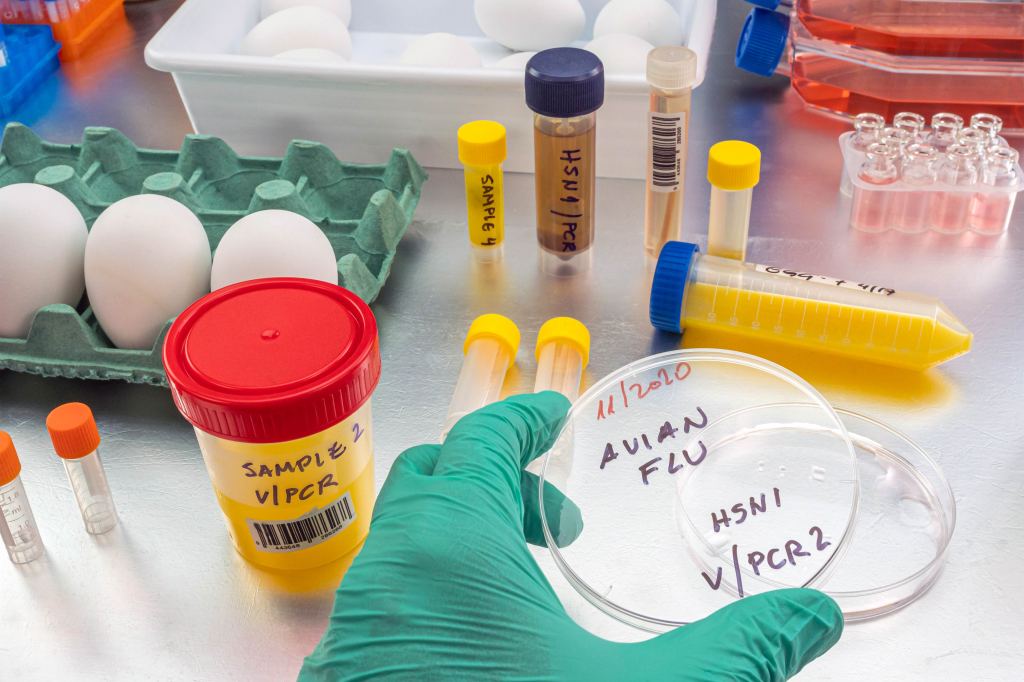
La gripe aviar es mala para las aves de corral y las vacas lecheras. No es una amenaza grave para la mayoría de nosotros… por ahora
Los titulares explotaron después que el Departamento de Agricultura confirmara que el virus de la gripe aviar H5N1 ha infectado a vacas lecheras en todo el país.
Las pruebas han detectado el virus en el ganado en nueve estados, principalmente en Texas y Nuevo México, y más recientemente en Colorado, dijo Nirav Shah, director principal adjunto de los Centros para el Control y Prevención de Enfermedades (CDC), en un evento del 1 de mayo.
Otros animales, y al menos una persona en Texas, también se infectaron con el H5N1. Pero lo que más temen los científicos es si el virus se propagara de manera eficiente de persona a persona. Eso no ha sucedido y podría no suceder. Shah dijo que los CDC consideran que el brote de H5N1 “es un riesgo bajo para el público en general en este momento”.
Los virus evolucionan y los brotes pueden cambiar rápidamente. “Como con cualquier brote importante, esto se mueve a la velocidad de un tren bala”, dijo Shah. “De lo que hablamos ahora es de un instantánea de ese tren que se mueve rápidamente”. Lo que quiere decir es que lo que hoy se sabe sobre la gripe aviar H5N1 seguramente cambiará.
Con eso en mente, KFF Health News explica lo que se necesita saber ahora.
¿Quién contrae el virus que causa la gripe aviar?
Principalmente las aves. Sin embargo, en los últimos años, el virus de la gripe aviar H5N1 ha estado saltando cada vez más de las aves a los mamíferos en todo el mundo. La creciente lista, de más de 50 especies, incluye focas, cabras, zorrinos, gatos y perros salvajes en un zoológico en el Reino Unido. Al menos 24,000 leones marinos murieron en brotes de gripe aviar H5N1 en Sudamérica el año pasado.
Lo que hace que el brote actual en el ganado sea inusual es que se está propagando rápidamente de vaca a vaca, mientras que los otros casos, excepto las infecciones de leones marinos, parecen limitados. Los investigadores saben esto porque las secuencias genéticas de los virus H5N1 extraídos de las vacas este año eran casi idénticas entre sí.
El brote de ganado también preocupa porque agarró al país desprevenido. Los investigadores que examinan los genomas del virus sugieren que originalmente se transmitió de las aves a las vacas a finales del año pasado en Texas, y desde entonces se ha propagado entre muchas más vacas de las que se han examinado.
“Nuestros análisis muestran que esto ha estado circulando en vacas durante unos cuatro meses, bajo nuestras narices”, dijo Michael Worobey, biólogo especializado en evolución de la Universidad de Arizona en Tucson.
¿Es este el comienzo de la próxima pandemia?
Aún no. Pero es algo que vale la pena considerar porque una pandemia de gripe aviar sería una pesadilla. Más de la mitad de las personas infectadas por cepas anteriores del virus de la gripe aviar H5N1 de 2003 a 2016 murieron.
Incluso si las tasas de mortalidad resultan ser menos severas para la cepa H5N1 que circula actualmente en el ganado, las repercusiones podrían implicar muchas personas enfermas y hospitales demasiado abrumados para manejar otras emergencias médicas.
Aunque al menos una persona se infectó con el H5N1 este año, el virus no puede provocar una pandemia en su estado actual.
Para alcanzar este horrible estatus, un patógeno necesita enfermar a muchas personas en varios continentes. Y para lograrlo, el virus H5N1 necesitaría infectar a toneladas de personas. Eso no sucederá a través de saltos ocasionales del virus de los animales de granja a las personas. Más bien, el virus debe adquirir mutaciones para propagarse de persona a persona, como la gripe estacional, como una infección respiratoria transmitida principalmente por el aire cuando las personas tosen, estornudan y respiran.
Como aprendimos de covid-19, los virus transmitidos por el aire son difíciles de frenar.
Eso aún no ha sucedido. Sin embargo, los virus H5N1 ahora tienen muchas oportunidades para evolucionar a medida que se replican dentro de los organismos de miles de vacas. Como todos los virus, mutan a medida que se replican, y las mutaciones que mejoran la supervivencia del virus se transmiten a la próxima generación. Y debido a que las vacas son mamíferos, los virus podrían estar mejorando en reproducirse dentro de células más cercanas a las nuestras que las de las aves.
La evolución de un virus de gripe aviar listo para una pandemia podría facilitarse por una especie de superpoder que poseen muchos virus. Es decir, a veces intercambian sus genes con otras cepas en un proceso llamado recombinación.
En un estudio publicado en 2009, Worobey y otros investigadores rastrearon el origen de la pandemia del virus de la gripe porcina H1N1 en eventos en los que diferentes virus que causaban esta gripe, la gripe aviar y la gripe humana mezclaban y combinaban sus genes dentro de cerdos que se estaban infectando simultáneamente. Los cerdos no necesitan estar involucrados esta vez, advirtió Worobey.
¿Comenzará una pandemia si una persona bebe leche contaminada con el virus?
Aún no. La leche de vaca, así como la leche en polvo y la fórmula infantil, que se venden en tiendas se consideran seguras porque la ley requiere que toda la leche vendida comercialmente sea pasteurizada. Este proceso de calentar la leche a altas temperaturas mata bacterias, virus y otros microorganismos.
Las pruebas han identificado fragmentos de virus H5N1 en la leche comercial, pero confirman que los fragmentos del virus están muertos y, por lo tanto, son inofensivos.
Sin embargo, la leche “cruda” no pasteurizada ha demostrado contener virus H5N1 vivos, por eso la Administración de Drogas y Alimentos (FDA) y otras autoridades sanitarias recomiendan firmemente a las personas que no la tomen, porque podrían enfermarse de gravedad o algo peor.
Pero, aún así, es poco probable que se desate una pandemia porque el virus, en su forma actual, no se propaga eficientemente de persona a persona, como lo hace, por ejemplo, la gripe estacional.
¿Qué se debe hacer?
¡Mucho! Debido a la falta de vigilancia, el Departamento de Agricultura (USDA) y otras agencias han permitido que la gripe aviar H5N1 se propague en el ganado, sin ser detectada. Para hacerse cargo de la situación, el USDA recientemente ordenó que se sometan a pruebas a todas las vacas lecheras en lactancia antes que los ganaderos las trasladen a otros estados, y que se informen los resultados de las pruebas.
Pero al igual que restringir las pruebas de covid a los viajeros internacionales a principios de 2020 permitió que el coronavirus se propagara sin ser detectado, testear solo a las vacas que se mueven entre estados dejaría pasar muchos casos.
Estas pruebas limitadas no revelarán cómo se está propagando el virus entre el ganado, información que los ganaderos necesitan desesperadamente para frenarlo. Una hipótesis principal es que los virus se están transfiriendo de una vaca a la siguiente a través de las máquinas utilizadas para ordeñarlas.
Para aumentar las pruebas, Fred Gingrich, director ejecutivo de la American Association of Bovine Practitioners, dijo que el gobierno debería ofrecer fondos a los ganaderos para que informen casos y así tengan un incentivo para hacer pruebas. De lo contrario, dijo, informar solo daña la reputación por encima de las pérdidas financieras.
“Estos brotes tienen un impacto económico significativo”, dijo Gingrich. “Los ganaderos pierden aproximadamente el 20% de su producción de leche en un brote porque los animales dejan de comer, producen menos leche, y parte de esa leche es anormal y no se puede vender”.
Gingrich agregó que el gobierno ha hecho gratuitas las pruebas de H5N1 para los ganaderos, pero no han presupuestado dinero para los veterinarios que deben tomar muestras de las vacas, transportar las muestras y presentar los documentos. “Las pruebas son la parte menos costosa”, explicó.
Si las pruebas en las granjas siguen siendo esquivas, los virólogos aún pueden aprender mucho analizando secuencias genómicas del virus H5N1 de muestras de ganado. Las diferencias entre las secuencias cuentan una historia sobre dónde y cuándo comenzó el brote actual, el camino que recorre y si los virus están adquiriendo mutaciones que representan una amenaza para las personas.
Sin embargo, esta investigación vital se ha visto obstaculizada porque el USDA publica los datos incompletos y con cuentagotas, dijo Worobey.
El gobierno también debería ayudar a los criadores de aves de corral a prevenir brotes de H5N1, ya que estos matan a muchas aves y representan una amenaza constante de potenciales saltos de especies, dijo Maurice Pitesky, especialista en enfermedades de aves de la Universidad de California-Davis.
Las aves acuáticas como los patos y los gansos son las fuentes habituales de brotes en granjas avícolas, y los investigadores pueden detectar su proximidad mediante el uso de sensores remotos y otras tecnologías. Eso puede significar una vigilancia rutinaria para detectar signos tempranos de infecciones en aves de corral, usar cañones de agua para ahuyentar a las bandadas migratorias, reubicar animales de granja o llevarlos temporalmente a cobertizos. “Deberíamos estar invirtiendo en prevención”, dijo Pitesky.
Bien, no es una pandemia, pero ¿qué podría pasarle a las personas que contraigan la gripe aviar H5N1 de este año?
Realmente nadie lo sabe. Solo una persona en Texas fue diagnosticada con la enfermedad este año, en abril. Esta persona trabajaba con vacas lecheras, y tuvo un caso leve con una infección en el ojo. Los CDC se enteraron de esto debido a su proceso de vigilancia. Las clínicas deben alertar a los departamentos de salud estatales cuando diagnostican a trabajadores agrícolas con gripe, utilizando pruebas que detectan virus de la influenza en general.
Los departamentos de salud estatales luego confirman la prueba y, si es positiva, envían una muestra de la persona a un laboratorio de los CDC, donde se verifica específicamente la presencia del virus H5N1. “Hasta ahora hemos recibido 23”, dijo Shah. “Todos menos uno resultaron negativos”.
Agregó que funcionarios del departamento de salud estatal también están monitoreando a alrededor de 150 personas que han pasado tiempo alrededor de ganado. Están en contacto con estos trabajadores agrícolas con llamadas telefónicas, mensajes de texto o visitas en persona para ver si desarrollan síntomas. Y si eso sucede, les harán pruebas.
Otra forma de evaluar a los trabajadores agrícolas sería testear su sangre en busca de anticuerpos contra el virus de la gripe aviar H5N1; un resultado positivo indicaría que podrían haberse infectado sin saberlo. Pero Shah dijo que los funcionarios de salud aún no están haciendo este trabajo.
“El hecho de que hayan pasado cuatro meses y aún no hayamos hecho esto no es una buena señal”, dijo Worobey. “No estoy muy preocupado por una pandemia en este momento, pero deberíamos comenzar a actuar como si no quisiéramos que sucediera”.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 5 months ago
Health Industry, Noticias En Español, Public Health, Rural Health, Colorado, FDA, Food Safety, New Mexico, texas
WHO Overturns Dogma on Airborne Disease Spread. The CDC Might Not Act on It.
The World Health Organization has issued a report that transforms how the world understands respiratory infections like covid-19, influenza, and measles.
Motivated by grave missteps in the pandemic, the WHO convened about 50 experts in virology, epidemiology, aerosol science, and bioengineering, among other specialties, who spent two years poring through the evidence on how airborne viruses and bacteria spread.
However, the WHO report stops short of prescribing actions that governments, hospitals, and the public should take in response. It remains to be seen how the Centers for Disease Control and Prevention will act on this information in its own guidance for infection control in health care settings.
The WHO concluded that airborne transmission occurs as sick people exhale pathogens that remain suspended in the air, contained in tiny particles of saliva and mucus that are inhaled by others.
While it may seem obvious, and some researchers have pushed for this acknowledgment for more than a decade, an alternative dogma persisted — which kept health authorities from saying that covid was airborne for many months into the pandemic.
Specifically, they relied on a traditional notion that respiratory viruses spread mainly through droplets spewed out of an infected person’s nose or mouth. These droplets infect others by landing directly in their mouth, nose, or eyes — or they get carried into these orifices on droplet-contaminated fingers. Although these routes of transmission still happen, particularly among young children, experts have concluded that many respiratory infections spread as people simply breathe in virus-laden air.
“This is a complete U-turn,” said Julian Tang, a clinical virologist at the University of Leicester in the United Kingdom, who advised the WHO on the report. He also helped the agency create an online tool to assess the risk of airborne transmission indoors.
Peg Seminario, an occupational health and safety specialist in Bethesda, Maryland, welcomed the shift after years of resistance from health authorities. “The dogma that droplets are a major mode of transmission is the ‘flat Earth’ position now,” she said. “Hurray! We are finally recognizing that the world is round.”
The change puts fresh emphasis on the need to improve ventilation indoors and stockpile quality face masks before the next airborne disease explodes. Far from a remote possibility, measles is on the rise this year and the H5N1 bird flu is spreading among cattle in several states. Scientists worry that as the H5N1 virus spends more time in mammals, it could evolve to more easily infect people and spread among them through the air.
Traditional beliefs on droplet transmission help explain why the WHO and the CDC focused so acutely on hand-washing and surface-cleaning at the beginning of the pandemic. Such advice overwhelmed recommendations for N95 masks that filter out most virus-laden particles suspended in the air. Employers denied many health care workers access to N95s, insisting that only those routinely working within feet of covid patients needed them. More than 3,600 health care workers died in the first year of the pandemic, many due to a lack of protection.
However, a committee advising the CDC appears poised to brush aside the updated science when it comes to its pending guidance on health care facilities.
Lisa Brosseau, an aerosol expert and a consultant at the Center for Infectious Disease Research and Policy in Minnesota, warns of a repeat of 2020 if that happens.
“The rubber hits the road when you make decisions on how to protect people,” Brosseau said. “Aerosol scientists may see this report as a big win because they think everything will now follow from the science. But that’s not how this works and there are still major barriers.”
Money is one. If a respiratory disease spreads through inhalation, it means that people can lower their risk of infection indoors through sometimes costly methods to clean the air, such as mechanical ventilation and using air purifiers, and wearing an N95 mask. The CDC has so far been reluctant to press for such measures, as it updates foundational guidelines on curbing airborne infections in hospitals, nursing homes, prisons, and other facilities that provide health care. This year, a committee advising the CDC released a draft guidance that differs significantly from the WHO report.
Whereas the WHO report doesn’t characterize airborne viruses and bacteria as traveling short distances or long, the CDC draft maintains those traditional categories. It prescribes looser-fitting surgical masks rather than N95s for pathogens that “spread predominantly over short distances.” Surgical masks block far fewer airborne virus particles than N95s, which cost roughly 10 times as much.
Researchers and health care workers have been outraged about the committee’s draft, filing letters and petitions to the CDC. They say it gets the science wrong and endangers health. “A separation between short- and long-range distance is totally artificial,” Tang said.
Airborne viruses travel much like cigarette smoke, he explained. The scent will be strongest beside a smoker, but those farther away will inhale more and more smoke if they remain in the room, especially when there’s no ventilation.
Likewise, people open windows when they burn toast so that smoke dissipates before filling the kitchen and setting off an alarm. “You think viruses stop after 3 feet and drop to the ground?” Tang said of the classical notion of distance. “That is absurd.”
The CDC’s advisory committee is comprised primarily of infection control researchers at large hospital systems, while the WHO consulted a diverse group of scientists looking at many different types of studies. For example, one analysis examined the puff clouds expelled by singers, and musicians playing clarinets, French horns, saxophones, and trumpets. Another reviewed 16 investigations into covid outbreaks at restaurants, a gym, a food processing factory, and other venues, finding that insufficient ventilation probably made them worse than they would otherwise be.
In response to the outcry, the CDC returned the draft to its committee for review, asking it to reconsider its advice. Meetings from an expanded working group have since been held privately. But the National Nurses United union obtained notes of the conversations through a public records request to the agency. The records suggest a push for more lax protection. “It may be difficult as far as compliance is concerned to not have surgical masks as an option,” said one unidentified member, according to notes from the committee’s March 14 discussion. Another warned that “supply and compliance would be difficult.”
The nurses’ union, far from echoing such concerns, wrote on its website, “The Work Group has prioritized employer costs and profits (often under the umbrella of ‘feasibility’ and ‘flexibility’) over robust protections.” Jane Thomason, the union’s lead industrial hygienist, said the meeting records suggest the CDC group is working backward, molding its definitions of airborne transmission to fit the outcome it prefers.
Tang expects resistance to the WHO report. “Infection control people who have built their careers on this will object,” he said. “It takes a long time to change people’s way of thinking.”
The CDC declined to comment on how the WHO’s shift might influence its final policies on infection control in health facilities, which might not be completed this year. Creating policies to protect people from inhaling airborne viruses is complicated by the number of factors that influence how they spread indoors, such as ventilation, temperature, and the size of the space.
Adding to the complexity, policymakers must weigh the toll of various ailments, ranging from covid to colds to tuberculosis, against the burden of protection. And tolls often depend on context, such as whether an outbreak happens in a school or a cancer ward.
“What is the level of mortality that people will accept without precautions?” Tang said. “That’s another question.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 5 months ago
COVID-19, Multimedia, Public Health, CDC, Video
Toxic Gas Adds to a Long History of Pollution in Southwest Memphis
MEMPHIS, Tenn. — For many years, Rose Sims had no idea what was going on inside a nondescript brick building on Florida Street a couple of miles from her modest one-story home on the southwestern side of town.
Like other residents, she got an unwelcome surprise in October 2022 at a public forum held by the Environmental Protection Agency at the historic Monumental Baptist Church, known for its role in the civil rights movement. The EPA notified the predominantly Black community that Sterilization Services of Tennessee —which began operations in the brick building in the 1970s — had been emitting unacceptably high levels of ethylene oxide, a toxic gas commonly used to disinfect medical devices.
Airborne emissions of the colorless gas can increase the risk of certain medical conditions, including breast cancer. Sims, who is 59 and Black, said she developed breast cancer in 2019, despite having no family history of it, and she suspects ethylene oxide was a contributing factor.
“I used to be outside a lot. I was in good health. All of a sudden, I got breast cancer,” she said.
Local advocates say the emissions are part of a pattern of environmental racism. The term is often applied when areas populated primarily by racial and ethnic minorities and members of low-socioeconomic backgrounds, like southwest Memphis, are burdened with a disproportionate amount of health hazards.
The drivers of environmental racism include the promise of tax breaks for industry to locate a facility in a heavily minority community, said Malini Ranganathan, an urban geographer at American University in Washington, D.C. The cheaper cost of land also is a factor, as is the concept of NIMBY — or “not in my backyard” — in which power brokers steer possible polluters to poorer areas of cities.
A manager at Sterilization Services’ corporate office in Richmond, Virginia, declined to answer questions from KFF Health News. An attorney with Leitner, Williams, Dooley & Napolitan, a law firm that represents the company, also declined to comment. Sterilization Services, in a legal filing asking for an ethylene oxide-related lawsuit to be dismissed, said the use of the gas, which sterilizes about half the medical devices in the U.S., is highly regulated to ensure public safety.
Besides southwest Memphis, there are nearly two dozen locales, mostly small cities — from Athens, Texas, to Groveland, Florida, and Ardmore, Oklahoma — where the EPA said in 2022 that plants sterilizing medical devices emit the gas at unusually high levels, potentially increasing a person’s risk of developing cancer.
The pollution issue is so bad in southwest Memphis that even though Sterilization Services planned to close shop by April 30, local community leaders have been hesitant to celebrate. In a letter last year to a local Congress member, the company said it has always complied with federal, state, and local regulations. The reason for its closure, it said, was a problem with renewing the building lease.
But many residents see it as just one small win in a bigger battle over environmental safety in the neighborhood.
“It’s still a cesspool of pollution,’’ said Yolonda Spinks, of the environmental advocacy organization Memphis Community Against Pollution, about a host of hazards the community faces.
The air in this part of the city has long been considered dangerous. An oil refinery spews a steady plume of white smoke. A coal plant, which is now closed, leaked components of coal ash, such as arsenic, into the ground and groundwater, according to a corrective action report from the Tennessee Valley Authority. The TVA is proposing to gut an existing gas plant and replace turbines in the facility with new ones. A continual stream of heavy trucks chug along nearby highways and roads. Other transportation sources of air pollution include the Memphis International Airport and barge traffic on the nearby Mississippi River.
Lead contamination is also a concern, not just in drinking water but in the soil from now-closed lead smelters, said Chunrong Jia, a professor of environmental health at the University of Memphis. Almost all the heavy industry in Shelby County — and the associated pollutants — are located in southwest Memphis, Jia added.
Sources of pollution are often “clustered in particular communities,” said Darya Minovi, a senior analyst with the Union of Concerned Scientists, a nonprofit that advocates for environmental justice. When it comes to sterilizing facilities that emit ethylene oxide, areas inhabited largely by Black, Hispanic, low-income, and non-English-speaking people are disproportionately exposed, the group has found.
Four sites that the EPA labeled high-risk are in low-income areas of Puerto Rico. Seven sterilizer plants operate in that U.S. territory.
The EPA, responding to public concerns and to deepened scientific understanding of the hazards of ethylene oxide, recently released rules that the agency said would greatly reduce emissions of the toxic gas from sterilizing facilities.
KeShaun Pearson, who was born and raised in south Memphis and has been active in fighting environmental threats, said he is frustrated that companies with dangerous emissions are allowed to create “toxic soup” in minority communities.
In the area where the sterilization plant is located, 87% of the residents are people of color, and, according to the Southern Environmental Law Center, life expectancy there is about 10 years lower than the average for the county and state. The population within 5 miles of the sterilizer plant is mostly low-income, according to the Union of Concerned Scientists.
Pearson was part of Memphis Community Against the Pipeline, a group formed in 2020 to stop a crude oil pipeline that would have run through Boxtown, a neighborhood established by emancipated slaves and freedmen after the signing of the Emancipation Proclamation of 1863.
That campaign, which received public support from former Vice President Al Gore and actress-activist Jane Fonda, succeeded. After the ethylene oxide danger surfaced in 2022, the group changed the last word of its name from “pipeline” to “pollution.”
Besides breast and lymphoid cancers, animal studies have linked inhaling the gas to tumors of the brain, lungs, connective tissue, uterus, and mammary glands.
Last year, with the help of the Southern Environmental Law Center, the south Memphis community group urged the Shelby County Health Department to declare the ethylene oxide situation a public health emergency and shut down the sterilizing plant. But the health department said the company had complied with its existing air permit and with the EPA’s rules and regulations.
A health department spokesperson, Joan Carr, said Shelby County enforces EPA regulations to ensure that companies comply with the federal Clean Air Act and that the agency has five air monitoring stations around the county to detect levels of other pollutants.
When the county and the Tennessee Department of Health did a cancer cluster study in 2023, the agencies found no evidence of the clustering of high rates of leukemia, non-Hodgkin lymphoma, or breast or stomach cancer near the facility. There were “hot and cold spots” of breast cancer found, but the study said it could not conclude that the clusters were linked to the facility.
Scientists have criticized the study’s methodology, saying it did not follow the Centers for Disease Control and Prevention’s recommendations for designing a cancer cluster investigation.
Meanwhile, several people have sued the sterilizing company, claiming their health has been affected by the ethylene oxide emissions. In a lawsuit seeking class-action status, Reginaé Kendrick, 21, said she was diagnosed with a brain tumor at age 6. Chemotherapy and radiation have stunted her growth, destroyed her hair follicles, and prevented her from going through puberty, said her mother, Robbie Kendrick.
In response to proposed stricter EPA regulations, meanwhile, the Tennessee attorney general helped lead 19 other state AGs in urging the agency to “forgo or defer regulating the use of EtO by commercial sterilizers.”
Sims said she’s glad her neighborhood will have one less thing to worry about once Sterilization Services departs. But her feelings about the closure remain tempered.
“Hope they don’t go to another residential area,” she said.
[Clarification: This article was updated at 3:15 p.m. ET on May 1, 2024, to specify which substances leaked into the ground and groundwater and what changes will occur related to the Tennessee Valley Authority’s activities in Shelby County, Tennessee.]
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 5 months ago
Public Health, Race and Health, States, Disparities, Environmental Health, Florida, Oklahoma, Tennessee, texas, Virginia
A Physician Travels to South Asia Seeking Enduring Lessons From the Eradication of Smallpox
Smallpox was certified eradicated in 1980, but I first learned about the disease’s twisty, storied history in 1996 while interning at the World Health Organization. As a college student in the 1990s, I was fascinated by the sheer magnitude of what it took to wipe a human disease from the earth for the first time.
Over the years, I’ve turned to that history over and over, looking for inspiration and direction on how to be more ambitious when confronting public health threats of my day.
In the late 1990s, I had the opportunity to meet some of the health care professionals and other eradication campaign workers who helped stop the disease. I came to see that the history of this remarkable achievement had been told through the eyes mostly of white men from the United States, what was then the Soviet Union, and other parts of Europe.
But I knew that there was more to tell, and I worried that the stories of legions of local public health workers in South Asia could be lost forever. With its dense urban slums, sparse rural villages, complicated geopolitics, corrupt governance in some corners, and punishing terrain, South Asia had been the hardest battlefield the smallpox eradicators had to conquer.
I decided to capture some of that history. That work became a podcast, an eight-episode, limited-series audio documentary, called “Epidemic: Eradicating Smallpox.”
My field reporting began in summer 2022, when I traveled to India and Bangladesh — which had been the site of a grueling battle in the war on the disease. I tracked down aging smallpox workers, some now in their 80s and 90s, who had done the painstaking work of hunting down every last case of smallpox in the region and vaccinating everyone who had been exposed. Many of the smallpox campaign veterans had fallen out of touch with one another. Their friendships had been forged at a time when long-distance calls were expensive and telegrams were still used for urgent messages.
How did they defeat smallpox? And what lessons does that victory hold for us today?
I also documented the stories of people who contracted smallpox and lived. What can we learn from them? The survivors I met are not unlike my father, who grew up in a rural village in southern India where his childhood was shaped by family finances that limited access to opportunity. The stories he shared with me about the big social and economic divides in India fueled my decision to choose a career in public health and to work for equity. As we emerge from the covid pandemic, that connection is a big part of why I wanted to go back in time in search of answers to the challenges we face today.
Unwarranted Optimism
I sought out Indian and Bangladeshi public health workers, as well as the WHO epidemiologists — largely from the U.S. and Europe — who had designed and orchestrated the eradication campaigns across South Asia. Those smallpox leaders of the 1960s and ’70s showed moral imagination: While many doctors and scientists thought it would be impossible to stop a disease that had lasted for millennia, the eradication champions had a wider vision for the world — not just less smallpox or fewer deaths but elimination of the disease completely. They did not limit themselves to obvious or incremental improvements.
Bill Foege, a campaign leader in the 1970s, said by contrast today’s policymakers can be very reluctant to support programs that don’t already have data to back them up. They typically want proof of sustainability before investing in novel programs, he said, but real-world sustainability often only becomes clear when new ideas are put into practice and at scale.
The smallpox eradication visionaries were different from these cautious current leaders. “They had ‘unwarranted optimism,’” Foege said. They had faith that they could make “something happen that could not have been foreseen.”
In India, in particular, many leaders hoped their nation could compete with other superpowers on the world stage. That idealism, in part, stoked their belief that smallpox could be stopped.
During the smallpox program in South Asia, Mahendra Dutta was one the biggest risk-takers — willing to look beyond the pragmatic and politically palatable. He was a physician and public health leader who used his political savvy to help usher in a transformative smallpox vaccination strategy across India.
The eradication campaign had been grinding in India for over a decade. India had invested time and resources — and no small amount of publicity — into a mass vaccination approach. But the virus was still spreading out of control. At a time when India’s leaders were eager to project strength as a superpower and protective of the nation’s image on the world stage, Dutta’s was one of the voices that proclaimed to India’s policymakers that mass vaccination wasn’t working.
Dutta told them it was past time for India to adopt a new, more targeted vaccine strategy called “search and containment.” Teams of eradication workers visited communities across India to track down active cases of smallpox. Whenever they found a case, health workers would isolate the infected person, then vaccinate anyone that individual might have come in contact with.
To smooth the way for the new strategy, Dutta called in favors and even threatened to resign from his job.
He died in 2020, but I spoke with his son Yogesh Parashar, who said Dutta straddled two worlds: the in-the-trenches realities of smallpox eradication — and India’s bureaucracy. “My father did all the dirty work. He got enemies also in the process, I’m sure he did, but that is what he did,” Parashar said.
A Failure to Meet Basic Needs
Smallpox workers understood the need to build trust through partnerships: The WHO’s global smallpox eradication program paired its epidemiologists with Indian and Bangladeshi community health workers, who included laypeople with training and eager and idealistic medical students. Those local smallpox eradication workers were trusted messengers of the public health program. They leveraged the region’s myriad cultures and traditions to pave the way for people to accept the smallpox campaign and overcome vaccine hesitation. While encouraging vaccine acceptance, they embraced cultural practices: using folk songs to spread public health messages, for example, and honoring the way locals used the leaves of the neem tree to alert others to stay away from the home of someone infected with smallpox.
Smallpox eradication in South Asia unfolded against a backdrop of natural disaster, civil war, sectarian violence, and famine — crises that created many pressing needs. By many, many measures, the program was a success. Indeed, smallpox was stopped. Still, in the all-consuming push to end the virus, public health writ large often failed to meet people’s basic needs, such as housing or food.
The smallpox workers I interviewed said they were sometimes confronted by locals who made it clear they had concerns that, even in the midst of a raging epidemic, felt more immediate and important than smallpox.
Eradication worker Shahidul Haq Khan, whom podcast listeners meet in Episode 4, heard that sentiment as he traveled from community to community in southern Bangladesh. People asked him: “There’s no rice in people’s stomachs, so what is a vaccine going to do?” he said.
But the eradication mission largely did not include meeting immediate needs, so often the health workers’ hands were tied.
When a community’s immediate concerns aren’t addressed by public health, it can feel like disregard — and it’s a mistake, one that hurts public health’s reputation and future effectiveness. When public health representatives return to a community years or decades later, the memory of disregard can make it much harder to enlist the cooperation needed to respond to the next public health crises.
Rahima Banu Left Behind
The eradication of smallpox was one of humankind’s greatest triumphs, but many people — even the grandest example of that victory — did not share in the win. That realization hit me hard when I met Rahima Banu. As a toddler, she was the last person in the world known to have contracted a naturally occurring case of variola major smallpox. As a little girl, she and her family had — for a time — unprecedented access to care and attention from public health workers hustling to contain smallpox.
But that attention did not stabilize the family long-term or lift them from poverty.
Banu became a symbol of the eradication effort, but she did not share in the prestige or rewards that came after. Nearly 50 years later, Banu, her husband, their three daughters, and a son share a one-room bamboo-and-corrugated-metal home with a mud floor. Their finances are precarious. The family cannot afford good health care or to send their daughter to college. In recent years when Banu has had health problems or troubles with her eyesight, there have been no public health workers bustling around, ready to help.
“I cannot thread a needle because I cannot see clearly. I cannot examine the lice on my son’s head. I cannot read the Quran well because of my vision,” Banu said in Bengali, speaking through a translator. “No one wants to know how I am living my life with my husband and children, whether I am in a good condition or not, whether I am settled in my life or not.”
Missed Opportunities
I believe some of our public health efforts today are repeating mistakes of the smallpox eradication campaign, failing to meet people’s basic needs and missing opportunities to use the current crisis or epidemic to make sustained improvements in overall health.
The 2022 fight against mpox is one example. The highly contagious virus spiked around the world and spread quickly, predominantly among men who have sex with men. In New York City, for example, in part because some Black and Hispanic people had a historical mistrust for city officials, those groups ended up with lower rates of Mpox vaccination. And that failure to vaccinate became a missed opportunity to provide education and other health care treatments, including access to HIV testing and prevention.
And so has it gone with the covid pandemic, too. Health care providers, the clergy, and leaders from communities of color were enlisted to promote immunization. These trusted messengers were successful in narrowing race-related disparities in vaccination coverage, not only protecting their own but also shielding hospitals from crushing patient loads. Many weren’t paid to do this work. They stepped up despite having good reason to mistrust the health care system. In some ways, government officials upheld their end of the social contract, providing social and economic support to help these communities weather the pandemic.
But now we’re back to business as usual, with financial, housing, food, health care, and caregiving insecurity all on the rise in the U.S. What trust was built with these communities is again eroding. Insecurity, a form of worry over unmet basic needs, robs us of our ability to imagine big and better. Our insecurity about immediate needs like health care and caregiving is corroding trust in government, other institutions, and one another, leaving us less prepared for the next public health crisis.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Public Health, Epidemic, vaccines
Los hirieron en el desfile del Super Bowl: un mes después se sienten olvidados
Este año, Jason Barton no quería ir al desfile del Super Bowl. La noche anterior le dijo a un compañero de trabajo que estaba preocupado por que ocurriera un tiroteo masivo. Pero era San Valentín, su esposa es fanática de los Kansas City Chiefs y él no podía permitirse pagar las entradas a los partidos, que habían aumentado muchísimo tras la victoria del equipo en el campeonato de 2020.
Así que Barton condujo 50 millas desde Osawatomie, Kansas, hasta el centro de Kansas City, Missouri, con su esposa Bridget, Gabriella, su hija de 13 años, y una amiga del colegio de la niña. Cuando por fin regresaron esa noche a casa, tuvieron que limpiar sangre de las zapatillas de Gabriella y encontraron una bala en la mochila de Bridget.
Gabriella tenía quemaduras en las piernas por los chispazos de una bala que rebotó cerca de ella, Bridget había sido pisoteada mientras protegía a su hija en medio del caos, y Jason le había practicado masajes cardíacos a un hombre herido de bala: cree que era Lyndell Mays, uno de los dos acusados de asesinato.
“Se supone que San Valentín es un día en el que nos divertimos y celebramos a nuestros afectos. Pero ya nunca habrá un San Valentín en el que no me acuerde de esto”, dijo Gabriella.
Un mes después del desfile —en el que esa crisis de salud pública que es la violencia armada en el país se transmitió por televisión en vivo— los Barton siguen impactados por el papel que les tocó en el epicentro de los acontecimientos.
Se encontraban a escasos metros de Lisa López-Galván, de 43 años, que fue asesinada. Otras 24 personas resultaron heridas. Los Barton no están incluidos en el número oficial de víctimas, sin embargo, quedaron traumatizados, física y emocionalmente, y el dolor impregna sus vidas.
Ahora, Bridget y Jason prefieren quedarse juntos en casa y siguen cancelando planes para salir; Gabriella cambió de proyecto y en vez de tomar clases de baile se anotó en un club de boxeo.
Durante el primer mes, los líderes comunitarios de Kansas City han discutido cómo atender a las personas que quedaron atrapadas bajo el fuego cruzado y cómo distribuir los más de $2 millones donados a los fondos públicos para las víctimas bajo el doloroso impacto inicial.
Hay muchas preguntas: ¿cómo compensar a las personas por los gastos en atención médica y psicológica, por los tratamientos de recuperación, por los salarios perdidos? ¿Qué ocurre con quienes padecen síntomas de estrés post traumático (TEPT), que pueden durar años? ¿Cómo hace una comunidad para identificar y atender a los heridos, que son las víctimas que a menudo se pasan por alto en los primeros informes sobre un tiroteo masivo?
Y la lista de heridos podría aumentar. Mientras investigan a cuatro de los sospechosos del tiroteo, la fiscalía y la policía de Kansas City convocan a otras víctimas a presentarse.
“En concreto, buscamos personas que hayan sufrido heridas cuando intentaban escapar y se produjo la estampida”, explicó la fiscal del condado de Jackson, Jean Peters Baker. Alguien que, “mientras huía, se cayó, se torció un tobillo, se rompió un hueso o lo pisotearon”.
Mientras tanto, las personas que se encargaron de recaudar dinero y facilitar la atención de los heridos debaten los criterios para distribuirlo. Gracias a las cuantiosas donaciones de famosos como Taylor Swift y Travis Kelce, algunas víctimas o sus familias dispondrán de cientos de miles de dólares para gastos médicos. A otras es posible que solo se les cubra la terapia.
Una investigación reciente de la Facultad de Medicina de Harvard calcula que el costo económico global de las lesiones causadas por armas de fuego en Estados Unidos asciende a $557,000 millones anuales. El 88% de ese monto se explica por la pérdida de calidad de vida de las personas heridas y sus familias. El estudio revela que, solo en el primer año, cada lesión no mortal por arma de fuego genera unos $30,000 de gastos de salud directos por superviviente.
Inmediatamente después de los tiroteos, mientras aparecían páginas como GoFundMe para ayudar a las víctimas, los ejecutivos de United Way of Greater Kansas City se reunieron para idear una respuesta colectiva de donación. Se les ocurrieron “tres círculos concéntricos de víctimas”, explicó Jessica Blubaugh, directora de Filantropía de United Way, y lanzaron la campaña #KCStrong.
“Obviamente, en el primer círculo estás las personas que sufrieron directamente el impacto de los disparos. En el siguiente círculo se encuentran los que sufrieron un impacto físico —no necesariamente de los disparos—, por ejemplo, personas que fueron pisoteadas o se rompieron un ligamento cuando estaban huyendo”, dijo Blubaugh. “Luego, en tercer lugar, están las personas que se encontraban en las inmediaciones y los transeúntes, que quedaron psicológicamente muy afectados”.
Estrés post traumático, pánico y el eco de los disparos
Bridget Barton regresó a Kansas City al día siguiente del tiroteo para entregar la bala que había encontrado en su mochila y declarar en la comisaría.
Ella no lo sabía, pero el alcalde Quinton Lucas y los jefes de policía y bomberos acababan de terminar una rueda de prensa fuera del edificio. Bridget fue acosada por los periodistas allí reunidos, entrevistas que ahora le resultan borrosas. “No sé cómo hacen esto todos los días”, recuerda que le dijo a un detective cuando por fin pudo entrar.
Mientras atraviesan el trauma, los Barton se han visto abrumados, al punto del agotamiento, por las buenas intenciones de amigos y familiares. Bridget usó las redes sociales para explicar que no ignoraba los mensajes pero que los iba respondiendo en la medida que podía. Algunos días apenas puedo mirar el teléfono, contó.
Una amiga de la familia compró nuevas mantas de Barbie para Gabriella y su amiga; las que llevaron al desfile se perdieron o estropearon. Bridget había intentado reemplazar ella misma las mantas en Walmart. Pero alguien la empujó accidentalmente y le dio un ataque de pánico. Así que abandonó el carrito y condujo de vuelta a casa.
“Estoy intentando controlar mi ansiedad”, cuenta Bridget. Eso significa que necesita terapia. Antes del desfile ya consultaba a un terapeuta y planeaba empezar la desensibilización y reprocesamiento por movimientos oculares, un método asociado al tratamiento del TEPT. Ahora, de lo primero que quiere hablar en terapia es del tiroteo.
Desde que Gabriella, alumna de 8vo grado, volvió a la escuela, tiene que lidiar con la inmadurez propia de la adolescencia: compañeros que la instan a superar lo ocurrido, que la señalan con el dedo o que incluso le dicen que debería haber sido ella la asesinada. Pero sus amigos la contienen y le preguntan cómo está. Le gustaría que más gente hiciera lo mismo con su amiga, que salió corriendo cuando empezó el tiroteo y así evitó que la hirieran. Gabriella se siente culpable por haberla llevado a lo que se convirtió en una experiencia aterradora.
“Podemos decirle todo el día: ‘No fue culpa tuya. No es tu responsabilidad’, lo mismo que yo me digo: ‘No fue culpa mía, ni mi responsabilidad'”, explica Bridget. “Pero igualmente lloré en el hombro de la madre de la otra niña diciéndole lo mucho que sentía haber agarrado primero a mi hija”.
Desde el tiroteo, las dos niñas han pasado mucho tiempo hablando. Según Gabriella, eso la ayuda a aliviar su propio estrés. También la alivia pasar tiempo con su perro y con su lagartija, maquillarse y escuchar música: la actuación del rapero Tech N9ne fue para ella un momento culminante de la celebración del Super Bowl.
Además de que las chispas le quemaron las piernas, en la estampida Gabriella cayó sobre el cemento y eso le reabrió una quemadura que tenía en el abdomen, causada por una plancha de pelo. “Cuando veo eso, me imagino a mi madre intentando protegerme y a todo el mundo corriendo”, dijo Gabriella.
Es difícil no sentirse olvidada por la gente, opina Bridget. El tiroteo, y especialmente sus sobrevivientes, han desaparecido en gran medida de los titulares excepto en las fechas de los juicios. Desde el desfile hubo otros dos tiroteos de gran repercusión en la zona. Y se pregunta si a la comunidad no le importa que ella y su familia sigan viviendo con las secuelas a diario.
“Voy a decirlo de la forma más clara posible. Estoy muy, pero muy enojada porque mi familia haya tenido que pasar por algo traumático”, se desahogaba Bridget en una reciente publicación en las redes sociales. “En realidad no quiero otra cosa [que]: ‘Tu historia también importa y queremos saber cómo te va’. ¿Lo hemos conseguido? Absolutamente no.”
¿Qué se necesita?
Ayudados en parte por famosos como Swift y Kelce, las donaciones para la familia de López-Galván, la única víctima mortal, y para otras víctimas llegaron en masa inmediatamente después del tiroteo. Swift y Kelce donaron $100,000 cada uno. Con la ayuda de un aporte inicial de $200,000 de los Kansas City Chiefs, la campaña #KCStrong de United Way alcanzó el millón de dólares en las dos primeras semanas y ahora llega a los $1,2 millones.
Se crearon seis fondos GoFundMe verificados. Uno, destinado exclusivamente a la familia López-Galván, ha recaudado más de $406,000. Otros más pequeños fueron creados por un estudiante universitario local y por fans de Swift. Las iglesias también se comprometieron y una coalición local recaudó $183,000, dinero destinado al funeral de López-Galván, a solventar la terapia para cinco víctimas y a pagar facturas médicas del hospital Children’s Mercy Kansas City, según dijo Ray Jarrett, director ejecutivo de Unite KC.
Los líderes de esta iniciativa encontraron modelos en otras ciudades. Blubaugh, de United Way, consultó a funcionarios e instituciones que habían tenido que dar respuesta a las víctimas de sus propios tiroteos masivos en Orlando (Florida), Buffalo (Nueva York) y Newtown (Connecticut).
“La desafortunada realidad es que en todo el país existen comunidades que ya se han enfrentado a tragedias como ésta, explicó Blubaugh. Así que lamentablemente hay un protocolo que, en cierto modo, ya está en marcha”.
A partir de que Blubaugh informó que el dinero de #KCStrong podría empezar a pagarse a finales de marzo, cientos de personas llamaron a la línea 211 de las organizaciones sin fines de lucro. United Way está consultando con los hospitales y las fuerzas del orden para identificar a las víctimas, y ofrecerles los servicios que puedan necesitar.
El abanico de necesidades es asombroso: varias personas siguen recuperándose en su casa, y otras necesitan apoyo emocional y psicológico. Muchas, al principio, ni siquiera fueron contabilizadas. Por ejemplo, un agente de policía que ese día vestía de civil y resultó herido. Según el jefe de policía Stacey Graves, ya se encuentra bien.
Determinar quién es elegible para recibir asistencia fue una de las primeras conversaciones que tuvieron los funcionarios de United Way cuando crearon el fondo. Y decidieron priorizar tres áreas: primero a los heridos y sus familias; segundo a servicios de salud mental y a organizaciones que ya estuvieran ayudando a las víctimas en prevención de la violencia, y en tercer lugar a los socorristas.
En concreto, los fondos se destinarán a cubrir los costos médicos o los salarios perdidos de quienes no hayan podido trabajar desde los tiroteos, explicó Blubaugh. Y agregó que si bien el objetivo es ayudar rápidamente a la gente también se debe utilizar el dinero de una manera juiciosa y estratégica.
“No tenemos una visión clara del panorama al que nos enfrentamos”, dijo Blubaugh. “No sólo no sabemos de cuánto dinero disponemos sino cuál es el panorama de las necesidades. Hacen falta ambas cosas para tomar decisiones”.
Experiencia de la violencia cotidiana en Kansas City
Jason utilizó el único día de licencia que le quedaba para quedarse en casa con Bridget y Gabriella. Como técnico de automatización nocturna, es el principal sostén de la familia. “No puedo faltar al trabajo, explicó. Sucedió. Fue una porquería. Pero es hora de seguir adelante.”
“Es un hombre de verdad”, afirma Bridget.
La primera noche que Jason fue al trabajo, el ruido repentino de los platos al caer sobresaltó a Bridget y Gabriella, que se abrazaron llorando. “Son esos recuerdos los que nos están atormentando”, dijo Bridget, enojada.
En cierto modo, el tiroteo ha unido más a la familia que había pasado por muchas cosas recientemente: Jason sobrevivió a un ataque al corazón y a un cáncer el año pasado; y criar a un adolescente nunca es fácil.
Bridget agradece que la bala se alojara en su mochila y no la alcanzara, y que las chispas le hayan quemado las piernas a Gabriella pero que no le dispararan.
Jason está agradecido por otra razón: no ha sido un atentado terrorista, como temía al principio. En cambio, se trata del tipo de violencia armada a la que estaba acostumbrado porque creció en Kansas City, una ciudad que alcanzó su pico de muertes el año pasado. Aunque Jason nunca le había tocado tan de cerca.
“Esta basura ocurre todos los días, dijo. La única diferencia es que nosotros estábamos ahí para verlo”.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Health Care Costs, Noticias En Español, Public Health, States, Emergency Medicine, Guns, Investigation, Kansas, Missouri
KFF Health News' 'What the Health?': The ACA Turns 14
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
The Affordable Care Act was signed into law 14 years ago this week, and Health and Human Services Secretary Xavier Becerra joined KFF Health News’ Julie Rovner on this week’s “What the Health?” podcast to discuss its accomplishments so far — and the challenges that remain for the health law.
Meanwhile, Congress appears on its way to, finally, finishing the fiscal 2024 spending bills, including funding for HHS — without many of the reproductive or gender-affirming health care restrictions Republicans had sought.
This week’s panelists are Julie Rovner of KFF Health News, Mary Agnes Carey of KFF Health News, Tami Luhby of CNN, and Alice Miranda Ollstein of Politico.
Panelists
Mary Agnes Carey
KFF Health News
Tami Luhby
CNN
Alice Miranda Ollstein
Politico
Among the takeaways from this week’s episode:
- The Supreme Court will hear oral arguments next week in a case that could decide whether the abortion pill mifepristone will remain easily accessible. The case itself deals with national restrictions rather than an outright ban. But, depending on how the court rules, it could have far-reaching results — for instance, preventing people from getting the pills in the mail and limiting how far into pregnancy the treatment can be used.
- The case is about more than abortion. Drug companies and medical groups are concerned about the precedent it would set for courts to substitute their judgment for that of the FDA regarding drug approvals.
- Abortion-related ballot questions are in play in several states. The total number ultimately depends on the success of citizen-led efforts to collect signatures to gain a spot. Such efforts face opposition from anti-abortion groups and elected officials who don’t want the questions to reach the ballot box. Their fear, based on precedents, is that abortion protections tend to pass.
- The Biden administration issued an executive order this week to improve research on women’s health across the federal government. It has multiple components, including provisions intended to increase research on illnesses and diseases associated with postmenopausal women. It also aims to increase the number of women participating in clinical trials.
- This Week in Medical Misinformation: The Supreme Court heard oral arguments in the case Murthy v. Missouri. At issue is whether Biden administration officials overstepped their authority when asking companies like Meta, Google, and X to remove or downgrade content flagged as covid-19 misinformation.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: The Washington Post’s “Arizona Lawmaker Tells Her Abortion Story to Show ‘Reality’ of Restrictions,” by Praveena Somasundaram. (Full speech here.)
Alice Miranda Ollstein: CNN’s “Why Your Doctor’s Office Is Spamming You With Appointment Reminders,” by Nathaniel Meyersohn.
Tami Luhby: KFF Health News’ “Georgia’s Medicaid Work Requirement Costing Taxpayers Millions Despite Low Enrollment,” by Andy Miller and Renuka Rayasam.
Mary Agnes Carey: The New York Times’ “When Medicaid Comes After the Family Home,” by Paula Span, and The AP’s “State Medicaid Offices Target Dead People’s Homes to Recoup Their Health Care Costs,” by Amanda Seitz.
Also mentioned on this week’s podcast:
- NPR’s “Standard Pregnancy Care Is Now Dangerously Disrupted in Louisiana, Report Reveals,” by Rosemary Westwood.
- The Washington Post’s “As the Cost of Storing Frozen Eggs Rises, Some Families Opt to Destroy Them,” by Amber Ferguson.
Click to open the transcript
Transcript: The ACA Turns 14
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News, and I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, March 21, at 10 a.m. As always, news happens fast and things might have changed by the time you hear this. So here we go.
We are joined today via video conference by Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Hello.
Rovner: Tami Luhby of CNN.
Tami Luhby: Hello.
Rovner: And my KFF Health News colleague Mary Agnes Carey.
Mary Agnes Carey: It’s great to be here.
Rovner: Later in this episode to mark the 14th anniversary of the Affordable Care Act, we’ll have my interview with Health and Human Services Secretary Xavier Becerra, but first, this week’s news. So it appears our long national nightmare following the progress of the fiscal 2024 spending bill for the Department of Health and Human Services is nearly over, nearly halfway through the fiscal year. The White House, House, and Senate have, as far as we can tell, reached a compromise on the last tranche of spending bills, which is a good thing because the latest temporary spending bill runs out at midnight Friday. Funding for the Department of Health and Human Services, from what I’ve seen so far, is basically flat, which is a win for the Democrats because the Republicans had fought for a cut of something in the neighborhood of 22%.
Now, assuming this all happens, the House is scheduled to vote, as we speak now, on Friday at 11 a.m., leaving the Senate not very much time to avert a possible partial shutdown. Democrats seem also to have avoided adding all manner of new restrictions on reproductive and gender-affirming health care to the HHS part of the bill. It’s the last big train leaving the station likely until after the election. So Alice, we’ll get to the add-ons in a minute, but have you seen anything in the HHS funding worthy of note or did they manage to fend off everything that would’ve been significantly newsworthy?
Ollstein: Like you said, it is basically flat. It’s a small increase, less than 1% overall for HHS, and then a lot of individual programs are just completely flat, which advocacy groups argue is really a cut when you factor in inflation. The cost of providing services and buying medications and running programs and whatnot goes up. So flat funding is a cut in practice. I’m hearing that particularly from the Title X family planning folks that have had flat funding for a decade now even as demand for services and costs have gone up.
So I think that in the current environment, Democrats are ready to vote for this. They don’t want to see a shutdown. And in the House, the bill passage will depend on those Democratic votes because they are likely to lose a lot of Republicans. Republicans are mad that there weren’t deeper cuts to spending and, as you alluded to, they’re mad that they didn’t get these policy rider wins they were banking on.
Rovner: As I’ve mentioned, since this is a must-pass bill, there are always the efforts to add non-spending things to it. And on health care, apparently, the effort to add the PBM, pharmacy benefit regulation bill we’ve talked about so much failed, but lawmakers did finally get a one-year deal to extend PEPFAR, the international AIDS/HIV program. Alice, you’ve been dutifully following this since it expired last year. Remind us why it got held up and what they finally get.
Ollstein: What happened in the end is it is a one-year reauthorization that’s a so-called clean reauthorization, meaning they are not adding new anti-abortion restrictions and provisions that the Republicans wanted. So what we reported this week is, like any compromise, no one’s happy. So Republicans are upset that they didn’t get the anti-abortion restrictions they wanted, and I’ll explain more on that in a second, and Democrats are upset that this is just a one-year reauthorization. It’s the first reauthorization that’s this sort of short-term stopgap length. In the program’s decades of history, it’s always been a full five-year reauthorization up until now. But the fight over abortion and accusations that program funds were flowing to abortion providers really split Congress on this.
Even though you had mainstream leadership Republicans who were saying, “Look, we just want to reauthorize this as-is,” you had a small but very vocal contingent of hard-line anti-abortion lawmakers backed by some really influential groups like the Heritage Foundation and SBA [Susan B. Anthony Pro-Life America] who were saying, “No, we have to insist on a shorter-term reauthorization,” so that they hope Trump will be in office next year and can impose these exact same anti-abortion restrictions through executive action. So they’re basically trying to punt control of the program into what they hope is a more favorable environment, where either they’ll have the votes in Congress to make these changes and restrictions to the program or they can do it through the White House.
Rovner: So basically, the fight over PEPFAR, not over. So as I already mentioned, Saturday is the 14th anniversary of the Affordable Care Act, which you’ll hear more about in my interview with HHS Secretary Becerra, but I wanted to pose to you guys one of the questions that I posed to him. As Nancy Pelosi famously predicted, at least according to public opinion polls, the more people learned about the health law, indeed, the more they are liking it. But it still lacks the popularity and branding of big government health programs, like Medicare and Medicaid, and I think lots of people still don’t know that lots of the provisions that they like, things like letting your adult children stay on your health plan until they’re 26 or banning preexisting condition exclusions, those were things that came from the Affordable Care Act. Any theories as to why it is still so polarizing? Republicans didn’t love Medicare and Medicaid at the beginning either, so I don’t think it’s just that Republicans still talk about it.
Luhby: Part of it I think is because there are so many provisions and they’re not labeled the Affordable Care Act like Medicare is. Actually to some extent, Medicaid may not be as well known in some states because states have different Medicaid programs and different names and so do the ACA exchanges. So that’s part of it, but also, things like why do you get a free mammogram and why you get to go for a routine checkup every year; that’s not labeled as an Affordable Care Act provision, that’s just the preventive services. So I think that it would be difficult now after 14 years to bring all of that into the everyday branding by doctors and health providers. But that’s certainly what the administration and advocates are trying to do by sending out a lot of messages that list all of the benefits of the ACA.
Rovner: I will say this is the biggest full-court press I’ve seen an administration do on the ACA in quite a while. Obviously, it’s a presidential election year and it’s something that the Biden administration is proud of, but at least I would think that maybe just all the publicity might be part of their strategy. Mac, you wanted to say something.
Carey: No, absolutely. It’s going to be part of the Biden reelection campaign. They’re going to be pushing it, talking a lot about it. We have to remember we’ve had this ringside seat to all the Republican opposition to the Affordable Care Act. All the conversation about we’re going to repeal it and put something better in, former President Trump is still sending that message out to the electorate. I don’t know how much confusion, if any confusion, it creates, but to Tami’s point, you’ve got millions of people that have gotten coverage under the Affordable Care Act but millions more have benefited by all these provisions we’re talking about: the preventive care provisions, leaving adult kids up to 26 on your health insurance plan, that kind of thing.
Also, give it time. Fourteen years is a long time, but it’s not the time of Medicare, which was created in 1965, and Medicaid. So I think over time, the Affordable Care Act is part of the fabric and it will continue to be. But absolutely, for sure, President Biden is going to run on this, like you said, Julie, full-court press, talk extensively about it in the reelection campaign.
Ollstein: It makes sense that they’re leaning really hard on Obamacare as a message because, even if everyone isn’t familiar with it, a lot more people are familiar with it and like it than, polling shows, on the Biden administration’s other big health care accomplishment, which is drug price negotiation, which polling shows that most people, and even most seniors, who are the ones who are set to benefit the most, aren’t aware that it exists. And that makes sense because they’re not feeling the impact of the lower prices yet because this whole thing just started and it won’t be until 2026 that they’ll really actually experience cheaper medications. But people are already feeling the direct impact of Obamacare on their lives, and so it does make sense that they’re going to lean really hard on this.
Rovner: Of course, we went through the same thing with Obamacare, which also didn’t take full effect until, really, this is really the 10th anniversary of the full effect of the Affordable Care Act because it didn’t take effect until 2014. Tami, you wanted to add something.
Luhby: No, I was going to say it’s also the seventh anniversary of the Trump administration and congressional Republicans trying to tear apart the Affordable Care Act and repeal and replace it, which is the messaging that you’re seeing now is very similar to what you saw in 2017. It’s just surprising to me that with very intensive messaging on both sides at that time about what the Republicans saying what the problems are and the Democrats saying what all of the benefits are, — including the protections for people with preexisting conditions and the other things we’ve mentioned — that more people don’t associate those provisions with the ACA now. But the Biden administration is trying to revive all of that and remind people, as they did in 2018 in the successful midterm elections for the Democrats, that the ACA does provide a lot of the benefits that they are taking advantage of and appreciate.
Rovner: I think, in some ways, the 2017 fight was one of the best things that ever happened to the ACA in terms of helping people understand what actually was in it, because the Democrats managed to frighten people about things that they liked being taken away. Here we go again. All right, let us turn to abortion. There’s a new report out from the Guttmacher Institute that finds a dramatic jump in the use of medication abortion in 2023, the first full year since the Supreme Court reversed the nationwide right to abortion in the Dobbs [v. Jackson Women’s Health Organization] case, more than 60% of abortions use medication rather than a procedure last year. This news comes as the Supreme Court next week prepares to hear oral arguments in a case that could dramatically restrict availability of the abortion pill mifepristone. Alice, remind us what’s at stake in this case. It’s no longer whether they’re going to just outright cancel the approval.
Ollstein: That’s right. So the Supreme Court is taking up the narrowed version of this from the 5th Circuit. So what’s at stake are national restrictions on abortion pills, but not a national outright ban like you mentioned. But those restrictions could be really sweeping and really impactful. It would prevent people from getting the pills through the mail like they currently do. It would prevent people from potentially getting them in any other way other than directly from a doctor. So this would apply to red states and blue states alike. It would override abortion rights provisions in blue states that have done a lot to increase access to the pills. And it would also restrict their use back to the first seven weeks of pregnancy instead of 10, which is a big deal because people don’t often find out they’re pregnant until getting close to that line or beyond.
So this is a really big deal, and I think you can really see, especially from the flurry of amicus briefs have been filed, that anxiety about this case in the medical community and the pharmaceutical community, the scientific community, it goes way beyond the impact just on abortion. People are really worried about setting a precedent where the FDA’s scientific judgment is second-guessed by courts, and they worry that a win for the anti-abortion groups in this case would open the door to people challenging all kinds of other medications that they have an issue with: contraception, covid vaccines, HIV drugs, the list goes on and on, gender-affirming care medications, all sorts of things. So there are the bucket of potential impacts on abortion specifically, which are certainly significant, and then there’s the bigger slippery slope fears as well.
Rovner: Also, this is obviously still way political. More than just the abortion pill. It’s been a while since we’ve talked about state ballot measures. We, I think, feel like we spent all of last year talking about abortion state ballot measures. Alice, catch us up real quick on where we are. How many states have them? And what is this campaign against, by the anti-abortion people, to try to prevent them from getting on the ballot?
Ollstein: Check me if I’m wrong, but I don’t believe we know for sure about, especially the states that have citizen-led ballot initiatives where people are gathering signatures. So Florida had one of the earliest deadlines and they did meet their signature threshold. But they are now waiting on the state Supreme Court to say whether or not they have a green light to go forward this fall. A lot of other states are still collecting signatures. I think the only states we know for sure are the ones where the state legislature is the one that is ordering it to be put on the ballot, not regular citizens gathering signatures.
We still don’t know, but things are moving forward. I was just in Arizona reporting on their efforts. Things are moving forward there. Things are moving forward in Montana. They just got a court ruling in their favor to put something on the ballot. And things are moving forward in Missouri, a lot of places. So this could be really huge. Of course, like you mentioned, anti-abortion groups and anti-abortion elected officials are doing a lot of different things to try to prevent this from going on the ballot.
It’s interesting, you heard arguments over the last couple years against this being more along the lines of, “Oh, this is allowing these out-of-state big-money groups to swoop in and mislead and tell us what to do,” and those were the anti-abortion arguments against allowing people to vote on this directly. Now, you’re hearing, I’m hearing, more arguments along the lines of, “This shouldn’t be something subject to a popular vote at all. We shouldn’t put this up for a vote at all.” They consider this a human rights issue, and so I think that’s a really interesting evolution as well, particularly when the fall of Roe [v. Wade] was celebrated for returning the question of abortion access to the people, but maybe not these people specifically.
Rovner: I’ve been interested in seeing some of these anti-abortion groups trying to launch campaigns to get people not to put signatures on petitions. That’s moving it back a step I don’t think I’d ever seen. I don’t think I’ve ever seen a campaign to say, “Don’t sign the petition that would put this on the ballot to let people vote on it.” But that’s what we’re seeing, right?
Ollstein: Well, that’s what I went to Arizona to see firsthand is how that’s working, and it’s fascinating. They really worry that if it gets on the ballot, it’ll pass. It has in every state so far, so it’s reasonable for them to assume that. So they’re trying to prevent it from getting on the ballot. The way they’re doing that is they’re tracking the locations of signature gatherers and trying to go where they are and trying to intervene and hold up signs. I saw this firsthand. I saw it at a street fair. People were gathering signatures and several anti-abortion demonstrators were standing right in front of them with big signs and trying to argue with people and deter them from signing. It was not working, from what I observed. And from the overall signature count statewide, it was not working in Arizona. But it’s fascinating that they’re trying this.
Carey: I was going to say just our reporting from our KFF Health News colleagues found that 13 states are weighing abortion-related ballot measures, most of which would protect abortion rights. To your point, the scope is pretty extensive. And for all the reasons Alice just discussed, it’s quite the issue.
Rovner: Yeah, and we will obviously talk more about this as the election gets closer. I know we talk about Texas a lot on this podcast, but this week, I want to highlight a study from next door in Louisiana, also a very strong anti-abortion state. A new report from three groups, all of which support abortion rights, charges that, as in Texas, women with pregnancy complications are being forced to wait for care until their conditions become critical. And in some cases, women with nonviable pregnancies are being forced to have C-section surgery because their doctors don’t dare use medication or other less-risky procedures in case they could be accused of performing an abortion.
At some point, you have to think that somebody is going to have a malpractice case. Having a C-section because your doctor is afraid to terminate a nonviable pregnancy seems like pretty dangerous and rather aggressive way to go. This is the first I’ve ever heard of this. Alice, have you heard anything about this?
Ollstein: Not the C-section statistics specifically, but definitely the delays in care and some of the other impacts described in that report have absolutely been reported in other states and in legal challenges that have come up in Texas, in Oklahoma, in Tennessee, in Idaho by people who were denied abortions and experienced medical harms because of it. So I think that fits into the broader pattern. And it’s just more evidence about how this is having a chilling effect on doctors. And the exact letter of the law may be one thing, and you have elected officials pointing to exemptions and provisions in the law, but the chilling effect, the fear and the confusion in the medical community, is something in addition to that.
Rovner: As we put it out before, doctors have legitimate fears even if they don’t want to get dragged into court and have to hire lawyers and take time off — even if they’re innocent, even if they have what they consider to be pretty strong evidence that whatever it was that they did was legitimate under the law in terms of taking care of pregnant women. A lot of them, they don’t want to come under scrutiny, let’s put it that way, and it is hard to blame them about that.
Meanwhile, the backlash over the Alabama Supreme Court decision that fertilized embryos for IVF have legal rights is continuing as blue states that made themselves safe spaces for those seeking abortion are now trying to welcome those seeking IVF. Anybody think this is going to be as big a voting issue as abortion this fall? It’s certainly looking like those who support IVF, including some Republicans, are trying to push it.
Carey: I would think yes, it absolutely will be because it has been brought into the abortion debate. The actual Alabama issue is about an Alabama law and whether or not this particular, the litigants who sued were … it was germane and covered by the law, but it’s been brought into the abortion issue. The whole IVF thing is so compelling, about storage of the embryos and what people have to pay and all the restrictions around it and some of the choices they’re making. I guess that you could say more people have been touched by IVF perhaps than the actual abortion issue. So now, it’s very personal to them and it’s been elevated, and Republicans have tried to get around it by saying they support it, but then there’s arguments that whether or not that’s a toothless protection of IVF. It came out of nowhere I think for a lot of politicians and they’ve been scrambling and trying to figure it out. But to your point, Julie, I do wonder if it will be elevated in the election. And it was something they didn’t think they’d have to contend with, rather, and now they do.
Rovner: Obviously, it’s an issue that splits the anti-abortion community because now we’ve had all these very strong pro-lifers like Mike Pence saying, “I created my family using IVF.” Nikki Haley. There are a lot of very strong anti-abortion Republicans who have used IVF. So you’ve got some on the far … saying, “No, no, no, you can’t create embryos and then destroy them,” and then you’ve got those who are saying, “But we need to make sure that IVF is still available to people. If we’re going to call ourselves pro-life, we should be in favor of people getting pregnant and having babies, which is what IVF is for.” Alice, I see you nodding your head.
Ollstein: Yeah. So we’re having sort of a frustrating discourse around this right now because Democrats are saying, “Republicans want to ban IVF.” And Republicans are saying, “No, we don’t. We support IVF. We love IVF. IVF is awesome.” And neither is totally accurate. It’s just missing a lot of nuance. Republicans who say they support IVF also support a lot of different kinds of restrictions on the way it’s currently practiced. So they might correctly argue that they don’t want to ban it entirely, but they do want it practiced in a different way than it is now, such as the production of many embryos, some of which are discarded. So I think people are just not being asked the right questions right now. I think you got to get beyond, “Do you support IVF?” That gives people a way to dodge. I think you really have to drill into, “OK. How specifically do you want this regulated and what would that mean for people?”
Carey: Right, and the whole debate with some of the abortion rights opponents, some of them want the federal government to regulate it. Mike Johnson, speaker of the House, has come out and said, “No, no, that can be done at the state level.” So they’ve got this whole split internally in the party that is, again, a fight they didn’t anticipate.
Rovner: Well, Mac, something that you alluded to that I was struck by was a piece in The Washington Post this week about couples facing increasing costs to store their IVF embryos, often hundreds of dollars a year, which is forcing them to choose between letting the embryos go or losing a chance to possibly have another child. It’s obviously a big issue. I’m wondering what the anti-IVF forces think about that. As we’ve seen in Alabama, it’s not like you can just pick your embryos up in a cooler and move them someplace else. Moving them is actually a very big deal.
I don’t wish to minimize this, but I remember you have storage units for things, not obviously for embryos. One of the ways that they make money is that they just keep raising the cost because they think you won’t bother to move your things, so that you’ll just keep paying the increased cost. It feels like that’s a little bit of what’s happening here with these stored embryos, and at some point, it just gets prohibitively expensive for people to keep them in storage. I didn’t realize how expensive it was.
Carey: They’re all over the place. In preparing for this discussion, I’ve read things about people are paying $600 a year, other people are paying $1,200 a year. There’s big jumps from year to year. It can be an extremely expensive proposition. Oh, my goodness.
Rovner: IVF itself, I think as we’ve mentioned, is also extremely expensive and time-consuming, and emotionally expensive. It is not something that people enter into lightly. So I think we will definitely see more as we go. There’s also women’s health news this week that doesn’t have to do with reproduction. That’s new. Earlier this week, President Biden issued an executive order attempting to ensure that women are better represented in medical research. Tami, what does this order do and why was it needed?
Luhby: Well, it’s another attempt by the Biden administration, as we’ve discussed, to focus on reproductive health and reproductive rights. During the State of the Union address earlier this month, Biden asked Congress to invest $12 billion in new funding for women’s health research. And there are actually multiple components to the executive order, but the big ones are that it calls for supporting research into health and diseases that are more likely to occur midlife for women after menopause, such as rheumatoid arthritis, heart attacks, osteoporosis, and as well as ways to improve the management of menopause-related issues.
We are definitely seeing that menopause care is of increasing focus in a multitude of areas including employer health insurance, but the executive order also aims to increase the number of women participating in clinical trials since they’re poorly represented now. We know that certain medications and certain treatments have different effects on women than men, but we don’t really know that that well because they’re not as represented in these clinical trials. Then it also directs agencies to develop and strengthen research and data standards on women’s health across all of the relevant research and funding opportunities in the government.
Rovner: I’ll say that this is an issue I have very strong feelings about because I covered the debate in 1992 about including women in medical research. At the time, doctors didn’t want to have women in clinical trials because they were worried about hormones, and they might get pregnant, and we wouldn’t really know what that meant for whatever it was that we were testing. Someone suggested that “If you’re going to use these treatments and drugs on women, maybe you should test them on women too.” Then I won an award in 2015 for a story about how they still weren’t doing it, even though it was required by laws.
Carey: And here we are, 2024.
Rovner: Yeah, here we are. It just continues, but at least they’re trying. All right, finally, this week in medical misinformation, we travel to the Supreme Court, where the justices heard oral arguments in a case brought by two Republican state attorneys general charging that the Biden administration, quote, “coerced” social media platforms, Google, Meta, and X, into downgrading or taking down what public health officials deemed covid disinformation. I didn’t listen to the arguments, but all the coverage I saw suggested that the justices were not buying what the attorneys general were selling.
Yet another public-health-adjacent case to watch for a decision later this spring, but I think this is really going to be an important one in terms of what public officials can and cannot do using their authority as public health officials. We’re obviously in a bit of a public health trust crisis, so we will see how that goes.
All right, that is the news for this week. Now, we will play my interview with HHS Secretary Xavier Becerra, then we will be back with our extra credits.
I am so pleased to welcome back to the podcast Health and Human Services Secretary Xavier Becerra. I’ve asked him to join us to talk about the Affordable Care Act, which was signed into law 14 years ago this weekend. Mr. Secretary, thanks so much for coming back.
Xavier Becerra: Julie, great to be with you on a great week.
Rovner: So the Affordable Care Act has come a long way, not just in the 14 years since President Obama signed it into law, but in the 10 years since the healthcare.gov website so spectacularly failed to launch, but this year’s enrollment setting a record, right?
Becerra: That’s right, and you should have said, “You’ve come a long way, baby.”
Rovner: So what do we know about this year’s enrollment numbers?
Becerra: Another record breaker. Julie, every year that President Biden has been in office, we have broken records. Today, more Americans have health insurance than ever in the history of the country. More than 300 million people can now go to a doctor, leave their child in a hospital and know they won’t go bankrupt because they have their own health insurance. That’s the kind of peace of mind you can’t buy. Some 21.5 million Americans today look to the marketplace on the Affordable Care Act to get their coverage. By the way, the Affordable Care Act overall, some 45 million Americans today count on the ACA for their health care insurance, whether it’s through the marketplace, through Medicaid, or some of these basic plans that were also permitted under the ACA.
Rovner: Obviously, one of the reasons for such a big uptake is the expanded subsidies that were extended by the Inflation Reduction Act in 2022, but those expire at the end of next year, the end of 2025. What do you think would happen to enrollment if they’re not renewed?
Becerra: Well, and that’s the big question. The fact that the president made health care affordable was the big news. Because having the Affordable Care Act was great, but if people still felt it was unaffordable, they wouldn’t sign on. They now know that this is the best deal in town and people are signing up. When you can get health insurance coverage for $10 or less a month in your premiums, that’s a great deal. You can’t even go see a movie at a theater today for under $10. Now, you can get health care coverage for a full month, Julie. Again, as I always tell people, that doesn’t even include the popcorn and the refreshment at the movie theater, and so it’s a big deal. But without the subsidies, some people would still say, “Ah, it’s still too expensive.” So that’s why the president in his budget calls for extending those subsidies permanently.
Rovner: So there are still 10 states that haven’t taken up the federal government’s offer to pay 90% of the costs to expand Medicaid to all low-income adults in their states. I know Mississippi is considering a bill right now. Are there other states that you expect could join them sometime in the near future? Or are any of those 10 states likely to join the other 40?
Becerra: We’re hoping that the other 10 states join the 40 that have come on board where millions of Americans today have coverage. They are forsaking quite a bit of money. I was in North Carolina recently where Gov. [Roy] Cooper successfully navigated the passage of expansion for Medicaid. Not only was he able to help some 600,000-plus North Carolinians get health coverage, but he also got a check for $1.6 billion as a bonus. Not bad.
Rovner: No, not bad at all. So many years into this law, I feel like people now understand a lot of what it did: let adult children stay on their parents’ health plans until the age of 26; banning most preexisting condition exclusions in health coverage. Yet most people still don’t know that those provisions that they support were actually created by Obamacare or even that Obamacare and the Affordable Care Act are the same thing. Medicare has had such great branding success over the years. Why hasn’t the ACA?
Becerra: Actually, Julie, I think that’s changing. Today, about two-thirds of Americans tell you that they support the marketplaces in the Affordable Care Act. I think we’re actually now beginning an era where it’s no longer the big three, where you had Social Security, Medicare, and Medicaid and everyone protects those. Today, I think it’s the big four, the cleanup hitter being marketplace. Today, you would find tens of millions of Americans who would say, “Keep your dirty, stinking hands off of my marketplace.”
Rovner: Well, we will see as that goes forward. Obviously, President Biden was heavily involved in the development of the Affordable Care Act as vice president, as were you as a member of the House Ways and Means Committee at the time. What do you hope is this administration’s biggest legacy to leave to the health law?
Becerra: Julie, I think it’s making it affordable. The president made a commitment when he was first running to be president. He said on health care he was going to make it more affordable for more Americans with better benefits, and that’s what he’s done. The ACA is perfect proof. And Americans are signing up and signaling they agree by the millions. To go from 12 million people on the Affordable Care Act marketplace to 21.5 million in three years, that’s big news.
Rovner: So if I may, one question on another topic. Next week, the Supreme Court’s oral arguments occur in the case it could substantially restrict the availability of the abortion pill mifepristone. Obviously, this is something that’s being handled by the Justice Department, but what is it about this case that worries you most as HHS secretary, about the potential impact if the court rolls back FDA approval to the 2016 regulations?
Becerra: Well, Julie, as you well know from your years of covering health care, today there are Americans who have less protection, fewer rights, than many of us growing up. My daughters, my three daughters today, have fewer protections and access to health care than my wife had when she was their age. That’s not the America most of us know. To see another case where, now, medication abortion, which is used by millions of Americans — in fact, it’s the most common form of care that is received by a woman who needs to have abortion services — that is now at stake. But we believe that if the Supreme Court believes in science and it believes in the facts, because mifepristone has been used safely and effectively publicly for more than 20 years, that we’re going to be fine.
The thing that worries me as much, not just in the reduction of access to care for women in America, is the fact that mifepristone went through a process at the FDA similar to scores and scores of other medications that Americans rely on, that have nothing to do with abortion. And if the process is shut down by the Supreme Court for mifepristone, then it’s probably now at risk for all those other drugs, and therefore those other drugs that Americans rely on for diabetes, for cancer, who knows what, might also be challenged as not having gone through the right process.
Rovner: I know the drug industry is very, very worried about this case and watching it closely, and so will we. Mr. Secretary, thank you so much for joining us.
Becerra: Always good to be with you, Julie.
Rovner: OK, we are back. It’s time for our extra-credit segment. That’s when we each recommend a story we read this week we think you should read, too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Tami, why don’t you go first this week?
Luhby: OK, my extra credit this week is an article about Georgia’s unique Medicaid program from KFF Health News’ Andy Miller and Renuka Rayasam. It’s titled “Georgia’s Medicaid Work Requirement Costing Taxpayers Millions Despite Low Enrollment.” And I’m really glad they did this story. I and many others wrote about Georgia launching this program initially but haven’t done follow-up. So I was very happy to see this story.
As many of our listeners probably know, the Trump administration allowed multiple states to impose work requirements in Medicaid for the first time in the program’s history in 2018. But the efforts were eventually stopped by the courts in all states except Georgia. Georgia was allowed to proceed with adding its work requirement to Medicaid because it was actually going to expand coverage to allowing adults with incomes up to 100% of the poverty line to qualify. So the Georgia Pathways to Coverage initiative began last June.
Andy and Renuka took a look at how it’s faring, and the answer is actually not so well. Only about 3,500 people have signed up, far short of the 25,000 that the state projected for the first year. What’s more, the program has cost taxpayers at least $26 million so far, with more than 90% of that going towards administrative and consulting costs rather than actual medical care for low-income people.
By contrast, expanding Medicaid under the Affordable Care Act to people with 138% of the poverty line would make at least 359,000 uninsured Georgia residents newly eligible for coverage and reduce state spending by $710 million over two years. That’s what the advocates are pushing. So we’ll see what happens in coming months. One thing that’s also noted in the story is that about 45% of Pathways applications were still waiting to be processed.
Rovner: I will point out that we did talk a couple of weeks ago about the low enrollment in the Georgia program. What we had not seen was how much it’s actually costing the states per enrollee. So it is really good story. Alice, why don’t you go next?
Ollstein: Yeah, so I have some very relatable news from CNN. It’s called “Why Your Doctor’s Office Is Spamming You With Appointment Reminders.” It’s about why we all get so many obnoxious repeat reminders for every medical appointment. It both explains why medical practices that operate on such a tiny profit margin are so anxious about no-shows and last-minute cancellations, and so that’s part of it. But also part of it is that there are all these different systems that don’t communicate with one another. So the prescription drug system and the electronic medical records system and the doctor’s office’s own system are all operating in parallel and not coordinating with one another, and that’s why you get all these annoying multiple reminders. The medical community is becoming aware that it’s backfiring because the more you get, the more you start tuning them out and you don’t pay attention to which ones might be important. So they are working on it. So a somewhat hopeful piece of news.
Rovner: Raise your hand if you have multiple patient portals that you have to deal with for your multiple …
Ollstein: Oh, my God, yes.
Rovner: I will note that everybody’s hands go up. Mac?
Carey: I have not one but two stories on a very important issue: Medicaid estate recovery. The first is from Paula Span at The New York Times. The headline says it all, “When Medicaid Comes After the Family Home.” And the second story is an AP piece by Amanda Seitz, and that’s titled “State Medicaid Offices Target Dead People’s Homes to Recoup Their Health Care Costs.” Now, these stories are both about a program that’s been around since 1993. That’s when Congress mandated Medicaid beneficiaries over the age of 55 that have used long-term care services, and I’m talking about nursing homes or home care, that states must try to recover those expenses from the beneficiaries’ estates after their deaths.
As you can imagine, this might be a problem for the beneficiaries. They might have to sell a family home, try to find other ways to pay a big bill from Medicaid. Rep. Jan Schakowsky, she’s a Democrat of Illinois, has reintroduced her bill. It’s called the Stop Unfair Medicaid Recoveries Act. She’s trying to end the practice. She thinks it’s cruel and harmful, and her argument is, in fact, the federal and state governments spend way more than what they collect, and these collections often go after low-income families that can’t afford the bill anyway.
So even though it’s been around, it’s important to read up on this. A critical point in the stories was do states properly warn people that assets were going to be recovered if they enroll a loved one in Medicaid for long-term care and so on. So great reading, people should bone up on that.
Rovner: This is one of those issues that just keeps resurfacing and doesn’t ever seem to get dealt with. Well, my story this week is from The Washington Post, although I will say it was covered widely in dozens of outlets. It’s called “Arizona Lawmaker Tells Her Abortion Story to Show ‘Reality’ of Restrictions.” On Monday, Arizona State Sen. Eva Birch stood up on the Senate floor and gave a speech unlike anything I have ever seen. She’s a former nurse at a women’s health clinic. She’s also had fertility issues of her own for at least a decade, having both had a miscarriage and an abortion for a nonviable pregnancy in between successfully delivering her two sons.
Now, she’s pregnant again, but with another nonviable pregnancy, which she plans to terminate. Her point in telling her story in public on the Senate floor, she said, was to underscore how cruel — her words — Arizona’s abortion restrictions are. She’s been subject to a waiting period, required to undergo an invasive transvaginal ultrasound to obtain information she and her doctor already knew about her pregnancy, and to listen to a lecture on abortion, quote, “alternatives,” like adoption, which clearly don’t apply in her case.
While she gave the speech on the floor, several of her Democratic colleagues stood in the camera shot behind her, while many of the Republicans reportedly walked out of the chamber. I will link to the story, but I will also link to the entire speech for those who want to hear it.
OK, that is our show. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us, too. Special thanks as always to our technical guru, Francis Ying, and our fill-in editor for today, Stephanie Stapleton. As always, you can email us your comments or questions. We’re at whatthehealth@kff.org, or you can still find me at X, @jrovner, or @julierovner at Bluesky and @julie.rovner at Threads. Mary Agnes, where are you hanging out these days?
Carey: I’m hanging out on X, @MaryAgnesCarey.
Rovner: Alice?
Ollstein: @AliceOllstein on X, and @alicemiranda on Bluesky.
Rovner: Tami?
Luhby: The best place to find me is at cnn.com.
Rovner: There you go. We will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Stephanie Stapleton
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ “What the Health?” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Health Care Costs, Health Industry, Insurance, Medicaid, Medicare, Multimedia, Pharmaceuticals, Public Health, States, Abortion, Biden Administration, Drug Costs, KFF Health News' 'What The Health?', Misinformation, Podcasts, Pregnancy, Prescription Drugs, Women's Health
Sitios de telesalud prometen una cura para la “menopausia masculina” a pesar de prohibiciones
Durante el boom de la telemedicina por la pandemia de covid-19, surgieron tiendas online que promocionaban la testosterona como remedio para las afecciones masculinas relacionadas con la edad, a pesar de las normas de la Administración de Drogas y Alimento
Durante el boom de la telemedicina por la pandemia de covid-19, surgieron tiendas online que promocionaban la testosterona como remedio para las afecciones masculinas relacionadas con la edad, a pesar de las normas de la Administración de Drogas y Alimentos (FDA) emitidas hace años que restringen este tipo de publicidad sobre “testosterona baja”.
En anuncios de Google, Facebook y otros medios, los sitios web de telemedicina sobre testosterona pueden prometer una solución rápida para la “lentitud” y la libido baja en los hombres. Pero los médicos dicen que no hay pruebas de su eficacia, y que es más probable que las causas del decaimiento masculino para el que se promociona la testosterona como solución sean las afecciones crónicas, una dieta inadecuada o un estilo de vida sedentario.
De hecho, los médicos piden precaución, y la FDA recomienda que todos los suplementos de testosterona lleven la advertencia de que pueden aumentar el riesgo de infarto de miocardio y accidente cerebrovascular.
Existen razones médicas válidas para tratar a algunos hombres con testosterona. La hormona existe como medicamento desde hace décadas, y entre los pacientes actuales se encuentran hombres con hipogonadismo, algunos transexuales que la utilizan para facilitar la transición física y, en ocasiones, mujeres con síntomas menopáusicos. También ha sido utilizada durante décadas por fisicoculturistas y atletas para aumentar su fuerza.
Sin embargo, los dispensarios en internet pueden exagerar la idea de lo que a veces se denomina “menopausia masculina”, para impulsar las ventas de inyectables potenciadores de la testosterona, muy rentables, ignorando a menudo las directrices de seguridad que deberían impedir el uso de la hormona en hombres sanos. Algunos de los sitios web se dirigen a veteranos militares.
“He visto anuncios en Internet que se pasan de la raya”, afirmó Steven Nissen, médico y director académico del Heart, Vascular, and Thoracic Institute de la Clínica Cleveland. “Para el estado de ánimo y la baja energía, recetar testosterona aporta poco o ningún beneficio. Están promoviendo la testosterona para indicaciones que no figuran en la etiqueta”.
Casi todos los sitios web sobre testosterona citan un estudio publicado en 2002 por científicos de los New England Research Institutes, que descubrieron que los niveles de testosterona caen un 1% al año en hombres mayores de 40 años. Stefan Schlatt, director del Centro de Medicina Reproductiva y Andrología de la Universidad de Muenster, en Alemania, dijo que los datos que respaldaban la estadística incluían a hombres mayores con una salud deteriorada cuyos niveles disminuían a causa de enfermedades.
“Los hombres sanos no muestran ese descenso”, señaló.
Ese estudio de 2002 dio lugar a una avalancha de anuncios de “baja T” en la televisión estadounidense, anuncios que más tarde fueron prohibidos por la FDA, en una sentencia de 2015 que acusaba a la industria farmacéutica de exagerar el fenómeno de la baja T para asustar a los hombres y hacerles comprar medicamentos.
Según otro estudio, el mercado de suplementos de testosterona se situó en $1,850 millones en 2023.
El diluvio de anuncios “ha alimentado la demanda de un producto en gran parte no cubierto, lo que permite altos márgenes de beneficio”, explicó Geoffrey Joyce, director de políticas de salud en el USC Schaeffer Center for Health Policy & Economics e investigador del National Bureau of Economic Research. “El motor principal es la demanda fabricada”.
Barbara Mintzes, profesora de política farmacéutica basada en la evidencia en el Centro Charles Perkins de la Universidad de Sydney, Australia, dijo que el bajo nivel de testosterona debería considerarse realmente como un signo de una enfermedad que necesita tratamiento. Mintzes dijo que la diabetes, las cardiopatías, la hipertensión, la obesidad, la exposición a sustancias químicas tóxicas como los PFAS y el estrés pueden reducir los niveles de testosterona.
Varios de los sitios web analizados por KFF Health News se presentan como revistas de noticias y fitness, con anuncios insertados en los artículos que dirigen a los lectores hacia formularios para pedidos de terapia de sustitución de testosterona, abreviada como TRT.
Los precios de la TRT oscilan entre $120 y $135 al mes, sin incluir los análisis de sangre iniciales por correo, que cuestan unos $60. Algunos sitios prometen aumentar la libido y reducir la grasa del estómago.
Por ejemplo, los anuncios de Male Excel en Google dicen que la TRT “mejora el estado de ánimo” y “restaura la vitalidad”. Y su sitio dice que el tratamiento con testosterona proporcionará “definición muscular”, “pérdida de peso”, “impulso explosivo”, “sueño más profundo” y “energía restaurada” por encima de un enlace a una evaluación gratuita en su plataforma de telesalud en línea.
Craig Larsen, director general de la empresa, no respondió a varios intentos de establecer contacto por teléfono y correo electrónico.
Tanto Male Excel como Hone Health se encuentran entre los sitios que se dirigen a los veteranos militares. Hone Health incluía un video de un veterano que afirmaba que un hospital del Departamento de Asuntos de Veteranos le había denegado el tratamiento con testosterona.
Saad Alam, CEO y cofundador de Hone, afirmó que su empresa es “conservadora” en el mercado. Dijo que Hone receta sólo a los hombres que son hipogonadales y les hace pruebas cada 90 días, a diferencia de otras empresas que operan sitios web de telesalud a las que calificó de “cazadoras de dinero”.
“Estoy de acuerdo en que los pacientes deben ser tratados por sus médicos. Pero el sistema de salud estadounidense no está en condiciones de atender a los hombres que tienen este problema, y algunos endocrinólogos prefieren tratar a pacientes que proporcionan mayores beneficios”, dijo Hone. “Por eso la gente acude a nosotros”.
Una forma popular de TRT es el cipionato de testosterona inyectable. Según la base de datos de precios de venta de Medicare, cuesta $0,027 por miligramo. Los proveedores en internet que venden el fármaco directamente a los consumidores en viales de 200 mg/mL por un precio medio de $129 al mes están cobrando el equivalente a $1,55 por miligramo, un margen de beneficio de más de 50 veces el precio promedio de Medicare.
Según un estudio de 2022, los sitios web de telesalud de TRT crean una forma de eludir a los médicos que se niegan a recetar la hormona. En ese estudio, Justin Dubin, urólogo del Memorial Healthcare System de Florida, se hizo pasar por un consumidor. Declaró tener un nivel de testosterona por encima de lo normal y manifestó su deseo de formar una familia, a pesar de que este tipo de terapia puede frenar la producción de esperma. Sin embargo, seis de las siete clínicas online de TRT le recetaron testosterona a través de un profesional médico.
“Y eso es preocupante”, afirmó Dubin. “La telemedicina ayuda a los hombres con hipogonadismo que podrían sentirse demasiado avergonzados para hablar de disfunción eréctil. Pero tenemos que hacer un mejor trabajo para entender lo que es una atención apropiada”.
Aun así, aunque la FDA no permite la comercialización off-label (la práctica de recetar medicamentos para un uso distinto par el que han sido aprobados), sí permite las recetas off-label.
El uso off-label de reemplazo de testosterona se ha convertido en algo común entre los veteranos. Y entre los militares masculinos que recibieron TRT en 2017, menos de la mitad cumplieron con las pautas de práctica clínica, según un informe del ejército estadounidense.
Phil Palmer, veterano del Cuerpo de Marines, de 41 años, que vive en las afueras de Charleston, Carolina del Sur, dijo que paga de su bolsillo los análisis de sangre y las recetas para una forma de testosterona de implante cutáneo y para el clomifeno, un medicamento que puede ayudar a contrarrestar la infertilidad masculina que es un efecto secundario del tratamiento con testosterona.
Palmer explicó que el tratamiento es algo que le atrae tanto a él como a otros veteranos que se enfrentan a las secuelas de haber servido en las fuerzas armadas.
“El entorno en el que servimos y los niveles de estrés tienen mucho que ver”, afirmó Palmer. “Estuvimos expuestos a pozos de quema tóxicos. El ejército no te enseña a comer bien: comíamos mucha comida procesada”.
En el ámbito médico, la TRT puede acelerar la recuperación de los soldados que tienen problemas de densidad ósea o lesiones de la médula espinal, indicó Mark Peterson, profesor de medicina física y rehabilitación en la Facultad de Medicina de la Universidad de Michigan. Pero, agregó, “para los hombres en el rango normal de T, el uso de una receta en línea para comprar testosterona para reducir la grasa del estómago puede ser contraproducente”.
Quienes la utilizan también se arriesgan a tener que tomar medicación de testosterona indefinidamente, porque la TRT puede hacer que el cuerpo deje de producir su propia hormona.
Palmer, que fundó una organización sin fines de lucro que ayuda a los veteranos a recuperarse a través del ejercicio, la nutrición y la tutoría, dijo que la medicación le ha sido útil, pero insta a sus compañeros veteranos a recibir atención médica en lugar de lo que él llamó sitios web de “bro science” que promocionan la testosterona. (La “bro science” surge cuando los relatos anecdóticos de personas que practican fisicoculturismo en el gimnasio se consideran más creíbles que la investigación científica)
“No se trata de una píldora mágica”, concluyó.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Aging, Insurance, Noticias En Español, Public Health, Telemedicine
KFF Health News' 'What the Health?': Maybe It’s a Health Care Election After All
The Host
Julie Rovner
KFF Health News
Julie Rovner is chief Washington correspondent and host of KFF Health News’ weekly health policy news podcast, “What the Health?” A noted expert on health policy issues, Julie is the author of the critically praised reference book “Health Care Politics and Policy A to Z,” now in its third edition.
The general election campaign for president is (unofficially) on, as President Joe Biden and former President Donald Trump have each apparently secured enough delegates to become his respective party’s nominee. And health care is turning out to be an unexpectedly front-and-center campaign issue, as Trump in recent weeks has suggested he may be interested in cutting Medicare and taking another swing at repealing and replacing the Affordable Care Act.
Meanwhile, the February cyberattack of Change Healthcare, a subsidiary of insurance giant UnitedHealth Group, continues to roil the health industry, as thousands of hospitals, doctors, nursing homes, and other providers are unable to process claims and get paid.
This week’s panelists are Julie Rovner of KFF Health News, Anna Edney of Bloomberg News, Joanne Kenen of Johns Hopkins University and Politico Magazine, and Margot Sanger-Katz of The New York Times.
Panelists
Anna Edney
Bloomberg
Joanne Kenen
Johns Hopkins Bloomberg School of Public Health and Politico
Margot Sanger-Katz
The New York Times
Among the takeaways from this week’s episode:
- It is unclear exactly what Trump meant in his recent remarks about possible cuts to Medicare and Social Security, though his comments provided an opening for Biden to pounce. By running as the candidate who would protect entitlements, Biden could position himself well, particularly with older voters, as the general election begins.
- Health care is shaping up to be the sleeper issue in this election, with high stakes for coverage. The Biden administration’s expanded subsidies for ACA plans are scheduled to expire at the end of next year, and the president’s latest budget request highlights his interest in expanding coverage, especially for postpartum women and for children. Plus, Republicans are eyeing what changes they could make should Trump reclaim the presidency.
- Meanwhile, Republicans are grappling with an internal party divide over access to in vitro fertilization, and Trump’s mixed messaging on abortion may not be helping him with his base. Could a running mate with more moderate perspectives help soften his image with voters who oppose abortion bans?
- A federal appeals court ruled that a Texas law requiring teenagers to obtain parental consent for birth control outweighs federal rules allowing teens to access prescription contraceptives confidentially. But concerns that if the U.S. Supreme Court heard the case a conservative-majority ruling would broaden the law’s impact to other states may dampen the chances of further appeals, leaving the law in effect. Also, the federal courts are making it harder to file cases in jurisdictions with friendly judges, a tactic known as judge-shopping, which conservative groups have used recently in reproductive health challenges.
- And weeks later, the Change Healthcare hack continues to cause widespread issues with medical billing. Some small providers fear continued payment delays could force them to close, and it is possible that the hack’s repercussions could soon block some patients from accessing care at all.
Also this week, Rovner interviews Kelly Henning of Bloomberg Philanthropies about a new, four-part documentary series on the history of public health, “The Invisible Shield.”
Plus, for “extra credit” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: The Washington Post’s “Navy Demoted Ronny Jackson After Probe Into White House Behavior,” by Dan Diamond and Alex Horton.
Joanne Kenen: The Atlantic’s “Frigid Offices Might Be Killing Women’s Productivity,” by Olga Khazan.
Margot Sanger-Katz: Stat’s “Rigid Rules at Methadone Clinics Are Jeopardizing Patients’ Path to Recover From Opioid Addiction,” by Lev Facher.
Anna Edney: Scientific American’s “How Hospitals Are Going Green Under Biden’s Climate Legislation,” by Ariel Wittenberg and E&E News.
Also mentioned on this week’s podcast:
- KFF Health News’ “Energy-Hog Hospitals: When They Start Thinking Green, They See Green,” by Julie Appleby.
- Stat’s “The War on Recovery: How the U.S. Is Sabotaging Its Best Tools to Prevent Deaths in the Opioid Epidemic,” by Lev Facher.
Click to open the transcript
Transcript: Maybe It’s a Health Care Election After All
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News, and I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, March 14, at 10 a.m. Happy Pi Day, everyone. As always, news happens fast and things might have changed by the time you hear this, so here we go. We are joined today via video conference by Margot Sanger-Katz of The New York Times.
Margot Sanger-Katz: Good morning, everybody.
Rovner: Anna Edney of Bloomberg News.
Anna Edney: Hi there.
Rovner: And Joanne Kenen of the Johns Hopkins University and Politico Magazine.
Joanne Kenen: Hey, everyone.
Rovner: Later in this episode we’ll have my interview with Dr. Kelly Henning, head of the public health program at Bloomberg Philanthropies. She’ll give us a preview of the new four-part documentary series on the history of public health called “The Invisible Shield;” It premieres on PBS March 26. But first this week’s news. We’re going to start here in Washington with the annual State of the Union / budget dance, which this year coincides with the formal launch of the general election campaign, with both President Biden and former President Donald Trump having clinched their respective nominations this week.
Despite earlier claims that this year’s campaign would mostly ignore health issues, that’s turning out not so much to be the case. Biden in his speech highlighted reproductive health, which we’ll talk about in a minute, as well as prescription drug prices and the Affordable Care Act expansions. His proposed budget released on Monday includes suggestions of how to operationalize some of those proposals, including expanding Medicare’s drug negotiating powers. Did anything in particular in the speech or the budget jump out at any of you? Anything we weren’t expecting.
Edney: I wouldn’t say there was anything that I wasn’t expecting. There were things that I was told I should not expect and that I feel like I’ve been proven right, and so I’m happy about that, and that was the Medicare drug price negotiation. I thought that that was a win that he was going to take a lap on during the State of the Union, and certainly he did. And he’s also talking about trying to expand it, although that seems to face an extremely uphill battle, but it’s a good talking point.
Rovner: Well, and of course the expanded subsidies from the ACA expire at the end of next year. I imagine there’s going to be enough of a fight just to keep those going, right?
Edney: Yeah, certainly. I think people really appreciate the subsidies. If those were to go away, then the uninsured rate could go up. It’s probably an odd place in a way for Republicans, too, who are talking about, again, still in some circles, in some ways, getting rid of Obamacare. We’re back at that place even though I don’t think anyone thinks that’s entirely realistic.
Rovner: Oh, you are anticipating my next question, which is that former President Trump, who is known for being all over the place on a lot of issues, has been pretty steadfast all along about protecting Medicare and Social Security, but he’s now backing away from even that. In an interview on CNBC this week, Trump said, and I’m quoting, “There is a lot you can do in terms of entitlements in terms of cutting” — which his staff said was referring to waste and fraud, but which appears to open that up as a general election campaign issue. Yes, the Biden people seem to be already jumping on it.
Sanger-Katz: Yes. They could not be more excited about this. I think this has been an issue that Biden has really wanted to run on as the protector of these programs for the elderly. He had this confrontation with Congress in the State of the Union last year, as you may remember, in which he tried to get them to promise not to touch these programs. And I think his goal of weaponizing this issue has been very much hindered by Trump’s reluctance to take it on. I think there are Republicans, certainly in Congress, and I think that we saw during the presidential primary some other candidates for president who were more interested in rethinking these programs and concerned about the long-term trajectory of the federal deficit. Trump has historically not been one of them. What Trump meant exactly, I think, is sort of TBD, but I think it does provide this opening. I’m sure that we’ll see Biden talking about this a lot more as the campaign wears on and it wouldn’t surprise me at all to see this clip in television ads and featured again and again.
Kenen: So it’s both, I mean, it’s basically, he’s talked about reopening the repeal fight as Julie just mentioned, which did not go too well for the Republicans last time, and there’s plenty to cut in Medicare. If you read the whole quote, he does then talk about fraud and abuse and mismanagement, but the soundbite is the soundbite. Those are the words that came out of his mouth, whether he meant it that way or not, and we will see that campaign ad a lot, some version of it.
Rovner: My theory is that he was, and this is something that Trump does, he was on CNBC, he knew he was talking to a business audience, and he liked to say what he thinks the audience wants to hear without — you would think by now he would know that speaking to one audience doesn’t mean that you’re only speaking to that one audience. I think that’s why he’s all over the place on a lot of issues because he tends to tailor his remarks to what he thinks the people he is speaking directly to want to hear. But meanwhile, Anna, as you mentioned, he’s also raised the specter of the Affordable Care Act repeal again.
Sanger-Katz: I do think the juxtaposition of the Biden budget and State of the Union and these remarks from Trump, who now is officially the presumptive nominee for president, I think it really does highlight that there are pretty high stakes in health care for this election. I think it’s not been a focus of our discussion of this election so far. But Julie, you’ve mentioned the expiration of these subsidies that have made Affordable Care Act plans substantially more affordable for Americans and substantially more appealing, nearly doubling the number of people who are enrolled in these plans.
That is a policy that is going to expire at the end of next year. And so you could imagine a scenario, even if Trump did not want to repeal the Affordable Care Act, which he does occasionally continue to make noises about, where that could just go away through pure inertia if you didn’t have an administration that was actively trying to extend that policy and you could see a real retrenchment: increases in prices, people leaving the market, potentially some instability in the marketplace itself, where you might see insurers exiting or other kinds of problems and a situation much more akin to what we saw in the Trump administration where those markets were “OK, but were a little bit rocky and not that popular.”
I think similarly for Medicare and Medicaid, these big federal health programs, Biden has really been committed to, as he says, not cutting them. The Medicare price negotiation for drugs has provided a little bit more savings for the program. So it’s on a little bit of a better fiscal trajectory, and he has these additional proposals, again, I think long shots politically to try to shore up Medicare’s finances more. So you see this commitment to these programs and certainly this commitment to — there were multiple things in the budget to try to liberalize and expand Medicaid coverage to make postpartum coverage for women after they give birth, permanently one year after birth, people would have coverage.
Right now, that’s an option for states, but it’s not required for every state. And additionally to try to, in an optional basis, make it a little easier to keep kids enrolled in Medicaid for longer, to just allow states to keep kids in for the first six years of life and then three years at a time after that. So again, that’s an option, but I think you see the Biden administration making a commitment to expand and shore up these programs, and I do think a Trump administration and a Republican Congress might be coming at these programs with a bit more of a scalpel.
Rovner: And also, I mean, one of the things we haven’t talked about very much since we’re on the subject of the campaign is that this year Trump is ready in a way that he was not, certainly not in 2016 and not even in 2020. He’s got the Heritage Foundation behind him with this whole 2025 blueprint, people with actual expertise in knowing what to turn, what to do, actually, how to manipulate the bureaucracy in a way that the first Trump administration didn’t have to. So I think we could see, in fact, a lot more on health care that Republicans writ large would like to do if Trump is reelected. Joanne, you wanted to add something.
Kenen: Yeah, I mean, we all didn’t see this year as a health care election, and I still think that larger existential issues about democracy, it’s a reprise. It’s 2020 all over again in many ways, but abortion yes, abortion is a health care issue, and that was still going …
Rovner: We’re getting to that next.
Kenen: I know, but I mean we all knew that was still going to be a ballot driver, a voter driver. But Trump, with two remarks, however, well, there’s a difference between the people at the Heritage Foundation writing detailed policy plans about how they’re going to dismantle the CDC [Centers for Disease Control and Prevention] as we currently know it versus what Trump says off the cuff. I mean, if you say to a normal person on the street, we want to divide the CDC in two, that’s not going to trigger anything for a voter. But when you start talking about we want to take away your health care subsidies and cut Medicare, so these are sort of, some observers have called them unforced errors, but basically right now, yeah, we’re in another health care election. Not the top issue — and also depending on what else goes on in the world, because it’s a pretty shaky place at the moment. By September, will it be a top three issue? None of us know, but right now it’s more of a health care election than it was shaping up to be even just a few weeks ago.
Rovner: Yeah. Well, one thing, as you said, that we all know will be a big campaign issue this fall is abortion. We saw that in the State of the Union with the gallery full of women who’d been denied abortion, IVF services, and other forms of reproductive health care and the dozens of Democratic women on the floor of the House wearing white from head to toe as a statement of support for reproductive health care. While Democrats do have some divides over how strongly to embrace abortion rights, a big one is whether restoring Roe [v. Wade] is enough or they need to go even further in assuring access to basically all manner of reproductive health care.
It’s actually the Republicans who are most on the defensive, particularly over IVF and other state efforts that would restrict birth control by declaring personhood from the moment of fertilization. Along those lines, one of the more interesting stories I saw this week suggested that Donald Trump, who has fretted aloud about how unpopular the anti-abortion position is among the public, seems less likely to choose a strong pro-lifer as his running mate this time. Remember Mike Pence came along with that big anti-abortion background. What would this mean? It’s not like he’s going to choose Susan Collins or Lisa Murkowski or some Republican that we know actually supports abortion rights. I’m not sure I see what this could do for him and who might fit this category.
Kenen: Well, I think there’s a good chance he’ll choose a woman, and we all have names at the tip of our tongues, but we don’t know yet. But yeah, I mean they need to soften some of this stuff. But Trump’s own attempt right now bragging about appointing the justices that killed Roe, at the same time, he’s apparently talking about a 15-week ban or a 16-week ban, which is very different than zero. So he’s giving a mixed message. That’s not what his base wants to hear from him, obviously. I mean, Julie, you’ll probably get to this, but the IVF thing is also pitting anti-abortion Republican against anti-abortion Republican, with Mike Pence, again, being a very good example where Mike Pence’s anti-abortion bona fides are pretty clear, but he has been public about his kids are IVF babies? I’m not sure if all of them are, but at least some of them are. So he does not think that two cells in a freezer or eight cells or 16 cells is the same to child. In his view, it’s a potential child. So yeah.
Edney: I think you can do a lot with a vice president. We see Biden has his own issues with the abortion issue and, as people have pointed out, he demurred from saying that word in the State of the Union and we see just it was recently announced that Vice President Kamala Harris is going to visit an abortion clinic. So you can appease maybe the other side, and that might be what Trump is looking to do. I think, as Joanne mentioned, his base wants him to be anti-abortion, but now you’re getting all of these fractures in the Republican Party and you need someone that maybe can massage that and help with the crowd that’s been voting on the state level, voting on more of a personal level, to keep reproductive rights, even though his base doesn’t seem to be that that’s what they want. So I feel like he may be looking to choose someone who’s very different or has some differences that he can, not acknowledge, but that they can go out and please the other side.
Rovner: Of course, the only person who really fits that bill is Nikki Haley, who is very, very strongly anti-abortion, but at least tried, not very well, but tried to say that there are other people around and they believe other things and we should embrace them, too. I can’t think of another Republican except for Nikki Haley who’s really tried to do that. Margot, you wanted to say something?
Sanger-Katz: Oh, I was just going to say that if this reporting is correct, I think it does really reflect the political moment that Trump finds himself in. I think when he was running the last time, I think he really had to convince the anti-abortion voter, the evangelical voter, to come along with him. I think they had reservations about his character, about his commitment to their cause. He was seen as someone who maybe wasn’t really a true believer in these issues. And so I think he had to do these things, like choosing Mike Pence, choosing someone who was one of them. Pre-publishing a list of judges that he would consider for the Supreme Court who were seen as rock solid on abortion. He had to convince these voters that he was the real deal and that he was going to be on their side, and I just don’t think he really has that problem to the same degree right now.
I think he’s consolidated support among that segment of the electorate and his bigger concern going into the general election, and also the primaries are over, and so his bigger concern going into the general election is how to deal with more moderate swing voters, suburban women, and other groups who I think are a little bit concerned about the extreme anti-abortion policies that have been pursued in some of these states. And I think they might be reluctant to vote for Trump if they see him as being associated with those policies. So you see him maybe thinking about how to soften his image on this issue.
Rovner: I should point out the primaries aren’t actually over, most of states still haven’t had their primaries, but the primaries are effectively over for president because both candidates have now amassed enough delegates to have the nomination.
Sanger-Katz: Yes, that’s right. And it’s not over until the convention, although I think the way that the Republicans have arranged their convention, it’s very hard to imagine anyone other than Trump being president no matter what happens.
Rovner: Yes.
Sanger-Katz: Or not being president. Sorry, being the nominee.
Rovner: Being the nominee, yes, indeed. Well, we are only two weeks away from the Supreme Court oral arguments in the abortion pill case and a little over a month from another set of Supreme Court oral arguments surrounding whether doctors have to provide abortions in medical emergencies. And the cases just keep on coming in court this week. A three-judge panel from the 5th Circuit Court of Appeals upheld in part a lower court ruling that held that Texas’ law requiring parents to provide consent before their teenage daughters may obtain prescription birth control, Trump’s federal rules requiring patient confidentiality even for minors at federally funded Title X clinics.
Two things about this case. First, it’s a fight that goes all the way back to the Reagan administration and something called the “Squeal Rule,” which I did not cover, I only read about, but it’s something that the courts have repeatedly ruled against, that Title X is in fact allowed to maintain patient privacy even for teenagers. And the second thing is that the lower court ruling came from Texas federal Judge Matthew Kacsmaryk, who also wrote the decision attempting to overturn the FDA’s approval of the abortion drug mifepristone. This one, though, we might not expect to get to the Supreme Court.
Kenen: But we’re often wrong on these kinds of things.
Rovner: Yeah, that’s true.
Kenen: I mean, things that seem based on the historical pathway that shouldn’t have gotten to the court are getting to the court and the whole debate has shifted so far to the right. An interesting aside, there is a move, and I read this yesterday, but now I’m forgetting the details, so one of you can clarify for me. I can’t remember whether they’re considering doing this or the way they’ve actually put into place steps to prevent judge-shopping.
Rovner: That’s next.
Kenen: OK, I’m sorry, I’m doing such a good job of reading your mind.
Rovner: You are such a good job, Joanne.
Kenen: But I mean so many in these cases go back to one. If there was a bingo card for reproductive lawsuits, there might be one face in it.
Rovner: Two, Judge [Reed] O’Connor, remember the guy with the Affordable Care Act.
Kenen: Right. But so much of this is going back to judge-shopping or district-shopping for the judge. So a lot of these things that we thought wouldn’t get to the court have gotten to the court.
Rovner: Yeah, well, no, I was going to say in this case, though, there seems to be some suggestion that those who support the confidentiality and the Title X rules might not want to appeal this to the Supreme Court because they’re afraid they’ll lose. That this is the Supreme Court that overturned Roe, it would almost certainly be a Supreme Court that would rule against Title X confidentiality for birth control, that perhaps they want to just let this lie. I think as it stands now it only applies to the 5th Circuit. So Texas, Louisiana, and I forget what else is in the 5th Circuit, but it wouldn’t apply around the country and in this case, I guess it’s just Texas because it’s Texas’ law that conflicts with the rules.
Kenen: Except when one state does something, it doesn’t mean that it’s only Texas’ law six months from now.
Rovner: Right. What starts in Texas doesn’t necessarily stay in Texas.
Kenen: Right, it could go to Nevada. They may decide that they have a losing case and they want to wait 20 years, but other people end up taking things — I mean, it is very unpredictable and a huge amount of the docket is reproductive health right now.
Rovner: I would say the one thing we know is that Justice Alito, when he said that the Supreme Court was going to stop having to deal with this issue was either disingenuous or just very wrong because that is certainly not what’s happened. Well, as Joanne already jumped ahead a little bit, I mentioned Judge Kacsmaryk for a specific reason. Also this week, the Judicial Conference of the United States, which makes rules for how the federal courts work, voted to make it harder to judge-shop by filing cases in specific places like Amarillo, Texas, where there’s only one sitting federal judge. This is why Judge Kacsmaryk has gotten so many of those hot-button cases. Not because kookie stuff happens all the time in Amarillo, but because plaintiffs have specifically filed suit there to get their cases in front of him. The change by the judicial conference basically sets things back to the way they used to be, right, where it was at least partly random, which judge you got when you filed a case.
Kenen: But there are also some organizations that have intentionally based themselves in Amarillo so that they’re there. I mean, we may also see, if the rules go back to the old days, we may also still say you have a better case for filing in where you actually operate. So everybody just keeps hopping around and playing the field to their advantage.
Rovner: Yeah. And I imagine in some places there’s only a couple of judges, I think it was mostly Texas that had these one-judge districts where you knew if you filed there, you were going to get that judge, so — the people who watch these things and who worry about judge-shopping seem to be heartened by this decision by the judicial conference. So I’m not someone who is an expert in that sort of thing, but they seem to think that this will deter it, if not stop it entirely.
Moving on, remember a couple of weeks ago when I said that the hack of UnitedHealth [Group] subsidiary Change Healthcare was the most undercovered story in health? Clearly, I had no idea how true that was going to become. That processes 15 billion — with a B — claims every year handles one of every three patient records is still down, meaning hospitals, doctor’s offices, nursing homes, and all other manner of health providers still mostly aren’t getting paid. Some are worrying they soon won’t be able to pay their employees. How big could this whole mess ultimately become? I don’t think anybody anticipated it would be as big as it already is.
Sanger-Katz: I think it’s affecting a number of federal programs, too, that rely on this data, like quality measurement. And it really is a reflection, first of all, obviously of the consolidation of all of this, which I know that you guys have talked about on the podcast before, but also just the digitization and interconnectedness of everything. All of these programs are relying on this billing information, and we use that not just to pay people, but also to evaluate what kind of health care is being delivered, and what quality it is, and how much we should pay people in Medicare Advantage, and on all kinds of other things. So it’s this really complex, interconnected web of information that has been disrupted by this hack, and I think there’s going to be quite a lot of fallout.
Edney: And the coverage that I’ve read we’re potentially, and not in an alarmist way, but weeks away from maybe some patients not getting care because of this, particularly at the small providers. Some of my colleagues did a story yesterday on the small cancer providers who are really struggling and aren’t sure how long they’re going to be able to keep the lights on because they just aren’t getting paid. And there are programs now that have been set up but maybe aren’t offering enough money in these no-interest loans and things like that. So it seems like a really precarious situation for a lot of them. And now we see that HHS [Department of Health and Human Services] is looking into this other side of it. They’re going to investigate whether there were some HIPAA violations. So not looking exactly at the money exchange, but what happened in this hack, which is interesting because I haven’t seen a lot about that, and I did wonder, “Oh, what happened with these patients’ information that was stolen?” And UnitedHealth has taken a huge hit. I mean, it’s a huge company and it’s just taken a huge hit to its reputation and I think …
Rovner: And to its stock price.
Edney: And it’s stock price. That is very true. And they don’t know when they’re actually going to be able to resolve all of this. I mean, it’s just a huge mess.
Rovner: And not to forget they paid $22 million in ransom two weeks ago. When I saw that, I assumed that this was going to be almost over because usually I know when a hospital gets hacked, everybody says, don’t pay ransom, but they pay the ransom, they get their material back, they unlock what was locked away. And often that ends it, although it then encourages other people to do it because hey, if you do it, you can get paid ransom. Frankly, for UnitedHealthcare, I thought $22 million was a fairly low sum, but it does not appear — I think this has become such a mess that they’re going to have to rebuild the entire operation in order to make it work. At least, not a computer expert here. But that’s the way I understand this is going on.
Kenen: But I also think this, I mean none of us are cyber experts, but I’m also wondering if this is going to lead to some kind of rethinking about alternative ways of paying people. If this created such chaos, and not just chaos, damage, real damage, the incentive to do something similar to another, intermediate, even if it’s not quite this big. It’s like, “Wait, no one wants to be the next one.” So what kind of push is there going to be, not just for greater cybersecurity, but for Plan B when there is a crisis? And I don’t know if that’s something that the cyberexperts can put together in what kind of timeline — if HHS was to require that or whether the industry just decides they need it without requirements that this is not OK. It’s going to keep happening if it’s profitable for whoever’s doing it.
Rovner: I remember, ruefully, Joanne and I were there together covering HIPAA when they were passing it, which of course had nothing whatsoever to do with medical privacy at the time, but what it did do was give that first big push to start digitizing medical information. And there was all this talk about how wonderful it was going to be when we had all this digitally and researchers could do so much with it, and patients would be able to have all of their records in one place and …
Kenen: You get to have 19 passwords for 19 different forums now.
Rovner: Yes. But in 1995 it all seemed like a great, wonderful new world of everything being way more efficient. And I don’t remember ever hearing somebody talking about hacking this information, although as I point out the part of HIPAA that we all know, the patient medical records privacy, was added on literally at the last minute because someone said, “Uh-oh, if we’re going to digitize all this information, maybe we better be sure that it doesn’t fall into the wrong hands.” So at least somebody had some idea that we could be here. What are we 20, 30 … are we 30 years later? It’s been a long time. Anyway, that’s my two cents. All right, next up, Mississippi is flirting with actually expanding Medicaid under the Affordable Care Act. It’s one of only 10 remaining states that has not extended the program to people who have very low incomes but don’t meet the so-called categorical eligibility requirements like being a pregnant woman or child or person with a disability.
The Mississippi House passed an expansion bill including a fairly stringent work requirement by a veto-proof majority last week, week before.
Kenen: I think two weeks ago.
Rovner: But even if it passed the Senate and gets signed by the governor, which is still a pretty big if, the governor is reportedly lobbying hard against it. The plan would require a waiver from the Biden administration, which is not a big fan of work requirements. On the other hand, even if it doesn’t happen, and I would probably put my money at this point that it’s not going to happen this year, does it signal that some of the most strident, holdout states might be seeing the attraction of a 90% federal match and some of the pleas of their hospital associations? Anna, I see you nodding.
Edney: Yeah, I mean it was a little surprising, but this is also why I love statehouses. They just do these unexpected things that maybe make sense for their constituents sometimes, and it’s not all the time. I thought that it seemed like they had come around to the fact that this is a lot of money for Mississippi and it can help a lot of people. I think I’ve seen numbers like maybe adding 200,000 or so to the rolls, and so that’s a huge boost for people living there. And with the work requirement, is it true that even if the Biden administration rejects it, this plan can still go into place, right?
Kenen: The House version.
Edney: The House version.
Kenen: Yes.
Edney: Yeah.
Rovner: My guess is that’s why the governor is lobbying so hard against it. But yeah.
Kenen: I mean, I think that we had been watching a couple of states, we keep hearing Alabama was one of the states that has been talking about it but not doing anything about it. Wyoming, which surprised me when they had a little spurt of activity, which I think has subsided. I mean, what we’ve been saying ever since the Supreme Court made this optional for states more than 10 years ago now. Was it 2012? We’ve been saying eventually they’ll all do it. Keeping in mind that original Medicaid in [19]65, it took until 1982, which neither Julie nor I covered, until the last state, which was Arizona, took regular Medicare, Medicaid, the big — forget the ACA stuff. I mean, Medicaid was not in all states for almost 20 years. So I think we’ve all said eventually they’re going to do it. I don’t think that we are about to see a domino effect that North Carolina, which is a purple state, they did it a few months ago, maybe a year by now.
There was talk then that, “Oh, all the rest will do it.” No, all the rest will probably do it eventually, but not tomorrow. Mississippi is one of the poorest states in the country. It has one of the lowest health statuses of their population, obesity, diabetes, other chronic diseases. It has a very small Medicaid program. The eligibility levels are even for very, very, very poor childless adults, you can’t get on their plan. But have we heard rural hospitals pushing for this for a decade? Yes. Have we heard chambers of commerce in some of these states wanting it because communities without hospitals or communities without robust health systems are not economically attractive? We’ve been hearing the business community push for this for a long time. But the holdouts are still holdouts and I do think they will all take it. I don’t think it’s imminent.
Rovner: Yeah, I think that’s probably a fair assessment.
Kenen: It makes good economic sense, I mean, you’re getting all this money from the federal government to cover poor people and keep your hospitals open. But it’s a political fight. It’s not just a …
Rovner: It’s ideology.
Kenen: Yes, it’s not a [inaudible]. And it’s called Obamacare.
Edney: And sometimes things just have to fall into place. Mississippi got a new speaker of the House in their state government, so that’s his decision to push this as something that the House was going to take up. So whether that happens in other places, whether all those cards fall into places can take more time.
Kenen: Well, the last thing is we also know it’s popular with voters because we’ve seen it on the ballot in what, seven states, eight states, I forgot. And it won, and it won pretty big in really conservative states like Idaho and Utah. So as Julie said, this is ideology, it’s state lawmakers, it’s governors, it’s not voters, it’s not hospitals, it’s not chambers of commerce. It’s not particularly rural hospitals. A lot of people think this makes sense, but their own governments don’t think it makes sense.
Rovner: Yes. Well, another of those stories that moves very, very slowly. Finally, “This Week in Medical Misinformation”: I want to call out those who are fighting back against those who are accusing them of spreading false or misleading claims. I know this sounds confusing. Specifically, 16 conservative state attorneys general have called on YouTube to correct a, quote, “context disclaimer” that it put on videos posted by the anti-abortion Alliance Defending Freedom claiming serious and scientifically unproven harms that can be caused by the abortion pill mifepristone.
Unfortunately, for YouTube, their context disclaimer was a little clunky and conflated medication and surgical abortion, which still doesn’t make the original ADF videos more accurate, just means that the disclaimer wasn’t quite right. Meanwhile, more anti-abortion states are having legal rather than medical experts try to “explain” — and I put explain in air quotes — when an abortion to save the life of a woman is or isn’t legal, which isn’t really helping clarify the situation much if you are a doctor worried about having your license pulled or, at best, ending up having to defend yourself in court. It feels like misinformation is now being used as a weapon as well as a way to mislead people. Or am I reading this wrong?
Edney: I mean, I had to read that disclaimer a few times. Just the whole back-and-forth was confusing enough. And so it does feel like we’re getting into this new era of, if you say one wrong thing against the disinformation, that’s going to be used against you. So everybody has to be really careful. And the disclaimer, it was odd because I thought it said the procedure is [inaudible]. So that made me think, oh, they’re just talking about the actual surgical abortion. But it was clunky. I think clunky is a good word that you used for it. So yeah.
Rovner: Yeah, it worries me. I think I see all of this — people who want to put out misinformation. I’m not accusing ADF of saying, “We’re going to put out misinformation.” I think this is what they’ve been saying all along, but people who do want to put out misinformation for misinformation’s sake are then going to hit back at the people who point out that it’s misinformation, which of course there’s no way for the public to then know who the heck is right. And it undercuts the idea of trying to point out some of this misinformation. People ask me wherever I go, “What are we going to do about this misinformation?” My answer is, “I don’t know, but I hope somebody thinks of something.”
Kenen: I mean, if you word something poorly, you got to fix it. I mean, that’s just the bottom line. Just like we as journalists have to come clean when we make a mistake. And it feels bad to have to write a correction, but we do it. So Google has been working on — there’s a group convened by the Institute of Medicine [National Academy of Medicine] and the World Health Organization and some others that have come out with guidelines and credible communicators, like who can you trust? I mean, we talked about the RSV [respiratory syncytial virus] story I did a few weeks ago, and if you Google RSV vaccine on and you look on YouTube or Google, it’s not that there’s zero misinformation, but there’s a lot less than there used to be. And what comes up first is the reliable stuff: CDC, Mayo Clinic, things like that. So YouTube has been really working on weeding out the disinformation, but again, for their own credibility, if they want to be seen as clean arbiters of going with credibility, if they get something mushy, they’ve got to de-mush it at the end.
Rovner: And I will say that Twitter of all places — or X, whatever you want to call it, the place that everybody now is like, “Don’t go there. It’s just a mess” — has these community notes that get attached to some of the posts that I actually find fairly helpful and it lets you rate it.
Kenen: Some of them, I mean overall, there’s actually research on that. We’ll talk about my book when it comes out next year, but we have stuff. I’m in the final stages of co-authoring a book that … it goes into misinformation, which is why I’ve learned a lot about this. Community Notes has been really uneven and …
Rovner: I guess when it pops up in my feed, I have found it surprisingly helpful and I thought, “This is not what I expect to see on this site.”
Kenen: And it hasn’t stopped [Elon] Musk himself from tweeting misinformation about drugs …
Rovner: That’s certainly true.
Kenen: … drugs he doesn’t like, including the birth control pill he tells people not to use because it promotes suicide. So basically, yeah, Julie, you’re right that we need tools to fight it, and none of the tools we currently have are particularly effective yet. And absolutely everything gets politicized.
Sanger-Katz: And it’s a real challenge I think for these social media platforms. You know what I mean? They don’t really want to be in the editorial business. I think they don’t really want to be in the moderation business in large part. And so you can see them grappling with the problem of the most egregious forms of misinformation on their platforms, but doing it clumsily and anxiously and maybe making mistakes along the way. I think it’s not a natural function for these companies, and I think it’s not a comfortable function for the people that run these companies, who I think are much more committed to free discourse and algorithmic sharing of information and trying to boost engagement as opposed to trying to operate the way a newspaper editor might be in selecting the most useful and true information and foregrounding that.
Kenen: Yeah, I mean that’s what the Supreme Court has been grappling with too, is another [inaudible] … what are the rules of the game? What should be legally enforced? What is their responsibility, that the social media company’s responsibilities, to moderate versus what is just people get to post? I mean, Google’s trying to use algorithms to promote credible communicators. It’s not that nothing wrong is there, but it’s not what you see first.
Rovner: I think it’s definitely the issue of the 2020s. It is not going away anytime soon.
Kenen: And it’s not just about health.
Rovner: Oh, absolutely. I know. Well, that is the news for this week. Now, we will play my interview with Dr. Kelly Henning of Bloomberg Philanthropies, and then we’ll come back with our extra credits.
I am so pleased to welcome to the podcast Dr. Kelly Henning, who heads the Bloomberg Philanthropies Public Health program. She’s here to tell us about a new documentary series about the past, present, and future of public health called “The Invisible Shield.” It premieres on PBS on March 26. Dr. Henning, thank you so much for joining us.
Kelly Henning: Thank you for having me.
Rovner: So the tagline for this series is, “Public health saved your life today, and you don’t even know it.” You’ve worked in public health in a lot of capacities for a lot of years, so have I. Why has public health been so invisible for most of the time?
Henning: It’s a really interesting phenomenon, and I think, Julie, we all take public health for granted on some level. It is what really protects people across the country and across the world, but it is quite invisible. So usually if things are working really well in public health, you don’t think about it at all. Things like excellent vaccination programs, clean water, clean air, these are all public health programs. But I think most people don’t really give them a lot of thought every day.
Rovner: Until we need them, and then they get completely controversial.
Henning: So to that point, covid-19 and the recent pandemic really was a moment when public health was in the spotlight very much no longer behind an invisible shield, but quite out in front. And so this seemed like a moment when we really wanted to unpack a little bit more around public health and talk about how it works, why it’s so important, and what some of the opportunities are to continue to support it.
Rovner: I feel like even before the pandemic, though, the perceptions of public health were changing. I guess it had something to do with a general anti-science, anti-authority rising trend. Were there warning signs that public health was about to explode in people’s consciousness in not necessarily a good way?
Henning: Well, I think those are all good points, but I also think that there are young generations of students who have become very interested in public health. It’s one of the leading undergraduate majors nowadays. Johns Hopkins Bloomberg School of Public Health has more applications than ever before, and that was occurring before the pandemic and even more so throughout. So I think it’s a bit of a mixed situation. I do think public health in the United States has had some really difficult times in terms of life expectancy. So we started to see declines in life expectancy way back in 2017. So we have had challenges on the program side, but I think this film is an opportunity for us to talk more deeply about public health.
Rovner: Remind people what are some of the things that public health has brought us besides, we talk about vaccines and clean water and clean air, but there’s a lot more to public health than the big headlines.
Henning: Yeah, I mean, for example, seat belts. Every day we get into our vehicle, we put a seat belt on, but I think most people don’t realize that was initially extremely controversial and actually not so easy to get that policy in place. And yet it saved literally tens of hundreds of thousands of lives across the U.S. and now across the world. So seat belts are something that often come to mind. Similar to that are things like child restraints, what we would call car seats in the U.S. That’s another similar strategy that’s been very much promoted and the evidence has been created through public health initiatives. There are other things like window guards. In cities, there are window guards that help children not fall out of windows from high buildings. Again, those are public health initiatives that many people are quite unaware of.
Rovner: How can this documentary help change the perception of public health? Right now I think when people think of public health, they think of people fighting over mask mandates and people fighting over covid vaccines.
Henning: Yeah, I really hope that this documentary will give people some perspective around all the ways in which public health has been working behind the scenes over decades. Also, I hope that this documentary will allow the public to see some of those workers and what they face, those public health front-line workers. And those are not just physicians, but scientists, activists, reformers, engineers, government officials, all kinds of people from all disciplines working in public health. It’s a moment to shine a light on that. And then lastly, I hope it’s hopeful. I hope it shows us that there are opportunities still to come in the space of public health and many, many more things we can do together.
Rovner: Longtime listeners to the podcast will know that I’ve been exploring the question of why it has been so difficult to communicate the benefits of public health to the public, as I’ve talked to lots of people, including experts in messaging and communication. What is your solution for how we can better communicate to the public all of the things that public health has done for them?
Henning: Well, Julie, I don’t have one solution, but I do think that public health has to take this issue of communication more seriously. So we have to really develop strategies and meet people where they are, make sure that we are bringing those messages to communities, and the messengers are people that the community feels are trustworthy and that are really appropriate spokespeople for them. I also think that this issue of communications is evolving. People are getting their information in different ways, so public health has to move with the times and be prepared for that. And lastly, I think this “Invisible Shield” documentary is an opportunity for people to hear and learn and understand more about the history of public health and where it’s going.
Rovner: Dr. Kelly Henning, thank you so much for joining us. I really look forward to watching the entire series. OK, we are back. It’s time for our extra-credit segment. That’s when we each recommend a story we read this week we think you should read, too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Joanne, you have everybody’s favorite story this week. Why don’t you go first?
Kenen: I demanded the right to do this one, and it’s Olga, I think her last name is pronounced Khazan. I actually know her and I don’t know how to pronounce her name, but Olga Khazan, apologies if I’ve got it wrong, from The Atlantic, has a story that says “Frigid Offices Might Be Killing Women’s Productivity.” Well, from all of us who are cold, I’m not sure I would want to use the word “frigid,” but of all of us who are cold in the office and sitting there with blankets. I used to have a contraband, very small space heater hidden behind a trash basket under my desk. We freeze because men like colder temperatures and they’re wearing suits. So we’ve been complaining about being cold, but there’s actually a study now that shows that it actually hurts our actual cognitive performance. And this is one study, there’s more to come, but it may also be one explanation for why high school girls do worse than high school boys on math SATs.
Rovner: Did not read that part.
Kenen: It’s not just comfort in the battle over the thermostat, it’s actually how do our brains function and can we do our best if we’re really cold?
Rovner: True. Anna.
Edney: This is a departure from my normal doom and gloom. So I’m happy to say this is in Scientific American, “How Hospitals Are Going Green Under Biden’s Climate Legislation.” I thought it was interesting. Apparently if you’re a not-for-profit, there were tax credits that you were not able to use, but the Inflation Reduction Act changed that so that there are some hospitals, and they talked to this Valley Children’s in California, that there had been rolling blackouts after some fires and things like that, and they wanted to put in a micro-grid and a solar farm. And so they’ve been able to do that.
And health care contributes a decent amount. I think it’s like 8.5% of U.S. greenhouse gas emissions. And Biden had established this Office of Climate Change [and Health Equity] a few years ago and within the health department. So this is something that they’re trying to do to battle those things. And I thought that it was just interesting that we’re talking about this on the day that the top story, Margot, in The New York Times is, not by you, but is about how there’s this huge surge in energy demand. And so this is a way people are trying to do it on their own and not be so reliant on that overpowered grid.
Rovner: KFF Health News has done a bunch of stories about contribution to climate change from the health sector, which I had no idea, but it’s big. Margot.
Sanger-Katz: I wanted to highlight the second story in this Lev Facher series on treatment for opioid addiction in Stat called “Rigid Rules at Methadone Clinics Are Jeopardizing Patients’ Path to Recovery From Opioid Addiction,” which is a nice long title that tells you a lot about what is in the story. But I think methadone treatment is a really evidence-based treatment that can be really helpful for a lot of people who have opioid addiction. And I think what this story highlights is that the mechanics of how a lot of these programs work are really hard. They’re punitive, they’re difficult to navigate, they make it really hard for people to have normal lives while they’re undergoing methadone treatment and then, in some cases, arbitrarily so. And so I think it just points out that there are opportunities to potentially do this better in a way that better supports recovery and it supports the lives of people who are in recovery.
Rovner: Yeah, it used the phrase “liquid handcuffs,” which I had not seen before, which was pretty vivid. For those of you who weren’t listening, the Part One of this series was an extra credit last week, so I’ll post links to both of them. My story’s from our friend Dan Diamond at The Washington Post. It’s called “Navy Demoted Ronnie Jackson After Probe Into White House Behavior.” Ronnie Jackson, in case you don’t remember, was the White House physician under Presidents [Barack] Obama and Trump and a 2021 inspector general’s report found, and I’m reading from the story here, quote, “that Jackson berated subordinates in the White House medical unit, made sexual and denigrating statements about a female subordinate, consumed alcohol inappropriately with subordinates, and consumed the sleep drug Ambien while on duty as the president’s physician.” In response to the report, the Navy demoted Jackson retroactively — he’s retired —from a rear admiral down to a captain.
Now, why is any of this important? Well, mainly because Jackson is now a member of Congress and because he still incorrectly refers to himself as a retired admiral. It’s a pretty vivid story, you should really read it.
OK. That is our show. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us, too. Special thanks as always to our technical guru, Francis Ying, and our editor, Emmarie Huetteman. As always, you can email us your comments or questions. We’re at whatthehealth@kff.org, or you can still find me at X, @jrovner. Margot, where are you these days?
Sanger-Katz: I’m at all the places @Sanger-Katz, although not particularly active on any of them.
Rovner: Anna.
Edney: On X, it’s @annaedney and on Threads it’s @anna_edneyreports.
Rovner: Joanne.
Kenen: I’m Threads @joannekenen1, and I’ve been using LinkedIn more. I think some of the other panelists have said that people are beginning to treat that as a place to post, and I think many of us are seeing a little bit more traction there.
Rovner: Great. Well, we will be back in your feed next week. Until then, be healthy.
Credits
Francis Ying
Audio producer
Emmarie Huetteman
Editor
To hear all our podcasts, click here.
And subscribe to KFF Health News’ “What the Health?” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Elections, Health Industry, Insurance, Medicaid, Medicare, Multimedia, Pharmaceuticals, Public Health, States, Abortion, Biden Administration, Contraception, Drug Costs, Health IT, KFF Health News' 'What The Health?', Misinformation, Podcasts, Pregnancy, Women's Health
They Were Injured at the Super Bowl Parade. A Month Later, They Feel Forgotten.
KFF Health News and KCUR are following the stories of people injured during the Feb. 14 mass shooting at the Kansas City Chiefs Super Bowl celebration. Listen to how one Kansas family is coping with the trauma.
Jason Barton didn’t want to attend the Super Bowl parade this year. He told a co-worker the night before that he worried about a mass shooting. But it was Valentine’s Day, his wife is a Kansas City Chiefs superfan, and he couldn’t afford to take her to games since ticket prices soared after the team won the championship in 2020.
So Barton drove 50 miles from Osawatomie, Kansas, to downtown Kansas City, Missouri, with his wife, Bridget, her 13-year-old daughter, Gabriella, and Gabriella’s school friend. When they finally arrived home that night, they cleaned blood from Gabriella’s sneakers and found a bullet in Bridget’s backpack.
Gabriella’s legs were burned by sparks from a ricocheted bullet, Bridget was trampled while shielding Gabriella in the chaos, and Jason gave chest compressions to a man injured by gunfire. He believes it was Lyndell Mays, one of two men charged with second-degree felony murder.
“There’s never going to be a Valentine’s Day where I look back and I don’t think about it,” Gabriella said, “because that’s a day where we’re supposed to have fun and appreciate the people that we have.”
One month after the parade in which the U.S. public health crisis that is gun violence played out on live television, the Bartons are reeling from their role at its epicenter. They were just feet from 43-year-old Lisa Lopez-Galvan, who was killed. Twenty-four other people were injured. Although the Bartons aren’t included in that official victim number, they were traumatized, physically and emotionally, and pain permeates their lives: Bridget and Jason keep canceling plans to go out, opting instead to stay home together; Gabriella plans to join a boxing club instead of the dance team.
During this first month, Kansas City community leaders have weighed how to care for people caught in the bloody crossfire and how to divide more than $2 million donated to public funds for victims in the initial outpouring of grief.
The questions are far-reaching: How does a city compensate people for medical bills, recovery treatments, counseling, and lost wages? And what about those who have PTSD-like symptoms that could last years? How does a community identify and care for victims often overlooked in the first flush of reporting on a mass shooting: the injured?
The injured list could grow. Prosecutors and Kansas City police are mounting a legal case against four of the shooting suspects, and are encouraging additional victims to come forward.
“Specifically, we’re looking for individuals who suffered wounds from their trying to escape. A stampede occurred while people were trying to flee,” said Jackson County Prosecutor Jean Peters Baker. Anyone who “in the fleeing of this event that maybe fell down, you were trampled, you sprained an ankle, you broke a bone.”
Meanwhile, people who took charge of raising money and providing services to care for the injured are wrestling with who gets the money — and who doesn’t. Due to large donations from celebrities like Taylor Swift and Travis Kelce, some victims or their families will have access to hundreds of thousands of dollars for medical expenses. Other victims may simply have their counseling covered.
The overall economic cost of U.S. firearm injuries is estimated by a recent Harvard Medical School study at $557 billion annually. Most of that — 88% — represented quality-of-life losses among those injured by firearms and their families. The JAMA-published study found that each nonfatal firearm injury leads to roughly $30,000 in direct health care spending per survivor in the first year alone.
In the immediate aftermath of the shootings, as well-intentioned GoFundMe pages popped up to help victims, executives at United Way of Greater Kansas City gathered to devise a collective donation response. They came up with “three concentric circles of victims,” said Jessica Blubaugh, the United Way’s chief philanthropy officer, and launched the #KCStrong campaign.
“There were folks that were obviously directly impacted by gunfire. Then the next circle out is folks that were impacted, not necessarily by gunshots, but by physical impact. So maybe they were trampled and maybe they tore a ligament or something because they were running away,” Blubaugh said. “Then third is folks that were just adjacent and/or bystanders that have a lot of trauma from all of this.”
PTSD, Panic, and the Echo of Gunfire
Bridget Barton returned to Kansas City the day after the shooting to turn in the bullet she found in her backpack and to give a statement at police headquarters. Unbeknownst to her, Mayor Quinton Lucas and the police and fire chiefs had just finished a press conference outside the building. She was mobbed by the media assembled there — interviews that are now a blur.
“I don’t know how you guys do this every day,” she remembered telling a detective once she finally got inside.
The Bartons have been overwhelmed by well wishes from close friends and family as they navigate the trauma, almost to the point of exhaustion. Bridget took to social media to explain she wasn’t ignoring the messages, she’s just responding as she feels able — some days she can hardly look at her phone, she said.
A family friend bought new Barbie blankets for Gabriella and her friend after the ones they brought to the parade were lost or ruined. Bridget tried replacing the blankets herself at her local Walmart, but when she was bumped accidentally, it triggered a panic attack. She abandoned her cart and drove home.
“I’m trying to get my anxiety under control,” Bridget said.
That means therapy. Before the parade, she was already seeing a therapist and planning to begin eye movement desensitization and reprocessing, a form of therapy associated with treating post-traumatic stress disorder. Now the shooting is the first thing she wants to talk about in therapy.
Since Gabriella, an eighth grader, has returned to middle school, she has dealt with the compounding immaturity of adolescence: peers telling her to get over it, pointing finger guns at her, or even saying it should have been her who was shot. But her friends are checking on her and asking how she’s doing. She wishes more people would do the same for her friend, who took off running when the shooting started and avoided injury. Gabriella feels guilty about bringing her to what turned into a horrifying experience.
“We can tell her all day long, ‘It wasn’t your fault. She’s not your responsibility.’ Just like I can tell myself, ‘It wasn’t my fault or my responsibility,’” Bridget said. “But I still bawled on her mom’s shoulder telling her how sorry I was that I grabbed my kid first.”
The two girls have spent a lot of time talking since the shooting, which Gabriella said helps with her own stress. So does spending time with her dog and her lizard, putting on makeup, and listening to music — Tech N9ne’s performance was a highlight of the Super Bowl celebration for her.
In addition to the spark burns on Gabriella’s legs, when she fell to the concrete in the pandemonium she split open a burn wound on her stomach previously caused by a styling iron.
“When I see that, I just picture my mom trying to protect me and seeing everyone run,” Gabriella said of the wound.
It’s hard not to feel forgotten by the public, Bridget said. The shooting, especially its survivors, have largely faded from the headlines aside from court dates. Two additional high-profile shootings have occurred in the area since the parade. Doesn’t the community care, she wonders, that her family is still living with the fallout every day?
“I’m going to put this as plainly as possible. I’m f—ing pissed because my family went through something traumatic,” Bridget vented in a recent social media post. “I don’t really want anything other [than], ‘Your story matters, too, and we want to know how you’re doing.’ Have we gotten that? Abso-f—lutely not.”
‘What Is the Landscape of Need?’
Helped in part by celebrities like Swift and Kelce, donations for the family of Lopez-Galvan, the lone fatality, and other victims poured in immediately after the shootings. Swift and Kelce donated $100,000 each. With the help of an initial $200,000 donation from the Kansas City Chiefs, the United Way’s #KCStrong campaign took off, reaching $1 million in the first two weeks and sitting at $1.2 million now.
Six verified GoFundMe funds were established. One solely for the Lopez-Galvan family has collected over $406,000. Smaller ones were started by a local college student and Swift fans. Churches have also stepped up, and one local coalition had raised $183,000, money set aside for Lopez-Galvan’s funeral, counseling services for five victims, and other medical bills from Children’s Mercy Kansas City hospital, said Ray Jarrett, executive director of Unite KC.
Money for Victims Rolls In
Donations poured in for those injured at the Super Bowl Parade in Kansas City after the Feb. 14 shootings. The largest, starting with a $200,000 donation from the Kansas City Chiefs, is at the United Way of Greater Kansas City. Six GoFundMe sites also popped up, due in part to $100,000 donations each from Taylor Swift and Travis Kelce. Here’s a look at the totals as of March 12.United Way#KCStrong: $1.2 million.Six Verified GoFundMe AccountsLisa Lopez-Galvan GoFundMe (Taylor Swift donated): $406,142Reyes Family GoFundMe (Travis Kelce donated): $207,035Samuel Arellano GoFundMe: $11,896Emily Tavis GoFundMe: $9,518Cristian Martinez’s GoFundMe for United Way: $2,967Swifties’ GoFundMe for Children’s Mercy hospital: $1,060ChurchesResurrection (Methodist) “Victims of Violence Fund”: $53,358‘The Church Loves Kansas City’: $183,000
Meanwhile, those leading the efforts found models in other cities. The United Way’s Blubaugh called counterparts who’d responded to their own mass shootings in Orlando, Florida; Buffalo, New York; and Newtown, Connecticut.
“The unfortunate reality is we have a cadre of communities across the country who have already faced tragedies like this,” Blubaugh said. “So there is an unfortunate protocol that is, sort of, already in place.”
#KCStrong monies could start being paid out by the end of March, Blubaugh said. Hundreds of people called the nonprofit’s 211 line, and the United Way is consulting with hospitals and law enforcement to verify victims and then offer services they may need, she said.
The range of needs is staggering — several people are still recovering at home, some are seeking counseling, and many weren’t even counted in the beginning. For instance, a plainclothes police officer was injured in the melee but is doing fine now, said Police Chief Stacey Graves.
Determining who is eligible for assistance was one of the first conversations United Way officials had when creating the fund. They prioritized three areas of focus: first were the wounded victims and their families, second was collaborating with organizations already helping victims in violence intervention and prevention and mental health services, and third were the first responders.
Specifically, the funds will be steered to cover medical bills, or lost wages for those who haven’t been able to work since the shootings, Blubaugh said. The goal is to work quickly to help people, she said, but also to spend the money in a judicious, strategic way.
“We don’t have a clear sightline of the entire landscape that we’re dealing with,” Blubaugh said. “Not only of how much money do we have to work with, but also, what is the landscape of need? And we need both of those things to be able to make those decisions.”
Firsthand Experience of Daily Kansas City Violence
Jason used his lone remaining sick day to stay home with Bridget and Gabriella. An overnight automation technician, he is the family’s primary breadwinner.
“I can’t take off work, you know?” he said. “It happened. It sucked. But it’s time to move on.”
“He’s a guy’s guy,” Bridget interjected.
On Jason’s first night back at work, the sudden sound of falling dishes startled Bridget and Gabriella, sending them into each other’s arms crying.
“It’s just those moments of flashbacks that are kicking our butts,” Bridget said.
Tell Us About Your Experience
We are continuing to report on the effects of the parade shooting on the people who were injured and the community as a whole. Do you have an experience you want to tell us about, or a question you think we should look into? Message KCUR’s text line at (816) 601-4777. Your information will not be used in an article without your permission.
In a way, the shooting has brought the family closer. They’ve been through a lot recently. Jason survived a heart attack and cancer last year. Raising a teenager is never easy.
Bridget can appreciate that the bullet lodged in her backpack, narrowly missing her, and that Gabriella’s legs were burned by sparks but she wasn’t shot.
Jason is grateful for another reason: It wasn’t a terrorist attack, as he initially feared. Instead, it fits into the type of gun violence he’d become accustomed to growing up in Kansas City, which recorded its deadliest year last year, although he’d never been this close to it before.
“This crap happens every single day,” he said. “The only difference is we were here for it.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Health Care Costs, Public Health, States, Emergency Medicine, Guns, Investigation, Kansas, Missouri
Movimientos en contra de las vacunas perjudican a los niños más vulnerables
Gayle Borne ha cuidado a más de 300 niños en Springfield, Tennessee. Niños que rara vez han visto a un médico y que han sido tan descuidados que ni siquiera pueden hablar.
Una ley que este estado aprobó en 2023 —que requiere el consentimiento de los padres biológicos o tutores legales para que los niños reciban vacunas de rutina— vuelve a estos niños aún más vulnerables.
Gayle Borne ha cuidado a más de 300 niños en Springfield, Tennessee. Niños que rara vez han visto a un médico y que han sido tan descuidados que ni siquiera pueden hablar.
Una ley que este estado aprobó en 2023 —que requiere el consentimiento de los padres biológicos o tutores legales para que los niños reciban vacunas de rutina— vuelve a estos niños aún más vulnerables.
Los padres temporales, trabajadores sociales y otros cuidadores no pueden otorgar ese permiso.
En enero, Borne llevó a una bebé que estaba cuidando, que nació con poco apenas 2 libras, a su primera cita médica. Los proveedores de salud dijeron que sin el consentimiento de la madre de la niña, no podían vacunarla contra enfermedades como la neumonía, la hepatitis B y la polio.
La madre no ha sido localizada, por lo que un trabajador social tuvo que solicitar una orden judicial para poder vacunarla. “Estamos esperando”, dijo Borne. “Nuestras manos están atadas”.
La ley de Tennessee también impide que las abuelas y otros cuidadores que acompañan a los niños a citas de rutina cuando los padres están trabajando, en rehabilitación, o simplemente no pueden ir, otorguen ese permiso.
La ley pretende “devolverles a los padres el derecho a tomar decisiones médicas para sus hijos”.
Enmarcada en la retórica de la elección y el consentimiento, esta ley es una de más de una docena de propuestas recientes y pendientes en todo el país que usan la libertad para decidir de los padres en contra de la salud comunitaria y de los niños.
En realidad, crean obstáculos para la vacunación, el fundamento de la atención pediátrica. Siembran dudas sobre la seguridad de las vacunas en un clima lleno de desinformación médica.
Esta tendencia ha explotado a medida que políticos e influencers en las redes sociales hacen afirmaciones falsas sobre los riesgos de las vacunas, a pesar de los estudios que muestran lo contrario.
Los médicos tradicionalmente brindan información sobre vacunas a los cuidadores y obtienen su permiso antes de administrar más de una docena de inmunizaciones infantiles que protegen contra el sarampión, la polio y otras enfermedades debilitantes.
Pero ahora, la ley de Tennessee exige que los padres biológicos asistan a citas de rutina y firmen formularios de consentimiento para cada vacuna administrada durante dos años o más.
“Los formularios podrían tener un efecto disuasorio”, opinó el doctor Jason Yaun, pediatra de Memphis y ex presidente del capítulo de Tennessee de la Academia Americana de Pediatría. “Las personas que promueven los derechos parentales sobre las vacunas tienden a minimizar los derechos de los niños”, dijo Dorit Reiss, investigadora de políticas de vacunas en la Facultad de Derecho de la Universidad de California en San Francisco.
Baja en la tasa de vacunación de rutina
La desinformación, junto con un movimiento por el derecho de los padres que aleja la toma de decisiones de la salud pública, ha contribuido a las tasas de vacunación infantil más bajas en una década.
Este año, legisladores en Arizona, Iowa y West Virginia han presentado proyectos de ley relacionados con el consentimiento.
Una enmienda del Parent’s Bill of Rights en Oklahoma busca asegurar que los padres sepan que pueden eximir a sus hijos de los mandatos de vacunación escolar junto con las lecciones sobre educación sexual y el SIDA.
En Florida, el escéptico médico que lidera el Departamento de Salud del estado recientemente desafió las recomendaciones de los Centros para el Control y la Prevención de Enfermedades (CDC) diciéndoles a los padres que podían enviar a los niños no vacunados a la escuela durante un brote de sarampión.
El año pasado, Mississippi comenzó a permitir exenciones de los requisitos de vacunación escolar por motivos religiosos debido a una demanda financiada por la Informed Consent Action Network (ICAN), que está catalogada como una de las principales fuentes de desinformación antivacunas por el Center for Countering Digital Hate.
Aunque algunos proyectos de ley fracasen, Reiss teme que el resurgimiento del movimiento por los derechos de los padres pueda llevar a abolir leyes que requieren vacunas de rutina para asistir a la escuela.
En un reciente mitín de campaña, el candidato presidencial republicano Donald Trump dijo: “No daré ni un centavo a ninguna escuela que tenga un mandato de vacunación”.
Este movimiento se remonta a la pandemia de influenza de 1918, cuando algunos padres se opusieron a reformas progresistas que volvieron obligatorio asistir a la escuela y prohibieron el trabajo infantil. Desde entonces, las tensiones entre las medidas estatales y la libertad de los padres han estallado ocasionalmente sobre una variedad de temas.
Las vacunas se convirtieron en un tema prominente en 2021, cuando el movimiento encontró puntos en común con personas escépticas sobre las vacunas contra covid.
“El movimiento de derechos parentales no comenzó con las vacunas”, dijo Reiss, “pero el movimiento antivacunas se ha aprovechado, ampliando su alcance”.
Cuando legisladores callan a expertos
En Tennessee, los activistas antivacunas y las organizaciones de tendencia libertaria arremetieron contra el Departamento de Salud del estado en 2021 cuando recomendó vacunas contra covid a menores, siguiendo la orientación de los CDC.
Gary Humble, director ejecutivo del grupo conservador Tennessee Stands, pidió a los legisladores que criticaran al departamento por aconsejar el uso de máscaras y la vacunación.
También hubo repercusiones después que Michelle Fiscus, entonces directora de inmunización del estado, envió un aviso a los médicos. Les recordó que no necesitaban el permiso de los padres para vacunar a adolescentes de 14 años o más que dieran su consentimiento, según una regla estatal de décadas llamada Doctrina del Menor Maduro (Mature Minor Doctrine).
En las semanas siguientes, los legisladores estatales amenazaron con retirarle al departamento su financiamiento, y lo presionaron para que redujera la promoción de la vacuna contra covid, según reveló The Tennessean.
Fiscus fue despedida abruptamente. “Hoy me convertí en la vigésimo quinta de los 64 directores de programas de inmunización estatales y territoriales en dejar su puesto durante esta pandemia”, escribió en un comunicado. “Eso es casi el 40% de nosotros”.
La tasa de mortalidad por covid en Tennessee aumentó, convirtiéndose en una de las más altas del país a mediados de 2022.
Para cuando dos legisladores estatales presentaron un proyecto de ley para revertir la doctrina, el departamento de salud guardó silencio sobre la propuesta. A pesar de los obstáculos para los niños en hogares temporales que requerirían de una orden judicial para vacunas de rutina, el Departamento de Servicios Infantiles de Tennessee tampoco dijo nada.
El representante republicano John Ragan, quien presentó el proyecto en abril de 2023, dijo: “Los niños pertenecen a sus familias, no al estado”.
El representante demócrata Justin Pearson habló en contra del proyecto de ley. “No tiene en cuenta a las personas y niños que son descuidados”, le dijo a Ragan. “Estamos legislando desde un lugar de privilegio y no reconociendo a las personas que no tienen estos privilegios”, agregó.
El proyecto de Ragan obtuvo la mayoría y el gobernador republicano Bill Lee lo firmó en mayo, haciéndolo efectivo de inmediato.
Deborah Lowen, entonces subcomisionada de salud infantil en el Departamento de Servicios Infantiles, recibió decenas de llamadas de médicos que ahora enfrentan pena de cárcel y multas por vacunar a menores sin un consentimiento adecuado. “Me sentí, y me siento, muy descorazonada”, dijo.
Derecho a la salud
Yaun, el pediatra de Memphis, dijo que se sintió conmocionado cuando se negó a administrar una primera serie de vacunas a un bebé acompañado por un trabajador social. “Ese niño está entrando en una situación en donde está rodeado de otros niños y adultos”, dijo, “donde podría estar expuesto a algo y fracasamos en protegerlo”.
“Hemos tenido muchos abuelos enojados en nuestra sala de espera que traen a sus nietos a las citas porque los padres están trabajando o pasando por un mal momento”, dijo Hunter Butler, pediatra en Springfield, Tennessee. “Una vez llamé a una instalación de rehabilitación para encontrar a una madre y hablar con ella por teléfono para obtener su consentimiento verbal para vacunar a su bebé”, dijo. “Y no está claro si eso estuvo bien”.
Las tasas de vacunación infantil han disminuido por tres años consecutivos en Tennessee. A nivel nacional, las tendencias en baja de la vacunación contra el sarampión llevaron a los CDC a estimar que un cuarto de millón de niños de jardín de infantes están en riesgo de contraer la enfermedad altamente contagiosa.
Las comunidades con tasas bajas de vacunación son vulnerables a medida que el sarampión aumenta a nivel internacional. Los casos confirmados de sarampión en 2023 fueron casi el doble que en 2022, un año en el que la Organización Mundial de la Salud (OMS) estima que más de 136,000 personas murieron por la enfermedad en todo el mundo.
Cuando los viajeros infectados en el extranjero llegan a comunidades con bajas tasas de vacunación infantil, el virus altamente contagioso puede propagarse rápidamente entre personas no vacunadas, así como entre bebés demasiado pequeños para ser vacunados y personas con sistemas inmunes debilitados.
“Existe un aspecto de libertad en el otro lado de este argumento”, dijo Caitlin Gilmet, directora de comunicaciones del grupo de defensa de vacunas SAFE Communities Coalition and Action Fund. “Deberías tener el derecho de proteger a tu familia de enfermedades prevenibles”.
A finales de enero, Gilmet y otros defensores de la salud infantil se reunieron en una sala del Capitolio de Tennessee en Nashville y ofrecieron un desayuno gratuito. Distribuyeron folletos mientras los legisladores y sus asistentes llegaban a comer. Un folleto describía el costo de un brote de sarampión en 2018-19 en el estado de Washington que enfermó a 72 personas, la mayoría de las cuales no estaban vacunadas. El brote costó $76,000 en atención médica, $2,3 millones para la respuesta de salud pública y aproximadamente $1 millón en pérdidas económicas debido a la enfermedad, cuarentena y atención.
Barb Dentz, defensora del grupo de base Tennessee Families for Vaccines, repitió que la mayoría de los constituyentes del estado apoyan políticas sólidas a favor de las vacunas. De hecho, siete de cada 10 adultos estadounidenses sostuvieron que las escuelas públicas deberían exigir la vacunación contra el sarampión, las paperas y la rubéola, en una encuesta del Pew Research Center realizada el año pasado.
Pero las cifras han estado disminuyendo. “Proteger a los niños debería ser algo tan obvio”, le dijo Dentz al representante republicano Sam Whitson. Whitson estuvo de acuerdo y reflexionó sobre una explosión de desinformación antivacunas. “El Dr. Google y Facebook han sido un desafío tan grande”, dijo. “Combatir la ignorancia se ha convertido en un trabajo de tiempo completo”.
Whitson fue uno de los pocos republicanos que votaron en contra de la enmienda de vacunas de Tennessee del año pasado. “La cuestión de los derechos de los padres realmente se ha afianzado”, dijo, “y puede ser utilizada a nuestro favor y en nuestra contra”.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
1 year 7 months ago
Health Industry, Noticias En Español, Public Health, States, Arizona, Children's Health, Iowa, Misinformation, Mississippi, Tennessee, vaccines, West Virginia