighting monopoly powers it aimed to tame prices and improve patients’ access to cheaper products.
The FTC’s action is a “shot across the bow for the pharmaceutical industry,” said Robin Feldman, a professor and drug industry expert at the University of California College of the Law-San Francisco. David Balto, a former FTC official and attorney who fought the 2019 Bristol-Myers Squibb-Celgene and 2020 AbbVie-Allergan mergers, said FTC’s action was long overdue.
The Horizon-Amgen merger would “cost consumers in higher prices, less choice, and innovation,” he said. “The merger would have given Amgen even more tools to exploit consumers and harm competition.”
The FTC also announced an expansion of a yearlong investigation of the PBMs, saying it was looking at two giant drug-purchasing companies, Ascent Health Services and Zinc Health Services. Critics claim the PBMs set up these companies to conceal profits.
When Amgen announced its purchase of Horizon in December — the biggest biopharma transaction in 2022 — it showed particular interest in Horizon’s drugs for thyroid eye disease (Tepezza) and severe gout (Krystexxa), for which the company was charging up to $350,000 and $650,000, respectively, for a year of treatment. The complaint said the merger would disadvantage biotech rivals that have similar products in advanced clinical testing.
Amgen could promote the Horizon drugs through “cross-market bundling,” the FTC said. That means requiring PBMs to promote some of Amgen’s less popular drugs — the Horizon products, in this case — in exchange for Amgen offering the PBMs large rebates for its blockbusters. Amgen has nine drugs that each earned more than $1 billion last year, according to the complaint, the most popular being Enbrel, which treats rheumatoid arthritis and other diseases.
The three biggest PBMs negotiate prices and access to 80% of prescription drugs in the U.S., giving them enormous bargaining power. Their ability to influence which drugs Americans can get, and at what price, enables the PBMs to obtain billions in rebates from drug manufacturers.
“The prospect that Amgen could leverage its portfolio of blockbuster drugs to gain advantages over potential rivals is not hypothetical,” the FTC complaint states. “Amgen has deployed this very strategy to extract favorable terms from payers to protect sales of Amgen’s struggling drugs.”
The complaint noted that biotech Regeneron last year sued Amgen, alleging that the latter’s rebating strategy harmed Regeneron’s ability to sell its competing cholesterol drug, Praluent. Amgen’s Repatha generated $1.3 billion in global revenue in 2022.
It “may be effectively impossible” for smaller rivals to “match the value of bundled rebates that Amgen would be able to offer” as it leverages placement of the Horizon drugs on health plan formularies, the complaint states.
Business analysts were skeptical that the FTC action would succeed. Until now the commission and the Department of Justice have shied away from challenging pharmaceutical mergers, a precedent that will be hard to overcome.
Research on the impact of mergers has shown that they often benefit shareholders by increasing stock prices, but hurt innovation in drug development by trimming research projects and staffing.
Waves of consolidation shrank the field of leading pharma companies from 60 to 10 from 1995 to 2015. Most of the mergers in recent years have involved “big fish buying up lots of little fish,” such as biotech companies with promising drugs, Feldman said.
The giant Amgen-Horizon merger is an obvious exception, and therefore a good opportunity for the FTC to demonstrate a “theory of harm” around drug industry bundling maneuvers with PBMs, said Aaron Glick, a mergers analyst with Cowen & Co.
But that doesn’t mean the FTC will win.
Amgen may or may not engage in anti-competitive practices, but “a separate question is, how does this lawsuit fit under current antitrust laws and precedent?” Glick said. “The way the law is set up today, it seems unlikely it will hold up in court.”
The FTC’s argument about Amgen’s behavior with Horizon products is hypothetical. The pending Regeneron suit against Amgen, as well as other, successful lawsuits, suggests that rules are in place to suppress this kind of anti-competitive behavior when it occurs, Glick said.
The judge presiding over the case in U.S. District Court in Illinois is John Kness, who was appointed by then-President Donald Trump and is a former member of the Federalist Society, whose membership tends to be skeptical of antitrust efforts. The case is likely to be settled by Dec. 12, the deadline for the merger to go through under current terms.
Amgen sought to undercut the government’s case by agreeing not to bundle Horizon products in future negotiations with pharmacy benefit managers. That promise, while hard to enforce, might get a sympathetic hearing in court, Glick said.
Still, even a loss would enable the FTC to shed light on a problem in the industry and what it sees as a deficiency in antitrust laws that it wants Congress to correct, he said.
The day after suing to stop the merger, the FTC announced it was pushing further into an investigation of pharmacy benefit managers that it began last June. The agency demanded information from Ascent and Zinc, the two so-called rebate aggregators — drug purchasing organizations set up by PBMs Express Scripts and CVS Caremark.
At a May 10 hearing, Eli Lilly & Co. CEO Dave Ricks said that most of the $8 billion in rebate checks his company paid last year went to rebate aggregators, rather than to the PBMs directly. A “big chunk” of the $8 billion went overseas, he said. Ascent is based in Switzerland, while Emisar Pharma Services, an aggregator established by PBM OptumRx, is headquartered in Ireland. Zinc Health Services is registered in the U.S.
Critics say the aggregators enable PBMs to obscure the size and destination of rebates and other fees they charge as intermediaries in the drug business.
The PBMs say their efforts reduce prices at the pharmaceutical counter. Testimony in Congress and in FTC hearings over the past year indicate that, at least in some instances, they actually increase them.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 5 months ago
Courts, Health Industry, Pharmaceuticals, Drug Costs, Prescription Drugs
Una FTC más agresiva persigue las fusiones en la industria farmacéutica y a los intermediarios del sector
Bajo la dirección de una agresiva opositora al comportamiento empresarial que menoscaba la competencia, la Comisión Federal de Comercio (FTC) está actuando contra las empresas farmacéuticas y los intermediarios del sector, como parte de la campaña de la administración Biden para reducir los precios de los medicamentos en las farmacias.
El 16 de mayo, la FTC interpuso una demanda para bloquear la fusión de las farmacéuticas Amgen y Horizon Therapeutics, alegando que la enmarañada red de acuerdos de la industria permitiría a Amgen aprovechar el poder monopolístico de dos de los principales medicamentos de Horizon que no tienen rivales.
En su demanda, la FTC alegó que si se permitía la compra que pretende Amgen por $27,800 millones, Amgen podría presionar a las empresas que gestionan el acceso a los medicamentos con receta —los gestores de beneficios de farmacia, o PBM— para que impongan los dos productos extremadamente caros de Horizon de una manera que eliminaría cualquier competencia.
Es la primera vez desde 2009 que la FTC intenta bloquear una fusión de empresas farmacéuticas, y esta demanda refleja el gran interés de la presidenta Lina Khan por las medidas antimonopolio. Al anunciar la demanda, la agencia declaró que al luchar contra los poderes monopolísticos pretendía controlar los precios y mejorar el acceso de los pacientes a productos más baratos.
Para Robin Feldman, profesor y experto en la industria farmacéutica de la Facultad de Derecho de la Universidad de California en San Francisco, la actuación de la FTC es “un golpe frontal a la industria farmacéutica”. David Balto, ex funcionario de la FTC y abogado que luchó contra las fusiones Bristol-Myers Squibb-Celgene en 2019 y AbbVie-Allergan en 2020, dijo que la acción de la FTC era necesaria desde hace mucho tiempo.
La fusión Horizon-Amgen “costaría a los consumidores precios más altos, menos opciones e innovación”, señaló. “La fusión habría dado a Amgen aún más herramientas para explotar a los consumidores y dañar la competencia”.
La FTC también anunció la ampliación de una investigación de un año sobre los PBM, indicando que se investigaban dos gigantescas empresas de compra de medicamentos, Ascent Health Services y Zinc Health Services. Los críticos afirman que los PBM crearon estas empresas para ocultar beneficios.
Cuando Amgen anunció la compra de Horizon en diciembre —la mayor operación biofarmacéutica de 2022— mostró especial interés por los medicamentos de Horizon para la enfermedad tiroidea ocular (Tepezza) y la gota grave (Krystexxa), por los que la empresa cobraba hasta $350,000 y $650,000, respectivamente, por un año de tratamiento. Según la demanda, la fusión perjudicaría a rivales biotecnológicos que tienen productos similares en fase avanzada de pruebas clínicas.
Según la FTC, Amgen podría promocionar los fármacos de Horizon a través de la “venta cruzada”. Esto significa exigir a los PBM que promocionen algunos de los medicamentos menos populares de Amgen —los productos Horizon, en este caso— a cambio de que Amgen ofrezca a los PBM grandes descuentos por sus superventas. Según la denuncia, Amgen tiene nueve medicamentos que el año pasado generaron más de $1,000 millones cada uno. El más popular es Enbrel, que trata la artritis reumatoide y otras enfermedades.
Los tres mayores PBM negocian los precios y el acceso al 80% de los medicamentos recetados en Estados Unidos, lo que les confiere un enorme poder de negociación. Su capacidad para influir en los medicamentos a los que tienen acceso los estadounidenses, y a qué precio, les permite obtener miles de millones en descuentos de los fabricantes.
“La posibilidad de que Amgen pudiera aprovechar su cartera de medicamentos superventas para obtener ventajas sobre sus rivales potenciales no es hipotética”, afirma la denuncia de la FTC. “Amgen ha desplegado esta misma estrategia para conseguir condiciones favorables de los pagadores y proteger así las ventas de los medicamentos de Amgen en dificultades”.
La denuncia señaló que la biotecnológica Regeneron demandó el año pasado a Amgen, alegando que la estrategia de reembolso de esta última perjudicó la capacidad de Regeneron para vender su medicamento competidor contra el colesterol, Praluent. Repatha, de Amgen, generó unos ingresos mundiales de $1,300 millones en 2022.
Según la demanda, “puede resultar completamente imposible” para los rivales más pequeños “igualar el valor de los reembolsos agrupados que Amgen podría ofrecer”, ya que aprovecha la colocación de los medicamentos de Horizon en los formularios de los planes de salud.
Los analistas de la industria se mostraron escépticos sobre el éxito de la acción de la FTC. Hasta ahora, la Comisión y el Departamento de Justicia han evitado cuestionar las fusiones farmacéuticas, un precedente difícil de superar.
Las investigaciones sobre el impacto de las fusiones han demostrado que a menudo benefician a los accionistas al aumentar el precio de las acciones; pero perjudican la innovación en el desarrollo de fármacos al recortar los proyectos de investigación y el personal.
Las olas de consolidación redujeron el número de empresas farmacéuticas líderes de 60 a 10 entre 1995 y 2015. Según Feldman, la mayoría de las fusiones de los últimos años se han producido entre “peces gordos que adquieren muchos peces pequeños”, como empresas de biotecnología con fármacos prometedores.
La gigantesca fusión Amgen-Horizon es una excepción obvia y, por tanto, una buena oportunidad para que la FTC demuestre la “teoría del daño” en las maniobras de consolidación de la industria farmacéutica con los PBM, dijo Aaron Glick, analista de fusiones de Cowen & Co.
Pero eso no significa que la FTC vaya a ganar.
Amgen puede incurrir o no en prácticas anticompetitivas, pero “otra cuestión es cómo encaja esta demanda en las leyes antimonopolio y los precedentes actuales”, señaló Glick. “Tal y como está configurada la ley hoy, parece poco probable que se sostenga en los tribunales”.
El argumento de la FTC sobre el comportamiento de Amgen con los productos Horizon es hipotético. La demanda pendiente de Regeneron contra Amgen, así como otras demandas que han prosperado, sugiere que existen normas para suprimir este tipo de comportamiento anticompetitivo cuando se produce, añadió Glick.
El juez que preside el caso en el Tribunal de Distrito de Estados Unidos en Illinois es John Kness, quien fue nombrado por el entonces presidente Donald Trump y es un ex miembro de la Federalist Society, cuyos miembros tienden a ser escépticos sobre los esfuerzos antimonopolio.
Es probable que el caso se resuelva antes del 12 de diciembre, fecha límite para que la fusión se lleve a cabo en los términos actuales.
Amgen trató de socavar los argumentos del Gobierno comprometiéndose a no agrupar los productos de Horizon en futuras negociaciones con los gestores de beneficios farmacéuticos (PBM). Esta promesa, aunque difícil de hacer cumplir, podría obtener una audiencia favorable en corte, apuntó Glick.
Sin embargo, incluso una derrota permitiría a la FTC arrojar luz sobre un problema en la industria y lo que considera una deficiencia en las leyes antimonopolio que quiere que el Congreso corrija, explicó.
Al día siguiente de ir a corte para detener la fusión, la FTC anunció que profundizaba en una investigación sobre los gestores de beneficios farmacéuticos que inició el pasado mes de junio. La agencia solicitó información a Ascent y Zinc, los dos llamados agregadores de reembolsos, organizaciones de compra de medicamentos creadas por los PBM Express Scripts y CVS Caremark.
En una audiencia celebrada el 10 de mayo, el CEO de Eli Lilly & Co., Dave Ricks, afirmó que la mayor parte de los $8,000 millones en cheques de reembolso que su empresa pagó el año pasado fueron a parar a los agregadores de reembolsos, en lugar de directamente a los PBM. Una “gran parte” de los $8,000 millones fue a parar al extranjero, indicó Ricks. Ascent tiene su sede en Suiza, mientras que Emisar Pharma Services, un agregador establecido por PBM OptumRx, tiene su sede en Irlanda. Zinc Health Services está registrada en Estados Unidos.
Los críticos afirman que los agregadores permiten a los PBM ocultar la cuantía y el destino de los reembolsos y otras comisiones que cobran como intermediarios en el negocio de los medicamentos.
Por su parte, los PBM aseguran que sus esfuerzos reducen los precios en el mostrador de la farmacia. Los testimonios en el Congreso y en las audiencias de la FTC del año pasado indican que, al menos en algunos casos, en realidad los aumentan.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
2 years 5 months ago
Courts, Health Industry, Noticias En Español, Pharmaceuticals, Drug Costs, Prescription Drugs